Espondilolise e espondilolistese ístmica de grau I no adolescente: Análise retrospectiva de 30 casos
Vânia OliveiraI, II, III; Ricardo Rodrigues-PintoI, II, III; Luís CostaI, II, III; Ângelo EncarnaçãoI, II, III; Armando CamposI, II, III; António OliveiraI, II, III
I. Instituto de Ciências Biomédicas Abel Salazar. Universidade do Porto. Portugal.
II. Serviço de Ortopedia e Traumatologia. Centro Hospitalar do Porto. Hospital de Santo António. Porto. Portugal.
III. Serviço de Radiologia. Centro Hospitalar do Porto. Hospital de Santo António. Portugal.
RESUMO
]]> Objectivo: a espondilolise e a espondilolistese ístmica grau I são causas de lombalgia nos adolescentes e associam-se a fractura de fadiga da pars interarticularis por movimentos repetidos de hiperextensão.Na literatura não existe consenso quanto aos benefícios do tratamento cirúrgico nestes doentes, muitas vezes atletas, e a controvérsia prolonga-se sobre qual a melhor técnica cirúrgica.
Os autores descrevem a técnica cirúrgica que sistematicamente utilizam e analisam os resultados obtidos.
Material e métodos: retrospectivamente, entre 2004 e 2013, foram avaliados 30 adolescentes, 12 com lise ístmica e 18 com espondilolistese ístmica grau I, operados pelo mesmo cirurgião. A reconstituição ístmica foi feita com autoenxerto de ilíaco e fixação pedicular posterior temporária.
Avalia-se a taxa de consolidação, complicações, dor (VAS), função (ODI) e o grau de satisfação.
Resultados: a idade média foi 16.3 anos (13-18) e o seguimento 23.5 meses (14-48).
Ocorreu consolidação em 100% dos casos. O VAS médio reduziu de 7.48 para 0.38 (p<0.0001) e, funcionalmente, o ODI médio melhorou de 38.55% para 1.59% (p<0.0001), de disfunção moderada para mínima.
A todos os doentes foi retirado o material após 1 ano de reconstituição ístmica. No total, 63.3% dos doentes eram desportistas e todos retomaram o nível prévio. Não se verificou progressão da listese nem complicações significativas. Os doentes encontram-se satisfeitos e repetiriam o tratamento.
Conclusão: as técnicas de artrodese obtêm bons resultados clínicos mas implicam perda de mobilidade segmentar e doença do nível adjacente. Comparativamente com técnicas dinâmicas, a técnica preconizada pelos autores permite não só a reconstituição ístmica eficaz como revela resultados superiores a médio prazo, o que supera a necessidade de segunda intervenção para extração do material.
A reconstituição ístmica com autoenxerto e fixação pedicular posterior temporária na espondilolise ou espondilolistese ístmica grau I obteve excelentes resultados clínicos e elevada taxa de consolidação. Esta técnica é defendida pelos autores mesmo em atletas de alta competição.
]]> Palavras chave: Lise ístmica, espondilolise, espondilolistese ístmica, lombalgia, adolescente, reconstituição ístmica, desportista.
ABSTRACT
Aim: the spondylolysis and grade I isthmic spondylolisthesis are causes of low back pain in adolescents. Both are associated with fatigue fracture of the pars interarticularis, induced by repeated hyperextension movements.
In the literature there is no consensus about the benefits of the surgical treatment in these patients, often athletes, and the controversy extends to the best surgical technique to perform.
The authors describe the surgical technique they systematically use and analyse outcome.
Material and methods: from 2004 and 2013, retrospectively were analysed 30 adolescents, 12 spondylolysis and 18 grade I isthmic spondylolisthesis, operated by the same surgeon for a isthmic reconstruction with iliac autograft and temporary posterior pedicle fixation.
The following parameters were evaluated: isthmus reconstitution, complications, pain (VAS), function (ODI) and patients’ satisfaction.
