Suicídio de um paciente: a experiência de médicos e psicólogos portugueses
Patient suicide: The experience of Portuguese doctors and psychologists
Inês Areal Rothesa*, Margarida Rangel Henriquesa, Renata Santos Correiaa
aFaculdade de Psicologia e de Ciências da Educação, Universidade do Porto, Porto, Portugal
RESUMO
Objetivo: Descrever o impacto do suicídio de um paciente em profissionais de saúde portugueses (psicólogos, psiquiatras e médicos de medicina geral).
]]> Método: Foi usado um questionário de autorresposta sobre características, experiência e impacto do suicídio de um paciente.Resultados: Duzentos e quarenta e dois profissionais responderam ao questionário e 64 tiveram, pelo menos, um paciente que se suicidou. Sofrimento emocional (47), preocupações, dúvidas e medo (35), frustração (28), choque e surpresa (23) foram os sentimentos mais relatados. Maior atenção, vigilância e rigor na avaliação e intervenção foram as reações mais frequentes após o suicídio do paciente (80). Aumento da insegurança e ansiedade foram também relatados (28). Colegas, contacto com a família do paciente e a revisão do caso foram os recursos de ajuda mais usados. Supervisor, revisão de caso e colegas foram avaliados como os mais úteis. Não foram encontradas diferenças de acordo com o género, idade ou grupo profissional na vivência deste acontecimento.
Conclusão: Os resultados mostram que o suicídio de um paciente tem um impacto profissional e emocional considerável. Porém, este acontecimento difícil também pode ser uma oportunidade de aprendizagem e crescimento profissional, levando a mudanças positivas e adequadas na prática clínica, relativamente à gestão do risco de suicídio e suas consequências.
Palavras-chave: Suicídio de paciente, Profissionais de saúde,Impacto emocional
ABSTRACT
Objective: To describe the impact of a patient suicide on Portuguese health professionals (psychologists, psychiatrists and general physicians).
Method: A self-report questionnaire, which assessed the characteristics, experience and impact of a patient suicide, was used.
Results: 242 health professionals filled the questionnaire and 64 professionals had been confronted with at least one patient suicide. Emotional suffering (47), concerns, doubts and fear (35), frustration (28) and shock and surprise (23) were the most common feelings reported by health professionals. Increased attention, vigilance and accuracy in assessment and intervention were the most frequent reaction after the patient suicide (80). Increased insecurity and anxiety were also reported (28). Colleagues, contact with patient's family and case review were the sources of help more frequently used, and supervisor, team case review and colleagues were rated as the most useful. There were no differences according to gender, age or professional group in the experience of this event.
Conclusion: The results show that the suicide of a patient has a considerable professional and emotional impact. However, this difficult event can also be an opportunity for learning and professional growth leading to positive and adequate changes in clinical practice with regard to the management of suicide risk and its aftermath.
]]> Keywords: Patient suicide. Health professionals. Emotional impact.
Introdução
Os comportamentos suicidários constituem um dos mais graves problemas de saúde pública, com grande impacto social no mundo ocidental. Os psiquiatras, médicos de medicina geral, psicólogos ou outros profissionais de saúde que perdem um paciente por suicídio estão expostos a uma das experiências mais perturbadoras da prática clínica1, 2, 3.
O suicídio de um paciente é reconhecido na literatura internacional como um risco dos profissionais de saúde4, 5, 6, 7, com acrescida probabilidade para aqueles que desenvolvem a sua atividade na área da saúde mental, tal como os psiquiatras e os psicólogos8, 9, 10, 11, 12, 13, 14. Paralelamente, a investigação sugere que 20-76 dos suicidas procuram um médico no mês anterior ao suicídio e que a maioria consulta o médico de medicina geral e familiar, não um psiquiatra15, 16, 17, 18, 19. Porém, a investigação acerca do impacto da morte por suicídio de pacientes em clínicos gerais tem sido negligenciada20, 21, 22, sendo que, no contexto nacional, esta escassez empírica estende-se aos demais profissionais, não existindo, até à data, em nosso conhecimento, nenhum estudo disponível sobre o impacto do suicídio de pacientes em profissionais de saúde portugueses.
Os profissionais de saúde que passam pela experiência do suicídio de um paciente reagem enquanto pessoas que perdem alguém significativo através de reações usuais de processo de luto (reações pessoais) e, simultaneamente, de acordo com o seu papel profissional específico (reações profissionais)23, 24.
Na literatura internacional as reações apontadas como mais comuns ao suicídio de um paciente são a negação, o choque, a tristeza, a raiva, a culpa, a descrença, a angústia, o sentimento de fracasso, o medo de acusações13, 14, 25, 26, 27, 28, 29. Vários autores exploraram a relação entre o impacto do suicídio e diferentes características do profissional, do paciente, da relação entre estes dois e de especificidades do suicídio5, 9, 10, 13, 25, 29, 30, 31, 32. Em relação ao género do profissional, os estudos tendem a ser concordantes na existência de diferenças significativas: as mulheres tendem a expressar mais frequentemente sentimentos de vergonha, responsabilização ou culpa, assim como tendem a colocar mais em causa o seu conhecimento e competência profissional como consequência do suicídio de um dos seus pacientes, em relação aos profissionais homens5, 31. Contudo, relativamente a outras variáveis, os resultados das diferentes investigações não são consensuais, revelando a necessidade de investimento neste foco específico de análise. Por exemplo, enquanto alguns estudos encontram relações significativas entre a idade dos profissionais e a intensidade das reações10 e na mudança das práticas clínicas6, outros estudos não encontraram estas diferenças9, 25, 29. Da mesma forma, relativamente ao grupo profissional, alguns dados empíricos apontaram para a não existência de diferenças31, enquanto outros revelaram, por exemplo, que os psiquiatras declaravam um maior sofrimento associado ao suicídio do paciente do que os psicólogos29. Outros dados mostraram que determinados grupos teriam uma maior tendência para operar mudanças nas práticas profissionais após o suicídio6.
As mudanças na prática profissional mais referidas como resultantes do suicídio de um paciente são a maior atenção a sinais de risco de suicídio, uma tendência maior para hospitalizar, mais interesse no fenómeno, procura de formação especializada na área, maior abertura à discussão de casos com colegas e maior atenção a implicações legais da prática profissional9, 10, 25, 26. Os recursos de ajuda apontados como mais úteis para lidar com esta experiência são a supervisão, a formação especializada, a discussão com colegas, a revisão do caso e a participação nas cerimónias fúnebres8, 9, 10, 33, 34.
Os objetivos deste estudo são: descrever as reações emocionais de psicólogos, psiquiatras e médicos de medicina geral perante o suicídio de um paciente, considerado pelos próprios com maior impacto, identificar as mudanças na prática clínica e vida pessoal decorrentes deste acontecimento, identificar os recursos de ajuda ou suporte usados para lidar com a situação e conhecer como estes profissionais de saúde avaliam a utilidade de cada suporte usado. O estudo pretende também contribuir para o conhecimento dos fatores relacionados com a experiência do suicídio de um paciente, investigando se existem diferenças nesta vivência devidas às características dos profissionais. Esperamos encontrar diferenças entre géneros e grupos profissionais. Esta investigação assume ainda particular relevância por ser o primeiro estudo em Portugal a disponibilizar dados empíricos na área.
