Introduction
The World Health Organization (WHO) in its “Global strategy on digital health 2020-2025” recognizes that information and communications technologies (ICT) present new opportunities and challenges for the achievement of all 17 Sustainable Development Goals and will be an essential enabling factor towards ensuring that more people worldwide benefit from universal health coverage, are better protected from health emergencies, enjoy better health and well-being (WHO’s triple billion targets included in its Thirteenth General Programme of Work, 2019-2023). The proper use of digital technologies considers safety, ethical use, cost-effectiveness, and affordability. It is people-centered, evidence-based, effective, efficient, sustainable, inclusive, equitable, and contextualized, supporting knowledge and practice associated with the development. ICT technologies are used to exchange valid information for diagnosis, treatment, and prevention of disease and injuries, research and evaluation, and the continuing education of healthcare workers to help deliver better healthcare services. They can help improve the health of individuals and communities.
The evolution of the Internet and how technology is integrated into so many daily activities in society is seen as a great opportunity to complement healthcare in ways that before were impossible. ICT is revolutionizing how procedures are carried out, offering innovations that promote healthcare efficiency and quality. ICT should not compromise communication, relationships with patients, understanding of relevant information, treatment, or the principal objectives of contact related to whatever health condition any person has, anywhere, at a specific moment. If used correctly, it can help overcome schedule obstacles and space limitations of health institutions, reduce the stress felt by health professionals, and facilitate simultaneous access to fundamental information while interacting with patients without compromising security issues, making patients and their families feel less abandoned and more accompanied by the health team.
Analyzing communication processes with patients who rely on ICT will help highlight what knowledge and skills are required for its effective use in evidence-based health practices. Health professionals should be prepared for the constant evolution of technology and digital solutions that can provide appropriate, humanized, and constructive responses to the needs of patients by communicating efficiently and transmitting clear, accurate, and safe health information.
This scoping review aims to review, explore, assess, and map studies that analyze the use of ICT by nurses within the scope of their professional activity to communicate with patients. The primary objectives are to identify situations in which the use of ICT is required, the challenges faced during the distant interactions, and the perceived needs to overcome them. Additionally, the review seeks to highlight communication skills that training programs should consider preparing nurses for an aging society in a digital and technologically dependent era.
1. Methods
A scoping review design was used to disseminate the field of inquiry and supported the process of identifying the knowledge gaps within the existing evidence (Arksey & O’Malley, 2005). This scoping review followed the guidelines of the Joanna Briggs Institute framework, with search results reported as defined by the PRISMA ScR for scoping review guidelines, respecting the five stages as described by the methodological framework of Arksey and O’Malley. As a complement, the recommendations by Levac et al. (2010) on the Arksey and O’Malley framework have been used. The final protocol was registered with the Open Science Framework in May 2024 (https://osf.io/yk5jp/).
1.1 Stage 1: identifying the research question
The article selection protocol began with the identification of a problem and research questions using the PCC acronym [P (Population = nurses); C (Concept = knowledge and skills in the use of ICT in communication processes with patients] and C (Context = hospital and primary health care centers)]. For the purpose and objectives of this review, the questions asked were: a) What are the situations in which ICT is used in nurse-patient communication? b) What are the benefits of using digital and technological solutions to communicate with patients? c) What are the problems and difficulties experienced by these health professionals in these interactions? d) Which digital communication skills, integrating the use of differentiated technologies, are needed and could/should be included in health professionals' professional training programs?
1.2 Stage 2: identifying relevant studies
The purpose of this study is mainly focused on using ICT specifically for communication purposes by nursing health professionals in hospitals and primary health care centers. The focus of this study was communication processes using different technologies and digital solutions between nurses and patients, and as such, papers were included if they had content related to the use of ICT in communication processes between health professionals and patients and were excluded if they were concerned with other non-digital communication processes or communication between health professionals and/or focused on the use of technologies mainly for clinical practices and health monitoring (eHealth). The systematic search strategy, conducted between February and April 2024, of Portuguese and English language articles published between 2014 and 2024 included papers exclusively related to nurse-patient communications using ICT, encompassing the following databases: Latin American and Caribbean Literature in Health Sciences (LILACS); ScienceDirect and PubMed using the Boolean operator “AND” and “OR”. Subsequently, other research was carried out in Google Scholar and different search engines using natural terms (grey literature) such as: “ICT used by nurses to communicate with patients,” “nurse-patient digital communication,” and “nursing remote communication with patients.” A ten-year focused time interval was defined because the digital landscape evolves very quickly to achieve relevance (a restricted number of studies could be included outside this date range if nothing more recent could be identified). Research studies, press releases, newspaper articles, editorials in journals, government, health service policy papers, and other grey literature were also considered.