Results: the mean age was 16.3 years (range 13-18) and follow-up 23.5 months (range 14-48).
Consolidation occurred in 100% of cases. The VAS decreased from 7.48 to 0.38 (p<0.0001) and ODI improved from 38.55% to 1.59% (p<0.0001), moderate to minimal disability.
]]> The instrumentation was removed after one year post isthmic reconstitution in all patients.In total, 63.3% of patients were athletes and all of them returned to their previous competition level.
There was no listhesis progression or significant complications.
Patients are satisfied and would repeat treatment.
Conclusion: the fusion techniques present good clinical results but are associated with loss of segment mobility and adjacent level disease. Compared with dynamic techniques, this technique recommended by the authors enables not only effective isthmic reconstitution as shows superior clinical outcomes in the medium term, which overcomes the need for second surgery to remove instrumentation.
The isthmic reconstitution with autograft and temporary posterior pedicle fixation in spondylolysis or isthmic spondylolisthesis grade I obtained excellent clinical results and high rate of bone defect healing. The authors advocate this technique even in elite athletes.
Key words: Isthmus lysis, spondylolysis, isthmic spondylolisthesis, back pain, adolescents, isthmic reconstitution, athletes.
INTRODUÇÃO
A lise ístmica ou espondilolise resulta do defeito uni ou bilateral da pars interarticularis. A espondilolistese ístmica ou tipo II segundo Wiltse1 corresponde a uma translação do corpo vertebral sobre o caudal na presença de defeito bilateral da pars, sendo esta translação de 0-25% no grau I de Meyerding. A etiologia é multifactorial: mecânica, hereditária e hormonal. Ambas são as causas mais frequentes de lombalgia em crianças e adolescentes com idade superior a 10 anos2,3,4. Associam-se a fractura de fadiga da pars por movimentos repetidos de hiperextensão, como ocorre em algumas atividades desportivas.
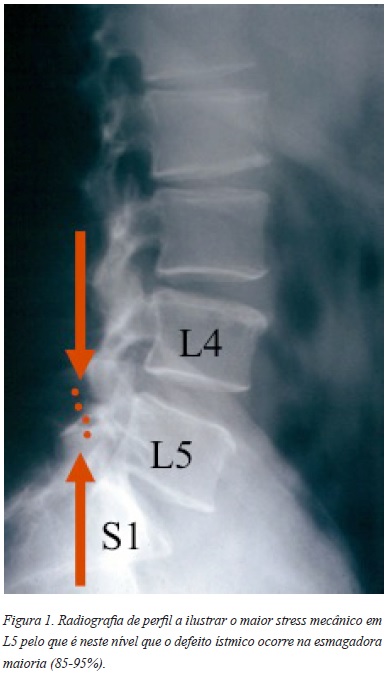
]]> A incidência da espondilolise na raça causasiana está avaliada de 3-6%5,6 sendo mais prevalente em jovens atletas7. Na esmagadora maioria (85-95%) o defeito é bilateral na vértebra L5, sendo L4 a segunda mais frequente5,6,8-10. Isto deve-se ao facto de a maior carga com movimentos de flexão/extensão se verificar no nível L5-S1 e, por isso, sofrer de elevado stress mecânico (Figura 1)11. São factores de risco a história familiar, etnia e outras anomalias na coluna vertebral como espinha bífida oculta5,6,10.

Na lise ístmica e espondilolistese grau I a progressão da listese é rara após a maturidade óssea e, na literatura, não está definido qual a progressão considerada significativa6,7. O estudo de Frennered et al.12 verifica progressão >=20% em apenas 4% com idade inferior a 16 e com 7 anos de seguimento. Não foi possível correlacionar a progressão da listese com outras variáveis como manutenção do desporto nem com achados radiológicos, excepto com a espinha bífida12,13. Existe consenso nos estudos publicados em que a progressão ocorre predominantemente no surto de crescimento da puberdade13.
