Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Jornal Português de Gastrenterologia
versão impressa ISSN 0872-8178
J Port Gastrenterol. vol.19 no.5 Lisboa set. 2012
Neuroendocrine tumor of the anal canal
Tumor neuroendócrino do canal anal
Adriana Borgonovi Christianoa, Caio Eduardo Gullob, Marianna Angelo Palmejanib, Aline Maria de Vita Marquesb, Amanda Pires Barbosab, Marcelo Pandolfi Bassoa, Luiz Guilherme Cernaglia Aureliano de Limac, João Gomes Netinhod,∗
a Resident in the Discipline of Coloproctology, Department of Surgery, Faculdade de Medicina de São José do Rio Preto (FAMERP), São José do Rio Preto, São Paulo, Brazil
b Graduation Student at Faculdade de Medicina de São José do Rio Preto (FAMERP), São José do Rio Preto, São Paulo, Brazil
c Resident in the Discipline of Pathology, Department of Pathology and Legal Medicine, Faculdade de Medicina de São José do Rio Preto (FAMERP), São José do Rio Preto, São Paulo, Brazil
d Department of Surgery, Faculdade de Medicina de São José do Rio Preto (FAMERP), São José do Rio Preto, São Paulo, Brazil
*Corresponding author
Abstract
We report a rare case of neuroendocrine tumor of the anal canal and its poor prognosis, plus discuss the need of immunohistochemical for an acurate diagnosis and to guide treatment.
Keywords Neuroendocrine tumor; Anal canal; Immunohistochemistry; Metastic disease
Resumo
Relatamos um caso raro de tumor neuroendócrino do canal anal e seu mau prognóstico, bem como a necessidade de imuno-histoquímica para o diagnóstico correto e para orientar o tratamento.
Palavras-chave Tumor neuroendócrino; Canal anal; Imunohistoquímica; Doença metastática
Introduction
The anal canal tumors are unusual lesions whose frequence is about 1.5% of the gastrointestinal tract neoplasias.1 The predominant histological type is the squamous cells cancer (SCC) (47%), followed by cloacogenic carcinoma and less commonly melanoma or mucinous adenocarcinoma.2 In relation to the neuroendocrine tumor (NET) occurrence on this location, its undeniable rarity justifies this case report.
Case description
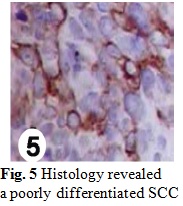
A 49-year-old woman presented with anal bleeding, smallcaliber stool with purulent discharge and severe proctalgia in the last three months. She had no abominal pain, no bowel habit changes, no fever, no loss weight and no inguinal lymphadenopathy. Investigation was conducted by the Colorectal Service of Hospital de Base, São José do Rio Preto, and started in August 2007. Two perianal condylomas and a hard anal mass were detected in the rectal exam and the pathological evaluation revealed condylomatosis and a poorly differentiated, ulcerated and invasive SCC. The patient was treated with Nigro.
