Serviços Personalizados
Journal
Artigo
Indicadores
Links relacionados
Compartilhar
GE-Portuguese Journal of Gastroenterology
versão impressa ISSN 2341-4545
GE Port J Gastroenterol vol.27 no.5 Lisboa out. 2020
https://doi.org/10.1159/000505580
CLINICAL CASE STUDY
Cytomegalovirus Colitis Mimicking Rectal Tumour in an Undiagnosed HIV Patient
Colite a CMV mimetizando tumor rectal num doente com VIH não diagnosticado
Manuel Rocha, Verónica Borges, Guilherme Simões, Sara Santos, Verónica Gamelas, Carlos Bernardes
Gastroenterology Department, Centro Hospitalar Universitário de Lisboa Central, Lisbon, Portugal
* Corresponding author.
ABSTRACT
Introduction: Cytomegalovirus (CMV) is the most common opportunistic agent in HIV-infected patients. It can affect the entire gastrointestinal tract, but frequently involves the oesophagus and the colon. Case Report: We report the case of a 70-year-old female, ultimately diagnosed with HIV infection, whose inaugural clinical manifestation was CMV colitis with endoscopic findings resembling a rectal tumour in which initial histological evaluation was not able to provide a proper diagnosis. Discussion/Conclusion: Since clinical presentation is variable and histopathological yield without immunohistochemical analysis is poor, recognizing CMV infection in the absence of known risk factors may be difficult. It is crucial to consider this entity with suspicious lesions or when initial evaluation, either clinical or histopathological, is inconclusive, thus avoiding potentially debilitating and superfluous treatment or life-threatening complications.
Keywords: CMV colitis,Rectal tumour, HIV infection, Coinfection
RESUMO
Introdução: O citomegalovírus (CMV) é o agente oportunista mais comum nos doentes com infeção pelo vírus da imunodeficiência humana (VIH). Pode afetar todo o trato gastrointestinal, mas frequentemente envolve o esófago e o cólon. Caso Clínico: Os autores apresentam o caso de uma doente do sexo feminino com 70 anos, com diagnóstico final de infeção por VIH, cuja manifestação clínica inaugural foi colite a CMV, com achados endoscópicos iniciais mimetizando um tumor rectal. Discussão/Conclusão: Uma vez que a apresentação clínica é variável e a rentabilidade da análise histopatológica sem imunohistoquímica é baixa, o reconhecimento da infeção por CMV na ausência de fatores de risco pode ser difícil. É crucial considerar esta entidade perante lesões suspeitas ou quando a avaliação inicial, clínica ou histopatológica, for inconclusiva, de forma a evitar potenciais terapêuticas debilitantes e/ou supérfluas bem como complicações graves.
Palavras-Chave: Colite CMV, Tumor rectal,Infecção VIH, Coinfecção
Introduction
Cytomegalovirus (CMV) is the most common opportunistic agent in HIV (human immunodeficiency virus)- infected patients and in up to 25% of cases it provides the basis for the initial clinical diagnosis of acquired immunodeficiency syndrome [1]. CMV can affect the entire gastrointestinal tract, but frequently involves the oesophagus and the colon [2]. In fact, colitis is the main extraocular manifestation of CMV disease in HIV-infected patients [3]. It is always important to be aware of this entity and diagnose it promptly, as life-threatening complications can occur, such as colonic perforation or gastrointestinal tract bleeding [4]. However, CMV infection diagnosis can be difficult, mainly if no risk factors are suspected (e.g., HIV infection, prolonged immunosuppression) or if its clinical suspicion was not raised for pathologists.