Nos casos sintomáticos, a lombalgia é exacerbada com a hiperextensão, pode ser constatada uma postura hiperlordótica e contractura da fáscia toracolombar. As alterações neurológicas ou radiculopatia são raras nesta faixa etária e nos casos mais graves pode verificar-se retração dos isquiotibiais, deformidade (step-off) na junção lombossagrada e desenvolver-se escoliose.
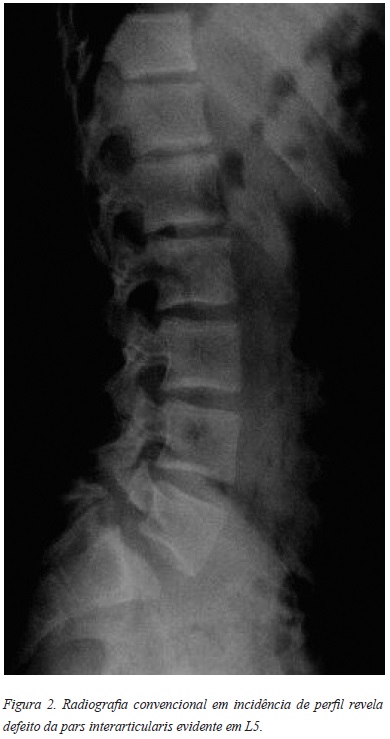
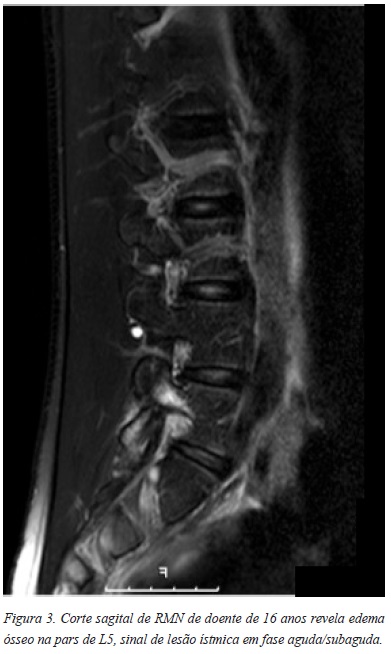
O diagnóstico faz-se com radiografias convencionais (Figura 2), quando é visível o defeito da pars. O sinal patognomónico “scotty dog” é visível nas incidências oblíquas. A cintigrafia óssea e a TAC são frequentemente utilizados para completar o estudo diagnóstico sendo que a PET Scan é o exame mais sensível. Na fase aguda/subaguda, a RMN pode revelar precocemente sinais de lesão da pars, com presença de edema ósseo (Figura 3)7.
]]>
Na literatura não existe consenso quanto aos benefícios do tratamento cirúrgico nestes doentes que são muitas vezes atletas e não pretendem terminar a carreira ou diminuir a performance. A controvérsia prolonga-se sobre qual a melhor técnica cirúrgica.
De facto, nos poucos estudos publicados, verifica-se que a maioria defende o tratamento conservador que abrange o repouso com interrupção temporária do desporto e uso de ortótese até 6 meses, bem como reabilitação fisiátrica. A reparação óssea espontânea pode ocorrer na espondilolise em fase precoce e maioritariamente com defeito unilateral da pars8,14. No entanto, os resultados clínicos e retorno às atividades não se correlacionam com a consolidação óssea, verificando-se bons a excelentes resultados em 78-96% dos casos, com 25-37% de reparação óssea8,15. Pizzutillo et al.16 obtiveram alívio da dor em 70% dos casos.
A opção pelo tratamento cirúrgico verifica-se, geralmente, nos casos sintomáticos resistentes às atitudes conservadoras, progressão da espondilolistese, ou alterações neurológicas. As técnicas cirúrgicas utilizadas são díspares, desde a artrodese até à reparação direta do defeito por técnicas diversas. Estão descritas na literatura variadas técnicas cirúrgicas para esta patologia, com bons resultados clínicos globais, continuando problemática a indicação cirúrgica.