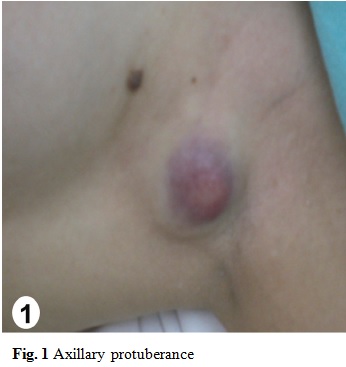
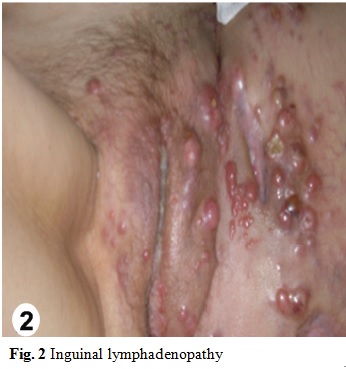
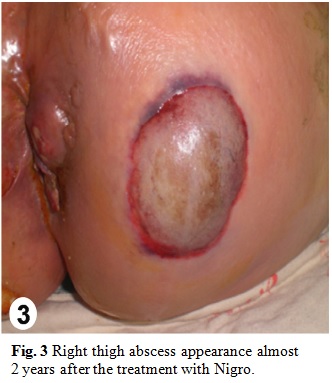
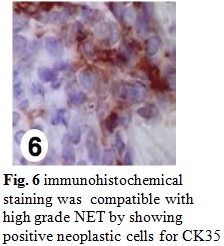
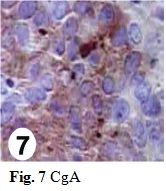
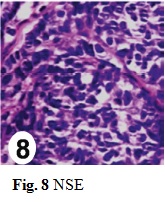
An incisional biopsy of the residual lesion was performed that resulted in no sign of malignancy. One year later, colonoscopy was normal and there were no metastasis in the imaging follow-up. After 7 months, the patient returned with 5 cm bilateral mammary and axillary protuberances (Fig. 1), right inguinal lymphadenopathy (Fig. 2) and ipsilateral thigh abscess (Fig. 3). In face of the possibility of canal anal tumor recurrence, it was sought colonoscopy and biopsy with immunohistochemical markers search in the potentially metastatic lesions. Neoplastic cells were immunoreactive for cytokeratin (CK) 35 (Fig. 6), cromogranin A (CgA) (Fig. 7) and neuron-specific enolase (NSE) (Fig. 8) that were compatible with metastatic high grade NET. The lamina revision of the primary anal lesion revealed poorly differentiated carcinoma (Fig. 5) in fibroconjunctive tissue with necrosis and angiolymphatic tumor embolization areas.
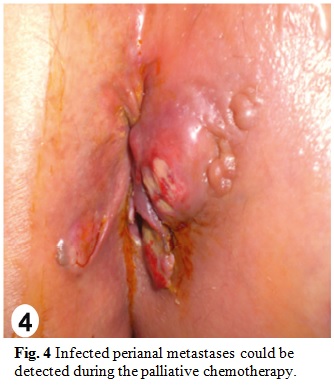
During the introduction of palliative chemotherapy with cisplatin and irinotecam, the patient developed enlargement of inguinal lymph nodes with abscesses and fistulization in addiction to Fournier syndrome. One month later, infected perianal metastases (Fig. 4) could be detected associated with recurrence of Fournier syndrome, contiguity intravaginal injury and septic shock treated with consecutive debridement, extended antibiotic therapy and estomal confection. Intraoperative findings included a metastatic mass in the greater omentum. Chemotherapy was discontinued because her immune status was impaired. Unfortunately she died in May 2009 from septic complications.
Discussion
NET can originate in any part of the body, for example, lungs, skin, urogenital system, digestive tract, thyroid and adrenal.3 When situated in large intestine (about 0.3-3.9% of all colorrectal tumors), they are histologically heterogeneous but share high aggressiveness4 being more common in caecum, rectum and sigmoid. Anal location is rare and indicates a poor prognosis.5,6 There is a variety of NET, rare and aggressive, with multidirectional differentiation, where are observed foci of this histological type, adenocarcinoma and SCC.7 The clinical presentation of NET does not differ from colorrectal adenocarcinomas. However a more advanced tumor stage can be observed at the time of its diagnosis. Rarely there are manifestations of paraneoplastic syndrome, carcinoid (diarrhea and rash) and metabolic abnormalities.8
It was observed that the differentiation of an epitelial tumor into NET is an independent unfavorable prognostic factor.9 For example, in relation to colorectal neoplasias, Thomas and Sobin (1995) found a 27% survival at 5 years for stages III and IV adenocarcinoma, but only three of 51 patients with the same staging and neuroendocrine differentiation remained alive for two years in that study.10 Specific markers that may be used to establish neuroendocrine differentiation comprise NSE, CD56, CgA and synaptophysin, being the two latter recommended due to their relative sensitivity and specificity.11 Immunohistochemical study is also critical to guide treatment, as Nigro is used for anal canal SCC, while surgical removal remains the best chance of cure for patients with NET.
