Psychosocial adjustment to breast cancer in women with conservative surgery vs mastectomy
Susana Fernandes1, Teresa McIntyre2, Ângela Leite3
1Faculdade de Psicologia, Educação e Desporto, Universidade Lusófona do Porto, Porto, Portugal
2College of Education and Behavioral Sciences, Houston Baptist University, Houston, USA
3Universidade Europeia, Laureate International Universities, Lisboa, Portugal
RESUMO
Este estudo compara o ajustamento psicossocial à doença em mulheres com cancro da mama submetidas a cirurgia de conservação e mastectomia, prevendo diferenças entre os dois grupos. Procura ainda avaliar se há diferenças no ajustamento ao longo de quatro momentos de avaliação. A amostra foi constituída por 74 mulheres no estádio I-III da doença submetidas a cirurgia. Todas as mulheres responderam a questionários de baseline, antes da cirurgia, e foram seguidas longitudinalmente até ao final dos tratamentos. As dimensões do ajustamento psicossocial avaliadas foram o estado emocional, as representações da doença e a funcionalidade, não se tendo verificado diferenças no ajustamento, para a grande maioria das variáveis psicossociais estudadas, em função do tipo de cirurgia. Contudo, encontramos diferenças significativas para as representações de doença (compreensão da doença) e para a funcionalidade (categoria lazer, sono e dimensão psicossocial), tendo os resultados sido mais favoráveis para as mulheres que realizaram uma mastectomia. Estes resultados são inesperados uma vez que a cirurgia de conservação pretende proporcionar um resultado cosmético mais satisfatório e com taxas de sobrevivência equivalentes às da mastectomia, fazendo supor que se conseguiria obter um melhor ajustamento psicossocial. Os dados encontrados sugerem que o tipo de cirurgia não parece predizer o ajustamento psicossocial. No entanto, considera-se que implicar as doentes na escolha do tipo de cirurgia, sempre que isso seja possível, pode beneficiar uma compreensão mais ajustada acerca da doença e do tratamento, com repercussões mais favoráveis ao nível emocional e da funcionalidade. ]]>
Palavras-chave: Cancro da mama, Ajustamento psicossocial, Tipo de cirurgia, Mastectomia, Cirurgia conservadora.
ABSTRACT
The aim of this study was to examine psychosocial adjustment differences between breast cancer women who underwent a lumpectomy or mastectomy, predicting differences between the two groups. The participants were 74 Portuguese recently diagnosed breast cancer patients, recruited in the main Oncology Hospital of the North of Portugal. The study design is longitudinal with four-time points: before surgery (baseline); two weeks after surgery, during adjuvant treatments; and at the end of adjuvant treatment. The evaluated dimensions were emotional state, illness perception and illness functional limitations. We didn’t find differences for most of the variables, between the two groups. However, we find significant differences for comprehension (illness perception) and for leisure, sleep and psychosocial dimension (perceived functioning), with better adjustment for women who underwent mastectomy. These results are unexpected since conservation surgery aims to provide a more satisfying cosmetic outcome and survival rates equivalent to those of mastectomy, assuming a better psychosocial adjustment. The data suggest that the type of surgery doesn’t seem to predict the psychosocial adjustment. However, involving patients in choosing surgery type, whenever it is possible, can benefits a better understanding about the disease and the treatment, with more favourable repercussions on the emotional level and functionality.
Key words: Breast cancer, Psychosocial adjustment, Type of surgery, Mastectomy, Conservation surgery.
O corpo de investigação atual na área da Psicologia Oncológica e, mais especificamente, acerca do ajustamento psicossocial ao cancro da mama, tem dado relevo ao papel de fatores socio-demográficos como a idade e o nível educacional; fatores clínicos e da doença, como o tipo de cirurgia e estádio da doença; estado emocional, como a ansiedade e a depressão; a personalidade; o coping e o suporte social (e.g., Aaronson et al., 2014; Bleiker, Hendriks, Otten Verbeek, & van der Ploeg, 2008; Çam, Gümus, & Saka, 2009; Denewer, Farouk, Mostafa & Elshamy, 2011; Dubashi, Vidhubala, Cyriac, & Sagar, 2010; Parker et al., 2007; Saita, Acquati, & Kayser, 2015; Skrzypczak, Laski, Czemiak, & Kycler, 2009; van den Berg et al., 2015). A literatura atual indica a possibilidade de vários tipos de resposta psicológica ao diagnóstico e tratamento do cancro da mama. Estas diferenças individuais sugerem que as pacientes com cancro da mama têm diferentes perceções da experiência de doença, sendo os fatores cognitivos, também, importantes determinantes da resposta psicológica (Buick, 1997; Millar, Purushotham, McLatchie, Georges, & Murray, 2005). Um dos temas que tem sido objeto de investigação na área da Psicologia Oncológica diz respeito à resposta psicológica das doentes com cancro da mama, em função do tipo de cirurgia a que são submetidas (Fonseca, Lencastre, & Guerra, 2014; Markopoulos et al., 2009; Medeiros et al., 2010; Nakatani et al., 2013).
As cirurgias mais comuns no tratamento do cancro da mama, em mulheres, são a cirurgia conservadora e a mastectomia. Na cirurgia conservadora remove-se apenas uma parte da mama, dependendo do tamanho e do local do tumor (Schwartz et al., 2007). A mastectomia é a cirurgia que remove toda a mama e, por vezes, outros tecidos próximos (Nava, Rocco, & Catanuto, 2015). Apesar de décadas de pesquisa dedicadas a estabelecer a equivalência entre a cirurgia conservadora e a mastectomia, continua a existir um número desproporcionalmente menor de mulheres submetidas a cirurgia conservadora em comparação com a mastectomia (Hoover, Bloom, & Patel, 2011).
Nas ultimas décadas, realizaram-se vários estudos com o intuito de verificar se a cirurgia de conservação, por ser menos mutilante, poderia conduzir a um melhor ajustamento psicossocial por parte das mulheres comparativamente à mastectomia (Markopoulos et al., 2009; Medeiros et al., 2010; Silva & Santos, 2010; Ursaru, Crumpei, & Crumpei, 2014; Veiga et al., 2010). Num estudo de revisão da literatura, conduzido por Moreira e Canavarro (2012), concluiu-se que a cirurgia conservadora não se encontra consistentemente associada a uma melhor adaptação ao cancro da mama, nomeadamente, no que respeita a melhor qualidade de vida, níveis inferiores de ansiedade e depressão, melhor funcionamento conjugal, entre outros. Contudo, alguns estudos relatam vantagem em realizar uma cirurgia mais conservadora visto estar associada a uma imagem corporal mais positiva (e.g., Arndt, Stegmaier, Ziegler, & Brenner, 2008; Hoover et al., 2011).
]]> Similarmente, encontramos diversa literatura em relação ao impacto psicológico da mastectomia em mulheres com cancro da mama (Arroyo & López, 2011; Brandberg et al., 2008; Metcalfe et al., 2012, 2015; Ominyi & Nwodom, 2012; Shrestha, 2012). Sobre esta temática verificamos que, embora alguns estudos relatem não ter encontrado nenhum efeito negativo da mastectomia sobre a ansiedade, depressão e qualidade de vida (e.g., Brandberg et al., 2008), outros referem um impacto negativo na sexualidade e na imagem do corpo (Arroyo & López, 2011). Também Metcalfe e colegas (2012) constataram que o funcionamento psicossocial não foi diferente, um ano após a cirurgia, entre mulheres que realizaram uma mastectomia e aquelas que realizaram uma mastectomia com reconstrução imediata. Ominyi e Nwodom (2012) relataram que um estágio mais avançado da doença está significativamente relacionado com pior qualidade de vida. A maioria das mulheres refere muito sofrimento, logo, as abordagens cirúrgicas mais conservadoras parecem falhar no seu intuito de diminuir o impacto negativo da mastectomia radical, quando prometiam alcançar uma melhor imagem do corpo e uma melhor qualidade de vida (Ominyi & Nwodom, 2012).O cancro da mama é a primeira causa de morte por cancro entre as mulheres de todo o mundo (Bustreo & Chestnov, 2015). Tal como acontece noutros países da Europa, em Portugal existe um risco elevado das mulheres desenvolverem cancro da mama (Ferlay et al., 2013), verificando-se que as pacientes se debatem com várias consequências da sua condição de saúde (Dias, 2002), designadamente, sintomatologia ansiosa e depressiva, que se afiguram como algumas das respostas comuns face à doença e tratamento (e.g., Fafouti et al., 2010).
