Serviços Personalizados
Journal
Artigo
Indicadores
Links relacionados
Compartilhar
Revista Portuguesa de Enfermagem de Saúde Mental
versão impressa ISSN 1647-2160
Revista Portuguesa de Enfermagem de Saúde Mental no.13 Porto jun. 2015
ARTIGO DE INVESTIGAÇÃO
Psychometric properties of the self-administered version of the "Self-Care Requisites Scale" among carers for the mentally ill*
Propiedades psicométricas da versão de auto preenchimento "Self-Care Requisites Scale" em cuidadores de doentes mentais*
Propiedades psicométricas de la versión autoadministrada "Self-Care Requisites Scale" en cuidadoras de enfermos mentales*
Núria Albacar-Ribóo**, Mar Lleixá-Fortuño***, María Teresa Lluch Canut****, Carlos Sequeira*****, José Carlos Carvalho******, Juan Francisco Roldán Merino*******
**Enfermera; Doctora por la Universidad de Rovira i Virgili; Profesora en la Universidad de Rovira i Virgili – Departamento de Enfermería, Avenida Remolins, 13-15, 43500 Tortosa (Tarragona), España. E-mail: nuria.albacar@urv.cat
***Enfermera; Psicóloga; Doctora por la Universidad de Rovira i Virgili: Profesora en la Universidad de Rovira i Virgili – Departamento de Enfermería, 43500 Tortosa (Tarragona), España. E-mail: mar.lleixa@urv.cat
****Enfermera especialista en Enfermería de Salud Mental; Doctora en Psicología. Catedrática de Enfermería Psicosocial y Salud Mental en la Universidad de Barcelona – Escuela de Enfermería, 08907 Hospitalet de Llobregat, Barcelona, España. E-mail: tlluch@ub.edu
*****Doutor em Ciências de Enfermagem; Coordenador do Grupo de Investigação NursID do Center for Health Technology and Services Research; Professor Coordenador na Escola Superior de Enfermagem do Porto, 4200-072 Porto, Portugal. E-mail: carlossequeira@esenf.pt
******Doutor em Ciências de Enfermagem; Professor Adjunto na Escola Superior de Enfermagem do Porto, 4200-072 Porto, Portugal. E-mail: zecarlos@esenf.pt
*******Doctor en Ciencias de Enfermería; Profesor Asociado en la Universidad Rovira i Virgili; Profesor Titular en la Escola Universitària d'Infermeria Sant Joan de Déu, 08950 Esplugues de Llobregat, Barcelona, España. E-mail: JRoldan@santjoandedeu.edu.es
ABSTRACT
INTRODUCTION: People with schizophrenia frequently need the assistance of a family member who may then become the main carer for the patient. For the carer this may be a difficult and complicated situation that needs to be taken into account in the design of healthcare intervention. Our plan was to carry out an evaluation of the carer, using the "Self-care Requisites Scale" of Roldan (2011). The aim of the study was to adapt the scale in such a way that it could be self-administered.
METHODOLOGY: The design was carried out in two phases. First the questionnaire was adapted so that it could be self-administered; this was done by consensus among a group of experts. In the second phase we analyzed the psychometric properties of the results in terms of reliability and validity.
RESULTS: The definitive questionnaire consisted of 35 items and 6 dimensions. The internal consistency coefficient for the instrument overall was 0.85. The strongest correlations were obtained between the majority of the sub-scales and the total scale.
CONCLUSIONS: The "Self-care Requisites Scale" is easily self-administered by the carers of people suffering schizophrenia. The results, in terms of both reliability and validity, were good.
Keywords: Carer; Schizophrenia; Self-care; Questionnaire
RESUMO
INTRODUÇÃO: As pessoas com esquizofrenia precisam frequentemente de cuidados diários de um familiar, que progressivamente se vai tornar no cuidador principal. Este viverá uma situação difícil e complexa, sendo necessário inclui-lo na implementação de qualquer tipo de intervenção em saúde. Propõe-se realizar a avaliação do cuidador, utilizando o "Questionário de requisitos Self-care" Roldan (2011). O objetivo do presente estudo foi realizar uma adaptação do questionário de forma a que possa ser utilizado na modalidade de auto-preenchimento.
METODOLOGIA: O desenho do estudo foi conduzido em duas fases. Primeiro, procedeu-se à adaptação do Questionário de auto-preenchimento, através do consenso de um painel de especialistas. Na segunda fase, foram analisados as propriedades psicométricas em termos de confiabilidade e validade.