Os autores descrevem a técnica cirúrgica que sistematicamente utilizam e analisam os resultados obtidos.
]]> MATERIAL E MÉTODOS
O estudo retrospectivo entre 2004 e 2013, engloba 30 adolescentes: 12 com lise ístmica e 18 com espondilolistese ístmica grau I. O defeito da pars ocorreu bilateralmente em 29 casos (96.7%) e na esmagadora maioria em L5 (86.7%).
Todos os doentes operados foram submetidos a tratamento conservador prévio, que não foi eficaz. O tempo de evolução dos sintomas variou entre 6 e 12 meses, desde o início até à intervenção cirúrgica.
A reconstituição ístmica foi feita com autoenxerto de ilíaco, após preparação do defeito da pars, e fixação pedicular posterior temporária a um nível (vértebra atingida e nível caudal) ou, em 2 casos, a 2 níveis uma vez que o defeito ocorreu em L4 e L5. Todos os doentes foram operados pelo mesmo cirurgião.
Foram avaliados os seguintes parâmetros: consolidação, complicações, dor (VAS), função (ODI) e grau de satisfação.
A fusão óssea foi assumida imagiologicamente quando pontes ósseas ou calo ósseo evidentes nas radiografias de controlo em todos os doentes. Em alguns casos associou-se a realização de TAC como confirmação sendo concordante em todos os doentes com a análise radiológica.
Os resultados foram analisados com o IBM SPSS Statistics 20.0 (Teste t).
RESULTADOS
A Tabela 1 apresenta os resultados obtidos. A distribuição por género foi simétrica, em média com idade de 16.3 anos (13-18) e seguimento de 23.5 meses (14-48).
]]>
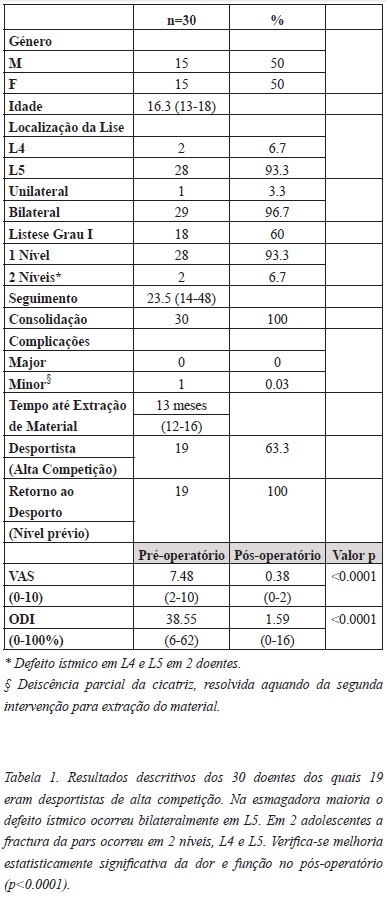
Atingiu-se a correção do defeito com consolidação em 100% dos casos (Figura 4).
Verifica-se redução significativa da dor com VAS médio de 7.48 para 0.38 (p<0.0001). Também funcionalmente o ODI melhorou muito significativamente de 38.55% para 1.59% (p<0.0001), de disfunção moderada para mínima.
]]> No total, 63.3% dos doentes eram desportistas de competição (ciclismo, natação, futebol, basquetebol, voleibol, ginástica e Ballet). Todos retomaram o nível prévio após a intervenção cirúrgica.A todos os doentes foi retirado o material após completar 1 ano da reconstituição ístmica (Figura 5), tendo sido em média aos 13 meses (12-16).
Não se verificou progressão da listese em nenhum caso e não se registaram complicações major como infecção, pseudartrose ou fractura/desmontagem da instrumentação. Ocorreu, no entanto, uma complicação minor (0.03%) em doente com deiscência parcial da ferida operatória resolvida aquando da segunda intervenção para extração do material, com correção da cicatriz.