Apesar do estado de arte não identificar claramente um pior ajustamento psicossocial das mulheres à mastectomia comparativamente à cirurgia conservadora, tem sido constatada a existência de impacto psicológico negativo, sobretudo no que diz respeito à imagem corporal. Os estudos realizados nesta área avaliaram o ajustamento psicossocial maioritariamente através da análise da depressão, da ansiedade, do bem-estar e da qualidade de vida, da imagem corporal e sexualidade. Neste estudo procuraremos ir mais longe, avaliando o ajustamento psicossocial das mulheres submetidas a mastectomia e a cirurgia de conservação, através da depressão e ansiedade, mas também através da funcionalidade e das perceções acerca da doença. A inclusão de variáveis que não têm sido consideradas em estudos anteriores pode ajudar a clarificar e ampliar o conhecimento acerca do impacto de cada um destes procedimentos cirúrgicos no ajustamento psicossocial das mulheres com cancro da mama.
Método
O objetivo deste estudo consiste em comparar o ajustamento psicossocial ao cancro da mama nas mulheres submetidas a cirurgia de conservação e nas submetidas a mastectomia, prevendo-se diferenças no ajustamento psicossocial (níveis de ansiedade e depressão, representações de doença e funcionalidade), independente e dependentemente do momento de avaliação.
Procedimentos
Trata-se de um estudo longitudinal, com vários momentos de avaliação: no primeiro momento (T1), aquando do planeamento cirúrgico; no segundo momento (T2), sensivelmente 1 mês após o primeiro momento e cerca de 2 a 3 semanas após a cirurgia; no terceiro momento (T3), nos 4 meses após o primeiro contacto, que coincide com a fase intermédia do tratamento (para as mulheres que se encontravam a realizar quimioterapia e radioterapia); e o quarto momento (T4) que ocorre no fim do tratamento.
Selecionaram-se mulheres que se dirigiam à consulta de planeamento cirúrgico do Instituto Português de Oncologia (IPO) do Porto, de forma consecutiva, não aleatória. Os critérios de inclusão no estudo foram: (1) ter sido diagnosticada com cancro da mama pela primeira vez, (2) realizar a cirurgia, (3) ter sido diagnosticada no estádio I-III da doença, (4) não estar a participar noutros estudos, (5) não sofrer de outra doença crónica, e (6) não ter diagnóstico de doença mental grave.
]]> Todos os procedimentos seguidos estavam de acordo com os padrões do comité ético do IPO e com a Declaração de Helsinki de 1975, revista em 2000. O consentimento informado para colaborar voluntariamente na pesquisa foi obtido.
Amostra
A população à qual se destinou o presente estudo foi composta por doentes recentemente diagnosticadas com cancro da mama, a realizar os seus tratamentos no IPO. O número de mulheres que aceitou participar no estudo foi 101 (T1). Contudo, em alguns casos, não foi possível continuar a avaliação após o primeiro momento devido a diversas circunstâncias, como a não confirmação após a cirurgia de doença oncológica ou dificuldade no contacto com a doente nos momentos previstos para o efeito. Assim, foram incluídas no estudo as mulheres com quem se manteve o contacto no planeamento cirúrgico e no pós-cirurgia (N=74), que constitui o total da amostra em estudo, correspondendo a uma taxa de participação de 73%. No último momento, foram avaliadas apenas 35 mulheres, devido à necessidade de interrupção da recolha de dados.
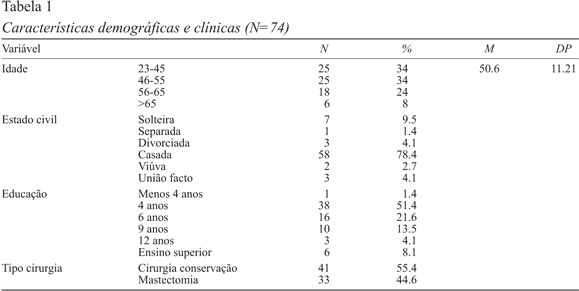
A amostra tem maioritariamente entre 23 e 55 anos, é casada e tem 4 anos de escolaridade. A maior parte está no estádio II da doença e foi submetida a uma cirurgia conservadora (Tabela 1).

]]> Instrumentos
Os instrumentos utilizados para medir as variáveis estudadas foram os questionários sócio-demográfico e clínico desenvolvido para o efeito e os questionários de auto-relato que se apresentam seguidamente:
O questionário sociodemográfico é constituído por questões que se referem à idade, escolaridade e estado civil; da situação clínica, foi registado o tipo de cirurgia e o estádio da doença.
Brief IPQ – Brief Illness Perception Questionnaire (Broadbent, Petrie, Main, & Weinman, 2006; tradução portuguesa de Araújo-Soares, Trovisqueira, & McIntyre, 2007, citados por Trovisqueira, 2007). O IPQ breve é constituído por nove itens que permitem avaliar: a dimensão das representações cognitivas de doença (consequências, duração, controlo pessoal, controlo através do tratamento e identidade); a dimensão das representações emocionais (preocupação e emoções): e ainda a compreensão da doença e representações causais. Trata-se de um questionário multifatorial. Cada dimensão constitui uma escala da qual fazem parte várias afirmações, sendo atribuída a cada uma destas afirmações uma resposta numa escala de Likert de 5 pontos (“sempre” a “nunca” na sub-escala identidade, e “discordo completamente” a “concordo completamente”, nas restantes sub-escalas). O score total de cada sub-escala resulta do somatório dos valores obtidos em cada afirmação. Para avaliar as qualidades psicométricas do IPQ-B, nesta amostra, seguimos os mesmos procedimentos do estudo original (Broadbent et al., 2006). Com o objetivo de testar a fidelidade teste-reteste, utilizaram-se as correlações de Pearson, entre o momento de avaliação inicial (T1) do IPQ-B e o segundo momento de avaliação (T2). Verificou-se que, no período de um mês, as dimensões do IPQ-B apresentam alguma variação, sendo esta mais evidente para as dimensões duração, identidade e consequências, que apresentam correlações abaixo de .50, possivelmente indicando uma menor estabilidade no tempo destas representações, nas mulheres com cancro da mama. As dimensões que se revelaram mais estáveis durante este período foram a compreensão, a resposta emocional, controlo pelo tratamento e a preocupação. Neste estudo, e para um período de intervalo de um mês, o IPQ-B mostrou correlações teste-reteste mais baixas do que as encontradas no estudo de Broadbent e colegas (2006) para as sub-escalas consequências, duração, controlo pessoal, identidade e resposta emocional. Obtiveram-se coeficientes teste-reteste mais elevados do que os citados por Broadbent e colegas (2006) para o controlo pelo tratamento, a compreensão e preocupação. O facto de se tratar de uma amostra com uma patologia diferente da do estudo original e com diagnóstico recente poderá explicar menos estabilidade no tempo de algumas das representações de doença.