1.3 Stage 3: study selection
As suggested by JBI (Peters et al., 2020), the selection of studies includes two phases: the first phase involves screening the title and abstract, while the second phase involves a full-text reading of the study based on the inclusion and exclusion criteria described above. Thus, through a preliminary selection, the title and abstract of each article were individually analyzed by two reviewers (MP, RSA) based on eligibility criteria to identify relevant articles and exclude irrelevant ones. Subsequently, the reviewers analyzed the full text of the articles for inclusion. In cases of disagreement between the two reviewers regarding the inclusion or exclusion of a particular study, a third reviewer (AM) was consulted. The Rayyan platform was used to aid with the management and elimination of duplicates of the collected references in databases (Ouzzani et al., 2016). Eligible articles were then analyzed and compiled following the recommendations of PRISMA-ScR. Titles and/or abstracts that were not suggestive of the intended theme, articles that did not allow their full reading, and records that did not cover the inclusion criteria and answer the guiding questions, including systematic reviews and other reviews with similar research, were excluded.
1.4 Stage 4: charting the data
The full text of the included abstracts was obtained to be read and determine which studies could be included in the review. Data extraction and analysis were focused on a descriptive approach. Articles were carefully analyzed and summarized (based on the research questions) and the data collected was organized in Microsoft Excel in a standardized evidence sheet, organized according to the following items: author(s); year of publication; country; study design type; methods; participants’ characteristics or target groups; communication context or location; purpose/aims of the study; data collection and analysis methods; and technology used in the study. The data retrieved from this analysis enabled the identification of relevant articles for this Scoping Review, since when compiling the information, articles were also identified that only the full-text reading allowed to verify the presence of reliability conditions related to the exclusion criteria.
1.5 Stage 5: collating, summarizing, and reporting the results
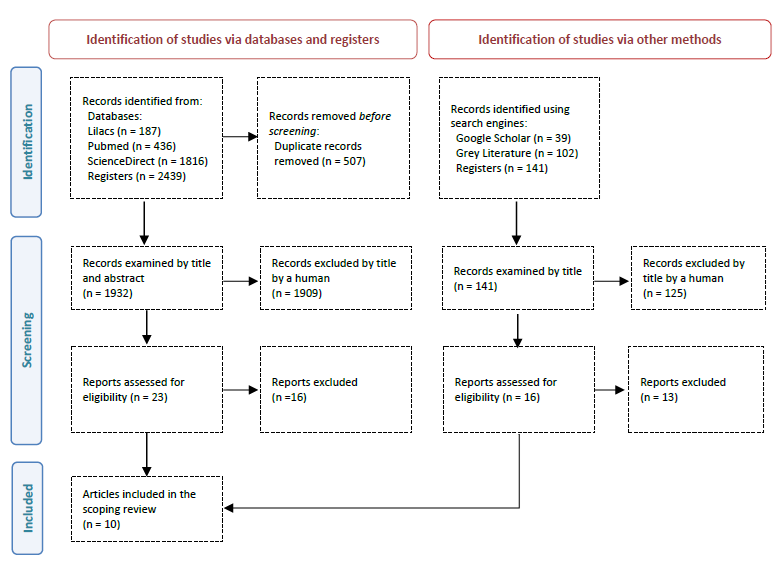
Finally, studies were summarized descriptively and compared for similarities and differences, data of interest were extracted in a summarized form and the results were reported. A second sheet was created with the key findings/results of the included studies, with the following data: ICT used in nurse-patient communication; Communication skills and interactions identified or considered in the studies; Perceptions of the benefits of using ICT; Difficulties felt in distant communication using ICT; and needs identified. The search strategy and the different stages of selection, eligibility, and inclusion of articles are shown in Figure 1.
