Introduction
Surgical site infection (SSI) is one of the most common and serious complications in perioperative healthcare. It represents a major risk for patient safety and for the quality of care. Surgical procedures are becoming more complex, and new medical devices and technologies are being introduced. Because of this, perioperative nursing practice requires strong scientific evidence and well-organized infection-prevention protocols.
The World Health Organization (WHO, 2018) estimates that up to 60% of SSIs can be prevented when clinical teams follow international guidelines and updated institutional protocols, such as those recommended by WHO and the Portuguese Directorate-General of Health (DGS, 2022). In Portugal, SSIs represent about 18% of all healthcare-associated infections, leading to longer hospital stays, higher morbidity and mortality, and increased hospital costs.
The epidemiological, clinical, and economic importance of SSI makes it essential to study perioperative nursing interventions that have proven effectiveness in prevention. Nurses play a key role in reducing surgical risks and improving patient safety.
The aim of this study is to identify and critically analyze perioperative nursing interventions that reduce SSI. This review provides an updated synthesis of scientific evidence to support continuous improvement of clinical practice, promote evidence-based professional training, and inform health policies focused on surgical safety and quality.
In Portugal, SSI continues to be one of the main causes of hospital morbidity (DGS, 2022). Understanding nursing interventions for SSI prevention is therefore essential to strengthen surgical safety at national and European levels, aligned with international commitments to healthcare quality and safety.
1. Theoretical framework
Healthcare-Associated Infections (HAIs) are a major global public health problem. They create high economic and social costs and increase patient dependence after hospital discharge (DGS, 2018; OPSS, 2019). In Europe, Surgical Site Infection (SSI) is one of the most common HAIs and is responsible for annual costs between 1.47 and 19.1 billion euros, extending hospital stay by an average of 6.5 days and tripling treatment costs (WHO, 2016).
In Portugal, the DGS (2015) reports that each SSI episode causes 7 to 11 extra hospital days and increases mortality risk 2 to 11 times. About 60% of SSIs are preventable through evidence-based protocols and the implementation of “bundles of interventions” (DGS, 2015). Alongside urinary tract infection and pneumonia, SSI is one of the most common and clinically important HAIs (DGS, 2017; Pina et al., 2010), significantly contributing to higher morbidity and mortality (Allegranzi et al., 2016; ECDC, 2019).
SSI is defined as an infection occurring at the surgical incision site (Rosa, 2017). It is a major postoperative complication and is associated with increased morbidity, mortality, hospital costs, and length of stay (Allegranzi et al., 2016). In Portugal, it accounts for 18% of hospital infections, especially in surgical units (DGS, 2022).
Preventing SSI is a multifactorial and dynamic process that requires a continuous and integrated patient-centered approach. Perioperative nurses must follow institutional protocols and the best available scientific evidence (AORN, 2019, 2020). Prevention strategies cover all three perioperative phases.
Preoperative interventions include proper antibiotic prophylaxis, skin preparation with 2% alcoholic chlorhexidine, and strict maintenance of normothermia (core temperature 36-38°C) (Gómez-Romero et al., 2017; Leaper & Ousey, 2015). Preoperative bathing with antimicrobial or non-antimicrobial soap is also recommended to reduce skin microbial load (Berríos-Torres et al., 2017). Correct timing of antibiotic administration is critical for treatment effectiveness.
Postoperative interventions include advanced measures such as negative pressure wound therapy and antiseptic dressings, which support healing and reduce infection risk (Leaper & Ousey, 2015). However, scientific evidence remains limited and inconsistent, highlighting the need for stronger randomized controlled trials to define best practices, target patient groups, and clinical applicability.
More recently, SSI prevention has adopted the concept of “bundles of interventions”, defined as groups of evidence-based practices applied together to maximize prevention effectiveness (WHO, 2015; Vieira & Bastos, 2022). These bundles show significant reductions in SSI when applied consistently.