RESULTADOS: O questionário final foi composta por 35 itens e 6 dimensões. O coeficiente de consistência interna para o total do instrumento foi de 0,85. As correlações mais fortes foram obtidas entre a maioria das sub-escalas e da escala total.
CONCLUSÕES: O "Questionário de requisitos de autocuidado" é de fácil auto preenchimento por cuidadores de pessoas com esquizofrenia. Obtiveram-se bons resultados em termos de confiabilidade e validade.
Palavras-Chave: Cuidador; Esquizofrenia; Questionário de auto-preenchimento
RESUMEN
INTRODUCCIÓN: Las personas con esquizofrenia necesitan a menudo el cuidado diario de un familiar, que se convertirá en la cuidadora principal. Ésta vivirá una situación difícil y compleja, siendo necesario incluirla en el diseño de cualquier tipo de intervención sanitaria. Se propone realizar la valoración de la cuidadora, utilizando la "Self-care requisites scale" de Roldan (2011). El objetivo de este trabajo fue realizar una adaptación para poderla utilizar de forma autoadministrada.
METODOLOGÍA: El diseño se realizó en dos fases. Primero se adaptó el cuestionario para poder ser autoadministrado, a través del consenso de un grupo de expertos. En la segunda fase, se analizaron las propiedades psicométricas en términos de fiabilidad y validez.
RESULTADOS: El cuestionario definitivo constó de 35 ítems y 6 dimensiones. El coeficiente de consistencia interna para el total del instrumento fue de 0,85. Las correlaciones más fuertes se obtuvieron entre la mayoría de las subescalas y la escala total.
CONCLUSIONES: La "Self-care requisites scale" es fácil de autoadministrar por las cuidadoras de personas con esquizofrenia. Se obtuvieron buenos resultados en cuanto a fiabilidad y validez.
Descriptores: Cuidadora; Esquizofrenia; Autocuidado; Cuestionario
Introduction
Beginning the 1980s a model of community care took root in Spain in which the chronically mentally ill, such as those diagnosed with schizophrenia, went from living their lives for the most part as interns in psychiatric hospitals to living at home. In Spain some 80% of people affected by schizophrenia (Touriño, Inglot, Baena, Fernández & Alvarez 2007) thus found themselves living their day to day lives among their families, with all the changes and repercussions that this may have entailed in family life.
Patients with schizophrenia are often dependent, requiring constant supervision and care from a family member who then becomes the main care provider (Karsch, 2003). In most cases this person, the carer, is a female family member (Ferré, Rodero, Vives & Cid, 2008; Sequeira, 2010). The main carer often finds herself (or himself) in a difficult and complicated situation that is laden with contradictions. On the one hand, there is the urge to care, to provide instrumental, affective, and emotional support which generates a sense of well-being (Dinis, Rodrigues-Ferreira & Carvalho, 2014). But on the other hand, the carer may feel ill at ease, in that the role assumed carries with it a loss of autonomy and a burden of responsibility, dedication, and hard work. In general, providing care in this way leads to uncertainty, exhaustion, dependence, and lifestyle changes that may have a profound effect on the carer’s personal and social life (Pereira & Vega, 2012; Sequeira, 2010). It is therefore of the utmost importance to include the family in the design of any intervention strategy on the part of the healthcare profession (Cardoso, Verderoce, Malagutti & Severino, 2012).
Numerous international organizations have stressed the need for promoting self-care in order to attain an appropriate level of health and well-being (European Parliament, 2006; WHO, 1998, 2009).
Evaluation, as a first step in the process of providing nursing care, must be carried out extremely carefully in order to uncover the shortcomings in self-care and to be able, later, to provide the care that is needed, thereby enhancing both the autonomy and the sense of well-being of the individual. Good evaluation requires a conceptual frame of reference as well as a worthy instrument of measurement. The theory that best supports the perspective of self-care and which also takes into account the carer as an agent of dependent care is Dorothea Orem's Self-Care Theory (SCT) (2001). SCT defines self-care as behavior that exists in specific situations in life, directed by individuals toward themselves or toward their surroundings, with the aim of regulating those factors that affect their development and functioning to the benefit of their lives, health, and well-being (Orem, 2001).