HADS – Hospital Anxiety and Depression Scale (Zigmond & Snaith, 1983; versão portuguesa de McIntyre, Pereira, Soares, Gouveia, & Silva, 1999) contém as dimensões depressão e ansiedade. A HADS é composta por uma sub-escala de ansiedade, constituída por 7 itens, e uma sub-escala de depressão, constituída por outros 7 itens, permitindo avaliar a morbilidade psiquiátrica na semana precedente. As respostas a cada item podem ser quantificadas numa escala de Likert, variando de 0 a 3, com os valores mais elevados a revelarem maior distress psicológico. No sentido de avaliar a consistência interna da escala, na nossa amostra, foi calculado o alfa de Cronbach, separadamente para as sub-escalas de ansiedade e depressão e para o total. Para as sub-escalas de ansiedade e depressão encontraram-se, respetivamente, valores de .75 e .81 e de .86 para o total da escala, o que revela uma elevada consistência interna.
SIP – Sickness Impact Profile (Bergner, Bobbitt, Carter, & Gilson, 1981; versão portuguesa de McIntyre, McIntyre, & Soares, 2000). A versão utilizada neste estudo é constituída por 127 itens distribuídos por 11 categorias. Esta versão foi testada numa amostra de 78 sujeitos pós-enfarte do miocárdio (Gouveia, 2004). As 11 categorias consideradas foram: locomoção, cuidados pessoais e movimento, mobilidade, tarefas domésticas, atividades recreativas e lazer, atividades sociais, emoções, alerta, sono e repouso, alimentação e comunicação. Estas categorias podem ser divididas em duas dimensões: a dimensão física (locomoção, tarefas domésticas, mobilidade, sono e repouso e emoções), e a dimensão de funcionalidade social (alerta, atividades sociais e atividades recreativas e lazer). Cada item tem um valor que reflete o grau de severidade da limitação. Quanto mais baixa for a pontuação, melhor é o estado de saúde do indivíduo. Para as análises, foi retirada a categoria comunicação, atendendo ao facto de que foram selecionados apenas os itens com uma frequência de resposta ≥5. Optamos também por retirar a categoria alimentação que apresentou uma frequência de resposta de apenas 9 participantes. Com o objetivo de determinar a fidelidade do SIP nesta amostra, calculou-se o coeficiente de alfa de Cronbach (consistência interna) para o total do SIP, considerando-se o valor de cada categoria como um item, à semelhança da versão original. Obteve-se um valor de alfa total de .76, o que indica uma consistência interna adequada.
]]> Análise estatística
Foram levados a cabo procedimentos relativos à estatística descritiva (frequência, média e desvio padrão) e à estatística inferencial (análise de covariância ANOVA e t Test para amostras emparelhadas), com recurso ao programa informático de análise estatística SPSS, versão 22.
Resultados
A nossa hipótese previa que o ajustamento psicossocial ao longo do processo de tratamento variasse em função do tipo de cirurgia, bem como em função dos momentos de avaliação. Esta hipótese foi testada recorrendo a ANOVAS para os quatro momentos de avaliação, tendo como variáveis dependentes as variáveis psicossociais (estados emocionais – ansiedade e depressão; perceção da doença – consequências, duração, controlo pessoal, controlo através do tratamento, identidade, preocupação, compreensão e resposta emocional; e a funcionalidade – locomoção, cuidados pessoais, mobilidade, tarefas domésticas, lazer, atividades sociais, emoções, alerta, sono, funcionalidade psicossocial e funcionalidade física) e como variáveis independentes os momentos de avaliação (T1, T2, T3 e T4) e o tipo de cirurgia (cirurgia conservadora e mastectomia). As dimensões relacionadas com a funcionalidade foram avaliadas apenas em três momentos (T2, T3, T4), visto que se considerou que a funcionalidade seria mais afetada após a cirurgia.
Estados emocionais
Os resultados obtidos através das análises de variância (Tabela 2) indicam que as médias da ansiedade e da depressão, nos quatro momentos, não apresentam diferenças estatisticamente significativas no que diz respeito ao tipo de cirurgia realizada. Além disso, verifica-se que, em ambos os tipos de cirurgia, a ansiedade e a depressão diminuem ao longo do processo de tratamento.
]]>
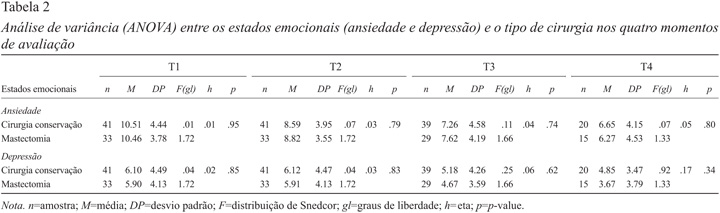
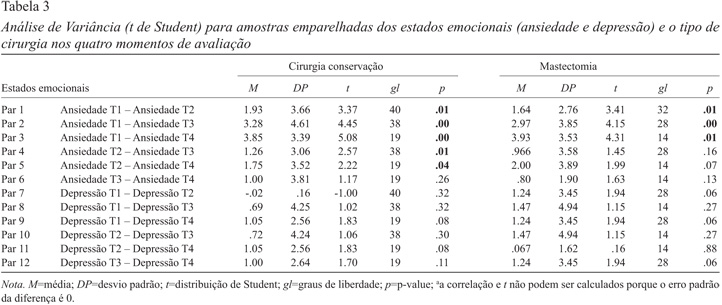
Procedemos ainda à análise de variância para amostras emparelhadas e constatamos que, em relação à depressão, não se encontram diferenças estatisticamente significativas entre os diferentes momentos, em ambos os grupos sujeitos a diferentes tipos de cirurgia (Tabela 3). No que diz respeito à ansiedade, encontramos diferenças estatisticamente significativas, em ambos os grupos (cirurgia conservadora e mastectomia), entre o 1º momento (T1) e todos os outros momentos (T2, T3 e T4), sendo que as mulheres sujeitas a cirurgia conservadora apresentam ainda diferenças significativas entre o 2º momento (T2) e os restantes (T3 e T4).
Perceção da doença
Na Tabela 4 encontramos os resultados das análises de variância (ANOVAS) referentes à perceção da doença.
]]>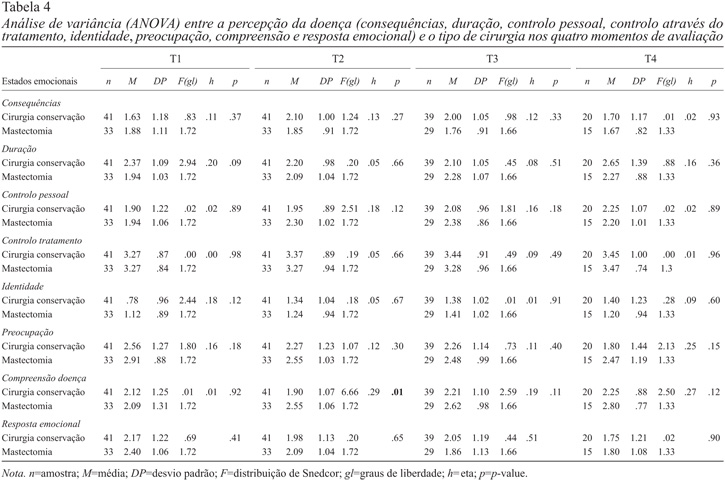
Os dados apresentam diferenças estatisticamente significativas entre os dois tipos de cirurgia para a compreensão, no segundo momento: nas mulheres submetidas a cirurgia de conservação, a compreensão acerca da doença é menor do que nas mulheres submetidas a mastectomia. Podemos ainda constatar que, nas mulheres que realizaram cirurgia de conservação, a compreensão diminui do primeiro para o segundo momento e aumenta até ao final do tratamento. Para as mulheres que realizaram mastectomia, a compreensão acerca da doença vai aumentando ao longo de todo o tratamento. No final do tratamento (T4), as mulheres com cirurgia de conservação continuam a relatar menor compreensão da doença do que as mastectomizadas.