]]> Método
Instrumento
Para estudar o impacto do suicídio de um paciente nos psicólogos, psiquiatras e médicos de medicina geral foi construído o Questionário Impacto do Suicídio de um Paciente (QISP) - versão para médicos e psicólogos (disponível em anexo). O desenvolvimento deste questionário foi baseado na revisão de literatura e nos instrumentos internacionais existentes de avaliação desta experiência8, 13, 25, 31, 32, 33. O QISP é composto por três partes principais. A primeira parte recolhe informação sociodemográfica e profissional dos participantes, tal como idade, género, grupo profissional, anos de prática, local de trabalho e a existência ou não de formação específica em prevenção do suicídio. A segunda parte questiona acerca do contacto dos profissionais com comportamentos suicidários na prática clínica e na vida pessoal. Na terceira parte solicita-se aos profissionais que identifiquem e caracterizem o suicídio do paciente que maior impacto lhes causou e, através de questões abertas, que descrevam o que sentiram na altura, que reações tiveram e que mudanças profissionais e pessoais decorreram como consequência deste acontecimento. Pede-se também aos profissionais que, retrospetivamente, avaliem em que medida aquele suicídio era previsível e prevenível. Apresenta-se ainda uma lista de possíveis recursos de apoio e solicita-se que perante cada um deles os profissionais se posicionem quanto à sua utilidade. Finalmente, o questionário inclui uma questão aberta que solicita aos médicos e psicólogos que, tendo em conta a própria experiência do suicídio de um paciente, aconselhem um colega inexperiente sobre a melhor forma de lidar com a situação.
Participantes e procedimentos
Os potenciais participantes foram recrutados através de um processo de amostragem misto: amostragem focalizada (targeted sampling)35 e amostragem bola de neve (snowball)36, 37. No primeiro processo, amostragem focalizada, foram identificados diferentes locais de trabalho de diferentes regiões do país, tais como hospitais, centros de saúde, faculdades, instituições de intervenção comunitária, onde se apresentou o estudo (presencialmente, via email ou carta) e convidou os profissionais, psicólogos, psiquiatras e médicos de medicina geral e familiar, a participarem.
No segundo método, bola de neve, caracterizado pelos participantes do estudo recrutarem outros potenciais participantes através das suas redes profissionais ou pessoais, utilizaram-se procedimentos adicionais no sentido de obter um conjunto inicial de participantes mais representativo do que a técnica clássica permite, tal como defendido na literatura38, 39, 40.
Estes procedimentos consistiram em: (1) solicitar aos profissionais (iniciais e intermediários) que enviassem aos investigadores contactos (email, telefone ou endereço) de profissionais potenciais participantes ou que eles próprios convidassem outros colegas a participar, ou seja, foi solicitado que nomeassem potenciais participantes mas também que os recrutassem para o estudo; (2) limitar, em parte dos participantes, o n.° de recrutados, solicitando que nomeassem entre 3-5 colegas; (3) no sentido de fomentar a colaboração efetiva dos profissionais, usou-se um sistema de incentivos na apresentação, promotores da participação (p. ex. texto personalizado, referência à importância de obter respostas naquele distrito ou zona do país). Estes procedimentos promovem composições de amostras que convergem e atingem um equilíbrio depois de um número relativamente limitado de cadeias, independentemente da amostra inicial, permitindo que se selecione arbitrariamente os primeiros participantes. Desta forma, apesar da seleção não randomizada, o viés introduzido é progressivamente eliminado, ultrapassando-se um dos problemas centrais da tradicional bola de neve - a amostra inicial aleatória - e evitando efeitos de designado voluntarismo e diferenças das redes entre profissionais.
Os dados foram recolhidos quer através de questionário on-line, cujo link foi enviado via email e colocado em sites de psicologia e medicina, quer através do questionário em suporte de papel enviado por correio e acompanhado com um envelope individual pré-pago para retorno. Os dados foram recolhidos em 2010 e 2011 e o anonimato e confidencialidade dos mesmos foram assegurados.
Análise de dados
Realizaram-se análises de conteúdo das respostas às questões abertas, usando dois avaliadores independentes para a categorização das mesmas. As análises estatísticas foram realizadas usando o SPPSS versão 19. Calcularam-se estatísticas descritivas e inferenciais. As diferenças na experiência do suicídio de um paciente devidas a características do profissional foram investigadas através de análises de variância &- ANOVA a um fator (one-way) seguidas do teste post-hoc de Tukey, do teste t de student para amostras independentes e testes qui-quadrado (com correção de Bonferroni).
]]> Para estas análises, a idade e os anos de prática foram recodificados em variáveis categoriais de três intervalos. Foi ainda calculada uma medida global do apoio usado pelos profissionais, recodificada numa escala de três pontos: recurso a ajuda baixo ou muito baixo, moderado e alto ou muito alto. Foi também calculado um score global para a avaliação da utilidade dos recursos, através da média desta medida.
Resultados
Características dos participantes
Participaram neste estudo 242 profissionais de saúde, cujas características estão descritas na Tabela 1. Cinquenta e três por cento eram psicólogos e 47 eram médicos, sendo que entre estes, 46 eram psiquiatras e 54 eram médicos de medicina geral e familiar. Quanto ao género, 70 eram mulheres e 30 eram homens. A idade média dos profissionais foi de 38 anos e a média de experiência clínica foi de 13 anos.
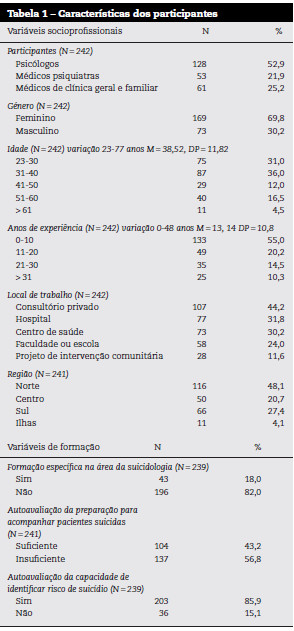
Em relação ao local de trabalho, 32 exercem a sua prática em hospitais, 30 em centros de saúde, 24 desenvolvem a sua atividade em faculdades ou escolas e 12 trabalham em projetos ou instituições de intervenção comunitária. Catorze por cento indicam outros locais, onde se incluem equipas de tratamento do Instituto da Droga e da Toxicodependência, Instituto Nacional de Emergência Médica e consulta de prevenção do suicídio, entre outros. Quase metade dos participantes (44) acumula os seus locais de trabalho com a prática clínica privada. Relativamente à distribuição destes locais no país: 48 eram do Norte, 21 do Centro, 27 do Sul e 4 dos Açores e da Madeira (3 profissionais trabalham em mais do que uma região e 2 não indicaram a mesma).