2. Results
The search resulted in 2073 records (without duplicates) of which 39 records were considered relevant and selected for their titles and/or abstracts. Of those, full-text articles were assessed for eligibility, which resulted in 10 articles for inclusion. The results of the identification process and selection phases of the study were described in detail based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) (Page et al., 2021) in Figure 1.
The selected studies were conducted in different countries, in different continents around the world, namely in Brazil (n = 2), Chile (n = 1), Netherlands (n = 1), Portugal (n = 1), Sweden (n = 2), South Correia (n =1), Spain (n =1) and USA (n = 1), evidencing the global importance of the use of technology in distant nurse-patient communication processes. The collected data was organized in two tables: Supplementary Material 1 with information about the author(s), year of publication, country, study design type, methods; participants’ characteristics or target groups, communication context or location, purpose/aims of the study, data collection and analysis methods, and technology used in the study; and Supplementary Material 2 with a summary of the key findings related to ICT used in the nurse-patient communication, identified communication skills and interactions, the benefits of using ICT, difficulties felt in distant communication while using ICT, and needs that can help overcome the limitations of distant nurse-patient communication.
ICT used in nurse-patient communication
The main technologies used by nurses to communicate with patients, mentioned in the selected articles, were telephone or cell phone (using only audio system) (Barbosa & Silva, 2017; Barbosa, 2017; Ravazi et al., 2015; Eriksson et al., 2020; Alpert et al., 2017; Navarro-Martinez et al., 2024; Houwelingen et al., 2016; Pimentel et al., 2022) and real-time video conferencing, available to any person with a smartphone or a computer with Internet connection, including social media networks (using video and audio system) (Barbosa & Silva, 2017; Barbosa, 2017; Ravazi et al., 2015; Escudero et al., 2022; Houwelingen et al., 2016; Pimentel et al., 2022; Yoo & Lee, 2022). Other ICT mentioned in the study were professional teleconsultation solutions in a confidential online environment (Escudero et al., 2022; Houwelingen et al., 2016), written electronic messaging by SMS or email (Barbosa, 2017; Ravazi et al., 2015; Alpert et al., 2017), and complementary electronic medical record systems to access patient data and add information related to the teleconsultation (Barbosa & Silva, 2017; Eriksson et al., 2020).
Communication skills and interactions identified or considered in the studies
The relevant skills, related to distant online communication processes referred in articles, were: being able to understand and learn verbal and non-verbal aspects of communication while using technology (Barbosa & Silva, 2017; Barbosa, 2017; Ravazi et al., 2015; Eriksson et al., 2020; Houwelingen et al., 2016; Pimentel et al., 2022); developing effective communication, based on authentic interpersonal relationships (bilateral process), essential to fulfil and respect the nurse-patient relationship and maintain mutual trust (Barbosa & Silva, 2017; Barbosa, 2017; Eriksson et al., 2020; Escudero et al., 2022; Houwelingen et al., 2016; Pimentel et al., 2022); knowing how to communicate well, in a clear and resolute manner, paramount for patient safety and avoid mistakes that could lead to misconduct of the assistance, and ensure that the receiver understood the message objectively (Barbosa, 2017; Houwelingen et al., 2016; Pimentel et al., 2022); having the ability to ask questions related to the patient’s problem and make the correct diagnosis, which is only possible if nurses know how to gather information, then use implicit and explicit information to identify the patients’ needs and translate healthcare information back into a language that is comprehensible to the patient (Ravazi et al., 2015; Eriksson et al., 2020; Houwelingen et al., 2016; Pimentel et al., 2022); interpreting and writing different electronic messages (received by and sent to the patients), including knowing how to answer and send reports that document the distant meetings (Razavi et al, 2015; Alpert et al., 2017; Houwelingen et al., 2016; Pimentel et al., 2022); having the ability to put patients at ease when they feel insecure about using technology (Houwelingen et al., 2016; Pimentel et al., 2022; Yoo & Lee, 2022); being able to consider ICT as a ‘‘humanizer’’ of care that can improve nurse-patient communication and reach those that cannot be reached without technology (Navarro-Martinez et al., 2024; Houwelingen et al., 2016; Pimentel et al., 2022); using different communication strategies regarding the patient type (Escudero et al., 2022; Houwelingen et al., 2016; Pimentel et al., 2022); and finally knowing how to enhance contact through technology (e.g., use of voice, light, background, body language) (Houwelingen et al., 2016).