However, some measures still lack solid scientific validation. For example, perioperative oxygen supplementation has produced contradictory results (Berríos-Torres et al., 2017). Continuous research and reinforced evidence-based practice remain essential for improving surgical patient safety and overall quality of healthcare (Ling et al., 2019).
2. Methods
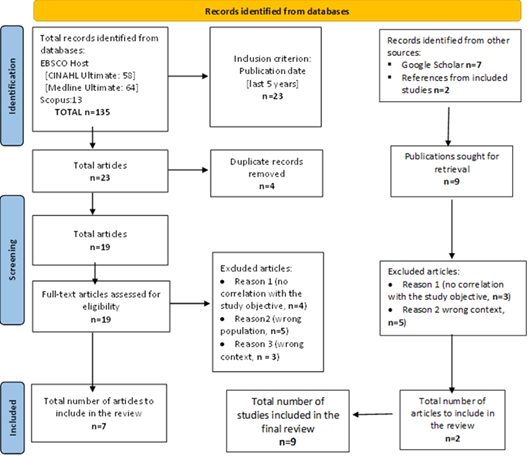
This study is a scoping review conducted according to the Joanna Briggs Institute (JBI, 2024) methodology and the PRISMA-ScR model. The research question was based on the PICO structure: What perioperative nursing interventions prevent surgical site infection in surgical patients?
Table 1 Components of the Research Question
| Text | |
|---|---|
| PARTICIPANTS | Surgical patient |
| INTERVENTIONS | Perioperative nursing intervention |
| COMPARISON | Not applicable |
| OUTCOME | Prevention of surgical site infection |
2.1. Inclusion Criteria
The review included studies written in English, Portuguese, French, or Spanish, published within the last five years (2019-2024). Only primary research articles written in these four languages were selected.
2.2. Search Strategy
The research followed three stages, according to the JBI methodology (Peters et al., 2020). First, an initial search was conducted in MEDLINE (via Pubmed Central) and CINAHL (via EBSCOShost) to identify search terms. In the second stage, a more comprehensive search was conducted in CINAHL, MEDLINE, Scopus, and Google Scholar, using the Boolean formula: (nursing interventions OR nursing interventions OR nursing care OR perioperative nurs* OR nurs* OR operative care) AND (Surgical patient OR surgical client OR perioperative client OR periorperative patient) AND (surgical wound infection). Finally, additional articles were searched in the bibliographic references of the selected studies. To ensure relevance, seven primary articles published between 2019 and 2024 in Portuguese, English or Spanish were included. The selection process followed the PRISMA-ScR model (Peters et al., 2020b Tricco et al., 2018), which guides the formulation of the question, definition of inclusion/exclusion criteria, location, selection, extraction, analysis, and synthesis of studies. The research was conducted between January and March 2024. The selection of studies was carried out by two independent reviewers, and disagreements were resolved by consensus.