A tendência para uma perceção mais negativa das consequências da doença, por parte das mulheres sujeitas a cirurgia de conservação, desaparece no final do tratamento.
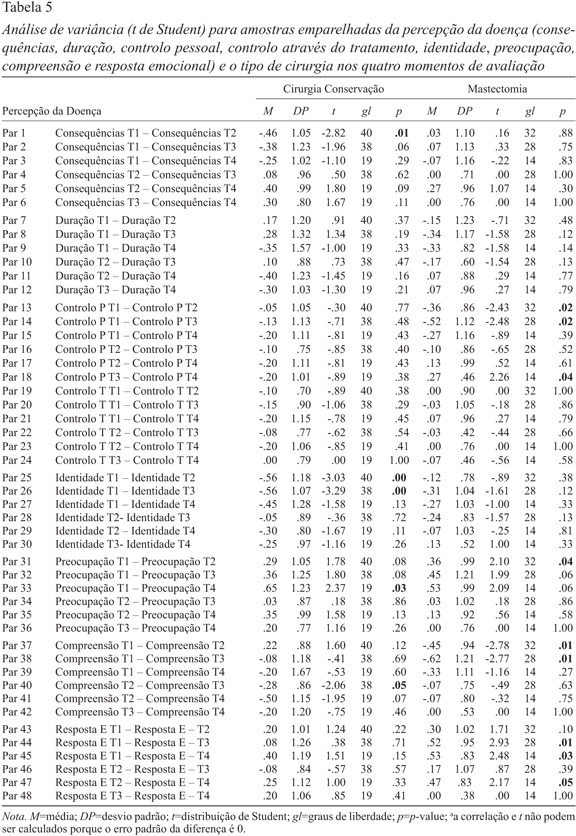
Procedemos ainda à análise de variância para amostras emparelhadas e constatamos que, nas mulheres submetidas a cirurgia conservadora, existem diferenças estatisticamente significativas em relação às consequências (medida em que a mulher perceciona que a doença afeta a sua vida) entre o 1º momento de avaliação (T1) e o 2º momento (T2), aumentando o valor (Tabela 5). O mesmo acontece, neste grupo, em relação à identidade (perceção de sintomas associados à doença), (entre T1 e T2 e entre T1 e T3, aumentando do T1 para os seguintes), à preocupação (entre T1 e T4, diminuindo) e à compreensão (entre T2 e T3, aumentando). No que diz respeito às mulheres que realizaram uma mastectomia, encontramos diferenças estatisticamente significativas em relação ao controlo pessoal (entre T1 e T2, entre T1 e T3, aumentando; e entre T3 e T4, diminuindo), à preocupação (entre T1 e T2, diminuindo), à compreensão (entre T1 e T2 e entre T1 e T3, aumentando), e à resposta emocional (entre T1 e T3, T1 e T4 e ainda entre T2 e T4, diminuindo).
Funcionalidade
Na Tabela 6, podemos observar os resultados das ANOVAS constatando-se que existem diferenças estatisticamente significativas relativamente ao lazer, no terceiro momento (T3): as mulheres que realizaram cirurgia de conservação apresentam mais limitações ao nível do lazer do que as mulheres que efetuaram uma mastectomia. No entanto, é de salientar que esta é uma área de bastante funcionalidade para os dois grupos. As áreas mais afetadas pela doença e tratamento, na perspetiva das pacientes, parecem ser as tarefas domésticas, o sono e as emoções.
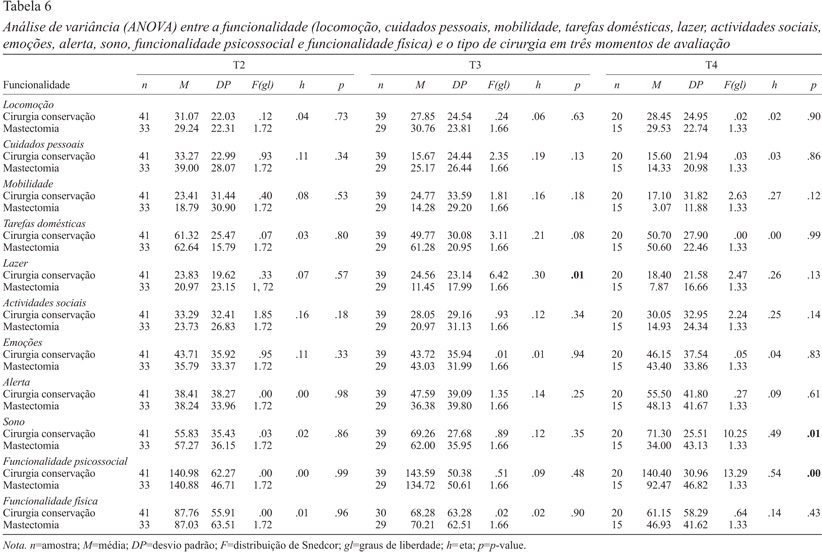
Em relação ao sono, encontrou-se diferenças estatisticamente significativas entre os dois grupos, no 4º momento (T4), bem como em relação à funcionalidade psicossocial, também no 4º momento (T4), sendo que as mulheres sujeitas a mastectomia apresentaram melhor funcionalidade do que as sujeitas a cirurgia de conservação. Aliás, as mulheres que efetuaram mastectomia apresentam níveis de funcionalidade superiores, ao longo de todo o processo de tratamento e, especialmente, no final deste.
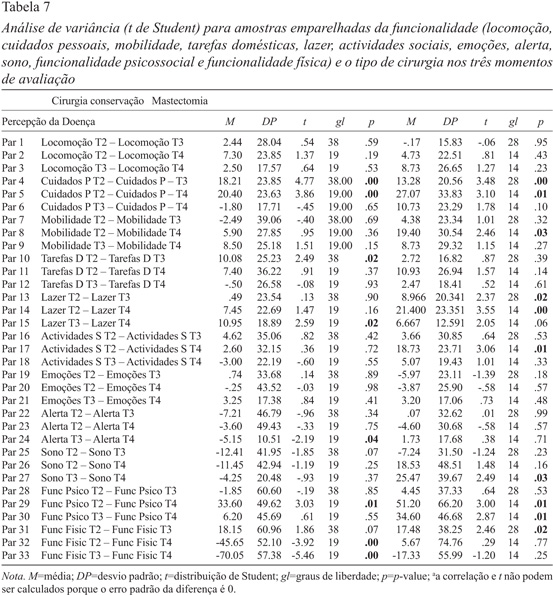
Na análise de variância para amostras emparelhadas verificamos que, nas mulheres sujeitas a cirurgia conservadora, existem diferenças estatisticamente significativas em relação aos cuidados pessoais (entre T2 e T3 e entre T2 e T4, diminuindo), às tarefas domésticas (entre T2 e T3, diminuindo), ao lazer (entre T3 e T4, diminuindo), ao alerta (entre T3 e T4, aumentando), ao funcionamento psicossocial (entre T2 e T4, diminuindo) e ao funcionamento físico (entre T2 e T4 e entre T3 e T4, diminuindo) (Tabela 7). Nas mulheres sujeitas a mastectomia, encontramos diferenças estatisticamente significativas relativamente aos cuidados pessoais (entre T2 e T3 e entre T2 e T4, diminuindo), à mobilidade (entre T2 e T4, diminuindo), ao lazer (entre T2 e T3 e entre T2 e T4, diminuindo), às atividades sociais (entre T2 e T4, diminuindo), ao sono (entre T 3 e T4, diminuindo), ao funcionamento psicossocial (entre T2 e T4 e T3 e T4, diminuindo) e ao funcionamento físico (entre T2 e T3).