Perceptions of the benefits of using ICT
All the studies in this review consider various benefits and positive aspects related to the use of diverse technologies and digital solutions to enhance distant communication with patients. Technology is seen as a facilitator, enabling increased accessibility for patients (contact without having to leave their home, reduced travel times) and for specialists/nurses who have immediate access to the necessary information related to their work processes, reducing costs of healthcare delivery, increasing the effectiveness and efficiency of the health services, especially in situations that demand immediate action (Barbosa & Silva, 2017; Barbosa, 2017; Ravazi et al., 2015; Eriksson et al., 2020; Navarro-Martinez et al., 2024; Pimentel et al., 2022; Yoo & Lee, 2022). Technology enables flexibility to communicate through different channels with patients, nurses have more autonomy regarding planning working schedules and have the freedom to choose a time and place to contact [Razavi et al., 2015; Houwelingen et al., 2016; Pimentel et al., 2022). Patients become more active communicators and more active participants in their own care (partnership building). In some cases, electronic and digital communication has a positive impact on communication and is seen as less intimidating than in-person encounters, reducing inequality in care access and strengthening citizen power, through greater availability, accessibility, convenience, speed, and humanization of services. In these cases, distant communication using ICT is seen as a promoter of proximity between nurses and patients (Barbosa, 2017; Ravazi et al., 2015; Alpert et al., 2017; Houwelingen et al., 2016; Pimentel et al., 2022). Using specific telenursing solutions helps guarantee the security of patient information and reduces the risk of cross-infection (Eriksson et al., 2020; Alpert et al., 2017; Pimentel et al., 2022). Finally, using technology to provide healthcare remotely in an integrated approach, combining both in-person and virtual care to meet the diverse needs of patients, is seen as positive and a major strategy to address the continuous increase in the demand for care and a shrinking care professional population (Razavi et al., 2015; Navarro-Martinez et al., 2024; Escudero et al., 2022; Houwelingen et al., 2016; Pimentel et al., 2022).
Difficulties felt in distant communication using ICT
Various difficulties and obstacles related to the use of ICT in communication and distant interactions with patients were identified. It is more difficult to perceive and understand nonverbal signals due to the "emotional" distance that physical distance in a virtual environment can provoke (related to eye contact, facial expressions, body positioning, gestures, and “clues” that could change the meaning of verbal expressions), requiring a greater degree of attention and could become an obstacle related to the practical dimension of care (Barbosa & Silva, 2017; Barbosa, 2017; Ravazi et al., 2015; Escudero et al. 2022; Pimentel et al., 2022). Distance communication can influence the consultation itself and the outcomes of the patient’s understanding of the issues discussed during the consultation and compliance with the proposed therapy. It is difficult to validate the data evaluated by the patient, patient satisfaction, and acceptance (Barbosa & Silva, 2017; Pimentel et al., 2022). It is more difficult to convey confidence and trust when using technology due to the absence of physical contact (it is difficult to validate what is being said by the patient), complicating the communication process. The lack of physical contact with patients obliges health professionals to use their professional experience and different methods to obtain accurate information from the patients to be able to evaluate their needs correctly (active learning) (Barbosa & Silva, 2017; Barbosa, 2017; Ravazi et al., 2015; Pimentel et al., 2022). Social issues associated with the advanced age of health service users and social inequalities associated with the need to use technology are of particular concern to nurses (Navarro-Martinez et al., 2024). Computer-mediated communication through electronic messages can be impersonal (Alpert et al., 2017; Pimentel et al., 2022) and difficulties felt in distant interactions (inadequately listening to the patient’s complaint, not asking enough questions, failures in the accessibility of the patient to the nurse, routines/guidelines not followed as they should, technical problems and inadequate communication problem, being misinterpreted, not being understood) hinders communication and can lead to incorrect evaluations of the patients, medical errors and malpractice (Barbosa, 2017; Escudero et al., 2022). Patients have high expectations and misconceptions about video consultations, but some limitations make it impossible to help all patients. In some cases, providing health care only digitally will not cover all aspects needed to treat a patient or all types of diseases, and cannot be used with all patients and in all situations (Razavi et al., 2015; Alpert et al., 2017; Navarro-Martinez et al., 2024). Also, patients’ inability, unfamiliarity with the