3. Results
After applying the inclusion criteria, seven articles were selected for the scoping review. The articles were analyzed independently by two reviewers, following the JBI methodology for scoping reviews. A data extraction grid (Table 2) was used to collect and summarize the data, presented in reverse chronological order. The methodological quality of each study was assessed using the Joanna Briggs Institute (JBI) Critical Appraisal Tools, according to the 2020 Scoping Review Manual. Title Author(s)/
Year Main topics of the article Perioperative nursing interventions Methodological quality
Table 2 Data Extraction Instrument for the Included Studies
| Title | Author(s)/Year | Main topics of the article | Perioperative nursing interventions | Methodology quality | |
|---|---|---|---|---|---|
| 1 | Perioperative Strategies for Surgical Site Infection Prevention | Bashaw, M. e Keister, K. (2019) | The perioperative team is involved in the SSI prevention process; perioperative nurses use several evidence-based best practices to prevent SSI and support safe surgery | Hand hygiene; Preparation of the surgical site - disinfection with skin antiseptics, following the manufacturers' recommendations; Preparation with aseptic technique and antimicrobial irrigation; Appropriate surgical clothing; Number of people present in the room. | Low quality (low level of evidence) |
| 2 | Implementing an OR Contact Precautions Decision Algorithm to Promote Interprofessional Teamwork for Infection Prevention | Lacourciere, A. et al. (2019) | Effective cleaning of the perioperative environment is essential to prevent the spread of pathogens. For patients with multidrug-resistant microorganisms, environmental cleaning must follow evidence-based practices. Infection prevention is a multidisciplinary responsibility supported by interprofessional education | Perioperative nurses view aseptic and sterile techniques as guiding principles of their practice; Use/implementation of algorithms as a decision-making tool; rapid identification of appropriate environmental cleaning procedures; Interprofessional education. | Moderate quality (intermediate level of evidence) |
| 3 | Perioperative Nursing Considerations for Patients Undergoing Total Hip or Knee Arthroplasty | Tripp, H. & Fencl, J. (2020) | To ensure safe arthroplasty care, perioperative nurses must understand all phases of the continuous care process. These patients have increased SSI risk, making prevention strategies essential | Hand hygiene with antiseptics; adequate clothing; use of sterile instruments; maintaining normothermia (warming systems, increased room temperature); aseptic technique; surgical skin preparation; antibiotic prophylaxis according to protocols; controlling staff circulation; maintaining homeostasis | Low quality (low level of evidence) |
| 4 | Nurse-Led Randomized Controlled Trials in the Perioperative Setting | Munday, J. et al. (2020) | Identify areas of perioperative care that have been the focus of randomised controlled clinical trials by nurses | SSI prevention interventions: postoperative shampoo wash; preoperative 2% chlorhexidine wipes; silver-impregnated dressings vs. standard sterile dry dressings (cardiac surgery); optimized hair removal techniques; antiseptic methods | High methodological quality (high level of evidence) |
| 5 | Still more to do to improve perioperative safety and prevent patient harm | Duff, J. (2021) | SSI is one of the most significant preventable adverse events in perioperative care. Patient safety is a collective responsibility that requires collaboration to ensure a safe environment | TeamSTEPPS and CUSP programs to improve teamwork and communication for a strong safety culture | Low quality (low level of evidence) |
| 6 | Effectiveness of nursing intervention in the ope rating room to prevent wound infections in patients undergoing orthopaedic surgery: A meta-analysis | Zhu, D. & Luo Q. (2023) | Evaluates nursing interventions to prevent wound infections in orthopedic surgery. These interventions reduced infection rates, improved recovery, and increased nurse satisfaction | The implementation of strict equipment control and disinfection standards is crucial to reducing wound infections, promoting physical recovery, and improving the quality of care. Nursing intervention in the operating theatre should focus on routine nursing and reinforcement of sterile care before and after surgery, considering the entire surgical process and sterile environment for comprehensive prevention of post-operative infections | High methodological quality (high level of evidence) |
| 7 | Evaluation of Antibiotic Allergies in Surgical Patients | Larry, R. & Bertram, C. (2021) | Perioperative antibiotics are essential for SSI prevention. Beta-lactams (e.g., cefazolin) are preferred, but allergies may lead to less effective alternatives | Perioperative antibiotic therapy using beta-lactams as first-line agents; crucial role of nursing team in managing prophylaxis | Moderate quality (intermediate level of evidence) |
| 8 | Patient participation in surgical site infection prevention: perceptions of nurses, physicians and patients | Oliveira, C. et al. (2023) | Cross-sectional study with 123 postoperative patients and 92 health professionals. Both groups strongly agree that patient participation is important in SSI prevention | Patient/family participation in SSI prevention; preferred strategies: oral education, videos, and leaflets | Moderate quality (intermediate level of evidence) |
| 9 | Clear Minds: Unravelling Delirium in Older Adults" | Magata, E. & Leon, J. (2023) | High global SSI incidence requires combining infection control knowledge with precise maintenance of a clean surgical field. A quasi-experimental study shows that implementing an SSI prevention bundle in elective cholecystectomies reduces SSI when uniformly applied | Maintaining normothermia (36.5-37.5°C) through monitoring, warming blankets, and heated fluids; avoiding hair removal unless necessary; performing hair removal close to surgery using appropriate clippers; glove changes to maintain sterility | Moderate quality (intermediate level of evidence) |
As shown in the previous table, several perioperative nursing interventions are widely recognized as essential for preventing surgical site infection (SSI). These include hand hygiene, correct preparation of the surgical field, the use of appropriate surgical clothing, limiting the number of professionals inside the operating room, and maintaining normothermia (Bashaw & Keister, 2019; Magata & De Leon, 2023; Tripp & Fencl, 2020).
