Servicios Personalizados
Revista
Articulo
Indicadores
Links relacionados
Compartir
Acta Obstétrica e Ginecológica Portuguesa
versión impresa ISSN 1646-5830
Acta Obstet Ginecol Port vol.11 no.4 Coimbra oct. 2017
CASE REPORT/CASO CLÍNICO
Necrotizing fasciitis after cesarean section: combination of vacuum assisted closure and antiseptic solution instillation as a successful treatment
Fasceíte necrotizante após cesariana: combinação de terapia de pressão negativa e instilação de solução antisséptica como tratamento eficaz
Tiago Aguiar*, Inês Nunes**, Nuno Muralha***, Carla Ramalho****, Nuno Montenegro*****
Centro Hospitalar São João
*Interno do Internato Complementar; Serviço de Ginecologia e Obstetrícia do Centro Hospitalar São João
**Assistente Hospitalar; Serviço de Ginecologia e Obstetrícia do Centro Hospitalar São João
**Assistente Hospitalar; Serviço de Cirurgia Geral do Centro Hospitalar São João
***Assistente Hospitalar Graduada; Serviço de Ginecologia e Obstetrícia do Centro Hospitalar São João
****Director de Serviço; Serviço de Ginecologia e Obstetrícia do Centro Hospitalar São João
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Necrotizing Fasciitis (NF) is an infectious and inflammatory process, with necrosis of the fascia muscularis and surrounding subcutaneous adipose tissue, evolving quickly and that can be potentially fatal. Although rare, NF can be one of the possible clinical presentations of surgical wound infection after cesarean delivery. A case of a patient who was submitted to a cesarean section during labor with later development of NF of the abdominal wall is presented. An integrated therapeutic approach with multiple surgical debridments and a combination of negative pressure wound therapy and instillation of antiseptic solutions was used, with full recovery of the patient.
Keywords: Puerperium; Cesarean Section; Necrotizing Fasciitis.
Introduction
Necrotizing Fasciitis (NF), is a severe infectious process, that includes necrosis and destruction of the fascia muscularis and surrounding subcutaneous adipose tissue, involving the entire space between the skin and the underlying muscular layers1.
Due to its rapid progression and high capacity of dissemination, NF can be potentially fatal. Therefore, a prompt diagnosis and an adequate therapeutic response are very important, in order to control damage extension and reduce associated mortality.
Although NF is a relatively rare disease, with 0.4 cases per 100.000 persons per year2, some studies have shown an increase in its incidence over the last two decades3-5. Despite the availability of better therapeutic options, the mortality rate remains high, ranging from 9% to 29%6.
Several risk factors have been identified, namely diabetes and obesity, which can partially explain the increasing number of NF cases in the recent years as their incidence has also been increasing. Immunosuppression, intravenous drug use, peripheral vascular disease, trauma and recent surgeries have also been associated with a higher probability of the occurrence of the disease7.
NF can be classified into four types, according to the pathogenic agent involved2. Type I consists in a polymicrobial infection, with at least one anaerobic agent involved combined with one or more aerobic or facultative anaerobic agent. This type of NF occurs mainly in individuals with several co-morbidities and affects more often the upper body and perineum (Fournier's gangrene). Type II is usually a monomicrobial infection, caused in the majority of the cases by Streptococcus pyogenes. It predominantly affects the limbs and is more frequent in patients without risk factors, usually starting with a cutaneous lesion. Type III includes monomicrobial infections involving Clostridium Species, and are more frequently seen in drug users, affecting trunk, limbs and perineum. It can also be caused by Vibrio Vulnificus, after exposure to contamined water. Type IV is the result of a fungal infection, usually in immunocompromised patients, and it can involve the upper body, limbs and perineum. Some authors, divide NF in only three sub-types, including fungal infections in the Type I8.
