Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
GE-Portuguese Journal of Gastroenterology
versión impresa ISSN 2341-4545
GE Port J Gastroenterol vol.27 no.2 Lisboa abr. 2020
https://doi.org/10.1159/000501401
ENDOSCOPIC SNAPSHOT
Tunneling Endoscopic Technique Moving through Zenkers Diverticulum
Tunelização da submucosa aplicada ao divertículo de Zenker
Margarida Flor de Lima, Nuno Nunes, Vera Costa Santos, Maria Antónia Duarte
Gastroenterology Department, Hospital do Divino Espírito Santo de Ponta Delgada, Ponta Delgada, Portugal
* Corresponding author.
Keywords: Zenkers diverticulum, Submucosal tunneling technique, Dysphagia
Palavras-Chave: Divertículo de Zenker, Técnica de tunelização da submucosa, Disfagiaativa
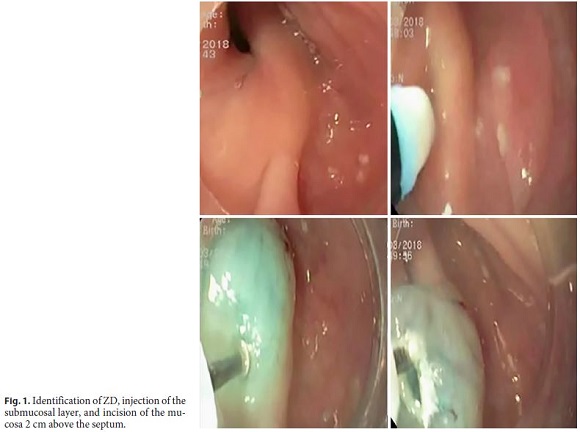
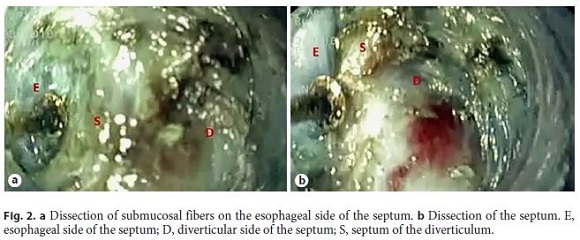
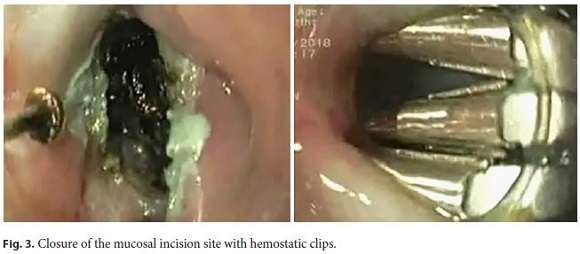
A 79-year-old male patient presents with intermittent dysphagia to solids, regurgitation, and halitosis. The patient had undergone a Zenkers diverticulum (ZD) septum division 6 years earlier, with recurrence of symptoms over the past 2 years. An upper digestive endoscopy revealed residual diverticulum of approximately 2 cm. A submucosal tunneling endoscopic septum division was performed under general anesthesia with endotracheal intubation, using a transparent cap (DH28GR; Fujifilm, Tokyo, Japan) attached to the tip of the gastroscope and insufflation with carbon dioxide. The submucosa was injected 2 cm above the septum, and a longitudinal mucosal incision of 1 cm was made at the tunnel entrance (Fig. 1). A submucosal longitudinal tunnel was created between the mucosal and muscular layers at both sides of the septum (Fig. 2), using a T-Type Hybrid-Knife® (Erbe Elektromedizin, Tübingen, Germany), followed by the dissection of the cricopharyngeal muscle fibers until the normal esophageal muscle was reached. Closure of the mucosal incision was made with hemostatic clips (InstinctTM; Cook Medical, Bloomington, IN, USA) (Fig. 3). The procedure lasted 64 min. There were no adverse events observed, and the patient started liquid diet 24 h later. Intravenous antibiotics were administered before the procedure and were continued for 2 days postoperatively. Proton-pump inhibitor treatment was initiated. The patient was discharged 48 h after the procedure. After 8 months, there was complete resolution of the initial symptoms.
ZD is a rare clinical finding, often manifested by symptoms such as dysphagia and regurgitation. If symptomatic, local treatment of ZD is recommended [1]. The development of several flexible endoscopic techniques demonstrates variable success rates and a recurrence rate of at least 10%, associated with the incomplete dissection of the diverticulum [2].
The tunneling endoscopic technique, after being developed for the treatment of achalasia, has been applied to other areas of intervention such as ZD [3, 4]. The tunneling technique aims to provide a complete myotomy of the septum, maintaining the mucosal integrity and potentially reducing the recurrence rate, although its efficacy is still restricted to case reports and small series. This method is also limited by local expertise. Further studies are needed before general application [4, 5].
References
1 Law R, Katzka DA, Baron TH. Zenkers Diverticulum. Clin Gastroenterol Hepatol. 2014 Nov;12(11):1773–82.
2 Ishaq S, Sultan H, Siau K, Kuwai T, Mulder CJ, Neumann H. New and emerging techniques for endoscopic treatment of Zenkers diverticulum: state-of-the-art review. Dig Endosc. 2018 Jul;30(4):449–60.
3 Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, et al. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010 Apr;42(4):265–71.
4 Li QL, Chen WF, Zhang XC, Cai MY, Zhang YQ, Hu JW, et al. Submucosal tunneling endoscopic septum division: a novel technique for treating Zenkers diverticulum. Gastroenterology. 2016 Dec;151(6):1071–4.
5 Brewer Gutierrez OI, Moran R, Yang J, Sanaei O, Kalloo AN, Kumbhari V, et al. Successful single-session cricopharyngeal and Zenkers diverticulum peroral endoscopic myotomy. Endoscopy. 2018 Aug;50(8):E220–1.
Statement of Ethics
This study did not require informed consent nor review/approval by the appropriate ethics committee.
Disclosure Statement
The authors have no conflicts of interest to declare.
* Corresponding author.
Margarida Flor de Lima
Gastroenterology Department, Hospital do Divino Espírito Santo de
Ponta Delgada, Avenida D. Manuel I, Matriz
PT–9500-370 Ponta Delgada (Portugal)
E-Mail margaridaflordelima@hotmail.com
Received: February 10, 2019; Accepted after revision: May 14, 2019














