INTRODUCTION
Iodine is an essential micronutrient to the normal functioning of the human body and its metabolism. Concurrently, this micronutrient is only present in small amounts, almost exclusively in the thyroid gland and enables the synthesis of thyroid hormones, one of the greatest moderators of cell metabolism and organ development (1, 2).
In 2007, the World Health Organization found that iodine deficiency remains a significant public health problem in Europe, despite its increased awareness. Salt iodization was unveiled as a solution, currently being the main preventive strategy to tackle iodine deficiency disorders. Its success is based on the implementation of iodised salt (IS) by the general population, and most notably, by the most susceptible groups to iodine deficiency disorders, like pregnant woman and children (1 - 3).
Studies performed in the Autonomous Regions of the Azores showed a significant lack of iodine intake for children and pregnant women. It was shown that 78% of Azorean children had an insufficient supply of iodine, attaining greater significance when compared to Mainland Portugal values (only 47% of children had iodine insufficiency), thus demonstrating the need of this micronutrient in this region (4 -6).This led to an increased awareness by the Autonomous Region of the Azores and its health institutions, which prompted the enlighten of the population on the benefits of the consumption of IS (4). To achieve this goal, health care professionals raised awareness through patient care visits and communication channels. These measures started to be implemented in the region in 2014 and 2015. The Government of the Azores implemented a broadcasting of 37 seconds, explaining the health implications of iodine deficiency (particularly in pregnancy and child development), recommending the consumption of iodine rich foods, and highlighting the importance of replacing non-iodised salt by IS. This broadcast was transmitted in the Azorean broadcaster RTP Açores, in order to specifically target the Azorean population. Awareness in patient care visits was mainly performed in health centers and consisted of a more individualized approach performed by health care workers (physicians, nutritionists, nurses, etc.). In these visits, iodine deficiency and IS's role and benefits were discussed with the patients with assistance from other educational materials (for example, pamphlets) (7).
One of the greatest steps instigated to improve the supply of iodine was the implementation of a government protocol that replaced non-iodised salt by IS, in all regional public administration services’ canteen/bar service, being public schools meals one of the main targets (8). Another measure enforced by the government was the free distribution of iodine supplements by primary care health centers to pregnant/breastfeeding women (9).
Despite most efforts have been made in the following years after implementation of these measures, some of them are still active today, mainly the utilization of IS in canteen/bar service and the free distribution of iodine supplements to pregnant/breastfeeding women. In a 2020 study conducted in São Miguel Island, Azores, it was observed a significant reduction in iodine deficiency in schoolchildren and pregnant women. Some of these results were attributed to the implementation of IS in Azorean houses and canteens of all public schools (10, 11). These efforts were directed at all Azorean population, including Faial Island’s population, and its effectiveness has yet to be determined.
METHODOLOGY
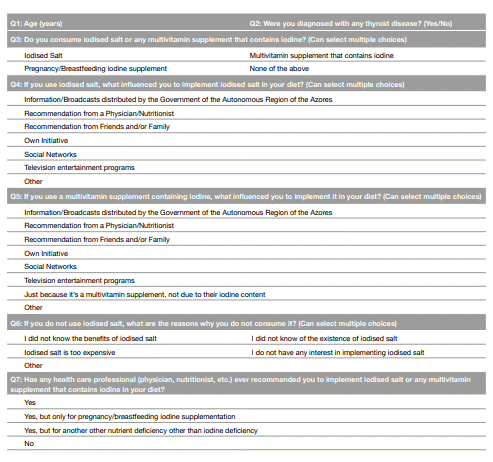
An observational and cross-sectional study was conducted, comprising all the individuals who presented themselves, in person, to the Unidade de Saúde da Ilha do Faial (USIF) for physician/nursing appointments or administrative procedures and the employees who reported to service at the USIF, from November 9th to November 14th, 2020. All individuals who were deprived of their autonomy and individuals who were not interested in participating in the study were excluded. The information was collected through the implementation of a questionnaire comprising questions on iodine consumption (IS or multivitamin supplements containing iodine ((MSCI)) and their reasons behind this implementation or non-implementation. Other questions such as age, personal history of thyroid disease and whether a health care professional recommended the use of IS or MSCI were assessed (Appendix 1). All the individuals who agreed to participate in the study were required to complete an informed consent form. Questionnaire answers were inserted in an anonymized database to preserve anonymity. Database management, statistical analysis and graphics was conducted using Microsoft Office Excel (Microsoft Office Excel for Windows, Version 16.23) and IBM Statistical Package for the Social Sciences (SPSS Statistics for Windows, Version 27.0; NY, USA). Statistical analysis consisted in descriptive analysis of the results, applying the chi-square test to compare variables and calculation of the odds ratio when adequate. Approval was obtained by the Ethics Committee of Unidade de Saúde da Ilha do Faial and from the Ethics Committee of Faculdade de Medicina da Universidade de Coimbra.