]]>
Discussão
A nossa hipótese previa que o ajustamento psicossocial ao longo do processo de tratamento variasse em função do tipo de cirurgia e em função dos vários momentos de avaliação. Não foi possível verificar a hipótese para a grande maioria das variáveis psicossociais estudadas. Verificaram-se, apenas, diferenças entre os grupos para a perceção de doença, designadamente, na compreensão da doença, e para a funcionalidade, na categoria lazer, sono e na dimensão psicossocial, tendo os resultados sido mais favoráveis para as mulheres que realizaram uma mastectomia. Observaram-se algumas diferenças ao longo do tratamento para a ansiedade, as perceções de doença e a funcionalidade.
A revisão da literatura não é unânime no que respeita às diferenças ao nível do ajustamento nas mulheres submetidas a cirurgia de conservação ou mastectomia. Contudo, podemos verificar que os nossos resultados vão ao encontro de alguma literatura existente. Num estudo português acerca da avaliação da qualidade de vida em mulheres com cancro da mama, os autores constataram que as mulheres submetidas a cirurgia de conservação evidenciavam uma “perceção da imagem corporal” mais negativa e uma maior “preocupação com a queda do cabelo” do que as mulheres mastectomizadas (Rebelo, Rolim, Carqueja, & Ferreira, 2007). Estes dados são parcialmente semelhantes aos do nosso estudo na medida em que as mulheres submetidas a uma cirurgia menos mutilante são as que apresentam mais dificuldades.
No que refere ao estado emocional, os valores de depressão e ansiedade por nós encontrados não variavam significativamente em função do grupo, indo ao encontro de Medeiros e colegas (2010), que consideram que a cirurgia conservadora não afeta os níveis de depressão nas mulheres com cancro da mama. Ao contrário, Fafouti e colegas (2010) afirmam que os sintomas depressivos e ansiosos são mais frequentes em mulheres com cancro da mama do que nos grupos de controle (mulheres sem cancro da mama), bem assim como Dubashi e colegas (2010), que constataram que a qualidade de vida e a sexualidade eram ligeiramente piores no grupo de conservação da mama quando comparado ao grupo mastectomia. Os resultados encontrados no nosso estudo vão de encontro aos de Parker e colegas (2007), em que se verificou que algumas mudanças de curto prazo no ajustamento (menos ansiedade, menos satisfação em relação ao corpo) foram semelhantes entre os grupos de cirurgia. Também Brandberg e colegas (2008) relatam não ter encontrado efeitos negativos da mastectomia sobre a ansiedade, depressão e qualidade de vida.
Verifica-se uma tendência para a diminuição da ansiedade em ambos os grupos, ao longo do tratamento (T1, T2, T3, T4). Estes resultados são concordantes com os de Burgess e colegas (2005), que referem que a percentagem de mulheres com cancro da mama que apresentavam depressão ou ansiedade na altura do diagnóstico, diminuía aos três meses após o diagnóstico, continuando a diminuir após um ano. Também Vahdaninia, Omidvari e Montazeri (2010) constataram que a ansiedade e depressão iam diminuindo ao longo do tempo de tratamento. Estes dados sugerem que a ansiedade pode ter carácter transitório, tendendo a resolver-se com o tempo para uma boa parte das mulheres, o que indica um ajustamento adequado ao nível psicológico.
]]> O conhecimento acerca das perceções de doença nas mulheres com cancro da mama ao longo do processo de tratamento é fundamental para a compreensão da forma como estas vão lidar com a doença (Broadbent et al., 2006; Leventhal et al., 1997). Segundo Buick (1997) e outros autores (e.g., Millar et al., 2005; Petrie & Weinman, 1997), as perceções de doença são preditores importantes da resposta psicossocial ao tratamento, em mulheres com cancro da mama. Neste estudo, procuramos especificar um pouco mais este aspeto, analisando as perceções de doença em função do tipo de cirurgia. Assim, constatou-se que as mulheres que realizaram mastectomia sentem que compreendem melhor a sua doença ao longo do processo de tratamento do que as mulheres que foram submetidas a cirurgia de conservação. Estes dados parecem sugerir que, para as mulheres submetidas a cirurgia de conservação, o facto de conservar a mama sabendo que sofrem de uma doença maligna gera mais dúvidas relativamente à natureza da doença, dos tratamentos propostos e acerca da evolução da própria doença, aumentando as dificuldades de compreensão da mesma.No que refere à identidade, que representa a perceção de sintomas associados à doença, para as mulheres submetidas a cirurgia de conservação, verificaram-se variações significativas, ao longo do tratamento, ocorrendo um aumento da perceção de sintomas que se mantém até ao final do tratamento. Apesar deste aumento, convém assinalar que os valores da perceção de identidade são tendencialmente baixos para todas as pacientes, o que poderá ser um indicador positivo, visto que alguns autores (e.g., Bradley, Calvert, Pitts, & Redman, 2001; Crist & Grunfeld, 2013) constataram que a perceção de sintomas mantinha o medo de recorrência e predizia uma maior utilização dos cuidados de saúde, em doentes com cancro. A perceção de aumento de sintomas durante os tratamentos complementares, provavelmente, é causada pelos efeitos secundários que advêm da quimioterapia e da radioterapia, e que podem ser considerados fatores de vulnerabilidade, conduzindo a um ajustamento pior durante o tratamento e nas fases posteriores da doença (Ganz et al., 2002; Hwang, Chang, & Park, 2013). Também Millar e colegas (2005) verificaram que a morbilidade psicológica, um ano após a cirurgia, tem por preditores o nível de distress pós-operatório, a perceção de sintomas e a perceção da duração da doença, o que indica que perceções de doença mais negativas produzem níveis de stress elevados.
Ainda, no que diz respeito às perceções de doença, verificamos algumas diferenças significativas entre os vários momentos de avaliação, quer para as mulheres que realizaram cirurgia de conservação quer para as mulheres mastectomizadas. Assim, e relativamente à preocupação, é possível constatar que o grau de preocupação com a doença vai diminuindo ao longo do tratamento, para as mulheres que realizam uma cirurgia de conservação. Provavelmente as incertezas sentidas face à doença e tratamento vão diminuindo ao longo deste processo. Em relação às consequências, as pacientes que realizaram cirurgia de conservação revelam um aumento da perceção de que a doença afeta as suas vidas, após a cirurgia. Talvez por realizarem uma cirurgia menos mutilante, estas mulheres poderiam à partida ter uma expetativa mais favorável relativamente ao pós-operatório, gerando-se uma possível discrepância entre aquilo que era a expetativa e a realidade deste momento (dores, dificuldade de mobilidade do braço, edemas, etc.) traduzindo-se neste aumento da perceção das consequências. Contudo, esta perceção parece ajustada, na medida em que em qualquer fase do tratamento há áreas da vida que são afetadas, quer pelo diagnóstico quer pelos tratamentos que este implica.
No que respeita ao grupo de mulheres que realizaram mastectomia, verificou-se que estas têm um aumento da perceção de controlo pessoal até à fase em que estão a realizar os tratamentos complementares, acreditando que podem fazer alguma coisa para melhorar a sua condição. A perceção do controlo pessoal diminui no final dos tratamentos; provavelmente nesta fase a confiança das pacientes é depositada nos tratamentos precedentes e não tanto naquilo que poderão fazer por elas próprias para melhorar o seu prognóstico. A preocupação, também, diminui nas mulheres que realizaram mastectomia entre a pré-cirurgia e a pós cirurgia. Esta diminuição da preocupação pode estar associada ao facto de as mulheres terem dado o primeiro passo do seu tratamento, extraindo o órgão que se encontra doente e a um provável aumento da confiança neste tipo de tratamento. A resposta emocional também vai diminuindo nos vários momentos, para as mulheres que realizam uma mastectomia. Esta diminuição pode ser vista como um indicador de um ajustamento futuro mais favorável.
