Serviços Personalizados
Journal
Artigo
Indicadores
Links relacionados
Compartilhar
GE-Portuguese Journal of Gastroenterology
versão impressa ISSN 2341-4545
GE Port J Gastroenterol vol.23 no.2 Lisboa abr. 2016
https://doi.org/10.1016/j.jpge.2015.08.005
IMAGES IN GASTROENTEROLOGY AND HEPATOLOGY
Extensive Esophageal Ulceration in a Renal Transplant Patient
Extensa Ulceração Esofágica num Doente Transplantado Renal
Marco Silvaa,* , Roberto Silvab, Guilherme Macedoa
a Gastroenterology Department, Centro Hospitalar São João, Faculty of Medicine of the University of Porto, Porto, Portugal
b Pathology Department, Centro Hospitalar São João, Faculty of Medicine of the University of Porto, Porto, Portugal
* Corresponding author.
Keywords: Cytomegalovirus Infection; Esophagitis; Kidney Transplantation
Palavras-chave: Infeção por Citomegalovirus; Esofagite; Transplante de Rim
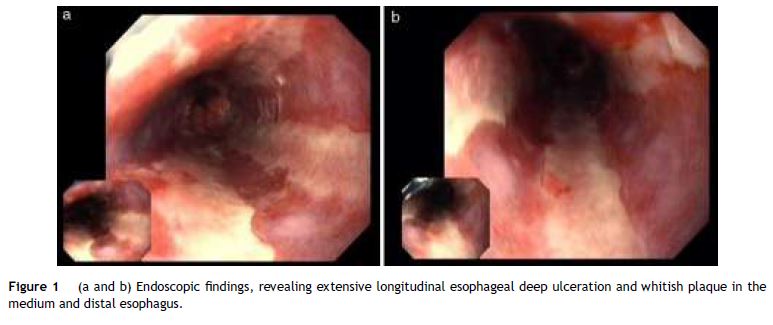
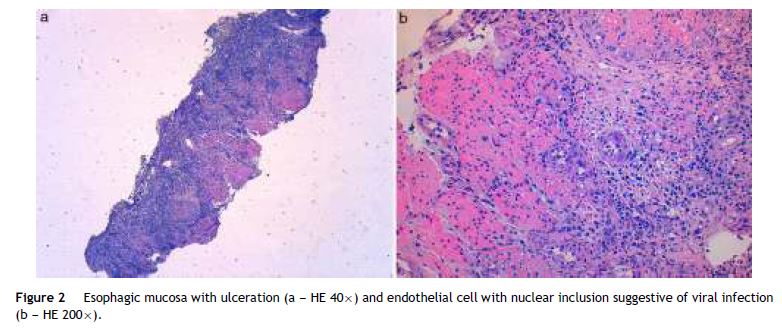
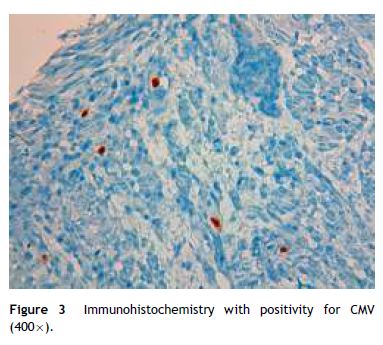
A 49 year-old male patient recurred to the emergency department complaining of anorexia, nausea, cough with mucopurulent sputum and dyspnea for 5 days. He had a history of poorly controlled type 1 diabetes mellitus with retinopathy, neuropathy and renal transplant (2 years before) for end-stage renal failure. The patient was taking immunosuppressive therapy with prednisolone (20 mg/day), tacrolimus (2 mg/day) and mycophenolic acid (720 mg/day). A chest X-ray, blood and urine tests performed were consistent with pneumococcal pneumonia and diabetic ketoacidosis. Therefore he was admitted. In the 4th day after admission the patient complained of heartburn and dysphagia. An upper endoscopy was performed and revealed extensive longitudinal esophageal deep ulceration and whitish plaque in the medium and distal esophagus (Fig. 1). The histopathological exam of the esophageal biopsy showed ulcerated esophageal mucosa with viral inclusion-like structures in the epithelium, suggestive of virus-induced esophagitis (Fig. 2). Cytomegalovirus (CMV) immunohistochemical was positive and confirmed the diagnosis of CMV esophagitis (Fig. 3). Ganciclovir (5 mg/kg every 12 h) was administered intravenously for 14 days, and it was well-tolerated. After 2 weeks of intense therapy and immunosuppressive regimen adjustments, dysphagia improved and he was discharged with oral valganciclovir (900 mg every 12 h).
