INTRODUCTION
Palmoplantar pustulosis (PPP) is a chronic and relapsing inflammatory disease of the palms and soles, characterized by the appearance of crops of scattered sterile pustules, in conjunction with erythematous keratotic plaques.1-4It has been classically described as a variant of psoriasis, although some authors nowadays regard it as a separate entity.1-3Concurrent plaque-type psoriasis has been reported in 18%-27% of the patients. PPP seems to be more prevalent in women, and is highly associated with smoking.1,4,5A link between PPP and allergic sensitization has been described.1,4Hereby we report two cases of difficult to treat plantar pustulosis perpetuated by allergic contact dermatitis (ACD).
CASE REPORT
A fifty two year-old woman with a twenty two year history of PPP was referred to our clinic. She also suffered from hidradenitis suppurativa (HS) and was receiving weekly subcutaneous adalimumab (40 mg), with clinical remission of HS and palmar involvement. However, lesions on the soles persisted for more than 6 months after clearing of the palms (Fig. 1. A), even after treatment with oral methotrexate (weekly doses of 20 mg). Subacute eczema of the dorsal surface of both feet was also evident.
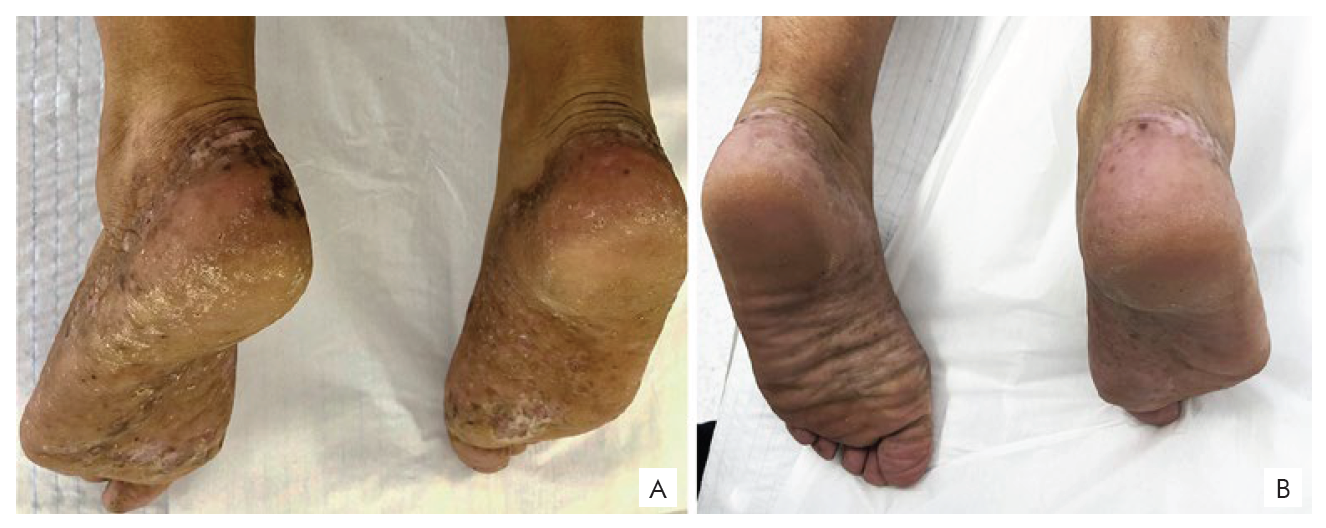
Figure 1 A) Plantar pustulosis with sensitization to cobalt chloride, potassium dichromate and paraphenylenediamine (first patient); B) Clinical response after two months of allergenic eviction (first patient).
The second case refers to a forty eight year-old woman with a fifteen year history of plantar pustulosis unsuccessfully treated with topical clobetasol ointment (the patient refused other treatments).
On both cases microbiological smears disclosed no dermatophytes or bacteria. To exclude a possible concomitant ACD, patch testing was performed with the Portuguese Contact Dermatitis Research group baseline series, alongside with shoe series (BIAL Aristegui). Following the European Society of Contact Dermatitis guidelines, the allergens were applied on the back for 48 hours and readings were performed on day (D) 3 and D7. On both days, positive reactions (2+ to 3+) to cobalt chloride 1% pet, potassium dichromate 0.5% pet and paraphenylenediamine (PPD) 1% pet were observed in the first patient, whereas cobalt chloride 1% pet, potassium dichromate 0.5% pet and nickel sulfate 5% pet were positive in the second. Contact sensitization to potassium dichromate was considered to have current relevance, since it is commonly used by the leather industry, as a tanning agent. Association between sensitization to cobalt and the use of leather shoes has also been shown,6 and it may encompass a current relevance. Leather shoes and leather insoles were commonly worn by the first and the second patient, respectively. PPD sensitization is less likely relevant, although it can be employed in the dyeing process of the shoes and cross-reactive azo dyes may be used to dye socks. Nickel sensitization was considered to have past relevance. Clinical remission was observed after allergenic eviction in both cases after two months of leather eviction (Fig. 1. B).
DISCUSSION
The relationship between PPP and ACD is still a matter of debate.
According to a recent systematic review, concomitant contact sensitization has been shown in 23.5% of 519 patients with PPP and allergen eviction seems to beneficial in most cases, although most of the follow-up data collected refers to metals mainly present in dental amalgams.1 PPP lesions are frequently more resistant to treatment than typical psoriatic plaques.3 To deal with a refractory dermatosis the usual option taken by the clinician is therapeutic optimization, with dosage increase or the addition of alternative agents. However, we highlight the role of ACD in the perpetuation of recalcitrant cases of PPP, probably due to koebnerization triggered by the allergic inflammatory response.1,4Patch testing must be considered in cases of absence of clinical response to treatment. Chromium and cobalt are known metal allergens, and their role in the onset/exacerbation of PPP has been described.1,7If relevant sensitization is found, establishing
measures for allergen eviction is mandatory, since it encompasses the potential to achieve complete remission.1