In order to put the conceptual framework of Orem into operation a "Self-care Requisites Scale" (SCRS) was created; the Spanish version, known as the "Escala de Requisitos de Autocuidado" (ERA) (Roldán, 2011; Roldán-Merino, Puig-Llobet, Lluch-Canut, Menarguez-Alcaina, Sabadell & QuestERA Working Group; Roldán-Merino, Lluch-Canut, Menarguez-Alcaina, Foix-Sanjuan, Haro Abad, & Quest ERA Working Group, 2014), was built upon the foundation of SCT.
The SCRS measures the degree of compliance of health carers and the capacity of the individual to live autonomously by reference to the eight universal requisites of self-care put forward by Orem. The SCRS is made up of 35 questions or items that work on a Likert scale model; each item has a value of from 1 to 5 points, where 1 means "very appropriate" and 5 "very inappropriate." The items of the various requisites display a certain dependency among themselves. The scale is divided into 6 dimensions to address the 8 requisites described by Orem (Table 1).

The overall SCRS score is the sum total of the scores for the individual items; the range of possible scores is from 35 to 175. A high score on an individual requisite or on the instrument overall indicates a lack of satisfaction of the requisites of self-care on the part of the carer, which would argue for the need for a specific nursing intervention. In contrast, a low score indicates fulfilment of the requisites of self-care.
The instrument has been validated in patients with schizophrenia, at the community level, and it has been shown to display good psychometric values; analysis of its internal consistency demonstrated high homogeneity among all the items on the questionnaire (Cronbach alpha for the scale overall was 0.87). Analysis of stability over time, measured by means of test-retest, showed a high level of concordance (the intraclass correlation coefficient for the scale was 0.90, while for each of the self-care requisites the score was greater than 0.70). The questionnaire has also shown evidence of having discriminating validity (Global Assessment of Functioning Scale p = 0.0001) and strong correlation with the Life Skills Profile scale (p <0.01). The SCRS was created for use by a trained expert dealing with people with a diagnosis of schizophrenia who were not hospitalized, but rather living in the community (Roldan, 2011; Roldán-Merino, Lluch-Canut et al, 2014).
The present study had as its goal the creation of an adapted questionnaire so as to enable use of the SCRS on a self-administered basis by carers of people with schizophrenia.
Methodology
The study was carried out in two phases. In the first of these an adaptation of the SCRS was developed for self-administration, and this was then tested in a pilot study to verify clarity, the level of comprehension, and the time needed to complete the questionnaire.
In order to formulate the adaptation, the author of the scale was contacted to secure permission for its use and to request his collaboration in the study. At the first meeting it was agreed, with the author, to use letters to differentiate the various versions of the SCRS scale. SCRS-c, then, is the original version, for use with schizophrenics living in the community. For our study the adaptation was designated as SCRS-a, with the affixed letter indicating self-administrated (‘autoadministrada’ in Spanish). For validation of the contents of SCRS-a a group was formed, made up of six specialists in mental health nursing, one of whom is also an expert in psychometrics. Two analysis and discussion sessions were held. The comments by the experts led to a number of modifications being made. A new item was added in the dimension of "Providing care regarding bodily elimination processes" concerning the matter of perspiration: 9. "Do you have problems with sweating?" The inclusion of this question was suggested by Roldán in the Conclusions of the SCRS validation study (Roldán, 2011; Roldán et al 2014). It was agreed to eliminate item 19: "Does the patient wear clean clothes that are appropriate to the time and place?" This question, under the aegis of dimension V, was deemed to lack justification in the hands of the carers. A number of changes were also subsequently made in the wording of questions so that they could be answered in a self-administered mode; for example, item 1 "Is the person able to carry out physical activity without showing signs of respiratory fatigue?" was changed to "Are you able to carry out physical activity without showing signs of respiratory fatigue?" The same procedure was followed for the rest of the questions in the questionnaire. By applying all the modifications decided upon the new version of the SCRS, the SCRS-a, was created.
Afterwards a pilot study with 18 carers was carried out. The results demonstrated that the carers completely understood all of the questions, and that the time they needed to complete the questionnaire ranged from 20 to 30 minutes. Therefore, no further changes were made to the SCRS-a scale.
In the second phase the psychometric properties of the questionnaire were analyzed in terms of reliability and validity. The population used in this phase of the study consisted of carers of people with schizophrenia. The carers were those who identified themselves as being responsible for providing care in the household without receiving any remuneration for so doing (Pereira & Vega, 2012).