RESULTS
A total of 128 people were eligible, where 102 agreed to participate, translating in a 79.7% response rate to the questionnaire. Two individuals were excluded due to incorrect filling of questionnaire and/ or questionnaire filling with conflicting information, translating into a total of 100 eligible questionnaires for analysis. 49 individuals claimed to use IS in their diet. The majority (n=47; 47%) declared to only use IS, 1 declared to use IS and a MSCI and 1 declared to use IS and pregnancy/ breastfeeding iodine supplementation (PBIS). 51 individuals claimed to not use IS, wherein 4 claimed to only use a MSCI. Age of responders varied between 18 and 86 years of age with a mean age of 49,81 years. IS consumption was analyzed according to each considered age group (Figure 1). 19 participants (19%) had a diagnosis of thyroid disease, where 10 (52.63%) stated the use of IS in their diet. In the group of 49 individuals that used IS, the major factor for its implementation was the recommendation from a physician and/or a nutritionist (n=18; 36.7%).

Figure 1 : Age distribution (years) according to the total number of participants and the number of participants that use and that do not use IS in their diets
This was followed by implementing IS by their own initiative (n=15; 30.6%). The information/broadcasts distributed by the Government of the Autonomous Region of the Azores influenced 12 individuals (24.5%) to use IS. Despite these being the main stated reasons for IS consumption, there were also other influencing factors (Table 1).
A total of 51 individuals denied using IS in their diets. When questioned about the reasons for its non-consumption, most participants responded that they were not aware about the existence of IS (n=21; 41.2%) and some did not know its benefits (n=11; 21.6%). Despite these being the main stated reasons for IS non-consumption, there were also other influencing factors (Table 2). 5 individuals claimed to take a MSCI, with only one of them (20%) stating to also use IS. 4 participants (80%) responded that they use this multivitamin supplement for their general health benefits and 1 participant (20%) did not specify the reason. Only 1 individual (1%) claimed to be taking pregnancy/ breastfeeding iodine supplement at the time of questionnaire filling. That individual also stated to consume IS in their diet. Of the 100 individuals in this study, 28 (28%) stated that a health care professional (physician, nutritionist, etc.) has recommended them the implementation of IS or a MSCI in their diets and 6 (6%) have been recommended only for PBIS. The remaining 66 (66%) individuals said to have never been recommended to implement IS or a MSCI in their diets. No one (n=0) was recommended to implement a MSCI for another nutrient deficiency besides iodine deficiency. Of the 28 individuals that receives a recommendation, 23 (82.14%) used IS in their diet (Table 3). Regarding
Table 1: Percentage and frequency of each answer to the question “If you use iodised salt, what influenced you to implement iodised salt in your diet?”

Table 2: Percentage and frequency of each answer to the question “If you do not use iodised salt, are the reasons why you do not consume it?”

Table 3: Usage of iodised salt in diet according to the presence of a recommendation by a health care professional (physician, nutritionist, etc.) to implement iodised salt or any multivitamin supplement that contains iodine
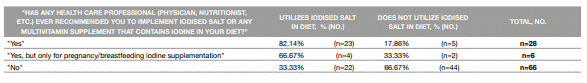
the individuals that have a diagnosis of thyroid disease (n=19; 19%), 7 (36.84%) said to have been recommended to implement IS or a MSCI in their diet, with 6 of those (78.71%) using IS. All the patients that stated “I did not know the benefits of iodised salt” (n=11; 100%), said to not have been recommended to implement IS or a MSCI. The chi-square test proved the existence of an association between presence of a health care professional (physician, nutritionist, etc.) recommendation to implement IS or a MSCI in an individual’s diet (excluding PBIS) and the consumption of IS (p<0.001). Further analysis through odds ratio calculation has shown that individuals who had a recommendation by a health care professional (physician, nutritionist, etc.) to implement IS or a MSCI (excluding PBIS) are 8 times more likely to use IS in their diet (OR=8,138; CI 95% (2,764;23,967)). There were no other variants in this study that demonstrated a statistically significant correlation (p<0.05) with IS consumption.