No que respeita à funcionalidade, encontramos diferenças significativas entre as mulheres que realizaram cirurgia de conservação e as mulheres que realizaram mastectomia, durante os tratamentos complementares e no final do tratamento, com resultados mais favoráveis a este último grupo, no que refere ao lazer, sono, e dimensão psicossocial. Os resultados encontrados no nosso estudo são difíceis de interpretar à luz da literatura existente, uma vez que esta apresenta resultados contraditórios. No entanto, os nossos resultados vão de encontro aos de Cohen, Hack, Moor, Katz e Goss (2000), que verificaram que as mulheres que efetuaram uma cirurgia de conservação tinham pior qualidade de vida do que as mulheres mastectomizadas. Estes resultados são algo inesperados uma vez que a cirurgia de conservação pretende proporcionar um resultado cosmético satisfatório com taxas de sobrevivência equivalentes às da mastectomia (Cardoso, Oliveira, & Cardoso, 2014), fazendo supor que se conseguiria obter um melhor ajustamento psicossocial, qualidade de vida e melhor funcionalidade nas mulheres submetidas a uma cirurgia de conservação. Os nossos resultados são semelhantes aos encontrados nos estudos de Härtl e colegas (2003); Yurek, Ferrar e Andersen (2000); e Rebelo e colegas (2007), na medida em que são as mulheres submetidas a uma cirurgia menos mutilante (cirurgia de conservação) as que apresentam mais dificuldades.
A funcionalidade apresenta uma tendência para piorar, quando se analisam as diferenças ao longo do tratamento (T2, T3 e T4) para cada um dos grupos. Deste modo, as mulheres que realizaram uma cirurgia de conservação pioram a sua funcionalidade ao nível dos cuidados pessoais, tarefas domésticas, lazer, funcionamento psicossocial e funcionamento físico. Por sua vez, as mulheres que realizaram uma mastectomia apresentam uma funcionalidade mais comprometida no que refere aos cuidados pessoais, mobilidade, lazer, atividades sociais, sono, funcionamento físico e funcionamento psicossocial. Importa observar que em ambos os grupos a funcionalidade fica mais comprometida à medida que se vão realizando os tratamentos e no final dos mesmos. É comumente aceite que tanto a radioterapia como os tratamentos sistémicos têm efeitos secundários indesejáveis e difíceis de suportar do ponto de vista físico, psicológico e social. Os efeitos secundários mais referidos pelas doentes, do ponto de vista físico, são a náusea, vómito e queda de cabelo (Binkley et al., 2012; Kaklamani & Gradishar, 2005), o que pode ter implicações na funcionalidade, explicando a sua diminuição ao longo do tratamento. Podemos presumir que algumas limitações do funcionamento físico podem contribuir para a uma perda de independência e da capacidade para realizar atividades sociais e profissionais usuais, bem como para o isolamento social. Segundo Miller, Jones e Carney (2005) e Vargas e colegas (2010), os distúrbios de sono são frequentes nestas mulheres, sendo um indicador do ajustamento psicossocial, o que sugere um impacto desfavorável no funcionamento diário.
A ausência de diferenças entre os dois grupos, para a maioria das variáveis estudadas, faz-nos considerar que provavelmente as grandes diferenças no ajustamento entre as mulheres que realizam cirurgia de conservação e mastectomia ocorram sobretudo ao nível da auto-estima, imagem corporal, ajustamento marital e sexual e menos ao nível das variáveis que foram consideradas no nosso estudo, embora estas estejam implicadas naquelas avaliadas por nós. Esta suposição é corroborada pelos estudos de Arndt e colegas (2008), que constataram que as mulheres submetidas a cirurgia conservadora relataram melhor funcionamento físico e funcionalidade, sendo sexualmente mais ativas e mais satisfeitas com sua imagem corporal do que as mulheres submetidas a uma mastectomia. Além disso, vários autores (e.g., Brandberg et al., 2008; Fonseca et al., 2014), constataram um impacto negativo na imagem corporal e na sexualidade em mulheres mastectomizadas.
Visto que o tipo de cirurgia não parece predizer o ajustamento psicossocial nas mulheres com cancro da mama, a oferta de apoio psicológico durante o processo de tratamento não deve ter por ponto de partida o tipo de cirurgia efetuada. Por essa razão, talvez seja pertinente envolver as doentes na escolha do tipo de cirurgia, sempre que isso se afigure como uma possibilidade, podendo as mulheres desenvolver uma compreensão mais ajustada acerca da doença e do tratamento, com repercussões mais favoráveis ao nível emocional e da funcionalidade.
No que se refere a algumas implicações práticas, podemos inferir a necessidade de fomentar consultas de psico-oncologia ou programas de intervenção destinados ao aumento do bem-estar das pacientes em tratamento para o cancro da mama, independentemente do tipo de cirurgia a que foram submetidas. As intervenções psicológicas para estas pacientes deverão ser efetuadas o mais precocemente possível (logo após o diagnóstico) e deverão ter um carácter continuado, pelo menos durante o processo de tratamento (6-8 meses após o diagnóstico).
É importante considerar algumas limitações metodológicas associadas a este estudo em termos da sua validade interna e externa. Em primeiro lugar, importa tecer um comentário acerca da dimensão da amostra e o uso do método de amostragem não probabilística consecutiva. O número reduzido de sujeitos coloca entraves ao nível da generalização dos resultados (validade externa) e da representatividade da amostra em relação à população em estudo. A amostra foi recolhida no Instituto Português de Oncologia, no Porto, região Norte do País e, como tal, devem ser tidas em consideração as características sociais e culturais desta região, devendo-se ter precauções na generalização dos resultados para outras regiões do país. O facto de se tratar de uma amostra não probabilística, aumenta a probabilidade de auto-seleção, o que resulta num grupo de participantes com características determinadas que podem ser diferentes das da população em geral, mais uma vez, limitando a generalização dos resultados.
]]> Apesar destas limitações, este estudo constitui-se como inovador na medida em que procura estudar longitudinalmente o ajustamento psicossocial das mulheres portuguesas com cancro da mama, durante o processo de tratamento em função do tipo de cirurgia. Estudos futuros devem tentar colmatar estas limitações, bem como procurar compreender outras variáveis que têm sido salientadas na revisão da literatura, e que não foram alvo deste estudo, como por exemplo o papel da família no ajustamento, e a imagem corporal e sexualidade. Outro aspeto a considerar em próximas investigações consiste em examinar o processo de ajustamento no final dos tratamentos complementares. A importância de investigar a longo prazo os efeitos de ser diagnosticada com cancro da mama, bem como do tipo de cirurgia utilizado, é premente, dado que cada vez mais a taxa de sobrevivência nesta doença é elevada.
