Introduction
Dermatological manifestations of COVID-19 (coronavirus disease 2019) are not frequent, and its true incidence is still unknown. We present a case of a patient infected with COVID-19, with dermatological lesions in the acral areas, exhibiting vesicles and pustules on painful and itchy purpuric areas. These were similar to what we commonly refer to in the clinical practice as chilblains (pseudo-chilblains).
With this article we aim to discuss this cutaneous manifestation of COVID-19, helping to better understand the disease and support an early clinical suspicion for cutaneous manifestations.
Case report
Female, 36-year-old. Previously healthy, no prior clinical history. She denies taking any medication or known drug allergies. No family history of interest in this clinical context.
Smoker (15 pack-years), she works as a kindergarten teacher.
She developed COVID-19 infection, with positive detection for viral RNA in the real-time polymerase chain reaction (rt-PCR) test on nasopharyngeal exudate. Symptomatic, with complaints of odynophagia, nasal obstruction, low fever, dry cough, headache, anosmia and ageusia, medicated with paracetamol 1 g po for three days. She accomplished home isolation, with no cohabitants present.
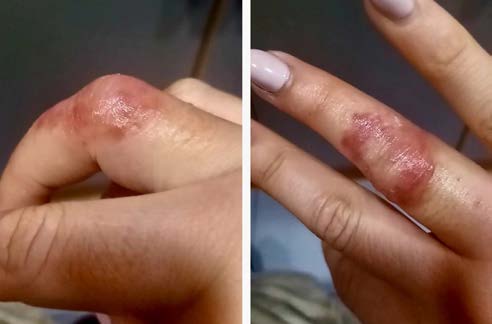
Seven days after the onset of symptoms, she presented with dermatological lesions in the acral areas bilaterally on the hands (4th finger of the right hand and 2nd finger of the left hand). She was referred to the Basic Emergency Service, where erythematous-violaceous papules/vesicles in the extensor dorsal areas of the fingers were observed (Fig. 1). With local inflammatory signs, the lesions were accompanied by a skin rash, redness, edema, local burning sensation, itching and slight pain (Fig. 2). Additionally, she had diffuse erythema in the subungual area of two fingers. She denied exposure to extreme cold or heat.
After requesting joint observation by Dermatology, given the non-existent clinical history of the pattern in this patient and not identifying any other triggering factor, skin lesions secondary to COVID-19 infection (pseudo-chilblains) were diagnosed. The patient underwent symptomatic treatment with pentoxifylline 400 mg po for 5 days. All lesions resolved completely within ten days, with no subsequent sequelae. There was no need for a skin biopsy.
Discussion
Since COVID-19, a clinical syndrome caused by the new coronavirus, named SARS-CoV-2 (severe acute respiratory syndrome, coronavirus 2) was reported in Wuhan, China, in December 2019, 107 million people have been infected worldwide and more than 2.3 million deaths have occurred (data obtained on February 12th 2021).1
The high rate of infection, low virulence and asymptomatic transmission of the disease promoted its rapid spread to various regions of the world, leading to the pandemic decreed by the World Health Organization (WHO) on 11th March 2020.
The lungs are the main target organ of infection, with symptoms ranging from a common cold to severe pneumonia with breathing difficulty, in addition to the involvement of several organs or systems, leading to sepsis and septic shock with multiorganic dysfunction.2) Most described cases are asymptomatic, mild or moderate.
The dermatological manifestations of COVID-19 are uncommon, they seem to be similar to those found in other diseases of viral etiology, and its true incidence is still unknown. The first description of cutaneous findings associated with COVID-19 was made by Recalcati,3 who reported skin rashes consistent with erythematous-violet macules and papules in the acral regions, with possible formation of blisters, in 20% of patients admitted to a hospital in Italy.
Five patterns of dermatological manifestations of COVID-19 have been described, classified into maculopapular eruptions (47%), erythema with vesicles or pustules in acral areas (pseudo-chilblains) (19%), urticarial lesions (19%), other vesicular eruptions (9%) and livedo or necrosis (6%).(4)
In this article, we describe a clinical case of a patient with dermatological lesions in the acral areas, adopting the appearance of vesicles or pustules, with asymmetrical, painful and itchy purple areas. These were accompanied by a burning sensation in the affected places and were similar to what we commonly refer to in the clinical practice as chilblains. These lesions frequently affect younger patients4 and are usually self-limiting or resolved with a symptomatic therapeutic course.
The pattern of pseudo-chilblains is characterized by an appearance of purpuric lesions on the hands and/or feet, with a late development in the evolution of COVID-19 disease. Fifty nine percent of patients appear with these lesions after all other symptoms.4 The severity of COVID-19 disease tends to be less acute in patients with this type of skin lesions, with a course of mild to moderate severity (without the need for hospital admission). Only 1.4% of patients with pseudo-chilblains associated with COVID-19 had a history of previous chilblains, and there seems to be a trend towards the presence of family clusters.4
Several studies have shown that the COVID-19 virus enters cells through angiotensin-converting enzyme 2 (ACE2) receptors, which are widely expressed in the vascular endothelium, respiratory epithelium, alveolar monocytes and macrophages.5 During the course of the disease, the virus generates a widespread damage, through a secondary viremia, against target organs that express ACE2 receptors, namely the heart, kidneys, gastrointestinal tract and distal vasculature.6 This viral dissemination process occurs mainly around the second week after the onset of the disease.
It has been observed in several organs of COVID-19 patients, a pathophysiological process of degeneration and necrosis of parenchymal cells, vasoconstriction and formation of hyaline microthrombi in small vessels.7 This underlying micro-ischemic process may be the pathophysiological mechanism in cases similar to that of the described patient.
In conclusion, attention should be paid to the fact that COVID-19 can be asymptomatic, from a respiratory point of view, up to 14 days after infection, and it is possible that skin manifestations may serve as an indicator of the disease.8