Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
GE-Portuguese Journal of Gastroenterology
versão impressa ISSN 2341-4545
GE Port J Gastroenterol vol.25 no.5 Lisboa out. 2018
https://doi.org/10.1159/000484939
CLINICAL CASE STUDY
A Rare Cause of Abdominal Pain in a Patient with Acute Necrotizing Pancreatitis
Uma Causa Rara de Dor Abdominal num Doente com Pancreatite Aguda Necrotizante
Joana C. Brancoa, Mariana F. Cardosoa, Luís Carvalho Lourençoa, Liliana Santosa, David Valadas Hortaa, Élia Coimbrab, Jorge A. Reisa
aServiço de Gastrenterologia, Hospital Professor Doutor Fernando Fonseca, Amadora, and
bServiço de Imagiologia, Hospital Cruz Vermelha, Lisbon, Portugal
* Corresponding author.
ABSTRACT
Introduction: Walled-off necrosis (WON) is a potentially lethal late complication of acute pancreatitis (AP) and occurs in less than 10% of AP cases. It can be located in or outside the pancreas. When infected, the mortality rate increases and can reach 100% if the collection is not drained. Its treatment is complex and includes, at the beginning, intravenous antibiotics, which permit sepsis control and a delay in the therapeutic intervention, like drainage. Nowadays, a minimally invasive approach is advised. Dependin on the location of the collection, computed tomography (CT)-guided drainage or endoscopic necrosectomy are the primary options, then complemented by surgical necrosectomy if needed. Infected WON of the abdominal wall has been rarely described in the literature and there is no report of any infection with Citrobacter freundii. Case: We present the case of a 61-year-old man with necrotizing AP complicated by WON of the left abdominal wall, infected with Citrobacter freundii that was successfully treated with CT-guided percutaneous drainage and intravenous antibiotics. Conclusion: Infected WON accounts for considerable mortality and its location in the abdominal wall is rare; it can be treated with antibiotics and CT-guided drainage with no need for further intervention.
Keywords: Acute pancreatitis, Walled-off necrosis, Computed tomography-guided percutaneous drainage, Citrobacter freundii infection, Abdominal pain
RESUMO
Introdução: A necrose pancreática coletada (NPC) é uma complicação potencialmente fatal da pancreatite aguda (PA) e ocorre em menos de 10% dos casos. Pode estar localizada dentro ou fora do pâncreas. Quando infetada, a mortalidade aumenta, podendo atingir os 100% se a coleção não for drenada. O seu tratamento é complexo e inclui, de início, antibioterapia intravenosa que permite o controlo da sepsis e um atraso na terapêutica de intervenção, como a drenagem. Atualmente é aconselhada uma abordagem minimamente invasiva. Dependendo da localização da coleção, a drenagem guiada por tomografia computorizada (TC) ou a necrosectomia endoscópica são as opções de primeira linha, posteriormente complementadas por necrosectomia cirúrgica, caso seja necessário. A NPC infetada na parede abdominal foi raramente descrita na literatura e não existe até ao momento nenhum caso de uma NPC infetada por Citrobacter freundii. Caso: Apresentamos o caso de um doente do sexo masculino de 61 anos com uma PA necrotizante complicada por NPC da parede abdominal esquerda, infetada por Citrobacter freundii, que foi tratada com sucesso através de drenagem percutânea guiada por TC e antibioterapia intravenosa. Conclusão: A NPC infetada condiciona mortalidade considerável e a sua localização na parede abdominal é rara; pode ser tratada através de antibioterapia e drenagem percutânea guiada por TC, sem necessidade de intervenção posterior.
Palavras-Chave: Pancreatite aguda, Necrose pancreática coletada,·Drenagem percutânea guiada por TC,·Infeção a Citrobacter freundii, Dor abdominal
Introduction
Walled-off necrosis (WON) is a rare and potentially lethal complication of acute pancreatitis (AP) which can occur in or outside the pancreatic tissue. WON is present in 1–9% of all AP cases [1] and it corresponds to an encapsulated collection of pancreatic and/or peripancreatic necrosis that occurs 4–6 weeks after the onset of necrotizing pancreatitis [2]. If left untreated, the mortality can reach 100% [1], mainly because of secondary infection. Currently, a minimally invasive and step-up approach is advised [3, 4], involving percutaneous drainage and endoscopic or surgical necrosectomy. Extrapancreatic WON is even rarer [1] with only a few cases being reported in the literature.