Case Report
Here we present the case of a 70-year-old, melanodermic, female patient who is a native of Cape Verde but has been resident in Portugal since 1997. She had previous history of arterial hypertension, medicated with lisinopril and amlodipine. The patient was referred from the Surgery Department because of an ulcerated rectal tumour with inconclusive histopathology on biopsies obtained from a previous colonoscopy. She also complained of anorexia and weight loss that was not quantified. The physical examination was unremarkable. The blood tests showed a microcytic and hypochromic anaemia (Hb 8.5 g/dL, MCV 72.6 fL, MCH 24.3 pg) and elevation of C-reactive protein (39.6 mg/L). The colonoscopy was repeated, which revealed irregular and ulcerated mucosa, with necrotic areas, between 10 and 18 cm from the anal verge (Fig. 1). On hepatic flexure, we found another ulcerated area involving one third of the luminal circumference (Fig. 2). Based on these findings (two ulcerated segments in the colon, blood test changes, and previous inconclusive biopsies), we requested CMV immunohistochemistry (IHC) on colonic samples, which were positive for its presence (Fig. 3). The patient was prescribed valganciclovir (1 g, 3 times daily) and was tested for HIV infection, which was also positive. When questioned at this stage, the patient confessed that her husband was diagnosed with HIV infection a few months earlier, information that she had not previously disclosed. There was clinical and endoscopic improvement after the valganciclovir therapy (21 days). The patient was referred to an immunodeficiency consultant and started a highly active antiretroviral therapy with a good response.
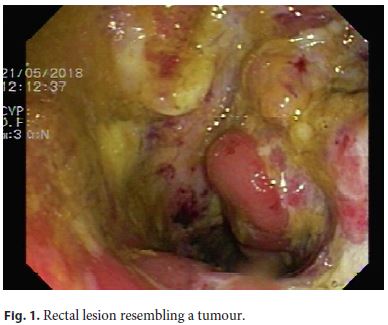
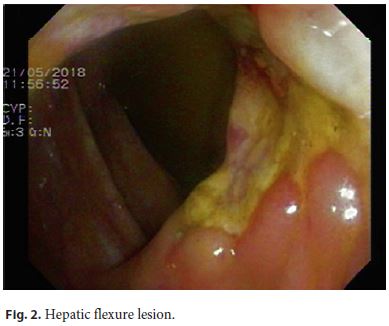
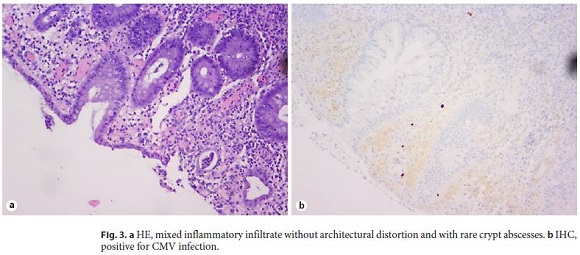
Discussion
This is a case of HIV infection with an initial clinical presentation of CMV colitis. In fact, the index colonoscopy showed only an ulcerated lesion in the rectum that resembled a malignant tumour. Several cases of CMV colorectal pseudotumors are reported in the literature [1, 5], and it is important to be aware of this condition, mainly in patients with risk factors associated with immunosuppression.
To identify CMV colitis, colonoscopy is preferred over flexible sigmoidoscopy, as more than one third of affected patients have gross disease restricted to proximal regions of the colon. Furthermore, it is also important to take multiple biopsy specimens as viral inclusions are most often present in the endothelial cells of the deeper layers of the bowel wall [2]. Histopathological examination of colorectal mucosal biopsies, stained with haematoxylin and eosin (HE), is a specific method (92–100%) but often insensitive (10–87%). IHC has been found to be more sensitive than HE staining (78–93%) but is not routinely used – only if there is a clinical suspicion raised by the clinician [6]. Another diagnostic tool is tissue polymerase chain reaction (PCR), which allows for rapid results and compared to IHC is more sensitive, with a high negative predictive value [7]. In fact, the European Crohn’s and Colitis Organisation recommend tissue PCR or IHC as the methods of choice for diagnosing CMV colitis [8].