The study was run in three institutions belonging to the Autonomous Community of Catalonia, Spain: the Pere Mata Terres de l’Ebre Foundation in Amposta-Tortosa, Tarragona; Adult Mental Health Center 1 of the Municipal Institute of Personal Services in Badalona, Barcelona; and the Mental Health and Family Association for Girona County, Girona.
The sample consisted of 77 carers, selected consecutively and non-probabilistically. All of the carers accompanying their patient family members on visits to participating centers for regular visits, hospital admissions, or association meetings between the months of March and November 2013 were included. The inclusion criteria were self-identification as a carer of a person diagnosed with schizophrenia, being an adult, signing informed consent, and understanding Spanish so as to be able to complete the validated Spanish-language form of the self-administered questionnaire. The exclusion criteria were observable cognitive deterioration and rejection of participation in the study.
A descriptive analysis was undertaken of all the variables included in the study. Central tendency and dispersion measurements were calculated both for each item and for the SCRS-a overall. SCRS-a reliability was analyzed by means of internal consistency with Cronbach alpha. Construct validity was also determined by analyzing the correlation with the Pearson correlation coefficient of the SCRS-a, which evaluated the convergent and discriminating validity, based upon the hypothesis that the correlation between each sub-scale and the overall scale should be stronger than the correlations among the sub-scales (Fayers & Machin, 2000).
The confidence level was set at 95%, and the difference between variables was considered significant at p≤0.05.
For analysis of the data we used the package SPSS Statistics for Windows (Version 17.0; SPSS Inc., Chicago IL, USA).
Prior to carrying out the study authorization was obtained from either the ethical committee or the management of the participating institutions, as the case may be, along with the information sheet, data protection sheet, and informed consent of the carers.
Results
The final version of the questionnaire that was used included 35 items grouped into the 6 Dimensions (Albacar, 2014) (Table 2).
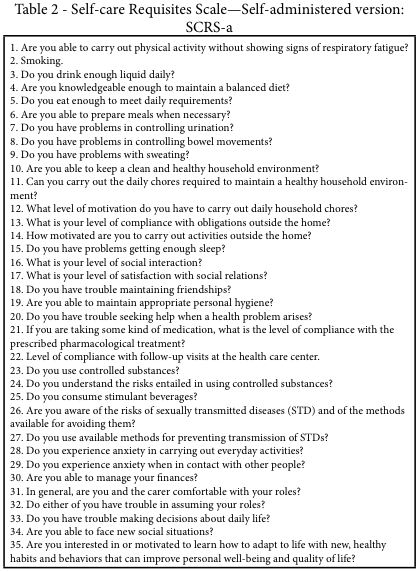

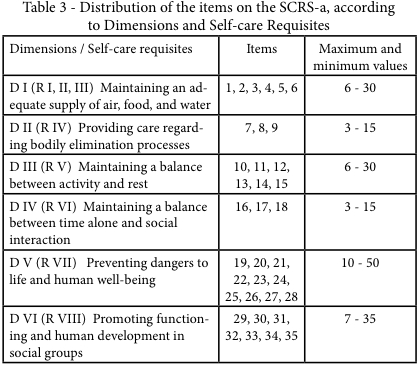
Table 3 shows the distribution of the 35 items among the 8 requisites for self-care that make up the conceptual structure that underlies the SCRS-a, along with the maximum and minimum values for each dimension and self-care requisite. The SCRS rearranges three of the self-care requisites put forward by Orem (Maintaining an adequate supply of air, food, and water) into a single dimension, which is why there are 6 dimensions and 8 requisites.
The overall score on the SCRS-a for the 77 carers participating in the study was 58.9 (SD 13.3) with a median of 54; the lowest score on the questionnaire was 39 while the highest was 103.
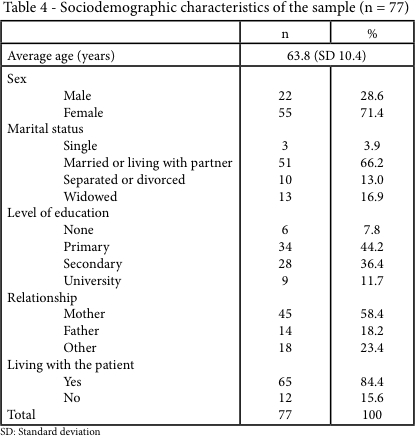
The average age of the carers was 63.8 (SD 10.4) and 71.4% of them were women. In terms of marital status 66.2% were married or had a partner, and more than 80% had completed primary or secondary school. In terms of the relationship with the patient, mothers (58.4%) were the carers in the main, and 84.4% of carers lived with their patient family members (Table 4).