Case Report
We present the case of a 61-year-old black male, with arterial hypertension and no other relevant medical history, who was admitted to our unit for surveillance after an endoscopic retrograde cholangiopancreatography (ERCP), performed due to suspected choledocholithiasis.
The patient had been submitted to an open cholecystectomy 1 month earlier due to acute gangrenous cholecystitis, with intraoperative cholangiogram revealing a stone in the distal common bile duct (CBD). The stone was extracted, but due to maintained cholestasis, a magnetic resonance cholangiopancreatography was performed, showing a dilated CBD and two foci with 6–7 mm suspected to correspond to choledocholithiasis.
The patient underwent an ERCP with difficult cannulation of an intradiverticular papilla. Following the placement of a guidewire in Wirsungs duct, cannulation of the CBD was attempted with the double-wire technique, without success. Infundibulotomy was necessary and the cholangiogram revealed a dilated CBD but no evidence of choledocholithiasis. Biliary sphincterotomy was performed, followed by further exploration of the biliary ducts with a Dormias basket and no material came out. These findings were presumed to be in relation with biliary stone migration. At the end of the procedure, a 5-Fr, 7-cm-long pancreatic plastic stent was placed as well as administration of 100 mg rectal indomethacin, for postprocedure pancreatitis prophylaxis.
On the next day, the patient developed complaints of mild epigastric pain and intense pain in the left quadrants of the abdomen, poorly controlled by analgesics, and vomiting. At physical examination, he was conscious, febrile (38 ° C), normotensive but tachychardic (109 bpm), had a normal oxygen saturation, normal breath and cardiac sounds, and dolorous palpation at the upper and left quadrants of the abdomen but no signs of peritoneal irritation. The laboratory analysis showed leukocytosis of 11,100 per mm3, a C-reactive protein (CRP) of 7.09 mg/dL (normal value: <0.3 mg/dL), and a hyperamylasemia of 1,037 U/L, with normal blood urea nitrogen and creatinine.
A diagnosis of iatrogenic AP BISAP 3 (age, systemic inflammatory response syndrome, and pleural effusion) was assumed and he was initially treated with aggressive fluidotherapy, analgesics, and nil per mouth. Nausea improved and oral intake was resumed. Cholestatic enzymes normalized and this alteration was assumed to have occurred in the context of biliary stone migration. However, due to maintained abdominal pain, fever, and a CRP rise to 32.7 mg/dL 72 h later, an abdominal computed tomography (CT) was asked, showing necrosis of the pancreatic tail, acute necrotic collections of both parietocolic gutters, perisplenic and perihepatic spaces and anterior pararenal fascia, and subcutaneous edema of the left abdominal wall. Urine and blood cultures were both negative.
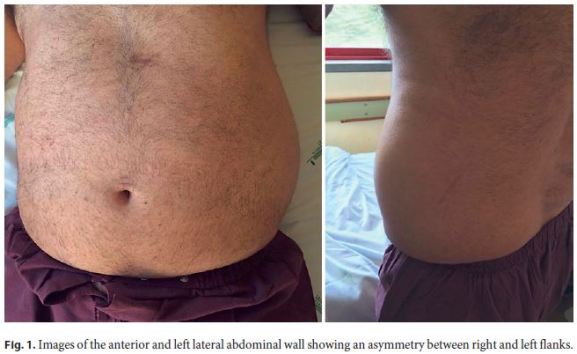
Towards suspicion of infected necrosis, meropenem 1 g q8h was started. Despite initial improvement, 2 weeks later, the left flank pain worsened, fever came back (with temperatures ranging between 38.3 and 38.5 ° C), and inflammatory parameters (IP) rose again (with a maximum CRP of 8 mg/dL). At this time, a mass in the left flank was noticed (Fig. 1). Abdominal ultrasonography and CT were performed and identified a well-delimitated heterogeneous subcutaneous collection in the left abdominal wall (9 × 7 × 6 cm). Vancomycin was added to meropenem empirically, as urine and blood cultures were again both negative.
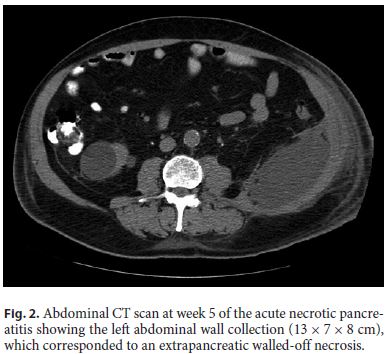
Even though there was a favorable response in the beginning, 10 days later, there was a new fever peak, of 38.6 ° C, and IP rose again (with a maximum CRP of 7 mg/dL). Abdominal CT showed increase in the left abdominal wall collection size (13 × 7 × 8 cm), corresponding to an extrapancreatic WON (Fig. 2).