Dezoito por cento dos participantes têm formação específica em suicídio, 43 classificam a sua formação como suficiente para acompanhar pacientes com comportamentos suicidários e a grande maioria dos profissionais de saúde (85) sente-se capaz de identificar pacientes em risco de suicídio. Simultaneamente, 60 concordam que necessitam de formação especializada na área, 85 julgam que é fundamental implementar planos de formação dirigidos a profissionais de saúde e 12 avaliam-se como bons formadores na área da suicidologia.
Contacto com comportamentos suicidários
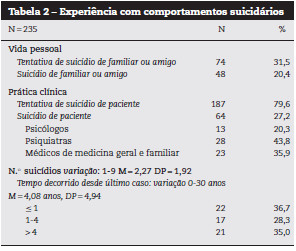
]]> A experiência dos participantes com comportamentos suicidários quer na vida privada quer na prática clínica está descrita na Tabela 2. Sessenta e quatro profissionais de saúde tiveram pelo menos um paciente que se suicidou, sendo que 44 são psiquiatras, 36 são médicos de medicina geral e familiar e 20 são psicólogos. Em média decorreram 4 anos desde o último suicídio do paciente e o preenchimento do questionário (M=4,1 anos, DP=4,9), sendo que para alguns profissionais decorreram meses e para outros 30 anos. Ter passado pela experiência do suicídio de um paciente relacionou-se significativamente com o género do profissional de saúde (X2 (correção de Yates)=17,65, df=1, p=0,000): a proporção de homens com esta experiência (46,5) é significativamente superior à das mulheres (18,9). Não se encontram, porém, diferenças significativas no número de suicídios de pacientes entre clínicos masculinos e femininos. Também foram encontradas diferenças significativas de acordo com o grupo profissional dos participantes (X2=40,99, df=2, p=0,000). As proporções de psicólogos, psiquiatras e médicos de medicina geral que tiveram, pelo menos, um paciente que se suicidou são significativamente diferentes: 11, 55 e 38, respetivamente. E foram também encontradas diferenças significativas no n.° de suicídios entre grupos (F (2, 60)=3,34, p=0,042). As diferenças encontradas nas médias de suicídios são de magnitude moderada (Eta squared=0,10). O teste post-hoc de Tukey revelou que a média de suicídios de pacientes entre os psiquiatras (M=2,86, DP=2,19) é significativamente superior à média de suicídios de pacientes entre os psicólogos (M=1,25, DP=0,87). A média de suicídios de pacientes dos médicos de medicina geral (M=2,09, DP=1,76) não difere significativamente dos restantes profissionais.
Características do paciente e suicídio com maior impacto
Os 64 profissionais que tiveram pelo menos um paciente suicida foram convidados a fornecer informações mais detalhadas sobre o suicídio que lhes tinha provocado maior impacto (Tabela 3).
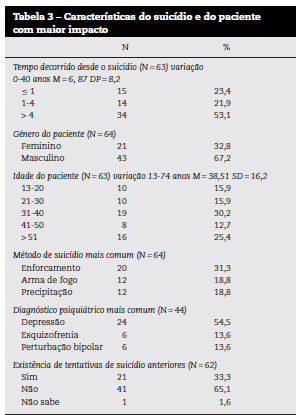
Mais de metade dos pacientes que se suicidaram eram do sexo masculino (67) e tinham idades compreendidas entre os 13-74 anos (M=38,5, DP=16,2). Em média, estes suicídios aconteceram há 7 anos. Para alguns profissionais decorreram meses desde o suicídio com maior impacto até ao preenchimento do questionário e para outros 40 anos. O método para cometer suicídio mais utilizado foi o enforcamento (32), seguido da arma de fogo e precipitação (19). Sessenta e nove por cento dos profissionais referem que o suicida tinha um diagnóstico psiquiátrico identificado, destacando-se a depressão como o mais comum (55), seguido da esquizofrenia e perturbação bipolar (14). Em 33 dos casos os profissionais de saúde descrevem a existência de tentativas de suicídio anteriores ao ato fatal.
Suicídio de um paciente: a experiência dos profissionais de saúde
]]> Forma como os profissionais tiveram conhecimento do suicídio do seu pacienteSessenta e oito por cento dos profissionais de saúde ficaram a saber do suicídio através dos familiares do paciente que comunicaram diretamente ao profissional ou fizeram chegar a informação à instituição onde este exercia funções. Em 19 dos casos a notícia foi dada por outros profissionais, como por exemplo, a assistente social ou elementos da equipa de enfermagem. Onze por cento dos profissionais de saúde tiveram conhecimento do suicídio através de outras pessoas que conheciam o suicida (que não familiares), como vizinhos ou outros pacientes amigos. Em 5 dos casos, a notícia chegou através de notificação formal da polícia ou do tribunal. Em 3 dos casos, o profissional de saúde foi chamados ao local do suicídio, sendo confrontado diretamente com o acontecimento, e a mesma percentagem (3) soube da notícia através de meios de comunicação social.
Perceção da possibilidade de prever e prevenir o suicídio
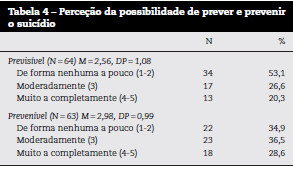
Mais de metade dos profissionais de saúde (53) percecionou o suicídio do seu paciente como sendo nada ou pouco previsível e 35 consideraram que não teria sido possível preveni-lo (Tabela 4).
Sentimentos perante o suicídio do paciente
Sessenta profissionais de saúde relataram o que sentiram após o suicídio do paciente. Os sentimentos descritos foram codificados em oito categorias descritas na Tabela 5. O sentimento mais relatado pelos profissionais de saúde foi o sofrimento emocional ou dor psicológica, referido por quase metade dos profissionais (47), incluindo tristeza, desespero, desgosto, sentimento de perda, dor e angústia, entre outros. A seguir, a categoria mais referida (35) é composta por preocupações, insegurança, dúvidas e medos, quer relativos ao futuro e a novos pacientes - «receio que voltasse a acontecer com outro doente» - quer em relação à intervenção realizada com o paciente falecido: «Questionei-me se teria feito tudo o que estava ao meu alcance para evitar esta situação». Vinte e oito por cento referiram a frustração ou outras emoções negativas, como zanga ou desilusão, dirigidas à situação, paciente ou familiares, e incluindo a culpabilização destes pelo suicídio. Vinte e três por cento dos profissionais de saúde sentiram-se chocados ou ficaram perplexos perante a situação. Vinte e dois por cento dos respondentes sentiram que falharam no reconhecimento dos sinais de risco ou que fracassaram na intervenção e 18 sentiram culpa e responsabilidade pelo suicídio. Sentimentos de impotência são descritos por 17 dos profissionais. E, finalmente, 7 revelaram aceitação ou resignação, sentindo o suicídio como um resultado possível, inevitável ou uma solução aceitável para uma dor insuportável e prolongada no tempo: «Aceitei: para a utente foi o culminar de um sofrimento de cerca de 40 anos».
