Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Acta Obstétrica e Ginecológica Portuguesa
versión impresa ISSN 1646-5830
Acta Obstet Ginecol Port vol.11 no.3 Coimbra set. 2017
CASE REPORT/CASO CLÍNICO
Vaginal leiomyoma: a common disease with a rare presentation
Mioma da vagina: apresentação rara de uma doença comum
Vânia Costa Ribeiro*, Helena Solheiro**, António Santos Paulo**
Centro Hospitalar Tondela-Viseu; Hospital São Teotónio, Departamento de Ginecologia-Obstetrícia
*Interna de Formação Especifica de Ginecologia e Obstetrícia, Maternidade Dr. Alfredo da Costa, Centro Hospitalar Lisboa Central
**Assistente Hospitalar Graduado de Ginecologia e Obstetrícia; Centro Hospitalar Tondela-Viseu, Hospital São Teotónio, Departamento de Ginecologia-Obstetrícia
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Leiomyomas are pelvic smooth muscle tumours that present with a variety of clinical symptoms depending on site location. Although leiomyomas can be present in the uterus, round ligament, peritoneum and blood vessels, vaginal occurrence is a rare finding. This report describes a patient with a vaginal leiomyoma in the posterior wall of the vagina with complaints of abundant vaginal discharge and pelvic pain. Transvaginal excision of the tumour was performed with histopathologic diagnose and complete cure of the patient.
Keywords: Vaginal leiomyoma; Vaginal tumour; Leiomyoma
Introduction
Vaginal leiomyomas are a rare presentation of a very common disease among women of reproductive age. They were first described in 1733 and since then approximately 300 cases have been reported1-3. They are more frequently found in the anterior vaginal wall although they can occur in lateral and posterior walls4,5. Despite being frequently small in size, they might present as a prolapsed vaginal mass associated with vaginal discharge, bleeding, dyspareunia or lower abdominal pain. When presenting during pregnancy they can lead to labour dystocia6-8.
In this report we sought to describe the clinical features and surgical treatment of this unusual vaginal tumour, in a patient referred to our hospital.
Case report
A 39-year-old, caucasian women, was referred to our Gynaecology Department, on December 2015, for vaginal discharge, pelvic pain and dyspareunia lasting for three months.
The vaginal examination revealed a nodular, non-tender mass with approximately 5 cm, attached to the posterior vaginal wall through a 2cm pedicle. The tumour was lined by vaginal mucosa with no signs of ulceration. Abundant vaginal discharge was present with no signs of infection. An incisional biopsy was performed which revealed a leiomyoma. Vaginal ultrasound was not conclusive for the possible aetiology of the tumour but an incisional biopsy was performed and revealed a leiomyoma.
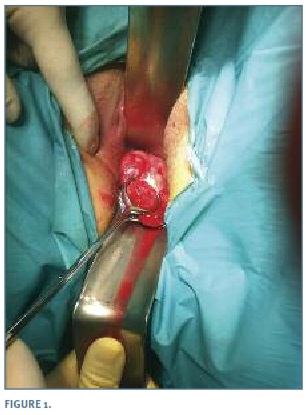
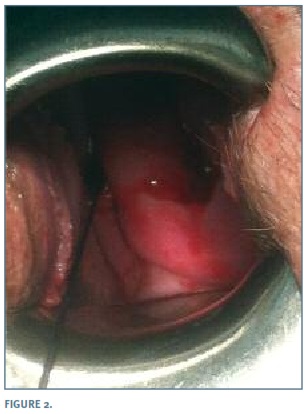
Based on histologic result we decided for surgical excision of the tumour, by vaginal approach, under sedation. We began by placing vaginal retractors to clearly identify the tumour pedicle which required clamping for its complete excision (Figura 1). Vaginal mucosa was then repaired with a single layer suture (Figura 2). The procedure lasted 30 minutes with no intra or post-operative complications. The patient was discharge 24 hours after surgery.
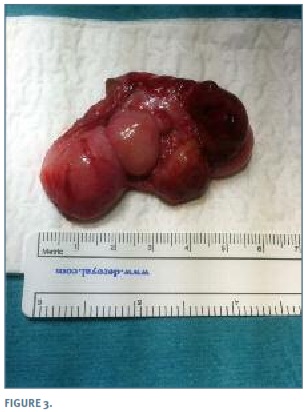
The excised mass had a maximum diameter of 5cm (Figura 3), weighed 16 grams, and had a bosselated surface with a firm consistence. The macroscopic anatomo-pathological evaluation showed a white appearance inside. Final histopathology defined the tumour as a leiomyoma.