Referências
Aaronson, N. K., Mattioli, V., Minton, O., Weis, J., Johansen, C., Dalton, S. O., . . . de Boer, A. (2014). Beyond treatment – Psychosocial and behavioural issues in cancer survivorship research and practice. European Journal of Cancer Supplements, 12, 54-64. doi: 10.1016/j.ejcsup.2014.03.005
Arndt, V., Stegmaier, C., Ziegler, H., & Brenner, H. (2008). Quality of life over 5 years in women with breast cancer after breast-conserving therapy versus mastectomy: A population-based study. Journal of Cancer Research and Clinical Oncology, 134, 1311. doi: 10.1007/s00432-008-0418-y [ Links ]
Arroyo, J. M. G., & López, M. L. D. (2011). Psychological problems derived from mastectomy: A qualitative study. International Journal of Surgical Oncology. http://dx.doi.org/10.1155/2011/132461 [ Links ]
Bergner, M., Bobbitt, R. A., Carter, W. B., & Gilson, B. S. (1981). The sickness impact profile: Development and final revision of a health status measure. Medical Care, 19, 787-805. [ Links ]
Binkley, J. M., Harris, S. R., Levangie, P. K., Pearl, M., Guglielmino, J., Kraus, V., & Rowden, D. (2012). Patient perspectives on breast cancer treatment side effects and the prospective surveillance model for physical rehabilitation for women with breast cancer. Cancer, 118, 2217-2216. doi: 10.1002/cncr.27469 [ Links ]
Bleiker, E. M., Hendriks, J. H., Otten, J. D., Verbeek, A. L., & van Der Ploeg, H. M. (2008). Personality factors and breast cancer risk: A 13-year follow-up. Journal of the National Cancer Institute, 100, 213-218. doi: 10.1093/jnci/djm280 [ Links ]
Bradley, E. J., Calvert, E., Pitts, M. K., & Redman, C. W. E. (2001). Illness Identity and self-regulatory model in recovery from early stage gynaecological cancer. Journal of Health Psychology, 6, 511-521. doi: 10.1177/135910530100600505 [ Links ]
Brandberg, Y., Sandelin, K., Erikson, S., Jurell, G., Liljegren, A., Lindblom, A., . . . Arver, B. (2008). Psychological reactions, quality of life, and body image after bilateral prophylactic mastectomy in women at high risk for breast cancer: A prospective 1-year follow-up study. Journal of Clinical Oncology, 26, 3943-3949. doi: 10.1200/JCO.2007.13.9568 [ Links ]
Broadbent, E., Petrie, K. J., Main, J., & Weinman, J. (2006). The Brief Illness Perception Questionnaire. Journal of Psychosomatic Research, 60, 631-637. doi: 10.1016/j.jpsychores.2005.10.020 [ Links ]
Buick, D. L. (1997). Illness representations and breast cancer: Coping with radiation and chemotherapy. In K. J. Petrie & J. A. Weinman (Eds.), Perceptions of health and illness (pp. 379-410). Amesterdam: Harwood Academic Publishers. [ Links ]
Burgess, C., Cornelius, V., Love, S., Graham, J., Richards, M., & Ramirez, A. (2005). Depression and anxiety in women with early breast cancer: Five year observational cohort study. British Medical Journal, 330, 702-705. [ Links ]
Bustreo, F., & Chestnov, O. (2015). A month to remember – Breast cancer awareness month. World Health Organization. http://www.who.int/mediacentre/factsheets/fs297/en/
Çam, O., Saka, Ş., & Gümüş, A. B. (2009). İnvestigation of factors affecting psychosocial adjustment of patients with breast cancer. Journal of Breast Health, 5, 73-81. [ Links ]
]]>Cardoso, M. J., Oliveira, H., & Cardoso, J. (2014). Assessing cosmetic results after breast conserving surgery. Journal of Surgical Oncology, 110, 37-44. doi: 10.1002/jso.23596 [ Links ]
Cohen, L., Hack, T. F., Moor, C., Katz, J., & Goss, P. E. (2000). The effects of type surgery and time on psychological adjustment in women after breast cancer treatment. Annals of surgical Oncology, 7, 427-434. doi: 10.1007/s10434-000-0427-9 [ Links ]
Crist, J. V., & Grunfeld, E. A. (2013). Factors reported to influence fear of recurrence in cancer patients: A systematic review. Psyco-Oncology, 22, 978-986. doi: 10.1002/pon.3114 [ Links ]
Denewer, A., Farouk, O., & Elshamy, K. (2011). Social support and hope among Egyptian women with breast cancer after mastectomy. Breast Cancer: Basic and Clinical Research, 5, 93. doi: 10.4137/BCBCR.S6655 [ Links ]
Dias, M. R. (2002). Cancro da mama: A (contra) informação dos mass media. In M. R. Dias & E. Duá (Coords.), Territórios da psicologia oncológica (pp. 235-264). Lisboa: Climepsi Editores. [ Links ]
Dubashi, B., Vidhubala, E., Cyriac, S., & Sagar, T. G. (2010). Quality of life among young women with breast cancer: Study from a tertiary cancer institute in south India. Indian Journal of Cancer, 47, 142-147. doi: 10.4103/0019-509X.63005 [ Links ]
Fafouti, M., Paparrigopoulos, T., Zervas, Y., Rabavilas, A., Malamos, N., Liappas, I., & Tzavara, C. (2010). Depression, anxiety and general psychopathology in breast cancer patients: A cross-sectional control study. In Vivo, 24, 803-810. [ Links ]
Ferlay, J., Steliarova-Foucher, E., Lortet-Tieulent, J., Rosso, S., Coebergh, J. W. W., Comber, H., . . . Bray, F. (2013). Cancer incidence and mortality patterns in Europe: Estimates for 40 countries in 2012. European Journal of Cancer, 49, 1374-1403. doi: 10.1016/j.ejca.2012.12.027 [ Links ]
Fonseca, S., Lencastre, L., & Guerra, M. (2014). Life satisfaction in women with breast cancer. Paidéia (Ribeirão Preto), 24, 295-303. doi: 10.1590/1982-43272459201403 [ Links ]
Ganz, P. A., Desmond, K. A., Leedham, B., Rowland, J. H., Meyerowitz, B. E., & Belin, T. R. (2002). Quality of life in long-term, disease free survivors of breast cancer: A follow-up study. Journal of the National Cancer Institute, 94, 39-49. doi: 10.1093/jnci/94.1.39 [ Links ]
Gouveia, J. L. R. V. (2004). Diferenças a nível de género na adaptação psicossocial a curto prazo no pós enfarte agudo do miocárdio. Dissertação de Mestrado na área de especialização de Psicologia da Saúde apresentada à Universidade do Minho.
Härtl, K., Janni, W., Kästner, R., Sommer, H., Strobl, B., Rack, B., & Stauber, M. (2003). Impact of medical and demographic factors on long-term quality of life and body image of breast cancer patients. Annals of oncology, 14, 1064-1071. doi: 10.1093/annonc/mdg289 [ Links ]
Hoover, S., Bloom, E., & Patel, S. (2011). Review of breast conservation therapy: Then and now. ISRN Oncology. http://dx.doi.org/10.5402/2011/617593 [ Links ]
Hwang, S. Y., Chang, S. J., & Park, B. (2013). Does chemotherapy really affect the quality of life of women with breast cancer?. Journal of Breast Cancer, 16, 229-235. http://dx.doi.org/10.4048/jbc.2013.16.2.229 [ Links ]
Kaklamani, V. G., & Gradishar, W. J. (2005). Adjuvant therapy of breast cancer. Cancer Investigation, 23, 548-560. http://dx.doi.org/10.1080/07357900500202937 [ Links ]
Leventhal, H., Benyamnini, Y., Brownlee, S., Diefenbach, M., Leventhal, E. A., Patrick-Miller, L., & Robitaille, C. (1997). Illness representations: Theoretical foundations. In K. J. Petrie & J. A. Weinman (Eds.), Perceptions of health & illness (pp. 19-45). Amsterdam: Harwood Academic Publishers. [ Links ]
Markopoulos, C., Tsaroucha, A. K., Kouskos, E., Mantas, D., Antonopoulou, Z., & Karvelis, S. (2009). Impact of breast cancer surgery on the self-esteem and sexual life of female patients. Journal of International Medical Research, 37, 182-188. doi: 10.1177/147323000903700122 [ Links ]
Mclntyre, T., Pereira, M. G., Soares, V., Gouveia, J., & Silva, S. (1999). Escala de Ansiedade e de Depressão Hospitalar - Versão portuguesa de investigação. Braga, Portugal: Departamento de Psicologia, Universidade do Minho. [ Links ]
McIntyre, T., McIntyre, S., & Soares, V. (2000). Versão portuguesa do SIP – Sickness Impact Profile. Não publicado.