CMV is a major cause of morbidity and a preventable cause of mortality in immunocompromised patients, especially transplant recipients and those infected with human immunodeficiency virus.1–3 CMV esophagitis has mostly been described in patients with acquired immunodeficiency syndrome, however, also may occur as a complication of immunosuppressive therapy, or even in immunocompetent patients.3,4 The gastro-intestinal tract is the commonest organ to be involved in CMV infection and esophagitis is the second most common gastrointestinal manifestation, next to colitis.2
Patients with CMV esophagitis present with odynophagia or dysphagia. Symptoms are indistinguishable from those associated with Candida or HSV esophagitis.5 Usually, the endoscopic appearance is typified by large shallow ulcers, either solitary or multiple, located in the middle or distal part of the esophagus.5 Histopathologic examination analysis demonstrating active disease and immunohistochemistry are the most reliable diagnostic methods in cases of tissue-invasive disease.3
Potent antiviral agents, are essential in the treatment of patients with non-HIV causes of immunosuppression, such as transplantation. For nonsevere CMV disease, valganciclovir (900 mg every 12 h) or intravenous ganciclovir (5 mg/kg every 12 h) are recommended as first-line treatment in adults. Conversion from intravenous ganciclovir to valganciclovir may be performed without interrupting dosing.1 When optimal drug exposure is required, such in severe or life-threatening CMV disease, those with high viral load, and those with questionable gastrointestinal absorption, intravenous ganciclovir is recommended.1,2 Dose reduction of immunosuppressive therapy should be considered in cases of severe CMV disease, in nonresponding patients, in patients with high viral loads or leukopenia.1
CMV-associated gastrointestinal infections are generally resolved without clinical symptoms in immunocompetent patients, but the infection can be fatal in the immunocompromised.5 Early recognition of this clinical entity is of vital importance to implement appropriate therapy and avoid potentially fatal complications.
References
1. Weile J, Streeck B, Muck J, Krebs G, Jakobus KH, Knabbe C, et al. Severe cytomegalovirus-associated esophagitis in an immunocompetent patient after short-term steroid therapy. J Clin Microbiol. 2009;47:3031-3. [ Links ]
2. Kotton CN, Kumar D, Caliendo AM, Asberg A, Chou S, Danziger-Isakov L, et al. Transplantation Society International CMV Consensus GroupUpdated international consensus guidelines on the management of cytomegalovirus in solid-organ transplantation. Transplantation. 2013;96:333-60. [ Links ]
3. Razonable RR, Humar A. AST Infectious Diseases Community of Practice. Cytomegalovirus in solid organ transplantation. Am J Transplant. 2013;4:93-106. [ Links ]
4. Lim DS, Lee TH, Jin SY, Lee JS. Cytomegalovirus esophagitis in an immunocompetent patient: case report. Turk J Gastroenterol. 2014;25:571-4. [ Links ]
5. Bernard S, Germi R, Lupo J, Laverrière MH, Masse V, Morand P, et al. Symptomatic cytomegalovirus gastrointestinal infection with positive quantitative real time PCR in apparently immunocompetent patients: a case series. Clin Microbiol Infect. 2015;15:531-5. [ Links ]
Ethical disclosures
Protection of human and animal subjects. The authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of data. The authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consent. The authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
Conflicts of interest
The authors have no conflicts of interest to declare.
* Corresponding author.
E-mail address: marcocostasilva87@gmail.com (M. Silva).
Acknowledgments
The authors wish to thank Dr. Rosa Coelho and Dr. João Magalhães, from the Gastroenterology and Pathology Department, for the support in their work.
Received 2 June 2015; accepted 26 August 2015