Discussion
Leiomyomas are very common between women in reproductive age, still, presentation in the vagina is a rare clinical finding. In 1941, at the Johns Hopkins Hospital, Bennett and Ehrlich described an incidence of 0.1% in 15 000 autopsies performed9. Similar to other leiomyomas they seem to be more prevalent between 35 and 50 years old women10.
These benign tumours are usually small in size, single and slow growing. Although in our clinical report we found a 5cm pedunculated leiomyoma covered with smooth intact vaginal mucosa, this tumour can vary from 0.5 to 15cm in diameter and may or may not be pedunculated with or without disrupted vaginal mucosa depending on its dimension11,12. The tumour presents, in the majority of situations, as a firm mass, but degenerative changes can alter the texture7. Normally they become symptomatic within a time course of 8.4 years after presentation and when reaching bigger diameters responsible for symptoms, depending on the site of occurrence13. Presentation in the anterior wall typically relates with obstructive urinary symptoms, frequency and dysuria.
Vaginal leiomyomas despite usually regarded as benign tumours are susceptive to undergo malignant transformation which is apparently more common in extra-uterine leiomyomas possibly due to increase of mitotic activity secondary to traumatic stimuli3,14. Malignant transformation is more common in the posterior wall and in a series of 11 cases the incidence of malignancy was reported as being 9.1%13. Malignancy appears to be more prevalent in association with fast growing tumours and post-menopausal status. In our case report malignancy was highly unlikely since, though it was a posterior tumour, it was small in size with well-defined margins and intact vaginal mucosa in a young patient.
When facing a vaginal tumour several entities must be taken into account in the differential diagnose. Clinicians should always exclude the likelihood of other benign lesions such as polyps, Skene duct abscess, Gartner's duct cysts, urethral diverticulum and vaginal cysts. A rapid growth and an infiltrative nature suggests malignancy so the possible diagnosis of leiomyosarcomas, squamous carcinomas, adenocarcinomas and more rarely metastases, should be ruled out.
Vaginal clinical inspection and incisional biopsy seem crucial to assess the origin, extent and histology of the tumour. Some case reports refer to preoperative vaginal ultrasound (US) and pelvic magnetic resonance (MRI) as being useful diagnostic methods mainly the MRI which has the capacity to accurately define the anatomic relationships of the tumour15-17 with other structures. Pelvic imaging, although helpful to define the boundaries of surgical excision, has limited value for etiological diagnose which can be overpassed by incisional biopsy.
To our understanding vaginal US or even MRI might be helpful to plan surgical excision of anterior vaginal tumours since they accurately define the relationship of the tumour with the urethra and bladder. However in the evaluation of posterior tumours, concomitant vaginal and rectal examination allows the clinician to define the boundaries of the tumour and for so imaging complementary diagnostic exams might not be needed in this particular situation. Also in what regards imaging evaluation, the clinician should be aware that US and MRI don't differentiated a leiomyoma from a leiomyosarcoma. Such as for uterine leiomyomas the US echogenicity and MRI signal of vaginal leiomyoma can be identical to leiomyosarcoma. US findings like central necrosis, mixed hyper and hypoechogenic parts, irregular distribution of vessels and low impedance flow can be found in both pathologies. MRI absence of calcifications seems to have a consistent presence in leiomyosarcomas but a high signal intensity is not a reliable predictor of the presence of sarcomatous degeneration18.
In our patient clinical inspection and biopsy allowed to clearly describe a pedunculated mass defined by histopathology as leiomyoma. The use of ultrasound didn´t add useful clinical information.
The treatment of choice for vaginal leiomyomas is trans-vaginal surgical excision which is curative and diagnostic excluding malignant cases13. Once leiomyomas are more prevalent during reproductive ages they can also present during pregnancy and according to previous reports, in this specific situation, surgical vaginal excision should be performed in symptomatic leiomyomas between the 16th and 32rd week of gestation allowing for cicatrisation of vaginal mucosa before delivery19.
Despite the effectiveness of treatment the recurrences should always be in the clinician mind as during fertility years leiomyomas can rapidly re-growth under estrogenic influence20 with a recurrence of symptoms.
We describe this rare vaginal tumour to raise awareness for leiomyomas in the differential diagnose when facing a vaginal tumour. This brief review of the literature enhances the importance of clinical observation and incisional biopsy to reach a clear diagnose and rule out malignancy before curative surgery which is widely important to minimize patient's symptoms and enhance life quality.
