Case Report/Case Presentation
This case reports an 80-year-old male patient with significant cardiac comorbidities including hypertension, type 2 diabetes and a previous ischaemic stroke. He reported epigastric pain, absence of passage of flatus and diminished elimination of faeces, within a period of 3 days. On physical examination, he was dehydrated, febrile, the abdomen was distended with hypoactive bowel sounds and a tender epigastric mass, without peritoneal signs.
The blood tests revealed leucocytosis and elevated C-reactive protein. An abdominal computed tomography showed an 11 cm air-filled central structure, apparently originating from the small bowel, described as a closed loop small bowel obstruction (Fig.1).
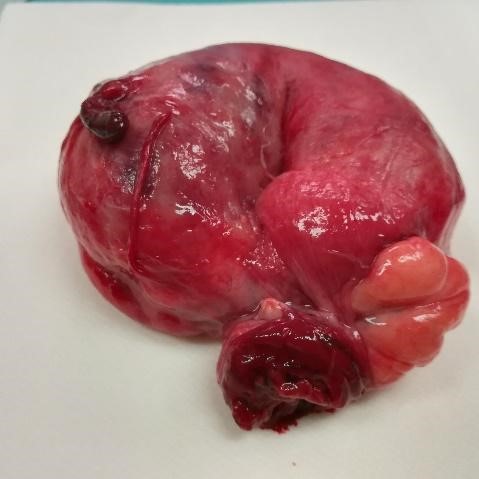
A laparotomy was performed and a large gas-filled diverticulum, at the antimesenteric border of the sigmoid colon, with an epiploon tourniquet at the diverticular neck was found (Fig. 2). It was associated with an extensive diverticulosis of the left colon. Diverticulectomy alone was safely performed (Fig.3).
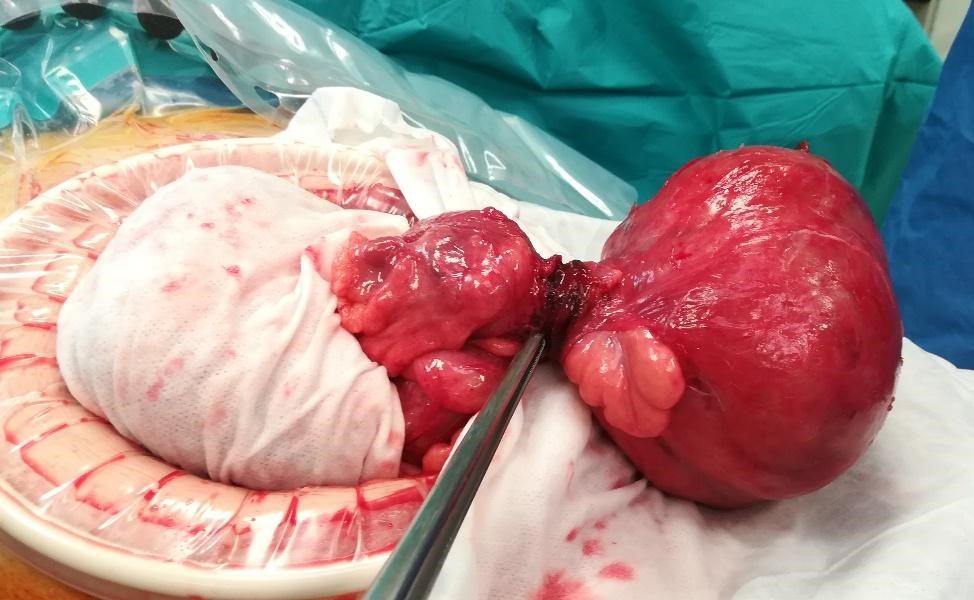
Figure 2: Giant colonic diverticulum, at the antimesenteric border of the sigmoid colon, with an epiploon tourniquet at the diverticular neck
The patient was discharged home after a normal postoperative period of 9 days. During the follow-up period of 6 months, he did not suffer any recurrence.
Discussion/Conclusion
A giant colonic diverticulum (GCD) is a rare complication of the common diverticular disease. Since it was first described in 19461,2, less than 200 cases have been reported in the literature worldwide.
A giant colonic diverticulum is 4 cm or greater in diameter and it can remain asymptomatic for a long period of time, until it reaches 7 cm or more3. In order to explain the size of the diverticula, it is postulated that the fibrous neck above the opening of the diverticulum acts as a one-way valve which allows air entry but not its exit1,2,3,4,5. It has also been attributed to the action of gas-forming organisms1,6. In spite of reports of GCD without additional diverticula, diverticulosis is present in 90% of cases and approximately 81% - 90% involve the sigmoid colon1,2,3,4,5.
Histologically, McNutt described three types of diverticula. Type I is a pseudodiverticulum with an out-pouching of mucosa and submucosa that protrudes through a defect in the colonic wall. Type II is not a diverticulum, but a walled-off abscess cavity due to perforation of a diverticulum that remains in contact with the lumen of the colon; the wall is made of fibrous scar tissue that enlarges to giant size. Type III is a true diverticulum, in which the wall contains all layers of the colonic wall1,2,3,4,5. Type III is the rarest described in reviews, found in only 12% of cases2.
Its presentation is generally non-specific. One third of patients present acutely with abdominal pain1 associated with fever, nausea, vomiting and rectal bleeding. As a chronic or sub-acute manifestation, symptoms include intermittent abdominal discomfort, bloating, and constipation, which may be associated with a palpable and soft abdominal mass, with variations in size. The presence of an intermittently palpable mass is responsible for the designation of ‘phantom tumour’, associated with GCD2,6. Approximately 10% of the patients are asymptomatic, but the mass can be detected either upon examination, or as an air-filled cystic image observed in an imaging procedure1,5. Diagnosis is based predominantly on abdominal computed tomography, which is the most accurate and recommended examination. The CT demonstrates a smooth-walled structure filled with stool and gas, that communicates with the colonic lumen1. Although the rarity of GCD can lead to the misdiagnosis of large bowel volvulus, as seen in the present case report6, other differential diagnoses include a duplication cyst, a giant Meckel’s diverticulum, duodenal diverticula, infected pancreatic pseudocyst and pneumatosis cystoides intestinalis7,8.
Due to their propensity to cause complications, surgical resection is the recommended treatment, even for asymptomatic patients3. The complications range from peritonitis, caused by the perforation of the GCD, abscess formation, intestinal obstruction, volvulus and infarction. The majority of patients are treated with colonic resection with en bloc resection of the diverticulum. However, Hartmann’s procedure and diverticulectomy are also performed. Non-surgical treatments might be indicated for high-risk patients, or those refusing surgery. Percutaneous drainage, stent placement, and antibiotics are typically followed by delayed elective segmental colectomy1,2.
The presented case describes an elderly patient, without previous manifestation of diverticular disease, in which the computed tomography did not reveal the accurate diagnosis. The acute presentation required urgent surgery and revealed a CGD of 11 cm in diameter and not a closed loop small bowel obstruction. Type III is the rarest described in reviews, with a proportion of 12% of cases found. Bearing in mind the age and comorbidities of the patient, diverticulectomy was a safe and adequate choice for this urgent procedure. The patient remained asymptomatic during the follow-up, with no evidence of recurrence.





![2-[18F]-FDG-PET in the Differential Diagnosis between Alzheimer’s Disease and Frontotemporal Dementia](/img/en/next.gif)