In addition, strict application of aseptic and sterile techniques, interprofessional education, and systematic environmental cleaning are identified as key practices for infection control (Bashaw & Keister, 2019; Lacourciere, 2019). Careful administration of antibiotic prophylaxis is also a central responsibility of the perioperative nursing team and requires precise management according to clinical recommendations (Larry & Bertram, 2021; Tripp & Fencl, 2020).
Effective communication and interprofessional collaboration are also essential strategies for reducing preventable adverse events related to SSI (Duff, 2021). Zhu and Luo (2023) show that providing nursing care in a sterile environment significantly decreases infection rates in orthopedic surgery, while Oliveira et al. (2023) highlight that active patient involvement is an important component of prevention.
Furthermore, Munday et al. (2020) and Magata & De Leon (2023) point out innovative developing strategies, such as the use of 2% chlorhexidine wipes, silver-containing dressings, and optimized hair removal techniques. These interventions show potential benefits but still require further scientific validation.
Overall, the available evidence shows that SSI prevention requires a multifactorial and integrated approach, supported by practices based on the best scientific evidence and coordinated actions between health professionals and patients. A critical analysis of these strategies must consider their alignment with national and international guidelines and identify remaining gaps in the literature regarding effectiveness and practical implementation.
4. Discussion
Preventing surgical site infection (SSI) is a fundamental part of perioperative nursing practice. It requires a systematic, multidimensional approach supported by strong scientific evidence. The results of this review are consistent with international guidelines from the World Health Organization (WHO, 2018), the Centers for Disease Control and Prevention (CDC, 2017, 2024), and the Portuguese Directorate-General of Health (DGS, 2022). These guidelines emphasize aseptic interventions, correct management of antibiotic prophylaxis, maintenance of normothermia, and active patient involvement.
The strong agreement between the practices identified in this review and the DGS (2022) recommendations demonstrates the maturity of scientific knowledge in this area. The “Bundle of Interventions” proposed by DGS includes validated practices such as hand hygiene, safe hair removal, antiseptic skin preparation, correct antibiotic prophylaxis, and maintenance of body temperature between 36°C and 38°C. The analyzed studies (Bashaw & Keister, 2019; Tripp & Fencl, 2020; Magata & De Leon, 2023; Zhu & Luo, 2023) show similar findings, reinforcing the role of perioperative nurses in implementing and monitoring these measures.
The literature consistently identifies hand hygiene and aseptic technique as core elements of SSI prevention. Bashaw & Keister (2019) and Lacourciere (2019) show that strong adherence to these practices reduces microbial load and improves patient safety. These findings support CDC (2024) and DGS (2022) recommendations for continuous monitoring of team adherence and regular auditing of aseptic practices.
Antibiotic prophylaxis is another essential intervention. Larry & Bertram (2021) and Tripp & Fencl (2020) emphasize the role of the nurse in managing the correct timing and dose, which are critical for effectiveness. Research by Berríos-Torres et al. (2017) and Oh et al. (2014) shows that extending antibiotics after wound closure does not prevent infection and may increase antimicrobial resistance. Therefore, strict compliance with time, type, and dose is an important indicator of quality and safety.