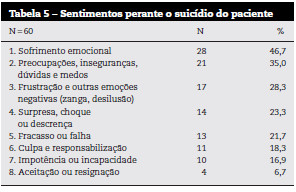
]]> Em relação à duração dos sentimentos descritos, 15 dos profissionais relataram que estes persistiram para além dos 6 meses após o suicídio do paciente, enquanto para mais de metade (57) estes sentimentos duraram menos de um mês.
Não se encontraram diferenças significativas entre os sentimentos relatados e o género, a idade, os anos de prática ou o grupo profissional dos participantes.
Mudanças na prática e outras reações
Além da descrição dos sentimentos, 40 participantes descreveram outras reações relacionadas com o suicídio do paciente e que, correspondem, principalmente, a mudanças na prática clínica. Estas são apresentadas na Tabela 6.
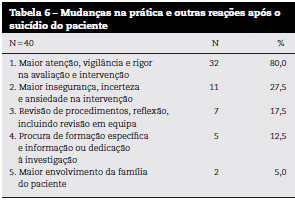
Oitenta por cento dos profissionais relataram que, depois de passarem pela experiência do suicídio de um paciente, tornaram-se mais atentos aos sinais de risco de suicídio e alteraram práticas de intervenção: «Passei a dar mais atenção à fase de melhoria sintomatológica e a valorizar seriamente todas as tentativas de suicídio»; «maior número de cuidados junto da família» e «maior número de internamentos nas primeiras 2 semanas após o início do tratamento». Paralelamente, 28 referiram uma maior insegurança e ansiedade na intervenção com potenciais suicidas e familiares, incluindo insegurança relativa às capacidades profissionais: «Que não percebia nada de psiquiatria», «questionei a minha capacidade para ser psicóloga» ou «receio de não ter capacidade profissional para enfrentar a situação», são alguns exemplos. A seguir a reação mais comum (18) foi a de rever procedimentos ou refletir acerca da intervenção, nomeadamente em equipa. Treze por cento procurou formação ou informação especializada ou dedicou-se à investigação na área. Por último, 5 dos profissionais de saúde referiu que passaram a envolver mais a família nestes casos.
Quatro profissionais de saúde (7) referiram implicações e mudanças na vida pessoal motivadas pelo suicídio do seu paciente. Uma maior capacidade de aceitação da vida em geral, vontade abandonar a psiquiatria (ainda que temporária), o ter que ir a tribunal por causa do caso e a opção pela saúde escolar, foram as implicações descritas.
Recursos de apoio e perceção da sua utilidade
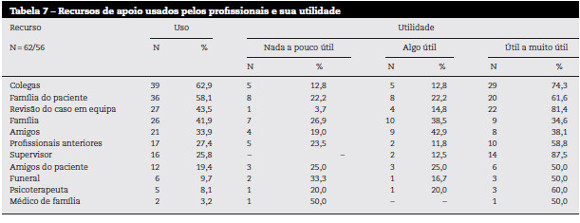
Perante uma lista de possíveis apoios, relativos à experiência do suicídio do paciente, 62 profissionais de saúde (97) indicaram quais os recursos usados e em que medida os mesmos foram úteis para lidar com a situação (Tabela 7). O recurso mais usado pelos profissionais foi o apoio dos colegas (63), seguido do contacto com a família do paciente (58), da revisão do caso em equipa (44) e do apoio da família do próprio profissional (42). Relativamente à utilidade destes apoios, os profissionais de saúde tendem a avaliar a supervisão como o recurso mais útil, seguindo-se a revisão do caso com a equipa e o apoio dos colegas. As medidas globais de uso de apoio (baixo ou muito baixo 68, moderado 25 e alto ou muito alto 7) e a medida global da avaliação da utilidade de recursos usados indicam-nos que, na generalidade, os profissionais de saúde tendem a recorrer pouco aos apoios apresentados, mas quando o fazem tendem a avaliá-los como úteis. A contrariar esta tendência, surgem a família e os amigos do profissional de saúde, cujas pontuações de utilidade são as mais baixas. Não se encontraram diferenças significativas de género na medida global de recurso a apoio, nem no score de utilidade. Da mesma forma não se encontraram diferenças nestas medidas entre os psicólogos e os médicos.
]]>
A grande maioria dos profissionais (98,4) referiram que não existe qualquer sistema formal de apoio na instituição onde trabalham, previsto para apoiar os profissionais que passam pela experiência de um paciente se suicidar.
Sugestões e outros comentários adicionais
Setenta por cento dos profissionais de saúde que passaram pelo suicídio de um paciente responderam ao desafio de aconselhar colegas inexperientes sobre a melhor forma de como lidar com este acontecimento. A sugestão mais frequente foi a de partilhar com colegas, incluindo colegas experientes e colegas de confiança (47). Seguiram-se conselhos de rigor na intervenção, nomeadamente na identificação do risco e na atuação vigilante e imediata, e onde se inclui o internamento e o encaminhamento para profissionais especializados (29). Proceder à revisão do caso (27) e procurar supervisão (20) foram também aconselhados. Aceitar que o suicídio de um paciente faz parte da profissão e evitar sentimentos de culpa foi referido por 13 dos profissionais. A mesma percentagem aconselha a que se articule com a família enlutada, incluindo a prestação de apoio, enquanto 11 salientam a importância de se manter nestes casos um distanciamento emocional do caso e da família, sendo que um dos profissionais desaconselha a participação nas cerimónias fúnebres. Por fim, 9 dos respondentes sugerem apoio interdisciplinar para o acompanhamento destes casos e que os profissionais perante o suicídio de um paciente recorram a psicoterapia.
Alguns profissionais (23) acrescentaram um comentário adicional relativo à vivência do suicídio do paciente. Estas observações foram no sentido de reforçar este acontecimento como uma experiência provável e perturbadora - «é uma morte que se carrega, é incomensurável» - apesar do reconhecimento do suicídio como uma possibilidade, um risco inevitável e a impossibilidade de prevenir todos os suicídios: «O suicídio de um paciente psiquiátrico é um mau outcome, mas provável em técnicos que lidem com pessoas em risco de suicídio». Nestas observações é também referida a necessidade de formação específica na área da suicidologia, especificamente por parte dos médicos de medicina geral e familiar: «é sempre uma experiência perturbante com que lido com alguma dificuldade. Os médicos de família necessitam de mais formação em saúde mental».
Discussão
Este estudo, realizado com psicólogos, psiquiatras e médicos de medicina geral e familiar, acrescenta novos dados à suicidologia, particularmente ao estudo do impacto do suicídio de um paciente em profissionais de saúde, área, até à data, inexplorada em Portugal.