DISCUSSION OF THE RESULTS
Even though, the effectiveness of measures designed to raise awareness on the importance of iodine in health is still under study, the tackle on iodine deficiency has made a tremendous evolution. This was achieve, not only because of government’s implemented efforts but also because of the population’s acknowledgment of this healthcare problem and their favorable response to these measures (1, 12-16). Of the countries that have recorded data on the consumption of IS, only 27.6% globally and 22.5% in Europe, have attained the goal of a minimum of 90% of households consuming adequately IS (15-40 mg iodine kg-1). As such, although some progress has been made, the road ahead is still long (1, 12, 15, 17, 18).
Unfortunately, only 49% of participants in our sample stated to supplement their diet with IS, which is far from the 90% goal, revealing that, even though studies show promising results, there is still an information gap between the general population and the government, "Information/Broadcasts distributed by the Goverment of theAutonomous Region of the Azores" 24.5% (n=12) organizations and health care workers (11). This is also translated by the fact that, most of participants who do not consume IS do not know about its existence or benefits, contrasting with studies in which the population showed greater knowledge about the topic and displaying higher IS consumption (13, 14).
Interestingly, contrary to some regions/countries where lack of use of IS correlates with its shortage, unavailable widespread sale and a higher cost of IS, these were not influential points in our population (13, 19 - 21). The efforts for awareness and intervention encouraging the increase of consumption of IS performed through personalized population approaches has been studied by other authors. These showed promising results and highlighted that interventions adapted to the community and its culture is a powerful weapon to tackle iodine deficiency (22). It is also displayed the importance of health care workers as a trusted source of information about IS consumption and iodine deficiency (13, 14, 22, 23). Even though the use of MSCI and PBIS was sparse in this study, the efforts put in action by the government are already showing an important improvement in pregnant and breastfeeding women, to whom the PBIS is readily prescribed and Usage of iodised salt in diet according to the presence of a recommendation by a health care professional (physician, nutritionist, etc.) to implement iodised salt or any multivitamin supplement that contains iodine freely provided (10). Increasing informed decision making and providing awareness on the benefits of PBIS might provide even further improve results in pregnant women (24).
Adding to similar international studies, a recent study in São Miguel Island, Azores, showed the remarkable effects of implementing mandatory IS in public school canteen/refectory/bar services and increasing household consumption of IS in schoolchildren, decreasing the number of children with iodine deficiency in that island (11, 15, 16, 25, 26). The 48.3% household IS consumption registered in São Miguel Island is similar to the reported 49% use of IS of individuals in this study, as this might demonstrate consistency in information spread and implementation of measures in São Miguel Island and Faial Island. Other interventions to improve household IS consumption have been ben discussed throughout literature such as mandatory, government regulated salt iodization in order to provide properly iodised salt with adequate concentration to all households (27 - 29). But this might not be required if new and already implemented measures are better enforced to create awareness on iodine deficiency and providing the correct and needed information.
Since this study was conducted on a primary care setting and the sample retrieved from individuals attending appointments and working in this setting, there might be at play an important selection bias, as these individuals might be more health conscious and knowledgeable about iodine deficiency and IS. Consequently, the fraction of individuals who implement IS on their diet might be higher in this study than that of the overall population of Faial Island. The sample size in this study was also smaller than ideal.
CONCLUSIONS
Despite the great efforts made, and many with fruitful results, it is still necessary to strengthen the promotion of IS, in substitution of non- iodized salt, through awareness campaigns tailored to the community. The government, health institutions and health care workers should maintain the efforts to raise awareness of iodine deficiency, its implications on the people’s health, and work together to promote the utilization of IS more closely within the community.
It would be important to repeat this study, expanding it to all the islands in the Azores, with surveys not only in health care institutions, but also through other forms of surveys to increase accessibility and sample size Although, in this studied population, health care professionals’ intervention was the main reason for IS implementation an individualized approach might not be sustainable to attain the 90% IS household consumption and improve iodine deficiency numbers. Having this into consideration, a mandatory, regulated salt iodization program can perhaps be considered solutions for this problem.
Further deepen the knowledge on IS consumption and the reasoning behind the community’s implementation of IS in their households, can provide some guidance on how to achieve the 90% household usage of IS goal and use the attained information to resolve this problem and others to come.
ACKNOWLEDGMENTS
For a start, I would like to give my thankfulness and gratefulness to Dr. Sara Melo, Dr. Miguel Oliveira, Dr. Maria Inês Ramalho and Dr. Miguel Pacheco for all their help, support and availability in every need and doubt that came in the path of doing and writing this study. I would also like to express my gratitude to Dr. Manuela Soares for her support and guidance on putting this study in to motion. I want to give a very special token of my appreciation to all the health care workers of the Unidade de Saúde da Ilha do Faial on helping in the making of this project.