Os doentes encontram-se satisfeitos e 100% repetiriam o tratamento.
DISCUSSÃO
]]> Existem poucos estudos publicados e com elevada heterogeneidade. Sendo a maioria atletas, o tratamento conservador exclusivo, implica a interrupção prolongada da atividade desportiva, frequentemente em fase de crescimento exponencial correspondente à puberdade e, por isso, com possível comprometimento da carreira e sucesso desportivos.Os estudos publicados raramente relatam o retorno desportivo e, quando o reportam, este ocorre a níveis variáveis, sem especificar se ao nível prévio.
As técnicas de artrodese obtêm bons resultados clínicos mas implicam perda de mobilidade no segmento, sobrecarga e doença do nível adjacente que se estimou ocorrer em 36.1%17. No estudo de Audat et al.17 após artrodese circunferencial (PLIF), com ou sem redução, a consolidação ocorreu em 50% após 1 ano e aumentou até aos 3 anos de seguimento, sendo que em nenhum caso se verificou antes dos 6 meses. Funcionalmente, o ODI melhorou gradualmente até aos 3 anos passando de 52% para 15% no grupo sem redução e de 50% para 4% quando redução associada17. Verifica-se também que após artrodese os adolescentes retomam o desporto numa decisão caso a caso e na dependência do cirurgião, frequentemente após 1 ano da fusão. No caso de desporto de colisão ou contacto, 30% dos cirurgiões defendem a não retoma18,19.
As técnicas de reconstituição têm a vantagem de preservar a mobilidade segmentar e, por isso, sem doença do nível adjacente associada.
Na literatura estão descritas técnicas diversas de reparação direta do defeito, com recurso a sistemas estabilizadores para promover a consolidação do defeito ósseo no istmo como o método do parafuso de compressão de Buck20, cerclage entre apófise espinhosa e transversas, técnica de Scott21-23, uso combinado de parafusos pediculares e fios ou cabos aço24, parafusos pediculares e ganchos25,26, ou parafusos pediculares e sistema dinâmico de barra em V27-29. O sucesso destas técnicas é variável e nem todos especificam qual o enxerto ósseo utilizado. O parafuso de compressão de Buck20 atravessa o istmo e limita a quantidade de enxerto comprometendo assim a sua reconstituição. No estudo de Johnson e Thompson23, a técnica de Scott obteve resultados satisfatórios em 90.9% dos casos, a reconstituição eficaz ocorreu em 77.2% com registo de complicações em 10 dos 22 casos. A dificuldade desta técnica reside em conferir compressão adequada no istmo sem conduzir à fractura da lâmina22,23. A combinação de parafusos pediculares e ganchos ou barra em V atingem maior estabilidade26,29. O sistema com barra em V foi primariamente descrito por Gillet et al27 que, tal como posteriormente Koptan et al.30 contraindicam esta técnica na presença de discopatia degenerativa. Nos estudos publicados verifica-se que há alívio da dor e preserva a altura do disco, previne a progressão de translação anterior e mantém a elasticidade dinâmica sem alterar a amplitude de movimento flexão/extensão27,29. No estudo de Chen et al.29 a redução da dor no pós-operatório foi significativa com VAS médio de 3.04 aos 35 meses em média de seguimento, e a amplitude de flexão/extensão não variou. No entanto, a consolidação ocorreu em apenas 66.67% dos casos e em média aos 6 meses, um caso apresentou reabsorção óssea no nível L5-S1, e não avaliaram especificamente atletas nem o retorno à atividade desportiva.
Sairyo et al.31 demonstraram que o sucesso da reconstituição ístmica tem vantagens mecânicas com proteção da doença do disco adjacente, um facto importante nesta população jovem.