Os dados empíricos deste estudo revelam que 27 dos profissionais de saúde experienciaram o suicídio de, pelo menos, um paciente. Esta frequência, entre os estudos que usaram amostras multidisciplinares, tem uma variação muito ampla: entre 195-706. Porém, diferenças na metodologia, nas taxas de resposta e na composição das amostras, em termos de grupos profissionais, limitam o valor destas comparações. Os dois estudos referenciados incluíram, para além de médicos e psicólogos, técnicos de serviço social, educadores sociais e enfermeiros como participantes, sendo este último o grupo com maior representatividade. Relativamente aos processos de amostragem, tal como no estudo português, foram identificados locais de trabalho, onde potencialmente os profissionais teriam pacientes que se tinham suicidado. Porém, no estudo com taxa mais elevada este processo incluiu uma pré-triagem destes locais, através de um questionário prévio às instituições, no sentido de identificar em quais tinha acontecido o suicídio de utentes nos últimos 5 anos. Apenas nas que responderam afirmativamente, os profissionais foram convidados a participar6. Ou seja, apesar de se tratarem de proporções de profissionais com pacientes que se suicidaram, a população da qual se extraíram os casos prevalentes é distinta, condicionando a comparabilidade. Num outro estudo, realizado com psiquiatras, psicólogos, enfermeiros, outros técnicos de saúde mental e técnicos de serviço social a taxa de suicídio de paciente encontrada foi de 21, mas esta prevalência apresentada refere-se ao período de estágio ou internato destes profissionais4.
]]> De acordo com o esperado, e com o descrito na literatura internacional9, 28, neste estudo encontraram-se diferenças significativas na frequência de suicídio de pacientes entre os três grupos profissionais, sendo que, para os psiquiatras este é um risco acrescido. Neste estudo, 55 dos psiquiatras tiveram pelo menos um paciente que se suicidou, reforçando a evidência que esta é uma experiência comum para estes profissionais. Esta frequência é comparável às taxas obtidas em estudos realizados com psiquiatras no Canadá (50)13 e nos EUA (51)10 e inferior às taxas obtidas em estudos com psiquiatras escoceses (68)8, irlandeses (80-82)41, 42 e belgas (92)43.A percentagem de psicólogos portugueses que tiveram um paciente que se suicidou foi de 11. Comparando com pesquisas norte-americanas, efetuadas com este grupo profissional, verifica-se que a taxa portuguesa é inferior à encontrada numa amostra de psicólogos (22)9, mas igual à obtida numa amostra de psicólogos estagiários (11)12.
Num estudo irlandês os autores encontraram uma frequência de 86 de médicos de medicina geral com pacientes que se tinham suicidado21, taxa consideravelmente mais elevada que a obtida no nosso estudo (38). No entanto, os dados empíricos disponíveis acerca da frequência do suicídio de pacientes dos médicos de medicina geral são muito escassos. Apesar desta lacuna, os estudos que procuram determinar as taxas de contacto dos suicidas com cuidados de saúde primários fornecem indicadores indiretos de que esta frequência será elevada: em média, cerca de metade dos suicidas contactam com médicos de medicina geral durante o ano antecedente à morte15, 16, 17, 18 e cerca de 20 estabelecem este contacto dias antes da morte18. Em pacientes idosos estes números são ainda mais impressionantes: 73 visita o seu médico de família no mês antecedente ao suicídio43. Estes dados foram calculados a partir da revisão de estudos que disponibilizam dados do contacto com os cuidados de saúde de suicidas antes do ato fatal (incluindo autopsias psicológicas e análise de registos)16, 18, ou na própria revisão de registos médicos e médico-legais17, 44.
Para além de diferenças entre os grupos profissionais, constatou-se que era mais provável um profissional de saúde masculino ter passado pela experiência do suicídio de um paciente que uma profissional de saúde feminina. Os dados disponíveis relativos a estas diferenças de género não são consensuais. Há estudos que encontraram, tal como neste, diferenças nas proporções entre os que tiveram e os que não tiveram pacientes suicidas45, enquanto noutros estudos estas diferenças não foram significativas9, 12. Outros dados mostram que, dentro dos que passaram pela experiência, os homens tiveram mais suicídios de pacientes que as mulheres43.
Este estudo mostra que o suicídio de um paciente tem um impacto emocional e profissional considerável nos médicos e psicólogos portugueses - «é uma experiência que não nos abandona enquanto formos terapeutas, fica cá dentro» causando sofrimento emocional e outros sentimentos negativos, tais como, medo, frustração, choque, sentimento de fracasso, culpa, entre outros, e levando a mudanças na prática clínica. Estes resultados estão de acordo com o encontrado em pesquisas internacionais.
Os resultados deste estudo permitem sintetizar o impacto do suicídio de um paciente em efeitos positivos e negativos para prática clínica, à semelhança do apresentado numa investigação com internos de psiquiatria46. Os efeitos positivos, referidos por uma percentagem elevada dos participantes, correspondem à experiência de aprendizagem que este acontecimento proporcionou, traduzindo-se numa maior atenção e rigor na avaliação do risco e na intervenção com eventuais suicidas. Incluíram ainda, ações realizadas com o intuito de melhorar a prática, tais como revisão de procedimentos e o investimento em formação especializada. Os efeitos negativos ou potencialmente prejudiciais para a prática clínica foram referidos por 28 dos profissionais de saúde e incluíram maior insegurança, incerteza e ansiedade ao lidar com pacientes e famílias e um enfraquecimento da confiança nas próprias capacidades profissionais. Litman24 reforça que níveis de ansiedade excessivos perante a possibilidade de comportamentos suicidas podem comprometer a eficácia dos terapeutas nestes casos. O suicídio de um paciente, considerado como um dos acontecimentos mais perturbadores da prática clínica1, 2, 3, pode também constituir-se como uma oportunidade de aprendizagem profissional.
Os sentimentos e reações descritos pelos profissionais de saúde deste estudo indicam a vivência de um processo de luto - «sentimento de perda, tristeza profunda, desgosto, dor» -. Simultaneamente, os resultados são também reveladores da existência de reequacionamento de questões profissionais, incluindo o confronto com limitações - «fiz tudo o que podia para evitar?» - e responsabilidades - «reforcei o meu sentimento de responsabilidade». Inclui ainda a adaptação de estratégias profissionais. De acordo com Litman24, após o suicídio de um paciente coexistem dois tipos de reação: uma reação pessoal relacionada com um processo de luto normal e uma reação relacionada com a função profissional específica.
Neste estudo 22 dos profissionais de saúde relataram sentimentos de fracasso e 18 de culpa perante o suicídio do seu paciente. Embora o tema da adaptação e coping pós-suicídio seja gerador de alguma discórdia na literatura, parece que poucos acontecimentos da prática clínica serão causadores de um sentimento de fracasso e culpa tão intensos como o suicídio de um paciente47. Perante outro tipo de mortes, nomeadamente decorrentes de doença grave não psiquiátrica, mais facilmente se considera a ocorrência como inevitável. Ao contrário, o suicídio é tendencialmente perspetivado como evitável e possível prevenir, gerando nos profissionais o sentimento de que poderiam ter feito melhor, deveriam ter estado mais atentos aos sinais ou que deviam ter sido mais rigorosos e vigilantes quanto a questões de internamento ou follow-up. Neste estudo, apenas 7 descreveu sentir o suicídio do seu paciente como um resultado inevitável ou uma solução aceitável (face a uma dor insuportável e prolongada no tempo). Simultaneamente, 53 retrospetivaram o suicídio do seu paciente como nada ou pouco previsível e 35 consideraram que não teria sido possível preveni-lo. Estes dados parecem refletir a dificuldade que é para os profissionais equilibrarem atitudes perante o suicídio de um paciente. Ou seja, considerarem o suicídio como inevitável e imprevisível pode protegê-los da culpa e evitar uma cultura de responsabilidade excessiva. Ao mesmo tempo, esta atitude poderá promover descrença nos efeitos da intervenção clínica8, agravada pelo fraco poder preditivo dos fatores de risco do suicídio48, 49 e pelo facto das estratégias de prevenção eficazes com base na evidência científica serem muito reduzidas50, 51.