Concerning treatment, all patients with CMV gastrointestinal disease should receive induction therapy with an antiviral agent for 3–6 weeks or until signs and symptoms have resolved. The options are ganciclovir, foscarnet (both intravenous), or oral valganciclovir (if the patient can absorb and tolerate oral therapy and/or in mild disease). Antiretroviral therapy should be initiated as soon as CMV retinitis has been excluded and the patient can tolerate oral medication. If the patient is already on antiretroviral therapy, this should be continued. Chronic maintenance therapy is not recommended for CMV gastrointestinal disease unless there is concurrent retinitis or recurrent gastrointestinal disease after induction therapy has been discontinued [9].
Thus, this case illustrates the importance of considering CMV infection when we face colorectal lesions that are suspicious or when the initial diagnosis (clinical or pathological) is not conclusive.
References
1 Lima M, Matos AP, Ramalho M. Cytomegalovirus pseudotumor of the colon in an HIV patient. Radiol Case Rep. 2018 Nov;14(2):273–7.
2 Bhaijee F, Subramony C, Tang SJ, Pepper DJ. Human immunodeficiency virus-associated gastrointestinal disease: common endoscopic biopsy diagnoses. Pathol Res Int. 2011 Apr;2011:247923. [ Links ]
3 Yoshida S, Mori N, Honda M. Cytomegalovirus colitis in a patient with HIV infection shortly after initiation of antiretroviral therapy. IDCases. 2019 May;17:e00552. [ Links ]
4 Barling DR, Tucker S, Varia H, et al. Large bowel perforation secondary to CMV colitis: an unusual primary presentation of HIV infection. BMJ Case Rep. 2016;2016:bcr2016217221. [ Links ]
5 Lionaki S, Altanis N, Papaxoinis K, Delladetsima I, Daikos G, Boletis JN. A cytomegalovirus-related pseudotumor in the colon of a renal transplant recipient shrunk by antiviral therapy. Transplantation. 2015 Jul;99(7):e46–7.
6 Ayre K, Warren BF, Jeffery K, Travis SP. The role of CMV in steroid-resistant ulcerative colitis: a systematic review. J Crohn’s Colitis. 2009 Sep;3(3):141–8.
7 Tun GS, Raza M, Hale MF, Lobo AJ. Polymerase chain reaction for detection of mucosal cytomegalovirus infection in patients with acute ulcerative colitis. Ann Gastroenterol. 2019 Jan-Feb;32(1):81–7.
8 Rahier JF, Magro F, Abreu C, Armuzzi A, Ben-Horin S, Chowers Y, et al.; European Crohn’s and Colitis Organisation (ECCO). Second European evidence-based consensus on the prevention, diagnosis and management of opportunistic infections in inflammatory bowel disease. J Crohn’s Colitis. 2014 Jun;8(6):443–68.
9 Panel on Opportunistic Infections in Adults and Adolescents with HIV. Guidelines for the prevention and treatment of opportunistic infections in adults and adolescents with HIV: recommendations from the Centers for Disease Control and Prevention, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. Available at: https://aidsinfo.nih.gov/contentfiles/lvguidelines/adult_oi.pdf (accessed July 01, 2019). [ Links ]
Statement of Ethics
The authors declare that the subject gave her written informed consent to publish this case.
Disclosure Statement
The authors have no conflicts of interest to disclose.
Funding Sources
The authors have no funding sources to declare.
* Corresponding author.
Manuel Rocha
Gastroenterology Department, Centro Hospitalar Universitário de Lisboa Central
Alameda de Santo António dos Capuchos
PT–1169-050 Lisbon (Portugal)
Received: October 19, 2019; Accepted: December 9, 2019
Author Contributions
All authors contributed to the literature review. Manuel Rocha prepared the manuscript. Verónica Borges, Guilherme Simões, Sara Santos, Verónica Gamelas, and Carlos Bernardes revised the manuscript.