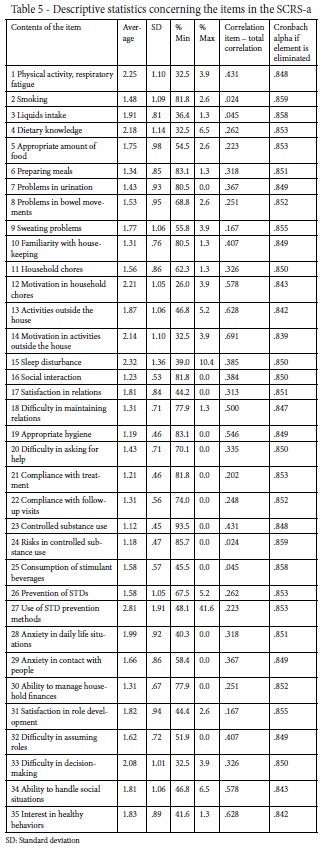
In the analysis of the items, the average value ranged from 1.12 to 2.81, while the standard deviation ranged from 0.45 to 1.91. The item with the strongest ceiling effect was number 27 (Use of STD prevention methods) (41.6%) while in terms of the floor effect the items with the highest scores were numbers 23 (Controlled substance use) (93.5%), 24 (Risks in controlled substance use) (85.7%), 6 (Preparing meals) (83.1%), and 19 (Appropriate hygiene) (Table 5).
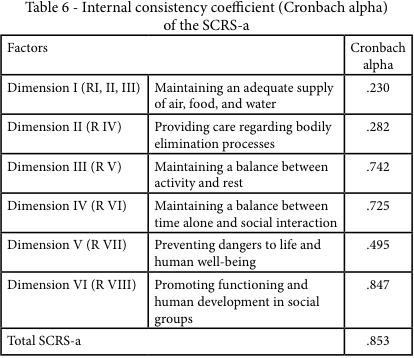
The internal consistency coefficient -the Cronbach alpha- was 0.85, and for three of the dimensions (Maintaining a balance between activity and rest, Maintaining a balance between time alone and social interaction, and Promoting functioning and human development in social groups) the scores were above 0.70 (Table 6).
Most items showed item correlation-total correlation scores above 0.20. Only 5 items showed lower correlations (2, 3, 9, 25, and 31). These items were smoking, liquids intake, sweating problems, consumption of stimulant beverages, and satisfaction in role development, respectively (Table 5).
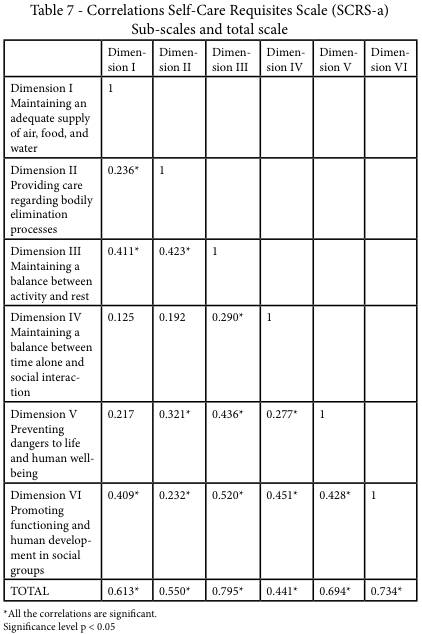
Analysis of the correlations between the sub-scales and the overall scale is presented in Table 7. As hypothesized, the strongest correlations were found between the majority of sub-scales and the total scale. Dimension III (Self-care requisite: maintaining a balance between activity and rest) and Dimension VI (Self-care requisite: promoting functioning and human development in social groups) correlated more strongly with the overall scale (r=0.795 and r=0.734, respectively), while Dimension IV (Self-care requisite: maintaining a balance between time alone and social interaction) correlated more weakly with the total scale (r=0.441). The strongest correlation among the subscales was between Dimension III and Dimension VI (r=0.520), while the weakest was between Dimension I and Dimension II (r=0.236). There was no significant correlation between the subscale of Dimension I and the subscales of Dimensions IV and V, nor was the correlation significant between the subscale of Dimension II and that of Dimension IV. All the other correlations were statistically significant (Table 7).
