A 37-year-old woman with a past medical history of obesity (body mass index 50 kg/m2) and Crohn’s disease (Montreal classification - A2 L2+L4 B1) was referred to our institution for bariatric surgery after several unsuccessful weight loss attempts. The diagnosis of Crohn’s disease was established at age 19 (Fig. 1) and at that time she started therapy with azathioprine and a prednisolone taper. Due to poor control of the disease, the patient underwent several long courses of corticosteroid therapy. At this point, she began to gradually increase her weight. Over the past 4 years, the patient has been on infliximab at 5 mg/kg every 8 weeks, with evidence of clinical and endoscopic remission.
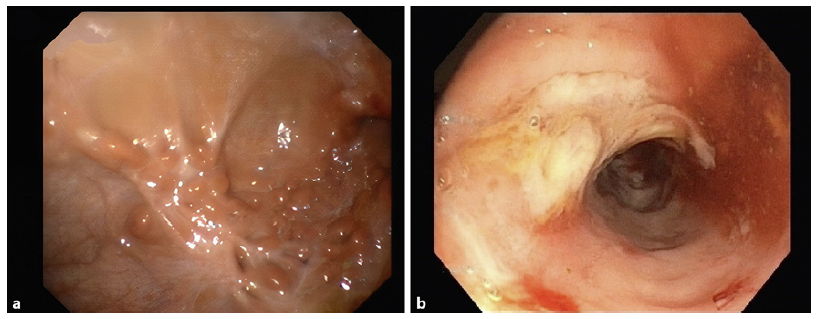
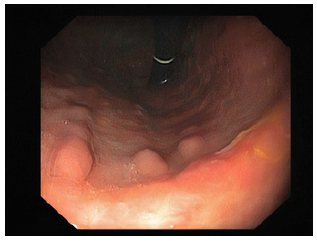
Fig. 1 Endoscopic exams at diagnosis. a Esophagogastroduodenoscopy - stomach with scattered scarring areas and multiple pseudopolyps. b Colonoscopy - congestive and friable colonic mucosa, with scattered erosions and ulcers, interspersed with normal-looking mucosa.
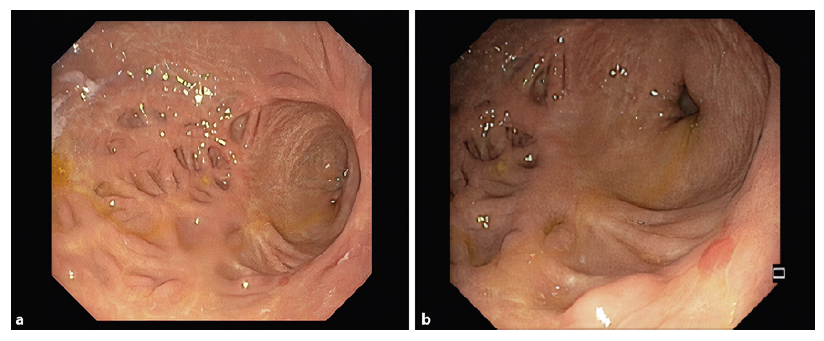
A preoperative esophagogastroduodenoscopy was requested in order to assess the upper gastrointestinal tract for any abnormal findings as well as the presence of Helicobacter pylori (HP) infection. The endoscopy revealed retracted scar tissue in the gastric body (Fig. 2a) and antrum (Fig. 2b), with lesions with a bamboo-joint-like appearance and several pseudopolyps (Fig. 3). The esophagus and duodenum appeared normal. Histopathologic examination of biopsies from the stomach demonstrated mild foveolar hyperplasia and HP-negative chronic gastritis, with no signs of activity. No epithelioid granulomas, glandular atrophy, dysplasia, or signs of malignancy were identified.
The patient underwent a sleeve gastrectomy without complications. The surgical specimen did not reveal any specific sign for inactive Crohn’s disease. Indeed, histopathological evaluation of the surgical specimen showed chronic gastritis and hyperplasia of the foveolar epithelium cells, without active inflammation, granulomas, dysplasia, or signs of malignancy. Five months after the surgery, she has already lost 36 kg and Crohn’s disease remains in remission.
Crohn’s disease is defined by chronic inflammation that may involve any site of the gastrointestinal tract.
Nevertheless, the stomach is rarely the sole or predominant site of Crohn’s disease accounting for less than 0.07% of all cases of gastrointestinal Crohn’s disease [1, 2]. We report a rare case of gastric Crohn’s disease with endoscopic findings consistent with cicatricial mucosa, remarkable for its exuberance. Furthermore, it has been shown that bariatric surgery may be an effective and safe option for weight loss in carefully selected patients with inflammatory bowel disease [3].