NF prompt diagnosis is essential in the establishment of the prognosis and it depends on a high level of clinical suspicion. The clinical presentation is unspecific: severe and disproportionate pain, extending beyond the affected skin with hardening of the subcutaneous cellular tissue and associated crepitation. Hemorrhagic bullae and cutaneous necrosis may develop associated with signs of systemic toxicity such as fever, hemodynamic instability and deterioration of the mental state, in more severe cases9. The laboratory assessment must include full blood cell count, inflammatory markers, blood cultures and microbiological study of exudates and affected tissues10. In the majority of cases, imaging assessment is not helpful, including computerized tomography scan (CT-scan) or magnetic resonance imaging (MRI), and as for the analytical work-up, it should not delay the surgical treatment.
NF diagnosis is clinical and must be considered a surgical emergency. Patient survival depends on a timely therapeutic intervention - consisting frequently on multiple surgical debridements of the affected areas, with removal of infected and necrotic tissues. Broad spectrum antibiotics must be started early, with adequate adjustment according to the microbiologic results as soon as possible. As a general rule, they should be continued until no more debridements are needed.
Beyond surgery and antibiotics, some adjuvant therapeutic options, such as oxygen therapy with hyperbaric chambers and negative pressure wound therapy (NPWT) can improve patient recovery11,12.
As mentioned before, recent surgery is a risk factor for the development of NF. In this context, cesarean section, one of the most frequently surgical procedures performed all over the world, represents an important cause of the overall surgical wound infections, with an incidence ranging from 3,7% to 9,8%13. Although rare, NF can be one of the possible clinical presentations of surgical wound infection after cesarean delivery.
Several risk factors have been implied in the development of surgical wound infection after a cesarean delivery. They can be divided into antepartum (obesity, smoking, low socioeconomic status, inadequate pre-natal surveillance, use of corticosteroids, gestational hypertensive disorders, diabetes, multiple pregnancy), intrapartum (urgent surgery, long term procedure, lack of adequate antibiotic prophylaxis and chorioamnionitis) and postpartum (anemia and wound hematoma) risk factors12.
In this report, we present a case of a NF after a cesarean section during labor in whom a novel therapeutic approach of NWPT with instillation of an antiseptic solution was used as an adjuvant therapy.
Case Report
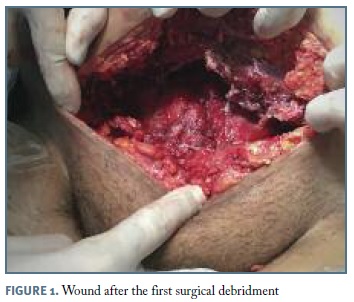
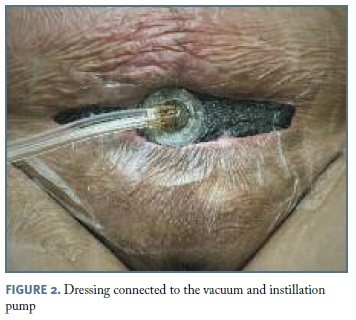
A 20-year-old puerperal obese female, 10 days after a cesarean section (done after a trial of fetal extraction with ventouse because of non-reassuring fetal status), was admitted to the hospital with fever, abdominal pain and fetid smell lochia since three days ago. The surgical wound was apparently well, but with cellulitis in the surrounding skin. Empirical intravenous combined antibiotics (gentamicin and clindamycin) were started assuming the diagnosis of puerperal endometritis. After 48 hours, the patient complained about increasing abdominal pain, maintained fever peaks of 39ºC. The blood workup revealed increasing anemia (from 8.6g/dL to 8.1g/dL), leukocytosis with neutrophylia (from 18.8x109 (83,3%) to 13.55 x109/L (81.1%)) and stable C-reactive protein (388 mg/dL to 357 mg/dL). The abdomen showed spreading cellulitis, with skin hardening, and exceedingly painful palpation of the superior edge of the surgical incision, until 10 cm away of it to the inferior ribs. Other concurrent diagnostic hypotheses were then raised: abdominal wall abscess, myositis or necrotizing fasciitis. The abdominal ultrassound and, after, the CT-scan favoured the clinical suspicion of necrotizing fasciitis. The patient was immediately taken to the operation room (OR) and the diagnosis of NF confirmed. Extensive debridement and necrosectomy were performed (Figure 1) straightway, with identification of three necrotizing loci sub-aponeurosis and supra-rectus abdominus. The wound was isolated with a dressing associating NPWT with instillation of saline solution (Figure 2).