Discussion
As noted earlier, the SCRS was built upon the foundation of a theory of nursing, the SCT of D. Orem, which is well known and frequently referred to by nurses in a variety of settings, and numerous studies (Marriner & Alligoog, 2007; Roldán, 2011; Roldán-Merino, Lluch-Canut et al, 2014).
In order to adapt the SCRS for use as a self-administered questionnaire, the SCRS-a, a methodological process recommended by metrics experts for processes of this kind was followed (Nunnally, 1994): the validity of the content was measured with qualitative methodology, and through consensus of a group of experts using the Delphi method the main indicators of reliability were also measured. The pilot study led to a number of changes proposed by the expert group, which were accepted; the SCRS-a then proved to be easily self-administered by carers of people with schizophrenia, thus demonstrating the functionality that had been ascribed to it in the pilot study.
The results obtained in our study with the SCRS - a were positive in terms of reliability, and they are comparable to the results obtained in other studies using the SCRS-c model (Miguel, 2014; Roldán, 2011; Roldán-Merino, Lluch-Canut et al, 2014). In terms of reliability, with both versions of the scale (SCRS-c and SCRS-a) the dimensions that scored higher than 0.70 on the Cronbach alpha were: D III (Maintaining a balance between activity and rest), D IV (Maintaining a balance between time alone and social interaction), and D VI (Promoting functioning and human development in social groups).
In like manner, convergent and discriminating validity, measured with the Pearson correlation coefficient, showed that both versions of the scale, the SCRS-c and the SCRS-a, had higher correlation values for the scale as a whole than between the sub-factors.
The main limitation of the study has to do with the size of the sample. It would be of value to carry out studies in similar circumstances and comparable contexts, but with larger samples. Validation of instruments is a long, ongoing process. Although this study has yielded metrical data about the SCRS-a instrument’s content validity, reliability, and convergent and discriminating validity, factorial analysis was not possible because of the small sample size. More psychometric studies need to be carried out in order to further explore and increase the reliability, validity, generalizability, and specificity of the instrument.
Conclusions
The SCRS-a has been shown to have high validity when evaluated by professional experts.
It is an easy-to-use scale in the hands of carers of people with schizophrenia.
It demonstrates good reliability in terms of internal consistency and good convergent and discriminating validity.
References
Albacar-Riobóo, N. (2014). Atenció d'infermeria a la cuidadora principal de persones amb esquizofrènia: Valoració dels requisits d'autocura i de la salut mental positiva. Doctoral thesis, Rovira i Virgili University, Tarragona. [ Links ]
Brunet, I., Belzunegui, Á., & Pastor, I. (2000). Les tècniques d’investigació social i la seva aplicació. Tarragona: Rovira i Virgili University.
Cardoso, L., Verderoce Vieira, M., Malagutti Ricci, M. A., & Severino Mazza, R. (2012). Perspectivas atuais sobre a sobrecarga do cuidador em saúde mental. Revista da Escola de Enfermagem da USP, 46(2). Retrieved from: http://www.scielo.br/pdf/reeusp/v46n2/a33v46n2.pdf [ Links ]
Dinis, C., Rodrigues-Ferreira, T., & Carvalho, J.C. (2014). Familiar cuidador da pessoa com psicose: Satisfação de cuidados. Revista Portuguesa de Enfermagem de Saúde Mental (Spe. 1). Retrieved from: http://www.scielo.mec.pt/pdf/rpesm/nspe1/nspe1a10.pdf [ Links ]
European Parliament. Committee on the Environment, Public Health and Food Safety (2006). On improving the mental health of the population. Towards a strategy on mental health for the European. Retrieved from: http://www.europarl.europa.eu/sides/getDoc.do?pubRef=-//EP//NONSGML+REPORT+A6-2006-0249+0+DOC+PDF+V0//EN [ Links ]
Fayers, P. M., & Machin, D. (2000). Quality of life: Assessment, analysis and interpretation. London: John Wiley & Sons. [ Links ]