Com este estudo ficamos também a saber que, em caso de suicídio de um paciente, não existem sistemas de apoio específicos nos diferentes locais de trabalho e que, para além disso, os profissionais de saúde tendem a não pedir ajuda nestas circunstâncias. Porém, quando recorrem a algum tipo de suporte avaliam-no, geralmente, como útil. Uma primeira possível explicação para os profissionais recorrerem pouco a ajuda é a da experiência não carecer de suporte específico. Mas os dados deste estudo contariam esta explicação: os recursos avaliados como menos úteis são, exatamente, os suportes não especializados ou específicos da situação - amigos e família do próprio profissional. Assim, outra hipótese de explicação prende-se com o estigma social e profissional a que se mantém ligado este acontecimento. O suicídio de um paciente é visto como um resultado profissional errado e associado a uma falha do clínico (como já discutido). Esta atitude pode contribuir para uma resistência na procura de ajuda e criar barreiras à adoção de ações adequadas pós-suicídio. Designadas na literatura internacional por medidas de postvention, estas ações incluem providenciar apoio à família do suicida, a outros elementos da equipa que tenham acompanhado o paciente (como por exemplo enfermeiros) e a outros pacientes (particularmente em meio hospitalar), assim como de garantir suporte ao próprio clínico25, 32, 47, 52, 53, 54, 55, 56, 57.
De acordo com o encontrado em pesquisas empíricas anteriores3, 5, 13, 43, 58, 59, o apoio dos colegas foi o recurso pós-suicídio mais utilizado pelos profissionais de saúde e avaliado como um dos mais úteis. O recurso avaliado com maior utilidade, o supervisor, foi usado por poucos profissionais, refletindo, provavelmente, a dificuldade em aceder à supervisão, quer pelo tipo de (in) disponibilidade deste recurso em meios institucionais, quer pelo facto de implicar em muitos casos, gastos económicos consideráveis. Apesar da escassez de dados empíricos específicos, a literatura defende que a supervisão pode ter um papel importante para o profissional de saúde em casos de suicídio de um paciente12, 13, 33, 52, 53, 60, 61.
]]> O contacto com a família do suicida, tendo uma dupla função, de apoio aos familiares e de integração da experiência por parte do profissional, e a revisão do caso em equipa, ambos claramente aconselhados na literatura como práticas a seguir pós-suicídio, foram validados pelos resultados deste estudo.Apenas 10 dos profissionais foram ao funeral do seu paciente, percentagem inferior à encontrada em amostras de psiquiatras belgas (17)59 (26)43 e escoceses (15)8 e psicólogos norte-americanos (18)12. Na literatura é referido que, na generalidade, os profissionais de saúde não vão às cerimónias fúnebres, mas aqueles que o fazem consideram-no útil, quer para si quer para a família enlutada12, 62, 63. Neste estudo, metade dos profissionais que foram ao funeral consideraram-no útil.
Para além da revisão de caso, da partilha com os colegas, da supervisão, do contacto com a família e da presença no funeral ou envio de cartão de condolências, a literatura aconselha também a formação especializada como recurso adequado para lidar com este acontecimento13, 56, 59, 64. Nesta investigação, apenas 18 têm formação especializada e mais de metade considera a sua preparação insuficiente para acompanhar pacientes suicidas. A necessidade de formação, para melhorar competências na intervenção com comportamentos suicidários, é reconhecida pela maioria dos participantes. Será assim essencial que a formação em suicidologia se generalize a mais profissionais de saúde. Esta formação, para além dos conteúdos tradicionalmente abordados (avaliação do risco, gestão da crise, epidemiologia, fatores de risco), deverá incluir procedimentos de postvention, assim como componentes formativas em que se antecipe o suicídio de um paciente como um risco provável, e se reflita acerca de questões de responsabilidade3, 64.
A formação suicidológica recebida nas diferentes formações académicas é escassa. Um estudo recente com profissionais de saúde portugueses revela que as dificuldades no acompanhamento de indivíduos suicidas podem situar-se em 4 níveis diferentes: nível técnico (p. ex. avaliação do risco), nível emocional (p. ex. medo que o indivíduo se suicide), nível relacional e comunicacional (p. ex. como dialogar com o paciente acerca da morte) e ao nível da abordagem da família.1 As limitações da formação com consequências ao nível das competências de avaliação e gestão de pacientes suicidas por parte dos profissionais de saúde não é exclusiva do nosso pais65, 66, 67. Acresce que tem vindo a ser demonstrado que uma das estratégias eficazes de prevenção do suicídio com base na evidência é a formação dos profissionais de saúde, com destaque para os médicos de família49, 50. Juntam-se ainda dados que revelam que dada a complexidade da intervenção com pacientes suicidas é necessário formação contínua, específica e baseada na experiência68.
Neste estudo, não se encontraram diferenças significativas entre géneros na experiência do suicídio de um paciente, ou seja, apesar de ser mais provável para um profissional de saúde homem ter tido um paciente que se suicidou, quando passam pela situação, homens e mulheres parecem ter vivenciado este acontecimento de forma semelhante. Também não foram encontradas diferenças entre géneros ao nível da utilização dos recursos de apoio pós-suicídio. Estes resultados contrastam com estudos anteriores5, 6, 14, 29, 31, 42.
Em relação ao grupo profissional a literatura não é consensual nem linear. Existem estudos que, tal como este, não encontraram diferenças entre grupos profissionais31. Outros obtiveram níveis de impacto emocional negativo significativamente mais elevado nos psiquiatras que nos psicólogos29. Outros ainda, não encontram diferenças na intensidade das respostas, mas identificaram efeitos significativos nas mudanças das práticas profissionais entre alguns grupos específicos6.
Este estudo apresenta algumas limitações metodológicas. Em primeiro lugar, a representatividade não pode ser garantida através do processo de amostragem utilizado (focalizada cruzado com bola de neve). Porém, foram usados procedimentos metodológicos adicionais que fazem com que um viés sistemático seja improvável. Em segundo lugar, o facto de se seguir um desenho que assegura o anonimato, torna impossível verificar que percentagem, dos que não responderam, teve ou não pacientes que se suicidaram, condicionando o valor da taxa de profissionais com suicídio de pacientes. Terceiro, e porque o objetivo do estudo era descrever os sentimentos e reações perante o suicídio de paciente considerado pelos profissionais de saúde com maior impacto, o estudo poderá não ser representativo de todos os suicídios com que os profissionais lidaram. De referir ainda a impossibilidade, do cálculo da taxa de resposta ao estudo dado o desenho metodológico.