A reassessment in the OR was planned in 48h for wound evaluation and infection control. The operative approach sequence used included: a pre-debridement deep cleaning with saline solution and neutral soap; excision of nonviable tissue; 10 minutes of dwelling time using an antiseptic solution. The wound was sealed with a foam dressing, transparent film and track pad connection to an adjustable vacuum and instillation pump. The NPWT was initiated inside the OR. The settings on the device's software (V.A.C. VeraFloTM Therapy®, Acelity, San Antonio, United States of America) included a dwell time of 10 minutes and a negative pressure of 125mmHg. The application of negative pressure was stopped every 4 hours for 10 minutes of dwelling time, and resumed automatically thereafter.
The wound reassessment with debridement of necrotic tissue and dressing change, were performed every 4 to 6 days, according to the intra-operative findings. In the first wound dressing, saline was instilled. After that, a solution containing undecilaminopropil betaine and polihexidine (Prontosan®; B. Braun, Queluz de Baixo, Portugal) was used. After the fourth debridement, we used a solution of Octenidin (Octenilin®; Schülke & Mayr GmbH, Norderstedt, Germany).
A total of 6 surgeries were performed, after which the wound was closed (apponeurosis suture with polypropylene suture 1-0 and skin interrupted suture with nylon suture 2-0) and a NWPT was applied. The dressing was removed 8 days after, and the stiches 3 days later.
The antibiotics were adjusted empirically soon after the NF diagnosis was made - vancomycin in association with piperacillin/tazobactam were added to clindamycin. A multiresistant Staphylococcus epidermidis (including methicillin, but sensitive to vancomycin) was isolated in the urine, vaginal discharge and wound exudate; blood cultures were negative - therefore, the antibiotic scheme was not changed and it was maintained during 20 days. The histological findings of the wound removed material revealed necrotic and inflammatory tissue.
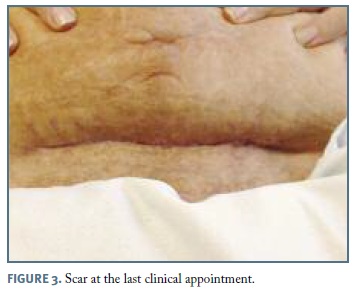
During the hospital stay, the patient remained at the Obstetrics ward, with progressive clinical and analytical improvement. She was discharged at the 29th day post-admission. No other complications occurred and the patient was referred to the Obstetric outpatient clinic for follow-up. She was discharged home one month later with excellent aesthetic and functional results (Figure 3).
Discussion
There is no data regarding the incidence of NF related to obstetric surgical procedures. Although rare, due to the inherent risk factors (namely the physiologic gestational immunosuppression), this disease can be dangerous and potentially fatal, carrying a high associated psychosocial burden14,15. In the reported case, obesity and an urgent cesarean section performed in labour stand out as the main risk factors.
Considering the specificities of this population, it's fundamental to precociously identify the risk factors, ideally during the antenatal period, therefore allowing its correction (if possible) and also enabling the implementation of preventive measures. In pregnant women submitted to cesarean section, the use of adequate antibiotic prophylaxis before the surgery, as well as the closing of the subcutaneous cellular tissue when its thickness is over 2 cm are strategies that can reduce the risk of surgical wound infection12.
One of the main challenges of NF is its early diagnosis8. In an early stage, physical signs are unspecific and can be diminished by the use of antibiotics or due to the weaker immune response (typical from pregnancy)9. Therefore, clinical suspicion is the most important element in the timely and adequate diagnosis16.
The therapeutic gold standard for NF is based on an early surgical intervention as well as the administration of antibiotics. Furthermore, some adjuvant measures can improve the patient recovery, reducing associated morbidity. The use of NWPT has increased lately. Systems of continuous or intermittent suction, combined with the instillation of antiseptic solutions prevent bacterial overgrowth and remove exudates, allowing a quicker growth of viable tissue12,17.
