Imagens Médicas
Uma Queimadura Solar Bizarra
1. Serviço de Medicina Interna, Hospital Distrital da Figueira da Foz, EPE; Figueira da Foz, Portugal.
2. Serviço de Dermatologia, Hospital Distrital da Figueira da Foz, EPE; Figueira da Foz, Portugal.
Abstract
Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome is a rare, complex, potentially life-threatening, drug - induced hypersensitivity reaction that often includes skin eruption, hematologic abnormalities, lymphadenopathy and organ involvement.
The authors present a clinical case of a 79-year-old Caucasian man presented to the emergency department due to a burn-in chest and abdomen after vacation and solar exposure without sunscreen protection. He has been taking the following medication for the past two years: perindopril + amlodipine, simvastatin and allopurinol. He had also an itchy maculopapular erythema on his back and confluent erythematous eruption on the lower limbs, similar to purpuric lesions. Laboratory data demonstrated a lymphopenia and elevated liver enzymes. According to RegiSCAR score, this case is classified as probable DRESS syndrome. Allopurinol was discontinued immediately, and the patient started prednisolone. He was observed one month later, with progressive improvement of the lesions.
Diagnosing DRESS syndrome can be challenging but should be suspected in a patient who receives a high-risk medication and presents with characteristic symptoms. Supportive therapy and prompt withdrawal of the culprit drug is the primary treatment. In the case presented, the patient complained of a burn but had a toxiderma caused by allopurinol which bizarrely manifested itself.
Keywords: Allopurinol/adverse effects; Drug Hypersensitivity Syndrome
Resumo
A síndrome de DRESS (drug rash with eosinophlia and systemic symptoms) trata-se de uma reação de hipersensibilidade induzida por fármacos, rara, complexa e potencialmente fatal. Geralmente evolui com erupção cutânea, alterações hematológicas, linfadenopatia, com envolvimento de órgãos.
Os autores apresentam o caso clínico de um homem caucasiano de 79 anos que deu entrada no serviço de urgência devido a uma queimadura no tórax e abdómen após férias e exposição solar sem proteção solar. A sua medicação habitual há 2 anos é: perindopril+amlodipina, sinvastatina e alopurinol. Apresentava também um eritema maculopapular pruriginoso no dorso e erupção eritematosa confluente nos membros inferiores, semelhantes a lesões purpúricas.
Dados laboratoriais demonstraram linfopenia e elevação das enzimas hepáticas. De acordo com o score RegiSCAR, este caso classifica-se como provável síndrome de DRESS. O alopurinol foi suspenso imediatamente e foi iniciada prednisolona. Foi observado um mês depois, com melhoria progressiva das lesões. O diagnóstico da síndrome de DRESS é desafiante e deve-se suspeitar do seu diagnóstico num doente sob fármacos de alto risco com clínica característica. A abordagem inicial consiste no tratamento de suporte e na suspensão imediata do fármaco. No caso apresentado, o doente queixava-se de queimadura, mas apresentava uma toxidermia por alopurinol que se manifestou de forma bizarra.
Palavras-chave: Alopurinol/efeitos adversos; Síndrome de Hipersensibilidade a Medicamentos
A 79-year-old Caucasian man presented to the emergency department due to a burn-in chest and abdomen after vacation and solar exposure without sunscreen protection.
His past medical history includes hypertension, dyslipidemia and hyperuricemia. He has been taking the following medication for the past two years: perindopril + amlodipine, simvastatin and allopurinol.