Neste contexto, a técnica de reconstituição ístmica utilizada pelos autores com fixação pedicular posterior temporária apresenta excelentes resultados clínicos e funcionais, sem complicações significativas e com retorno ao nível desportivo prévio quando atletas. Implica, no entanto, uma segunda intervenção cirúrgica para extração do material. Este estudo tem limitações inerentes a ser retrospectivo e a avaliação da consolidação não recorreu à tomografia computorizada em todos os doentes, baseando-se nas pontes ósseas radiologicamente evidentes no rx convencional. O recurso a TAC foi reservado para os casos em que o rx convencional não era conclusivo quanto à consolidação indiscutível da pars. A concordância inter-observador em análise cega foi, no entanto, total.
Comparativamente com as técnicas dinâmicas descritas na literatura, a técnica preconizada pelos autores permite não só a reconstituição ístmica eficaz, com 100% de consolidação, como revela resultados clínicos superiores a médio prazo, o que supera em grande escala a necessidade de segunda intervenção para extração do material.
Na espondilolistese de grau superior a I, os autores defendem a artrodese circunferencial devido à discopatia, instabilidade e desequilíbrio sagital associados.
]]> CONCLUSÃO
O tratamento cirúrgico da espondilólise e espondilolistesis ístmica está indicado nos adolescentes sintomáticos, após falência do tratamento conservador.
A técnica de reconstituição ístmica com autoenxerto e fixação pedicular posterior temporária na espondilolise ou espondilolistese ístmica grau I alia excelentes resultados clínicos a elevada taxa de consolidação.
Esta técnica é defendida pelos autores mesmo em adolescentes que são atletas, em que se verificou ser possível retomar a atividade desportiva a nível de alta competição.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Wiltse LL, Newman PH, Macnab I. Classification of spondylolysis and spondylolisthesis. Clin Orthop. 1976 Jun; 117: 23-29
2. Turner PG, Green JH, Galasko CS. Back pain in childhood. Spine. 1989 Aug; 14 (8): 812-814
3. King HA. Back pain in children. Pediatr Clin North (Am). 1984 Oct; 31 (5): 1083-1095
4. Altaf F, Heran MKS, Wilson LF. Back pain in children and adolescentes. BJJ. 2014 Jun; 96-B (6): 717-723
]]> 5. Amato ME, Totty WG, Gilula LA. Spondylolysis of the lumbar spine: demonstration of defects and laminal fragmentation. Radiology. 1984 Dec; 153 (3): 627-6296. Fredrickson BE, Baker D, McHolick WJ. The natural history of spondylolysis and spondylolisthesis. JBJS (Am). 1984 Jun; 66 (5): 699-707
7. Standaert CJ, Herring SA. Spondylolysis: a critical review. Br J Sports Med. 2000 Dec; 34 (6): 415-422
8. Blanda J, Bethem D, Moats W. Defects of pars interarticularis in athletes: a protocol for nonoperative treatment. J Spinal Disord. 1993 Oct; 6 (5): 406-411
9. Soler T, Calderón C. The prevalence of spondylolysis in the Spanish elite athlete. Am J Sports Med. 2000 Jan; 28 (1): 57-62
10. Turner RH, Bianco AJ. Spondylolisthesis in Children and Teen-Agers. J Bone Joint Surg (AM). 1971 Oct; 53 (7): 1298-1306
11. Dietrich M, Kurowski P. The importance of mechanical factors in the etiology of spondylolysis: a model analysis of loads and stresses in human lumbar spine. Spine. 1985; 10 (6): 532-542 [ Links ]
12. Natural history of symptomatic isthmic low-grade spondylolisthesis in children and adolescents: a seven-year follow-up study. J Pediatr Orthop. 1991; 11 (2): 209-213 [ Links ]
