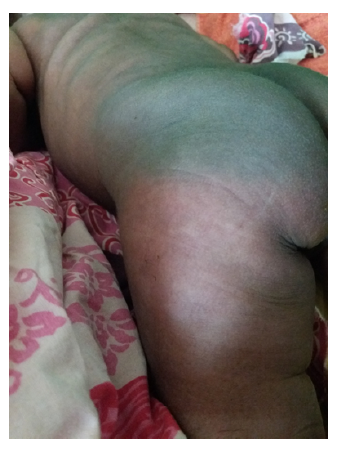
A term female infant weighing 4190 g was born by cesarean section due to prolonged labor and meconium-stained fluid at the Bafatá Regional Hospital, Guinea-Bissau. Bag-mask ventilation was required and Apgar scores were six and eight at 1 and 5 minutes, respectively. Due to unavailability of the only neonatal resuscitation table with heating, the newborn remained with the mother. Considering the risk of sepsis, ampicillin and gentamicin were started. On the third day of life, the newborn presented with multiple firm subcutaneous nodules and plaques associated with erythema in the axillary region, posterior trunk, buttocks, and thighs (Figures 1and2), as well as irritability.
What is your diagnosis?
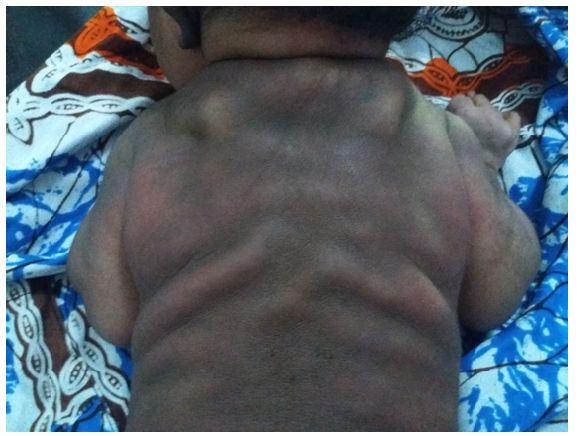
Figure 1 Firm nodules in the upper region of the posterior trunk () and erythematous plaques in the axillary region and posterior trunk.
Diagnosis
Subcutaneous fat necrosis
Considering the risk factors and clinical presentation with typical manifestations, the diagnosis of subcutaneous fat necrosis (SCFN) was established. In the clinical setting of a regional hospital in Guinea-Bissau, the availability of blood tests is very limited and there is no ultrasound imaging support. Therefore, blood calcium levels could not be monitored, and the clinical advice was to encourage hyperhydration through breastfeeding. As blood cultures were not available, and given the risk of sepsis, the newborn completed a seven-day course of antibiotics. She was discharged on the tenth day of life after clinical improvement, with lesions of low extent, almost imperceptible erythema, and no signs of irritability. On follow-up, one week later, the newborn was re-evaluated and showed only induration of the skin in the affected areas without erythema.
Discussion
SCFN of the newborn is a relatively rare condition and clinicians are becoming increasingly aware of its diagnosis and correct evaluation.1 It has been widely described in the literature as a mostly benign and self-limited condition, which was confirmed by the present clinical case.2,3 It usually presents with multiple firm subcutaneous nodules or plaques that may be associated with erythema on the cheeks, buttocks, back, or limbs, often sparing the anterior trunk.3,4 Some of the established risk factors include exposure to hypoxia, hypothermia, meconium aspiration, sepsis, gestational diabetes, and pre-eclampsia.2,4,5) The differential diagnosis should include sclerema neonatorum, which is usually generalized and characterized by hardening of the skin accompanied by respiratory and motor difficulties and is often associated with a poor prognosis.2,4
The exuberance of the present case is uncommon and its management can be challenging without adequate resources. The diagnosis can be made through clinical presentation, medical history, and course of the disease. Possible complications, especially hypercalcemia, should always be kept in mind, as the condition can evolve to calcification, including nephrocalcinosis and nephrolithiasis.2,4 Due to the risk of hypercalcemia, caution should be exercised with vitamin D supplementation (especially where it is routine, which is not the case in Guinea-Bissau), suspending it until SCFN resolution. Nonetheless, most cases resolve spontaneously without relevant long-term sequelae.1)
In conclusion, this case highlights how prompt clinical diagnosis allows for more attentive clinical surveillance for possible complications. Furthermore, clinicians should always strive for the most accurate diagnosis, even in the absence of technological medical resources in low-resource settings such as the one considered here.
Take-home messages
SCFN is a rare and often self-limited condition.
In low-resource settings, surveillance and management of major SCFN complications, namely hypercalcemia, may be difficult, but prompt diagnosis is crucial to provide appropriate clinical management with available resources.
Spontaneous SCFN resolution without long-term sequelae is the most common outcome.