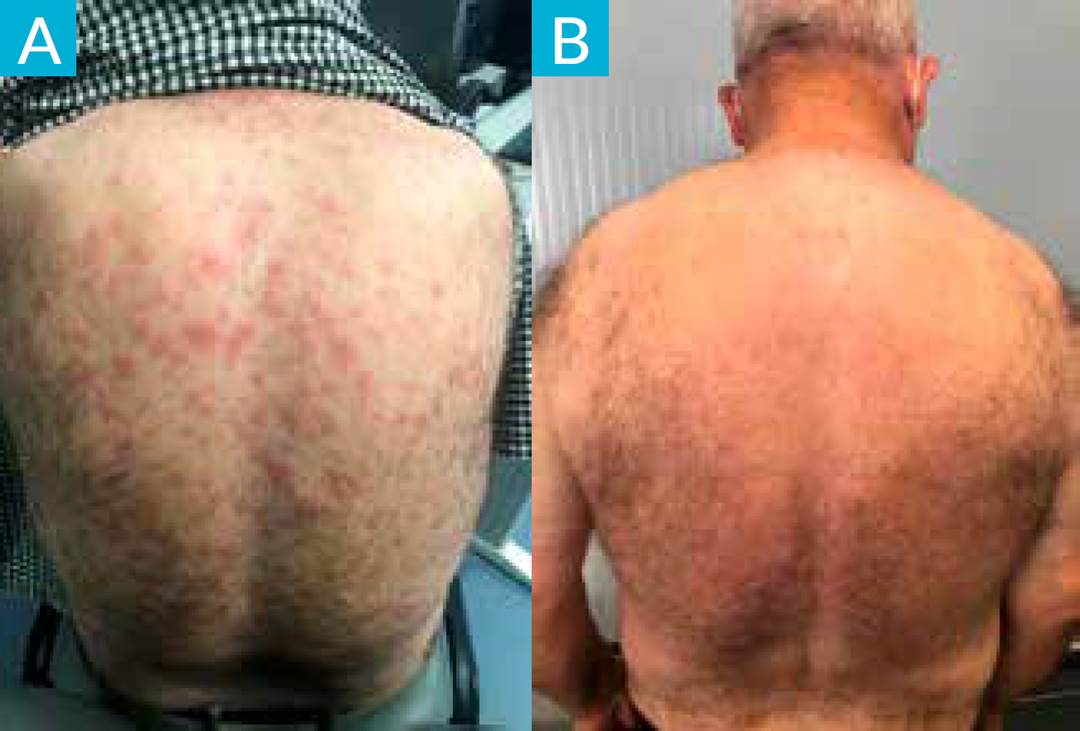
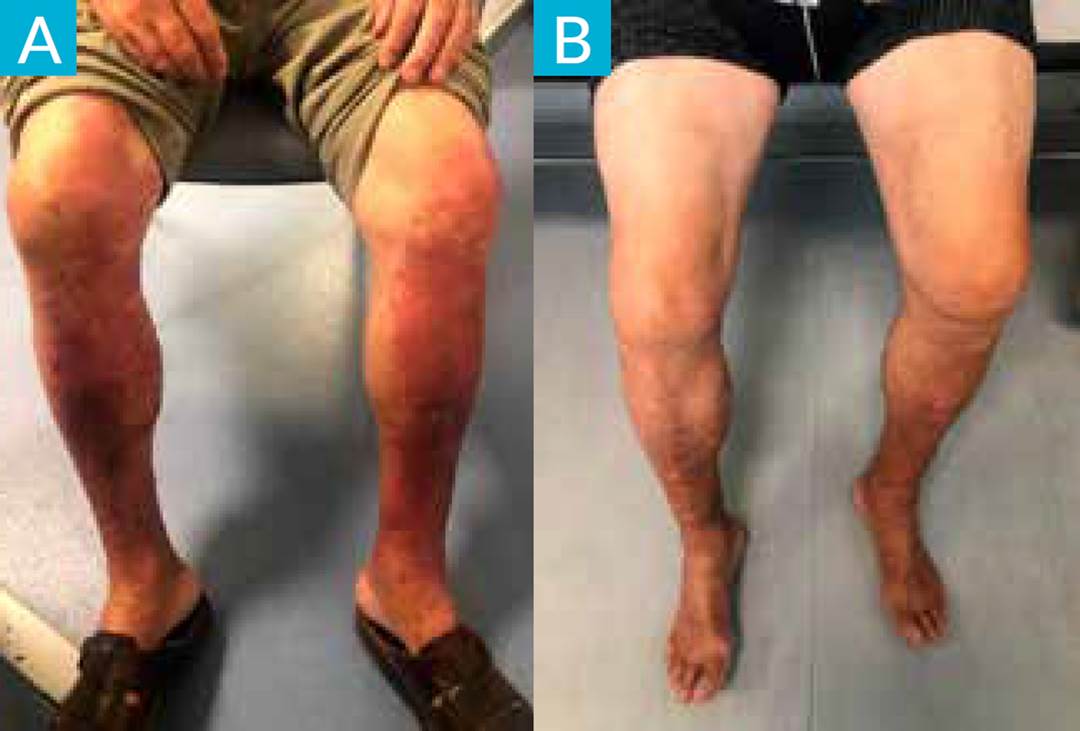
On initial examination, his temperature was 37ºC with vitals within normal limits. His cardiopulmonary and abdominal exams were unremarkable. He had also an itchy maculopapular erythema on his back (Fig. 1A) and confluent erythematous eruption on the lower limbs, similar to purpuric lesions (Fig. 2A).