Medeiros, M. C., Veiga, D. F., Sabino Neto, M., Abla, L. E. F., Juliano, Y., & Ferreira, L. M. (2010). Depression and conservative surgery for breast cancer. Clinics, 65, 1291-1294. http://dx.doi.org/10.1590/S1807-59322010001200011 [ Links ]
Metcalfe, K. A., Semple, J., Quan, M. L., Vadaparampil, S. T., Holloway, C., Brown, M., . . . Narod, S. A. (2012). Changes in psychosocial functioning 1 year after mastectomy alone, delayed breast reconstruction, or immediate breast reconstruction. Annals of Surgical Oncology, 19, 233-241. doi: 10.1245/s10434-011-1828-7 [ Links ]
Metcalfe, K. A., Zhong, T., Narod, S. A., Quan, M. L., Holloway, C., Hofer, S., . . . Semple, J. (2015). A prospective study of mastectomy patients with and without delayed breast reconstruction: Long-term psychosocial functioning in the breast cancer survivorship period. Journal of Surgical Oncology, 111, 258-264. doi: 10.1002/jso.23829 [ Links ]
Millar, K., Purushotham, A., McLatchie, E., Georges, W. D., & Murray, G. D. (2005). A 1-year prospective study of individual variation in distress, and illness perceptions, after treatment for breast cancer. Journal of Psychosomatic Research, 58, 335-342. [ Links ]
Miller, S. L.B., Jones, L. E., & Carney, C. P. (2005). Psychiatric sequele following breast cancer chemotherapy: A pilot study using claims data. Psychosomatics, 46, 517-522. http://dx.doi.org/10.1176/appi.psy.46.6.517 [ Links ]
Moreira, H., & Canavarro, M. C. (2012). Tipo de cirurgia, adaptação psicossocial e imagem corporal no cancro da mama. Psicologia, Saúde & Doenças, 13, 169-190. [ Links ]
Nakatani, Y., Iwamitsu, Y., Kuranami, M., Okazaki, S., Yamamoto, K., Watanabe, M., & Miyaoka, H. (2013). Predictors of psychological distress in breast cancer patients after surgery. Kitasato Medical Journal, 43, 49-56. [ Links ]
Nava, M. B., Rocco, N., & Catanuto, G. (2015). Conservative mastectomies: An overview. Gland Surgery, 4, 463-466. doi: 10.3978/j.issn.2227-684X.2015.04.06 [ Links ]
Ominyi, J., & Nwodom, M. (2012). Psychological impact of mastectomy and breast reconstruction. International Journal of Science and Research (IJSR), 3, 551-556. [ Links ]
Parker, P. A., Youssef, A., Walker, S., Basen-Engquist, K., Cohen, L., Gritz, E. R., . . . Robb, G. L. (2007). Short-term and long-term psychosocial adjustment and quality of life in women undergoing different surgical procedures for breast cancer. Annals of Surgical Oncology, 14, 3078-3089. doi: 10.1245/s10434-007-9413-9 [ Links ]
Petrie, K. J., & Weinman, J. A. (1997). Perceptions of health and illness. In K. J. Petrie & J. A. Weinman (Eds.), Perceptions of health and illness (pp. 1-46). Amesterdam: Harwood Academic Publishers. [ Links ]
Rebelo, V., Rolim, L., Carqueja, E., & Ferreira, S. (2007). Avaliação da qualidade de vida em mulheres com cancro de mama: Um estudo exploratório com 60 mulheres portuguesas. Psicologia, Saúde & Doenças, 8, 13-32. [ Links ]
Saita, E., Acquati, C., & Kayser, K. (2015). Coping with early stage breast cancer: Examining the influence of personality traits and interpersonal closeness. Frontiers in Psychology, 6, 88. doi: 10.3389/fpsyg.2015.00088 [ Links ]
Schwartz, G. F., Veronesi, U., Clough, K. B., Dixon, J. M., Fentiman, I. S., Heywang-Köbrunner, S. H., . . . Palazzo, J. P. (2007). Consensus conference on breast conservation. Seminars in Breast Disease, 10, 178-185. doi: 10.1053/j.sembd.2007.10.005 [ Links ]
Shrestha, K. (2012). Psychological impact after mastectomy among Nepalese women: A qualitative study. Nepal Medical College Journal, 14, 153-156. [ Links ]
Silva, G. D., & Santos, M. A. D. (2010). Stressors in breast cancer post-treatment: A qualitative approach. Revista Latino-Americana de Enfermagem, 18, 688-695. doi: 10.1590/S0104-11692010000400005 [ Links ]
Skrzypczak, M., Łaski, P., Czerniak, U., & Kycler, W. (2009). Do chronological age and selected socio-demographic factors affect quality of life in females with breast cancer?. Anthropological Review, 72, 31-44. doi: 10.2478/v10044-008-0014-4 [ Links ]
Trovisqueira, A. (2007). Impacto de uma intervenção informativa baseada na teoria das cognições de doença, em doentes no pós-enfarte do miocárdio. Tese de Mestrado, Universidade do Minho, Braga. [ Links ]
Ursaru, M., Crumpei, I., & Crumpei, G. (2014). Quality of life and religious coping in women with breast cancer. Procedia Social and Behavioral Sciences (ISI Proceedings), 114, 322-326. doi: 10.1016/j.sbspro.2013.12.705 [ Links ]
Vahdaninia, M., Omidvari, S., & Montazeri, A. (2010). What do predict anxiety and depression in breast cancer patients? A follow-up study. Social Psychiatry Epidemiology, 45, 355. doi: 10.1007/s00127-009-0068-7 [ Links ]
van den Berg, S. W., Gielissen, M. F., Custers, J. A., van der Graaf, W. T., Ottevanger, P. B., & Prins, J. B. (2015). BREATH: Web-based self-management for psychological adjustment after primary breast cancer – Results of a multicenter randomized controlled trial. Journal of Clinical Oncology, 33, 2763-2771. doi: 10.1200/JCO.2013.54.9386
Vargas, S., Wohlgemuth, W. K., Antoni, M. H., Lechner, S. C., Holley, H. A., & Carver, S. C. (2010). Sleep dysfunction and psychosocial adaptation among women undergoing treatment for non-metastatic breast cancer. Psycho-Oncology, 19, 669-673. doi: 10.1002/pon.1603 [ Links ]
Veiga, D. F., Campos, F. S. M., Ribeiro, L. M., Archangelo Junior, I., Veiga Filho, J., Juliano, Y., . . . Ferreira, L. M. (2010). Mastectomy versus conservative surgical treatment: The impact on the quality of life of women with breast cancer. Revista Brasileira de Saúde Materno Infantil, 10, 51-57. doi: 10.1590/S1519-38292010000100005 [ Links ]
Yurek, D., Ferrar, W., & Andersen, B. L. (2000). Breast cancer surgery: Comparing surgical groups and determining individual differences in postoperative sexuality and body change stress. Journal of Consulting and Clinical Psychology, 68, 697-709. http://dx.doi.org/10.1037/0022-006X.68.4.697 [ Links ]
Zigmond, A. S., & Snaith, R. P. (1983). The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica, 67, 361-370. doi: 10.1111/j.1600-0447.1983.tb09716.x [ Links ]
A correspondência relativa a este artigo deverá ser enviada para: Susana Fernandes, Faculdade de Psicologia, Educação e Desporto, Universidade Lusófona do Porto, R. de Augusto Rosa 24, 4000-098 Porto, Portugal. E-mail: susanamrfernandes@gmail.com
]]> Submissão: 21/12/2015 Aceitação: 26/05/2017 ]]>