digital setting, and lack of sufficient knowledge of how to communicate and behave in the video consultation meetings affect the quality of online care. Technical problems, the quality of the internet connection and ignorance related to the use of technology are difficulties felt both by patients and nurses (Barbosa, 2017; Ravazi et al., 2015). Environment and context aspects associated with not knowing how to use the technology correctly in long-distance interactions (such as not being able to use the camera, the incorrect position of the camera, looking at the camera but not at the person, the patient leaves your field of vision, ...) create barriers that compromise the communication process (Barbosa, 2017; Ravazi et al., 2015). It may be a further role of nurses to teach the patient to use technology, thus reinforcing their digital leadership (Razavi et al., 2015; Navarro-Martinez et al., 2024; Pimentel et al., 2022) but they lack professional experience and insufficient training in distance consultation using technology. Nurses are aware of the importance of being well-trained to be able to apply new digital systems and their usefulness in training patients to be able to use such systems, but most nurses are not trained or are insufficiently trained to use these technologies effectively. Leaders fail to promote and encourage its use; therefore, the potential of telehealth fails to reach full utilization (Navarro-Martínez et al., 2024; Houwelingen et al., 2016; Pimentel et al., 2022; Yoo & Lee, 2022). Other barriers associated with the lack of technological resources, lack of adequate or obsolete equipment, logistical and financial constraints (by health services and patients), compromise distant communication and telenursing (Navarro-Martinez et al., 2024; Pimentel et al., 2022). Patient security, privacy issues, legal coverage and the protocols that guide their actions as professionals, the legal validity of the consultation, content to be addressed and records, and data protection, are of the utmost importance (Barbosa, 2017; Alpert et al., 2017; Navarro-Martinez et al., 2024; Pimentel et al., 2022). Digital literacy of patients and nurses, lack of regulations or good practice guidelines and all the other aspects referred previously feed feelings of skepticism and criticism in using technology to communicate, combined with the reluctances associated with resistance to change, fear of the unknown or inappropriate use, by both professionals and patients, compromising the transition to technological solutions (Razavi et al., 2015; Navarro-Martinez et al., 2024; Pimentel et al., 2022).
Needs identified
The complex nature of healthcare associated with an aging population suffering from multiple chronic diseases requires new ways of providing care to patients and citizens, making it difficult for nurses to stay up to date. There is an increasing need for training courses to review all the changes occurring (Razavi et al., 2015). All the studies included in this review refer to the need for continuous training programs to help healthcare professionals develop better interpersonal communication skills when using technological solutions in distant communication with patients. Nurses need to develop the ability to perceive how patients receive the messages and whether they have fully understood them. Communicating well through technology, developing “relationship” skills, and knowing how to interpret verbal and non-verbal signals (being a good listener and good interpreter) must be taught to avoid errors related to the care (Barbosa & Silva, 2017; Barbosa, 2017). Nurses must develop new and advanced communication skills to access and give advice (interpreting skills) to compensate for the lack of visual signs in distant communication (Eriksson et al., 2020). Telehealth-specific training (such as talking to a camera, being recorded, having good diction, not speaking with your back to the microphone, lowering your voice, expressions, acronyms, slang in excess, maintaining visual contact, keen observation, tone of voice) must be taught to overcome communication barriers (Barbosa, 2017). Competence development of care professionals for today’s health care, providing care digitally, is a necessity (Razavi et al., 2015) to overcome resistance to digital communication (Alpert et al., 2017). The development of communication skills as part of the training of nursing students is a cornerstone of nursing care (Escudero et al., 2022) and the nursing profession must contribute to and keep pace with the digital transformation to ensure digital health technology is developed and applied in a way that meets the needs of individuals, families, communities, and the health workforce (Navarro-Martinez et al., 2024). Institutions should provide resources to ensure the use of health ICT by nurses, ensuring access to appropriate equipment and training for its use. Each care context must have a procedure that includes the criteria, standards, and recommendations for telenursing. Health institutions should partner with other entities to improve equity in access to distance services and promote digital health literacy (Navarro-Martinez et al., 2024; Pimentel et al., 2022).