The main goals of this case report is to raise the attention of obstetricians and gynecologists to the increasing incidence of wound infection in the context of cesarean deliveries, of which necrotizing fasciitis is a possible clinical manifestation and to describe one of the novel approaches to treat this condition. As in other contexts, also in the obstetric population, the approach combining surgical debridments with NWPT and instillation of antiseptic solutions seems to be a safe option in the treatment of NF and therefore can apparently be used in cases similar to the one that we describe.
REFERENCES
1. Bisno AL, Brito MO, Collins CM. Molecular basis of group A streptococcal virulence. Lancet Infect Dis 2003;3:191-200. [ Links ]
2. Misiakos EP, Bagias G, Patapis P, Sotiropoulos D, Kanavidis P, Machairas A. Current concepts in the management of necrotizing fasciitis Front Surg. 2014;1:36 [ Links ]
3. Poromanski I, Andriessen A. Developing a tool to diagnose cases of necrotising fasciitis. J Wound Care 2004;13:307-310. [ Links ]
4. Sun X, Xie T. Management of Necrotizing Fasciitis and Its Surgical Aspects. Int J Low Extrem Wounds 2015;14:328-334. [ Links ]
5. Das DK, Baker MG, Venugopal K. Increasing incidence of necrotizing fasciitis in New Zealand: a nationwide study over the period 1990 to 2006. J Infect 2011;63:429-433. [ Links ]
6. Magala J, Makobore P, Makumbi T, Kaggwa S, Kalanzi E, Galukande M. The clinical presentation and early outcomes of necrotizing fasciitis in a Ugandan Tertiary Hospital - a prospective study. BMC Res Notes 2014;7:476. [ Links ]
7. Anaya DA, Dellinger EP. Necrotizing soft-tissue infection: diagnosis and management. Clin Infect Dis 2007;44:705-710. [ Links ]
8. Cocanour CS, Chang P, Huston JM, Adams Jr. CA, Diaz JJ, Wessel CB, Falcione BA, Bauza GM, Forsythe RA, Rosengart MR. Management and Novel Adjuncts of Necrotizing Soft Tissue Infections. Surg Infect (Larchmt). 2017;18:250-272. [ Links ]
9. Waldron C, Solon JG, O'Gorman J, Humphreys H, Burke JP, McNamara DA. Necrotizing fasciitis: The need for urgent surgical intervention and the impact of intravenous drug use. Surgeon 2015;13:194-199. [ Links ]
10. Wong CH, Khin LW, Heng KS, Tan KC, Low CO. The LRINEC (Laboratory Risk Indicator for Necrotizing Fasciitis) score: a tool for distinguishing necrotizing fasciitis from other soft tissue infections. Crit Care Med 2004;32:1535-1541. [ Links ]
11. Hollabaugh RS, Jr., Dmochowski RR, Hickerson WL, Cox CE. Fournier's gangrene: therapeutic impact of hyperbaric oxygen. Plast Reconstr Surg 1998;101:94-100. [ Links ]
12. Fitzwater JL, Tita AT. Prevention and management of cesarean wound infection. Obstet Gynecol Clin North Am 2014;41:671-689. [ Links ]
13. Tran TS, Jamulitrat S, Chongsuvivatwong V, Geater A. Risk factors for postcesarean surgical site infection. Obstet Gynecol 2000;95:367-371. [ Links ]
14. Lowthian JT, Gillard LJ, Jr. Postpartum necrotizing fasciitis. Obstet Gynecol 1980;56:661-663. [ Links ]
15. Golde S, Ledger WJ. Necrotizing fasciitis in postpartum patients. A report of four cases. Obstet Gynecol 1977;50:670-673. [ Links ]
16. Chan T, Yaghoubian A, Rosing D, Kaji A, de Virgilio C. Low sensitivity of physical examination findings in necrotizing soft tissue infection is improved with laboratory values: a prospective study. Am J Surg 2008;196:926-930. [ Links ]
17. Gupta S, Gabriel A, Lantis J, Teot L. Clinical recommendations and practical guide for negative pressure wound therapy with instillation. Int Wound J 2016;13:159-174. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Tiago Aguiar
E-mail: tiagomdiasaguiar@gmail.com
Recebido em: 01/02/2017
Aceite para publicação: 13/06/2017
Acknowledgements
We would like to acknowledge the patient for the permission to publish this case report.