REFERENCES
1. Costantini E, Cochetti G, Porena M. Vaginal para-urethral myxoid leiomyoma: case report and review of the literature. Int Urogynecol J Pelvic Floor Dysfunct 2008; 19:1183-1185. [ Links ]
2. Tourneux JP. Les fibromes du vagina. Progr Med Paris 1934; 41:1569. [ Links ]
3. Cobanoglu O, Gurkan Zorlu C, Ergun Y, Kutluay L. Leiomyosarcoma of the vagina. Eur J Obstet Gynecol Reprod Biol 1996:70:205-207. [ Links ]
4. Young SB, Rose PG, Reuter KL. Vaginal fibromyomata: Two cases with preoperative assessment, resection and reconstruction. Obstet Gynecol 1991; 78:972-974. [ Links ]
5. Elsayes KM, Narra VR, Dillman JR, Velcheti V, Hameed O, Tongdee R, et al. Vaginal Masses: Magnetic Resonance Imaging Features with Pathologic Correlation. Acta Radiol 2007; 8:921-933. [ Links ]
6. Park SJ, Choi SJ, Han KH, Park KH, Chung H, Song JM. Leiomyoma of the vagina that caused cyclic urinary retention. Acta Obstet Gynecol Scand 2007; 86:102-104. [ Links ]
7. Oruc S, Karaer O, Kurtul O. Coexistence of a prolapsed, pedunculated cervical myoma and pregnancy complications: a case report. J Reprod Med 2004; 49:575-577. [ Links ]
8. Sadan O, Kruger S, van Iddekinge B. Vagina tumors in pregnancy. Case report and review of the literature. Acta Obstet Gynecol Scand 1987; 66:559-562. [ Links ]
9. Bennett HG Jr, Erlich MM. Myoma of the vagina. Am J Obstet Gynecol 1941; 42:314-320. [ Links ]
10. Imai A, Furui T, Hatano Y, Suzuki M, Suzuki N, Goshima S. Leiomyoma and rhabdomyoma of the vagina. Vaginal myoma. J Obstet Gynaecol 2008; 28:563-566. [ Links ]
11. Sherer DM, Cheung W, Gorelick C, Lee YC, Serur E, Zinn HL, et al. Sonographic and magnetic resonance imaging findings of an isolated vaginal leiomyoma. J Ultrasound Med 2007; 26: 1453-1456. [ Links ]
12. Ruggieir AM, Brody JM, Curhan RP. Vaginal leiomyoma. A case report with imaging findings. J Reprod Med 1996; 41:875-877. [ Links ]
13. Liu MM. Fibromyoma of the vagina. Eur J Obstet Gynecol Reprod Biol 1988; 29:321-328. [ Links ]
14. Haque AU, Moatasim A, Aslam F. Mitotically active leiomyoma: a word of caution. Int J Pathol 2004; 2:38-41. [ Links ]
15. Shadbolt CL, Coakley FV, Qayyum A, Donat SM. MRI of vaginal leiomyomas. J Comput Assist Tomogr 2001; 25:355-357. [ Links ]
16. Pavlica P, Bartolone A, Gaudiano C, Barozzi L. Female paraurethral leiomyoma: ultrasonographic and magnetic resonance imaging findings. Acta Radiol 2004; 45:796-798. [ Links ]
17. Ikeda R, Suga K, Suzuki K. MRI appearance of a leiomyoma of the female urethra. Clin Radiol 2001;56: 76-79. [ Links ]
18. Amant F, Coosemans A, Debiec-Rychter M, Timmerman D, Vergote I. Clinical management of uterine sarcomas. Lancet Oncol. 2009; 10(12):1188. [ Links ]
19. Jeng CJ, Lee TM, Huang SH, Lee FK, Tzeng CR. Rapidly growing vaginal leiomyoma: Case report. J Gynecol Surg 2003; 19:33-36. [ Links ]
20. Maruo T, Ohara N, Wang J, Matsuo H. Sex steroidal regulation of uterine leiomyoma growth and apoptosis. Hum Reprod Update. 2004; 10:207-220. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Vânia Costa Ribeiro
E-mail: dokvcr@gmail.com
Conflict of interest
The authors acknowledge no conflicts of interest, financial or otherwise, that may have impacted this manuscript.
Recebido em: 05/06/2016
Aceite para publicação: 04/09/2016