Laboratory data demonstrated a lymphopenia, hemoglobin and platelets within normal limits, sedimentation rate 40 mm/1 h (baseline < 13), creatine phosphokinase 724 units/L (baseline < 174), C-reactive protein 60.12 mg/L (baseline < 5) and elevated liver enzymes with AST 59 units/L (baseline 0-38), ALT 72 units/L (baseline 0-41) and LDH 384 units/L (baseline < 250).
Chest X-ray demonstrated no acute processes. Abdominal ultrasound demonstrated no abnormalities.
Viral serologies (hepatitis A/B/C, EBV, CMV, HSV, VZV and HHV-6) and autoimmune studies were normal as well as serum electrolytes and thyroid function tests.
According to RegiSCAR score, this case is classified as probable DRESS syndrome (5 points).
Allopurinol was discontinued immediately, and the patient started prednisolone 40 mg/day for 1 week, in a slow weaning scheme. He was observed one month later, with progressive improvement of the lesions (Figs. 1B and 2B).
Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome is a rare, complex, potentially life-threatening, drug - induced hypersensitivity reaction that often includes skin eruption, hematologic abnormalities, lymphadenopathy and organ involvement.1-3
The drugs mainly implicated are allopurinol and anticonvulsants, followed by antibiotics.1-4
The onset of DRESS occurs within the first two months after the introduction of the culprit drug and is characterized by prodromal symptoms like fever or lymphadenopathy.4) The reaction usually lasts more than 15 days with several flare-ups.4
The pathogenesis of this syndrome is hypothesized to be secondary to an accumulation of toxic drug metabolites due to various enzymatic deficiencies.1,2,5
The typical initial skin lesion is a morbilliform or maculopapular eruption.5 Subsequently, it progresses to a diffuse, confluent and more infiltrated erythema and edema, but also purpuric lesions.1-5
The liver is the most common organ affected in this syndrome.5) Liver involvement is generally mild with rare progression to fulminant hepatic failure.5) Hematological findings are also commonly seen in DRESS syndrome, with eosinophilia being the most common manifestation.5) However, its absence does not exclude the diagnosis.5
Diagnosis is often difficult. So, several diagnostic criteria have been developed, the score of the RegiSCAR group.4
Supportive therapy and prompt withdrawal of the culprit drug is the primary treatment. Discontinuation of the culprit drug is sometimes sufficient to achieve resolution of the disease.1-4
To define the culprit drug, it is important to consider all drugs introduced in therapy in the 3-8 weeks preceding the onset of symptoms, but this can be complicated in the case of multiple therapies or a long latency between the start of therapy and the onset of the reaction.4
In the case presented, the patient complained of a burn but had a toxiderma caused by allopurinol which bizarrely manifested itself.
Agradecimento/Acknowledgment
Margarida Gaudêncio - Assistente Hospitalar de Medicina Interna; Instituto Português de Oncologia Coimbra; Coimbra, Portugal.
Referências
1. Pichler W Drug hypersensitivity: classification and clinical features. Uptodate. [Access September 2021] Available from: Available from: https://www.uptodate.com/contents/drug-hypersensitivity-classification-and-clinical-features
.
[ Links ]
2. Kasper DL, Fauci AS, Hauser SL, Longo DL, Jameson JL, Loscalzo J. Harrison's Principles of Internal Medicine. 20th ed. New York: McGraw Hill Education; 2021.
[ Links ]
3. Cabañas R, Ramírez E, Sendagorta E, Alamar R, Barranco R, Blanca-López N, et al. Spanish Guidelines for Diagnosis, Management, Treatment, and Prevention of DRESS Syndrome. J Investig Allergol Clin Immunol. 2020;30:229-53. doi: 10.18176/jiaci.0480.
[ Links ]
4. Toniato A, Gamba C, Schroeder JW, Fabbri V, Bernal Ortiz SV, Borgonovo L, et al. Role of Multiple Comorbidities and Therapies in Conditioning the Clinical Severity of DRESS: A Mono-Center Retrospective Study of 25 Cases. Int J Mol Sci. 2021;22:7072. doi: 10.3390/ijms22137072.
[ Links ]
5. Hakim C, Melitas C, Nguyen E, Ngo K. Atypical Manifestation of DRESS Syndrome. Case Rep Gastrointest Med. 2020;2020:6863582. doi: 10.1155/2020/6863582.
[ Links ]