Proper skin preparation is also essential. Bashaw & Keister (2019), Tripp & Fencl (2020), and Dockery et al. (2021) demonstrate that using appropriate antiseptic solutions, such as 2% alcoholic chlorhexidine, significantly reduces skin microbial load. Preoperative bathing with antiseptic agents, recommended by DGS (2022) and Edmiston et al. (2014), must include clear patient instructions to ensure effectiveness.
Hair removal, when necessary, should be performed using electric clippers immediately before surgery, avoiding razors that increase the risk of micro-injuries and infection (Munday et al., 2020). Ruler et al. (2009) confirm that hair removal should be avoided when possible and done only when clinically justified.
Maintaining intraoperative normothermia is another well-established protective factor. Evidence (Magata & De Leon, 2023; Tripp & Fencl, 2020) shows that temperatures below 36°C reduce tissue perfusion and wound healing, increasing infection risk. Recommended strategies include forced-air warming, warmed fluids, and continuous temperature monitoring.
The operating room environment is another important determinant of surgical safety. Limiting foot traffic, controlling entry and exit, and using clothing and drapes that preserve the microbiological barrier-even under humidity-are evidence-based practices (Bashaw & Keister, 2019; Shaw et al., 2018; Vieira & Bastos, 2022). However, environmental cleaning remains challenging due to inconsistent practices and insufficient monitoring. Recent studies (Lacourciere, 2019; Xie et al., 2024) highlight the need for systematic approaches incorporating human factors and systems engineering to improve safety.
Interprofessional communication is also essential. Duff (2021), Reyes & Cuzzamu (2022), and Clendinning (2020) show that effective communication and teamwork increase adherence to prevention measures and reduce errors. Programs such as TeamSTEPPS and the Comprehensive Unit-based Safety Program (CUSP) have shown positive results in improving collaboration and safety culture.
Patient involvement is another key component. Oliveira et al. (2023) show that active participation improves adherence to hygiene measures, increases patient satisfaction, and enhances safety perception. Other studies (Agreli et al., 2019; Jerónimo & Gomes, 2020; Lomba et al., 2023) reinforce that patient education must be part of infection control programs.
Emerging research areas include silver dressings and preoperative chlorhexidine bathing. Although Munday et al. (2020) and Magata & De Leon (2023) present promising results, evidence is still heterogeneous. Meta-analyses indicate benefits in orthopedic surgery, but inconsistent findings in cardiac and gynecological specialties. Therefore, adoption of these technologies should consider evidence strength, cost-effectiveness, and clinical context.
Overall, this review reinforces that SSI prevention requires a combined and integrated approach. Perioperative nurses are central to connecting clinical practice, quality management, and health education. Applying evidence-based interventions, continuous training, and strong ethical commitment to patient safety are essential for high-quality surgical care. This review contributes to consolidating knowledge about effective perioperative nursing interventions and highlights gaps related to adherence and cost-effectiveness.
Tabela 3 Perioperative Nursing Interventions Identified for SSI Prevention
| Main category | Specific intervention | Recommendations |
| 1. Fundamental Practices | Hand hygiene; aseptic technique; surgical clothing and drapes; environmental cleaning and disinfection | Ensure team adherence; apply strict protocols |
| 2. Patient care | Antibiotic prophylaxis; skin preparation; electric hair removal; preoperative antiseptic bathing; glycemic control; nutritional optimization | Careful administration; avoid unnecessary hair removal; reinforce patient education |
| 3. Environmental Management | Limiting staff circulation; maintaining normothermia; ventilation control in the operating room | Reduce contamination risk; maintain body temperature between 36-38°C |
| 4. Facilitating Factors | Interprofessional communication; active patient participation | Continuous staff training; involve patients in prevention processes |
| 5. Emerging / Future Themes | New antiseptic technologies | Need for further research |
Implications for Practice
This scoping review highlights the essential role of perioperative nurses in preventing surgical site infection (SSI). It reinforces the importance of a structured clinical practice supported by strong scientific evidence. The results emphasize the need for strict implementation of measures such as hand hygiene, proper antibiotic prophylaxis, and effective interprofessional communication.