Ferré Grau, C., Rodero Sánchez, V., Vives Relats, C., & Cid Buera, D. (2008). El mundo del cuidador familiar. Una visión teórica y un modelo práctico para el cuidado. Tarragona: SILVA Editorial. [ Links ]
Karsch, U.M. (2003). Idosos dependentes: Famílias cuidadores. Cadernos de Saúde Pública, 19(3), 861-866. Retrieved from: http://www.scielosp.org/pdf/csp/v19n3/15890.pdf [ Links ]
Marriner-Tomey, A., & Alligoog, M. R. (2006). Nursing theorists and their work. (6th ed.). St. Louis: Mosby. [ Links ]
Miguel Ruiz, D. (2014). Valoración de la salud mental positiva y de los requisitos de autocuidado, en pacientes hospitalizados diagnosticados de esquizofrenia, según la teoría de enfermería de Dorothea Orem. Doctoral thesis, University of Barcelona, Barcelona, Spain. Retrieved from: http://www.tdx.cbuc.es/bitstream/handle/10803/275959/MDMR_TESIS.pdf?sequence=1 [ Links ]
Nunnally, J. C., & Bernstein, I. H. (1994). Psychometric theory (3rd ed.). New York: McGraw-Hill. [ Links ]
Orem, D. E. (2001). Nursing: Concepts of practice (6th ed.). St. Louis: Mosby. [ Links ]
Pereira da Mata, M. A., & Vega Rodríguez M. T. (2012). El cuidado no remunerado de mayores dependientes en el noreste de Portugal. Prisma Social, 8. Retrieved from: https://bibliotecadigital.ipb.pt/bitstream/10198/8396/1/01-cuidado-no-remunerado-portugal.pdf [ Links ]
Roldán Merino, J. F. (2011). Estudio métrico de la Escala de Requisitos de Autocuidado (ERA), basada en la teoría de D. Orem para pacientes diagnosticados de esquizofrenia. Doctoral thesis, University of Barcelona, Barcelona, Spain. Retrieved from: http://www.tdx.cat/bitstream/handle/10803/38012/JFRM_TESIS.pdf?sequence=1 [ Links ]
Roldán-Merino, J., Puig-Llobet, M., Lluch-Canut, T., Menarguez-Alcaina, M., Sabadell Gimeno, M., & QuestERA Working Group (2014). Validez de contenido de la Escala de Requisitos de Autocuidado (ERA) en personas con esquizofrenia. Revista Presencia, 10(19). [ Links ]
Roldán-Merino, J., Lluch-Canut, T., Menarguez-Alcaina, M., Foix-Sanjuan, A., Haro Abad, J. M., & Quest ERA Working Group (2014). Psychometric evaluation of a new instrument in Spanish to measure self-care requisites in patients with schizophrenia. Perspectives in Psychiatric Care, 50(2), 93-101. Retrieved from: http://onlinelibrary.wiley.com/doi/10.1111/ppc.12026/pdf [ Links ]
Sequeira, C. (2010). Cuidar de idosos com dependência física e mental. Lisbon: Lidel. [ Links ]
Touriño, R.., Inglott, R.., Baena, E., Fernández, J., & Álvarez, C. A. (2007). Guía de intervención familiar en la esquizofrenia. Barcelona: Glosa. [ Links ]
World Health Organization (1986). The Ottawa charter for health promotion. Retrieved from: http://www.who.int/healthpromotion/conferences/previous/ottawa/en/ [ Links ]
World Health Organization (2009). The Nairobi Global Conference on health promotion. Retrieved from: http://www.who.int/healthpromotion/conferences/7gchp/en/ [ Links ]
Acknowledgements
We would like to thank the participating centers as well as the nurses who have collaborated in data collection.
We also wish to acknowledge all the carers, and especially those who participated in the study, for their dedication and daily efforts. And the QuestERA Working Group: Alba AM, Argemí M, Blazquez MC, Bogas JL, Beltrán JJ, Cabello I, Casas I, Castro M, Cobo R, Feria I, Falco AM, Farreras P, Ferré C, Foix-Sanjuan A, Grumaches G, Guardia J, Haro JM, Herrero MP, Jettha C, Julia E, Menarguez M, Miguel D, Miguel J, Morcillo E, Marquez I, Moreno A, Montserrat M, Nuñez M, Ochoa S, Pino J del, Puig-Llobet M, Quilez J, Ramió A, Ramon J, Royo D, Sabadell M, Saez S, Santos A, Selva FJ, Senz M, Soler A, and Teba S.
Recebido a 28 de fevereiro de 2015
Aceite para publicação a 30 de maio de 2015
*This article has been drawn from the doctoral thesis of Núria Albacar-Riobóo: Nursing care of the main carer for people with schizophrenia: Evaluation of the self-care requirements for positive mental health. Rovira i Virgili University, Tarragona, Spain. Defended September, 2014.