13. Blackburne JS, Velikas EP. Spondylolisthesis in children and adolescents. JBJS (Br). 1977 Nov; 59-B (4): 490-494
14. Morita T, Ikata T, Katoh S. Lumbar spondylolysis in children and adolescents. JBJS (Br). 1995 Jul; 77 (4): 620-625
]]> 15. Steiner ME, Micheli LJ. Treatment of Symptomatic Spondylolysis and Spondylolisthesis with the Modified Boston Brace. Spine. 1985 Dec; 10 (10): 937-94316. Pizzutillo PD, Hummer CD III. Nonoperative treatment for painful adolescent spondylolysis or spondylolisthesis. J Pediatr Orthop. 1989; 9: 538-540 [ Links ]
17. Audat ZM, Darwish FT, Al Barbarawi MM, Obaidat MM, Haddad WH, Bashaireh WM, et al. Surgical management of low grade isthmic spondylolisthesis; a randomized controlled study of the surgical fixation with and without reduction. Scoliosis. 2011; 6 (14)
18. Rubery PT, Bradford DS. Athletic activity after spine surgery in children and adolescents: results of a survey. Spine. 2002 Fev 15; 27 (4): 423-427
19. Herman MJ, Pizzutillo PD, Cavalier R. Spondylolysis and spondylolisthesis in the child and adolescent athlete. Orthop Clin N Am. 2003 Jul; 34 (3): 461-467
20. Bonnici AV, Koka SR, Richards DJ. Results of Buck screw fusion in grade I spondylolisthesis. J R Soc Med. 1981 May; 84 (5): 270-273
21. Nicol RO, Scott JH. Lytic spondylolysis: repair by wiring. Spine. 1986 Dec; 11 (10): 1027-1030
22. Scott JHS. The Edinburgh repair of isthmic (Group II) spondylolysis. JBJS (Br). 1987; 69-B: 491 [ Links ]
23. Johnson GV, Thompson AG. The Scott wiring technique for direct repair of lumbar spondylolysis. JBJS (Br). 1992 May; 74-B (3): 426-430
24. Songer MN, Rovin R. Repair of the pars interarticularis defect with a cable-screw construct: a preliminary report. Spine. 1998 Jan 15; 23 (2): 263-269
]]> 25. Morscher E, Gerber B, Fasel J. Surgical treatment of spondylolisthesis by bone grafting and direct stabilization of spondylolysis by means of a hook screw. Arch Orthop Trauma Surg. 1984 Sep; 103 (3): 175-17826. Fan J, Yu GR, Liu F, Zhao J, Zhao WD. Direct repair of spondylolysis by TSRH's hook plus screw fixation and bone grafting: biomechanical study and clinical report. Arch Orthop Trauma Surg. 2010 Fev; 130 (2): 209-215
27. Gillet P, Petit M. Direct repair of spondylolysis without spondylolisthesis, using a rod-screw construct and bone grafting of the pars defect. Spine. 1999 Jun 15; 24 (12): 1252-1256
28. Teplick JG, Laffey PA, Berman A, Haskin ME. Diagnosis and evaluation of spondylolisthesis and/or spondylolysis on axial CT. AJNR Am J Neuroradiol. 1986; 7 (3): 479-491 [ Links ]
29. Chen X-s, Zhou S-y, Jia L-s, Fang L, Zhu W. A universal pedicle screw and V-Rod system for lumbar isthmic spondylolysis: a retrospective analysis of 21 cases. PLOS One. 2013; 8 (5) [ Links ]
30. Koptan WM, Elmiligui YH, ElSharkawi MM. Direct repair of spondylolysis presenting after correction of adolescent idiopathic scoliosis. Spine J. 2011; 11 (2): 133-138 [ Links ]
31. Sairyo K, Goel VK, Faizan A, Vadapalli S, Biyani S. Buck's direct repair of lumbar spondylolysis restores disc stresses at the involved and adjacent levels. Clin Biomech. 2006 Dec; 21 (10): 1020-1026
Conflito de interesse:
Nada a declarar.
]]>Vânia Oliveira
Serviço de Ortopedia
Centro Hospitalar do Porto
Hospital Santo António
Largo Prof. Abel Salazar
4099-001 Porto
Portugal
vaniacoliveira@gmail.com
Data de Submissão: 2014-07-16
Data de Revisão: 2014-09-03
Data de Aceitação: 2014-10-21
]]>