A investigação futura deverá explorar relações entre atitudes perante o suicídio e impacto do suicídio de um paciente, aprofundar o estudo dos efeitos das variáveis socioprofissionais, incluindo variáveis de formação, e ainda estudar dificuldades específicas dos profissionais perante comportamentos suicidários. Aconselha-se ainda o uso de entrevistas de profundidade no sentido de apurar fatores chave para o processo de adaptação e aprendizagem após o suicídio de um paciente.
Como referiram os profissionais de saúde, o suicídio de um paciente apesar de ser «um risco inevitável para quem trabalha com certo tipo de população, é uma experiência muito difícil de viver». Assim, caberá à investigação produzir mais conhecimento sobre o impacto deste acontecimento, os processos de adaptação por parte dos profissionais e os fatores que medeiam o mesmo, no sentido de promover que esta experiência difícil seja uma oportunidade de crescimento pessoal e profissional e potencie intervenções futuras de qualidade com pacientes em risco.
]]> Bibliografía
1. Deutsch CJ. Self-reported sources of stress among psychotherapists. Prof Psychol-Res Pract. 1984; 15:833-45. [ Links ]
2. Menninger WW. Anxiety in the psychotherapist. Bull Menninger Clin. 1990; 54:232-46. [ Links ]
3. Menninger WW. Patient suicide and its impact on the psychotherapist. Bull Menninger Clin. 1991; 55:216-27. [ Links ]
4. Brown HN. The impact of suicide on therapists in training. Compr Psych. 1987; 28:101-12. [ Links ]
5. Gaffney P, Russell V, Collins K, Bergin A, Halligan P, Carey C, et-al. Impact of patient suicide on front-line staff in Ireland. Death Studies. 2009; 33:639-56. [ Links ]
6. Gulfi A, Dransart D, Heeb JL, Gutjahr E. The Impact of patient suicide on the professional reactions and practices of mental health caregivers and social workers. Crisis. 2010; 31:202-10. [ Links ]
7. Linke S, Wojciak J, Day S. The impact of suicide on community mental health teams: findings and recommendations. Psych Bull. 2002; 26:50-2. 2002. [ Links ]
8. Alexander D, Klein S, Gray N, Dewar I, Eagles J. Suicide by patients: questionnaire study of its effect on consultant psychiatrists. BMJ. 2000; 320:1571-4. [ Links ]
9. Chemtob CM, Hamada RS, Bauer G, Kinney B, Torigoe RY. Patient suicide: frequency and impact on psychologists. Am J Psychiatry. 1988; 19:416-20. [ Links ]
10. Chemtob CM, Hamada RS, Bauer G, Kinney B, Torigoe RY. Patients' suicides: frequency and impact on psychiatrists. Am J Psychiatry. 1988; 145:224-8. [ Links ]
11. Chemtob CM, Bauer GB, Hamada RS, Pelowsky SR, Muraoka MY. Patient suicide: occupational hazard for psychologists and psychiatrists. Am J Psychiatry. 1989; 20:294-300. [ Links ]
12. Kleespies PM, Penk WE, Forsyth JP. The stress of patient suicidal behavior during clinical training: incidence, impact, and recovery. Am J Psychiatry. 1993; 24:293-303. [ Links ]
13. Ruskin R, Sakinofsky I, Bagby RM, Dickens S, Sousa G. Impact of patient suicide on psychiatrists and psychiatric trainees. Acad Psychiatry. 2004; 28:104-10. [ Links ]
14. Wurst FM, Kunz I, Skipper G, Wolfersdorf M, Beine K, Thon N. The therapists' reaction to a patient suicide, results of a survey and implications for healthcare professionals' well-being. Crisis. 2011; 32:99-105. [ Links ]
15. Bryan CJ, Rudd MD. Managing suicide risk in primary care. New York: Springer Publishing Company; 2011. [ Links ]
16. Luoma JB, Martin CE, Pearson JL. Contact with mental health and primary care providers before suicide: a review of the evidence. Am J Psychiatry. 2002; 159:909-16. [ Links ]
17. Pearson A, Saini P, da Cruz D, Miles C, While D, Swinson N, et-al. Primary care contact prior to suicide in individuals with mental illness. Br J Gen Pract. 2009; 59:825-32. [ Links ]
18. Pirkis J, Burgess P. Suicide and recency of health care contacts: a systematic review. Br J Psychiatry. 1998; 173:462-74. [ Links ]
19. Slap G, Vorters D, Khalid N, Margulis S, Forke C. Adolescent suicide attempters: do physicians recognize them?. J Adolesc Health. 1992; 13:286-92. [ Links ]
20. Davidsen AS. 'And then one day he'd shot himself. Then I was really shocked': general practitioners' reaction to patient suicide. Patient Educ Couns. 2011; 85:113-8. [ Links ]
21. Halligan P, Corcoran P. The impact of patient suicide on rural general practitioners. Br J Gen Pract. 2001; 51:295-6. [ Links ]
22. Kendall K, Wiles R. Resisting blame and managing emotion in general practi the case of patient suicide. Soc Sci Med. 2010; 70:1714-20. [ Links ]
23. Horn P. Therapists' psychological adaptation to client suicide. Psychotherapy. 1994; 31:190-5. [ Links ]
24. Litman RE. When patients commit suicide. Am J Psychother. 1965; 19:570-6. [ Links ]
25. Hendin H, Lipschitz A, Maltsberger JT, Haas AP, Wynecoop S. Therapists' reactions to patients' suicides. Am J Psychiatry. 2000; 157:2022-7. [ Links ]
26. Yousaf F, Hawthorne M, Sedgwick P. Impact of patient suicide on psychiatric trainees. Psych Bull. 2002; 26:53-5. [ Links ]
27. Foley S, Kelly B. When a patient dies by suicide: incidence, implications and coping strategies. Adv Psych Treat. 2007; 13:134-8. [ Links ]
28. VanLith CD. Psychotherapists as patient suicide survivors: a review of the literature on psychiatrists and psychologists, including those in training. California: Biola Univ; 1996. Doctoral dissertation. [ Links ]
29. Wurst FM, Mueller S, Petitjean S, Euler S, Thon N, Wiesbeck G, et-al. Patient suicide: a survey of therapists' reactions. Suicide Life Threat Behav. 2010; 40:328-36. [ Links ]
30. Kahne MJ. Suicide among patients in mental hospitals: a study of the psychiatrists who conducted their psychotherapy. Psychiatry. 1968; 31:32-43. [ Links ]
31. Grad OT, Zavasnik A, Groleger U. Suicide of a patient: gender differences in bereavement reactions of therapists. Suicide Life Threat Behav. 1997; 27:379-86. 1997. [ Links ]
32. Hendin H, Haas AP, Maltsberger J, Szanto K, Rabinowicz H. Factors contributing to therapists' distress after the suicide of a patient. Am J Psychiatry. 2004; 161:1442-6. [ Links ]
33. Kleespies PM, Smith MR, Becker BR. Psychology interns as patient suicide survivors: incidence, impact and recovery. Prof Psychol-Res Pract. 1990; 21:257-63. [ Links ]