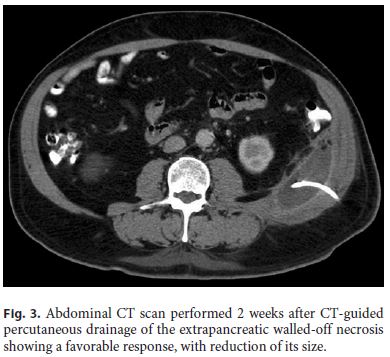
The patient was submitted to CT-guided percutaneous drainage of the collection with placement of an 8.5-Fr pig-tail catheter. Citrobacter freundii was isolated in the purulent fluid, susceptible to piperacillin/tazobactam, which was administered for 14 days. Three-times a day irrigation and washing of the WON with a 0.9% saline solution was performed. The patient reported symptomatic improvement, IP normalized, and the collection regressed (Fig. 3), so the drain was removed 15 days after its insertion and the patient was discharged.
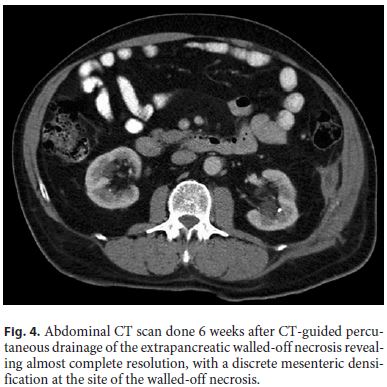
A month later, radiologic imaging confirmed persistent resolution of the collection (Fig. 4).
Discussion
Acute necrotizing pancreatitis (ANP) is reported to occur in 5–20% of all episodes of AP [1, 2]. The natural history of intra-/peripancreatic necrosis is variable: it may remain solid or liquefy, remain sterile or become infected, persist or disappear [2].
Local complications of AP should be suspected when there is persistence or recurrence of abdominal pain, increases in organ dysfunction, and/or the development of clinical signs of sepsis (fever or leukocytosis) [2], as was the case in our patient. In the context of ANP, local complications are acute necrotic collections and WON. Both can be intra- and/or extrapancreatic, be located in single or multiple sites, and vary in size; they differ according to the time of development after the onset of ANP – WON being the late complication, after 4–6 weeks of the initial episode – and to morphologic characteristics, related to that time. The term pancreatic abscess should be abandoned, according to the 2012 Revised Atlanta Classification [2].
WON occurs in 1–9% of all AP cases [1] and consists of necrotic tissue contained within an enhancing wall of reactive tissue. It is a mature, encapsulated collection of pancreatic and/or peripancreatic necrosis and has a welldefined inflammatory wall [2]. The probability of developing WON can be predicted according to Balthazar and Ransons radiographic staging criteria; grade E, the most severe, is defined by the presence of two or more fluid collections or gas within the pancreas or peripancreatic inflammation, and the probability of developing WON is 57% [5], as happened in this case report.
The mortality rate from sterile ANP is 10% and rises to 30% when infection is present [6], and WON, especially when infected, is a life-threatening adverse event of AP.
Another interesting peculiarity of this case was the infectious agent of the WON. Colonic translocation of bacterial flora seems to be the responsible for necrotic pancreatic infection [7], and the most typical organisms are gut flora associated and Candida spp. [8]. Citrobacter freundii are gram-negative bacilli and constitute an infrequent etiology of infection in general [9], responsible for only 0.8% of gram-negative infections and more commonly cause urinary tract infections [10]. The antimicrobial susceptibility varies and normally it can be treated with a single antibiotic [9] as in this case. The mortality rate of Citrobacter spp. infections is 6.8% [11].
Ideally, therapeutic intervention is delayed to allow maturation of WON [12] and antibiotics may facilitate this delay [13]. The PANTER study demonstrated that a step-up approach, starting with CT-guided percutaneous drain placement, was superior to up-front open surgical necrosectomy, demonstrating the value of a minimally invasive approach [4]. It is of note that 35% of patients who established necrotic collections did not require any further intervention over simple small-diameter percutaneous catheter drainage [4]. However, they often fail drainage and ultimately require further intervention, either endoscopic or surgical. A gold-standard minimally invasive management algorithm would take into accountthe clinical condition of the patient, anatomical location of the collection, and expertise in the techniques. Many patients may benefit from the use of a multimodal approach with more than one technique [13]. In general, lateral collections and those extending behind the colon are usually better approached from the left or right flank whereas those medial collections where a percutaneous route is compromised by overlying bowel, spleen, or liver, may be better approached endoscopically [13].