The patterns, advances, gaps, evidence for practice, and research recommendations (Bradbury-Jones et al., 2021) are shown in Table 1. The results were summarized under two patterns. These included types of information and communication technologies and the specific communication skills required in distant nurse-patient interactions. This review showed that there is strong evidence supporting the benefits of using ICT in nurse-patient distance communication in countries all over the world. All the studies referred to the need for specific training and education for nursing professionals in the use of technology and digital solutions for communication purposes to overcome all the mentioned limitations and constraints.
Table 1 Summary of the review according to the PAGER framework
| Patterns | Types of ICT | Communication skills using ICT |
| Advances | Strong evidence supports the substantial use of different technology and digital solutions in nurse-patient communication. | Studies refer the relevance of developing specific distant communicating skills that can help avoid errors and risks related to the care while using ICT. |
| Gaps | Lack of studies to understand which technologies are more adequate and should be accessible to nurses and patients. | Lack of research specifically related to which skills nurses (and patients) should develop for safe and effective distant communication using ICT. |
| Evidence for Practice | Technology is seen as a facilitator (enabling increased accessibility, providing health care that would not be possible in certain situations) and as a strategy to overcome the continuous increase in the demand for care and a shrinking care professional population. | Nurses need to develop specific communication skills to adapt to evolution and new ways of providing care to patients, only possible with education and continuous training programs. |
| Research Recommendations | Research is needed to identify which ICT present the best results and respond effectively to the needs and preferences of both patients and nursing health professionals. | Research is needed for a greater understanding of how patients, families and caretakers perceive distant communication processes while using ICT with health providers and which skills are required to avoid risks. |
3. Discussion
The primary aim of this scoping review was to map the evidence on the use of information and communication technology (ICT) in distant nurse-patient communication. The 10 studies analyzed different types of interactions and presented proof of ICT’s potential. Although many aspects of the results could be discussed, the focus will be to point out specific skills that should be developed by nursing students in training programs to respond to the needs identified in the studies, that help overcome the difficulties felt and guarantee effective distance communication with patients while using ICT.
Communication is a basic and fundamental resource in patient care since it supports all the interactions between the institution, health professionals, and the patient throughout the care journey. It is always present, conveying conscious and unconscious contents, linked to the context in which it occurs (Ramos & Bortagarai, 2012), and can, therefore, interfere with the quality of the care perceived by the patients who are increasingly well-informed and demanding. In the last years, we have assisted a significant paradigm shift, fundamentally altering the traditional processes through which nurses acquire and assess diagnostic data, make clinical decisions, engage with patients and their families, and administer treatments (Martinez & Jones, 2018). The influence of technology on the nature and content of communications gives rise to the possibility of depersonalization of interpersonal relationships, together with sensory and nonverbal limitations (Barbosa & Silva, 2017).
The selected studies reveal many benefits of the use of technologies in nurse-patient communication, but it is also evident that authentic interpersonal relationships are harder to achieve due to the lack of the necessary knowledge and skills to communicate efficiently, with both health professionals and patients, to overcome the difficulties felt in the long-distance interactions using different technology. Nurses insist on the importance of specific professional training to accompany the technical demands and digital evolution. Essential communication skills must be identified, and a specific educational curriculum defined accordingly, to prepare students for the future of digital communication in health. Moscato et al. (2007) claim that one of the strongest predictors of patient satisfaction with telenursing is clarity of communication and suggest that telenursing education programmes should include content that allows them to expand their interpersonal communication skills (Eriksson et al., 2020; Moscato et al., 2007).
