Description
The intrauterine device is the most used long-acting reversible contraceptive method, mainly due to its high efficiency, safety, and user-independence. The levonorgestrel releasing intrauterine device (LNG-IUD) offers additional therapeutic advantages for managing abnormal uterine bleeding. Complications are rare and occur most frequently at the time of insertion; however, they can come up at any point of its use. Malposition has been stated to occur in up to 10 percent of women, while perforation has been reported for 1 in 1000 cases1,2. Migration without previous partial or complete perforation at the time of insertion is considered rare, and has been attributed to spontaneous uterine contractions, bowel peristalsis and bladder contractions3.Recent consensus opinion states that the most common migration mechanism consists in the device being forced into the myometrium at time of insertion1.
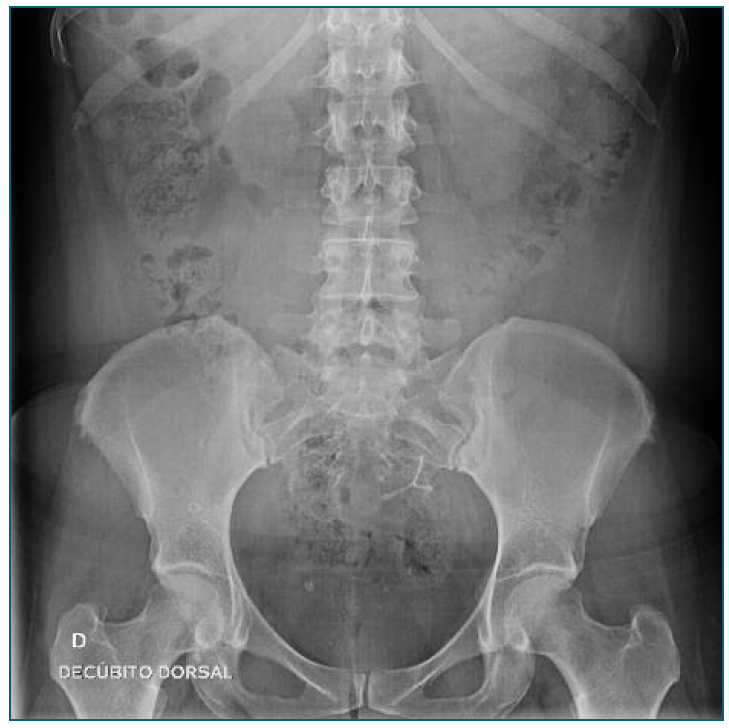
The authors report the case of a woman in her early 30s, gravida 4 para 2, referred to our centre due to abnormal uterine bleeding. The patient had an LNG-IUD inserted 3 years prior and she recalled the insertion as uneventful. At gynaecologic examination, the strings of the device could not be found. A transvaginal ultrasound confirmed the absence of the intrauterine device in situ and an abdominal x-ray showed the presence of the device intra-abdominally (figure 1). Laparoscopic removal was accepted by the patient. Intraoperatively, the LNG-IUD body was identified within the abdominal cavity, emerging from the uterine fundus adjacent to the left uterine horn, with the both strings entirely wi-thin the abdominal cavity, attached to the device and lying in the pouch of Douglas; unexpectedly, both LNG-IUD arms were intramyometrial (figure 2). The surgical removal of the device was achieved using bipolar energy, cut, and traction. The patient was discharged on the first postoperative day and was followed up six weeks after, with no recurrence of her symptoms.
Although the exact timing of uterine perforation cannot be accurately defined, the inverted positioning of the device suggests the occurrence of an intrauterine inversion, followed by perforation and migration. This mechanism excludes the moment of the insertion as the event leading to the perforation. Our case em-phasises that the mechanisms of uterine perforation and migration of intrauterine devices are not completely understood. To our knowledge, this is the first case describing uterine perforation through a device’s lower extremity, in a 180o inverted position. We believe that regular ultrasound follow-up is important to identify IUD malposition at an early stage.