The findings summarize current knowledge, identify gaps in practice, and guide the adoption of safer and more effective approaches. These conclusions can support the development of evidence-based clinical protocols, strengthen continuous professional training, and contribute to health policies aimed at reducing surgical infections and improving care quality.
Future Research Directions
Despite the promising antimicrobial properties of silver-impregnated dressings, scientific evidence on their effectiveness in SSI prevention remains limited and inconsistent across surgical specialties. Orthopedic studies, especially in arthroplasty, indicate possible reductions in infection rates, while results in cardiac and general surgery are contradictory.
Significant gaps remain regarding the ideal type of dressing, silver concentration, duration of application, and identification of patient subgroups at higher risk of infection. Therefore, multicenter, randomized, and controlled studies are needed to determine optimal use and to integrate these dressings effectively into SSI prevention practices.
Further research is also recommended on professional adherence to preventive measures, the economic impact of interventions, and the effectiveness of patient-centered educational strategies, ensuring that recommendations are applicable in real clinical settings.
Conclusion
Surgical site infection remains one of the most common and preventable complications in perioperative care, with direct implications for patient safety, care quality, and the sustainability of health systems.
This scoping review mapped the main perioperative nursing interventions proven to be effective in preventing SSI. The findings highlight the importance of aseptic practices, correct antibiotic prophylaxis, maintaining normothermia, and adequate skin preparation.
The results confirm that SSI prevention must be approached in a combined and integrated way, using both technical interventions (e.g., environmental control, safe hair removal, hand hygiene) and non-technical interventions (e.g., communication, leadership, patient involvement). Systematic and monitored implementation strengthens the safety culture and leads to measurable improvements in clinical quality.
The adoption of the “Intervention Bundle” proposed by the Portuguese Directorate-General of Health (2022) provides a structured framework for standardizing preventive practices, resulting in significant gains in safety and efficiency. Effective implementation requires coordinated action between professionals and institutions, supported by strong institutional policies, continuous training, and regular audits.
Perioperative nurses emerge as key agents of change. They act not only as technical professionals but also as clinical leaders, educators, and promoters of organizational improvement. Applying scientific evidence in daily practice reinforces the ethical and professional commitment to patient safety.
In summary, SSI prevention goes beyond technical actions - it is an ethical, scientific, and institutional imperative that requires competence, shared responsibility, and a strong safety culture. Investment in applied research, updated protocols, and enhanced team skills is essential for sustainably reducing infection rates and promoting patient-centered, safe surgical care.
Implications for Health Policy and Practice
The results of this review provide scientific and technical support for health decision-makers and managers. They contribute to updating institutional protocols and strengthening infection control programs. Their integration can promote standardization of perioperative practices in Portugal, aligned with the objectives of the National Program for Infection Prevention and Control and Antimicrobial Resistance (PPCIRA).
Implementing these recommendations-supported by continuous education, clinical supervision, and systematic audits-reinforces patient safety culture and organizational efficiency. Furthermore, integrating evidence-based practices into European infection control strategies positions Portuguese nursing as a reference in delivering surgical care of excellence, grounded in science, ethics, and quality.
Authors' contribution
Conceptualization, L.J. e A.A.; data curation, L.J. e A.A.; formal analysis, L.J. e A.A.; funding acquisition, L.J. e A.A.; investigation, L.J. e A.A.; methodology, L.J. e A.A.; project administration, L.J. e A.A.; resources, L.J. e A.A.; software, L.J. e A.A.; supervision, L.J. e A.A.; validation, L.J. e A.A.; visualization, L.J. e A.A.; writing- original draft, L.J. e A.A.; writing- review & editing, L.J. e A.A.