The results in this systematic review provide sufficient information to define which specific distance communication skills, using ICT, should be considered in professional learning programs for nurses. Effective distant nurse-patient communication is crucial for creating positive care outcomes; therefore, 1) Nurses should know how to interpret and understand patients’ verbal and non-verbal signals while using technology to make the correct diagnosis. 2) During the consultation, nurses should be able to help the patient gain confidence and communicate in a clear and resolute manner, to avoid mistakes and misconduct in the treatments. 3) Nurses should ensure that all sent and received written messages are expressed and understood with objectivity. 4) Nurses should report and document all the implicit and explicit information about the interventions. 5) Nurses should develop continuous technological and digital knowledge and competencies to keep pace with the digital health transformation and to autonomously understand and overcome constraints related to minor equipment problems and software limitations used in distant communication interactions without the need for an IT team. 6) Nurses should know how to enhance contact while using a video camera (correct projection of voice, adequate light, background, body language, maintain visual contact, etc.) and teach patients how to apply the same techniques for effective communication for both. 7) Nurses should be fully aware of security practices in the use of ICT in communications to guarantee patient safety and avoid risks.
Nurses need the competence to integrate current technologies into their care pathways (Houwelingen et al., 2016). A better understanding of nursing telehealth trustable professional activities (NT-EPAs) and the required competencies can be used by nursing schools that are considering including or expanding telehealth education in their curriculum and contributing to the development of nursing telehealth education. Modern telenursing strategies will necessarily depend on a collaborative, organized, and systematic effort between the various actors of the different levels of health system management (Pimentel et al., 2022). The International Council of Nurses (ICN), in 2023, stated that the nursing profession must contribute to keep pace with the digital transformation to ensure digital health technology is developed and applied in a way that meets the needs of individuals, families, communities, and the health workforce (Navarro-Martinez et al., 2024). Therefore, these health professionals’ knowledge and experience should be considered by organizations and institutions to develop adequate ICT solutions that facilitate and promote effective distance communication without compromising their professional workflow or the health and safety of their patients.
The main limitation of this study is related to the difficulty in obtaining recent data with sufficient evidence of the use of ICT exclusively for distant nurse-patient communication purposes. Most references mention telenursing systems that include access to information geographically distant through mobile applications and Internet of Things devices (eHealth) and electronic medical record systems for patient care management that include communication with other health professionals.
Conclusion
The analysis of the studies in this review showed that in health, distant communication using diverse technology cannot be a substitute for face-to-face interactions, but it can complement them and reduce the need for face-to-face consultations in situations in which providing health care to patients would not be possible. The way nurses and patients communicate together is crucial for creating positive care outcomes, which is the basis for safe care. Technology is seen as having a positive impact on communication, enabling increased accessibility in health care to meet the diverse needs of patients, and is seen as a strategy to overcome the continuous increase in the demand for care and a shrinking care professional population. Despite the difficulties identified, doubts, and reluctance felt to embrace technological solutions in communication, due to limited knowledge of the use of technology, both health professionals and patients acknowledged its benefits and demonstrated a willingness to accept, learn, and adapt to the imposed digital transformations of our time. To overcome most of the listed difficulties and answer to the growing digital demands, specific training programs related to the development of effective communication skills using ICT by nurses with patients were identified and should be considered by nursing schools, lifelong training courses, and health institutions. Further studies should be conducted to elaborate a greater understanding of how patients, families, and caretakers perceive distant communication processes using technology with health providers, identifying the ones that present the best results, and then help ICT companies develop technical and digital solutions that respond effectively to the distant communication needs and preferences of both patients and health professionals.
Author contributions
Conceptualization, R.S.A. and A.M.; data curation, M.P. and R.S.A.; formal analysis, M.P.; funding acquisition, A.M.; investigation, M.P. and R.S.A.; methodology, M.P. and R.S.A.; project administration, M.P. and R.S.A.; resources, M.P., R.S.A. and A.M.; software; M.P. and R.S.A.; supervision, A.M.; validation, A.M.; visualization, M.P. and R.S.A.; writing-original draft, M.P.; writing-review and editing, M.P. and R.S.A.