In the reported case, an antibiotic known to penetrate the necrotic pancreatic parenchyma (meropenem, a carbapenem) was started as there was no clinical improvement within the first 2 weeks and as soon as the patient showed signs of sepsis, in order to allow necrosis organization. We pursued the step-up approach and used the percutaneous route as he had a lateral WON, in the left flank, and in this case, it was sufficient to reach therapeutic success.
References
1 Stamatakos M, Stefanaki C, Kontzoglou K, Stergiopoulos S, Giannopoulos G, Safioleas M: Walled-off pancreatic necrosis. World J Gastroenterol 2010;16:1707–1712. [ Links ]
2 Banks PA, Bollen TL, Derveni C, Gooszen HG, Johnson CD, Sarr MG, Tsiotos GG, Vege SS; Acute Pancreatitis Classification Working Group: Classification of acute pancreatitis – 2012: revision of the Atlanta classification and definitions by international consensus. Gut 2013;62:102–111. [ Links ]
3 Haghshenasskashani A, Laurence J M, Kwan V, et al: Endoscopic necrosectomy of pancreatic necrosis: a systematic review. Surg Endosc 2011;25:3724–3730. [ Links ]
4 Balthazar EJ, Robinson DL, Megibow AJ, Ranson JH: Acute pancreatitis: value of CT in establishing prognosis. Radiology 1990;174:331–336. [ Links ]
5 Kumar N, Conwell DL, Thompson CC: Direct endoscopic necrosectomy versus step-up approach for walled-off pancreatic necrosis: comparison of clinical outcome and health care utilization. Pancreas 2014;43:1334–1339. [ Links ]
6 Dugernier T, Dewaele J, Laterre PF: Current surgical management of acute pancreatitis. Acta Chir Belg 2006;106:165–171. [ Links ]
7 van Minnen LP, Nieuwenhuijs VB, de Bruijn MT, Verheem A, Visser MR, van Dijk JE, Akkermans LM, Gooszen HG: Effects of subtotal colectomy on bacterial translocation during experimental acute pancreatitis. Pancreas 2006;32:110–114. [ Links ]
8 Dragonetti GC, Licht H, Rubin W: Pancreatitis. Evaluation and treatment. Prim Care 1996;23:525–534. [ Links ]
9 Samonis G, Karageorgopoulos DE, Kofteridis DP, Matthaiou DK, Sidiropoulou V, Maraki S, et al: Citrobacter infections in a general hospital: characteristics and outcomes. Eur J Clin Microbiol Infect Dis 2009;28:61–68. [ Links ]
10 Jones RN, Jenkins SG, Hoban DJ, Pfaller MA, Ramphal R: In vitro efficacy of six cephalosporins tested against Enterobacteriaceae isolated at 38 North American medical centres participating in the SENTRY Antimicrobial Surveillance Program, 1997–1998. Int J Antimicrob Agents 2000;15:111–118. [ Links ]
11 Mohanty S, Singhal R, Sood S, Dhawan B, Kapil A, Das BK: Citrobacter infections in a tertiary care hospital in Northern India. J Infect 2007;54:58–64. [ Links ]
12 Mathers B, Moyer M, Mathew A, Dye C, Levenick J, Gusani N, et al: Percutaneous debridement and washout of walled-off abdominal abscess and necrosis using flexible endoscopy: a large single-center experience. Endosc Int Open 2016;4:E102–E106. [ Links ]
13 Logue J, Carter C: Minimally Invasive Necrosectomy Techniques in Severe Acute Pancreatitis: Role of Percutaneous Necrosectomy and Video-Assisted Retroperitoneal Debridement. Gastroenterology Research and Practice Volume 2015, Article ID 693040, 6 pages. [ Links ]
Statement of Ethics
Informed consent of the patient was obtained.
Disclosure Statement
The authors have no conflicts of interest to declare.
* Corresponding author.
Dr. Joana C. Branco
Serviço de Gastrenterologia
Hospital Professor Doutor Fernando Fonseca – IC 19
PT–2720-276 Amadora (Portugal)
E-Mail cbranco.joana@gmail.com
Received: August 24, 2017; Accepted after revision: November 3, 2017