Only early detection of the disease can result in some benefit on its evolution because adjuvant interventions such as radio and chemotherapy do not constitute an impact factor to improve survival in these cases. However new lines of chemotherapy are being developed using streptozotocin and 5-fluorouracil or doxorubicin with 5-fluorouracil.12 Also palliative options such as surgery, manufacture of colostomy and radiotherapy should be evaluated to improve the life quality of patients with advanced disease.
References
1. Dallan LAP, Cruz SHA, Rosa DL, Bin FC, Nadal SR, Capelhuchnik P, et al. Avaliação dos resultados do tratamento de 14 doentes de carcinoma espinocelular anal. Rev Bras Coloproct. 2006;26:34-40. [ Links ]
2. Guimarães AP, Matos D, Segreto R, Forones NM. Carcinoma espinocelular de canal anal: análise de 11 casos. Arq Gastroenterol. 2001;38:9-13. [ Links ]
3. Garcia-Carbonero R, Capdevila J, Crespo-Herrero G, Díaz-Pérez JA, Martínez Del Prado MP, Alonso Orduna V, et al. Incidence, patterns of care and prognostic factors for outcome of gastroenteropancreatic neuroendocrine tumors (GEP-NETs): results from the National Cancer Registry of Spain (RGETNE). Ann Oncol. 2010;21:1794-803. [ Links ]
4. Akintola-Ogunremi O, Pfeifer JD, Tan BR, Zhu X, Hart J, Goldblum JR, et al. Analysis of protein expression and gene mutation of c-kit in colorectal neuroendocrine carcinomas. Am J Surg Pathol. 2003;27:1551-8. [ Links ]
5. Simon SR, Fox K. Neuroendocrine carcinoma of the colon. Correct diagnosis is important. J Clin Gastroenterol. 1993;17:304-7. [ Links ]
6. Modlin IM, Lye KD, Kidd M. A 5-decade analysis of 13,715 carcinoid tumors. Cancer. 2003;97:934-59. [ Links ]
7. Novello P, Duvillard P, Grandjouan S, Elias D, Rougier P, Bognel C, et al. Carcinomas of the colon with multidirectional differentiation. Report of two cases and review of the literature. Dig Dis Sci. 1995;40:100-6. [ Links ]
8. Gaffey MJ, Mills SE, Lack EE. Neuroendocrine carcinoma of the colon and rectum. A clinicopathologic, ultraestructural and immunohistochemical study of 24 cases. Am J Sug Pathol. 1990;14:1010-23. [ Links ]
9. Atasoy P, Bozdogan O, Öztürk S, Ensari A. BCL2 expression and its correlation with neuroendocrine differentiation in colon carcinoma. Tumori. 2004;90:233-8. [ Links ]
10. Thomas RM, Sobin LH. Gastrointestinal cancer. Cancer. 1995;75:154-70. [ Links ]
11. Washington MK, Tang LH, Berlin J, Branton PA, Burgart LJ, Carter DK, et al. Protocol for the examination of specimens from patients with neuroendocrine tumors (carcinoid tumors) of the colon and rectum. Arch Pathol Lab Med. 2010;134: 176-80. [ Links ]
12. Villalonga R, Basany EE, Cano LM, Landolfi S, Armengol Carrasco M. Neuroendocrine carcinomas of the colon and rectum. A units experience over six years. Rev Esp Enferm Dig (Madrid). 2008;100:11-6. [ Links ]
Conflicts of interest
The authors have no conflicts of interest to declare.
*Corresponding author
E-mail address: jgnetinho@riopreto.com.br (J. Gomes Netinho).
Received 23 March 2011; accepted 24 June 2011
Abbreviation
SCC squamous cells cancer
NET neuroendocrine tumor
CK citokeratin
CgA cromogranin A
NSE neuron-specific enolase