34. Pilkinton P, Etkin M. Encountering suicide: the experience of psychiatric residents. Acad Psychiatry. 2003; 27:93-9. [ Links ]
35. Watters JK, Biernacki P. Targeted sampling: options for the study of hidden populations. Soc Probl. 1989; 36:416-30. [ Links ]
36. Browne K. Snowball sampling: using social networks to research non-heterosexual women. Int J Soc Res Method. 2005; 8:47-60. [ Links ]
37. Faugier J, Sargeant M. Sampling hard to reach populations. J Adv Nurs. 1997; 26:790-7. [ Links ]
38. Heckathorn D. Respondent-driven sampling: a new approach to the study of hidden populations. Soc Probl. 1997; 44:174-99. [ Links ]
39. Heckathorn D. Respondent-driven sampling: II. Deriving valid population estimates from chain-referral samples of hidden populations. Soc Probl. 2002; 49:11-34. [ Links ]
40. Negreiros J, Magalhães A. Estimativas da prevalência do consumo problemático de drogas - Portugal 2005. Lisboa: Instituto da Droga e da Toxicodependência, I.P; 2009. [ Links ]
41. Landers A, O'Brien S, Phelan D. Impact of patient suicide on consultant psychiatrists in Ireland. Psych Online. 2010; 34:136-40. [ Links ]
42. Cryan EMJ, Kelly P, McCaffrey B. The experience of patient suicide among Irish psychiatrists. Psych Bull. 1995; 19:4-7. [ Links ]
43. Rothes I, Scheerder G, van Audenhove C, Henriques M. Patient suicide: The experience of Flemish psychiatrists. Suicide Life Threat Behav. 2013. [ Links ]
44. Juurlink DN, Herrmann N, Szalai JP, Kopp A, Redelmeier DA. Medical illness and the risk of suicide in the elderly. Arch Intern Med. 2004; 164:1179-84. [ Links ]
45. Pope KS, Tabachnick BG. Therapists' anger, hate, fear, and sexual feelings: National survey of therapist responses, client characteristics, critical events, formal complaints, and training. Prof Psychol-Res Pract. 1993; 24:142-52. [ Links ]
46. Courtenay KP, Stephens JP. Patient suicide experienced by psychiatric trainees. Psych Bull. 2001; 25:51-2. [ Links ]
47. Lloyd GG. Suicide in hospital: guidelines for prevention. J R Soc Med. 1995; 88:344-6. [ Links ]
48. Eagles J, Klein S, Gray N, Dewar I, Alexander D. Role of psychiatrists in the prediction and prevention of suicide: a perspective from north-east Scotland. Br J Psychiatry. 2001; 178:494-6. [ Links ]
49. Powell J, Geddes J, Deeks J, Goldacre M, Hawton K. Suicide in psychiatric hospital in-patients: risk factors and their predictive power. Br J Psychiatry. 2000; 176:266-72. [ Links ]
50. Mann JJ, Apter A, Bertolote J, Beautrais A, Currier D, Haas A, et-al. Suicide prevention strategies: a systematic review. JAMA. 2005; 294:2064-74. [ Links ]
51. van der Feltz-Cornelis CM, Sarchiapone M, Postuvan V, Volker D, Roskar S, Grum AL, et-al. Best practice elements of multilevel suicide prevention strategies: a review of systematic reviews. Crisis. 2011; 32:319-33. [ Links ]
52. Ellis TE, Dickey TO, Jones EC. Patient suicide in psychiatry residency programs: a national survey of training and postvention practices. Acad Psychiatry. 1998; 22:181-9. [ Links ]
53. Campbell C, Fahy T. The role of the doctor when a patient commits suicide. Psychiatric Bulletin. 2002; 26:44-9. [ Links ]
54. Farberow N. The mental health professional as suicide survivor. Clin Neuropsy. 2005; 2:13-20. [ Links ]
55. Hodelet N, Hughson M. What to do when a patient commits suicide?. Psych Bull. 2001; 25:43-5. [ Links ]
56. Michel K, Armson S, Fleming G, Rosenbauer C, Takahashi Y. After suicide: who counsels the therapist?. Crisis. 1997; 18:128-39. [ Links ]
57. Sakinofsky I. The aftermath of suicide: managing survivors' bereavement. Can J Psychiatry. 2007; 52:129S-36S. [ Links ]
58. Goldstein LS, Buongiorno PA. Psychotherapists as suicide survivors. Am J Psychother. 1984; 38:392-8. [ Links ]
59. Pieters G, de Gucht V, Joos G, de Heyn E. Frequency and impact of patient suicide on psychiatric trainees. Eur Psychiatry. 2003; 18:345-9. [ Links ]
60. Knox S, Burkard AW, Jackson JA, Schaack AM, Hess SA. Therapists-in-training who experience a client suicide: implications for supervision. Prof Psychol-Res Pract. 2006; 37:547-57. [ Links ]
61. Lafayette JM, Stern TA. The impact of a patient's suicide on psychiatric trainees: a case study and review of the literature. Harv Rev Psychiatry. 2004; 12:49-55. [ Links ]
62. Campbell FR. Aftermath of suicide: the clinician's role. En: Simon R.I., Hales R.E., editors. Textbook of suicide assessment and management. Washington, DC: American Psychiatric Publishing; 2006. 459-76. [ Links ]
63. Tanney B. After a suicide: a helper's handbook. En: Mishara B., editors. The impact of suicide. New York: Springer Publishing Company; 1995. 85-99. [ Links ]
64. Brown HN. Patient suicide during residency training (1): incidence, implications, and program response. J Psychiatr Educ. 1987; 11:201-16. [ Links ]
65. Hawgood JL, Krysinska KE, Ide N, de Leo D. Is suicide prevention properly taught in medical schools?. Med Teach. 2008; 30:287-95. [ Links ]
66. Palmieri G, Forghieri M, Ferrari S, Pingani L, Coppola P, Colombini N, et-al. Suicide intervention skills in health professionals: a multidisciplinary comparison. Arch Suicide Res. 2008; 12:232-7. [ Links ]
67. Schmitz WM, Allen MH, Feldman BN, Gutin NJ, Jahn DR, Kleespies PM, et-al. Preventing suicide through improved training in suicide risk assessment and care: an american association of suicidology task force report addressing serious gaps in U.S. mental health training. Suicide Life Threat Behav. 2012; 42:292-304. doi: 10.1111/j.1943-278X. 2012.00090.xDOI: 10.1111/j.1943-278X. 2012.00090.x. [ Links ]
68. Scheerder G, Reynders A, Andriessen K, van Audenhove C. Suicide intervention skills and related factors in community and health professionals. Suicide Life Threat Behav. 2010; 40:115-24. [ Links ]
Financiamento
Este artigo foi financiado pela Fundação para a Ciência e Tecnologia (FCT) como uma bolsa de investigação do QREN - POPH - Tipologia 4.1 - Formação Avançada subsidiada pelo Fundo Social Europeu e fundos nacionais de MCTES.
]]>Conflito de interesses
Os autores declaram não haver conflito de interesses.
Agradecimentos
Gostaríamos de expressar o nosso agradecimento a todos os médicos e psicólogos que participaram no estudo e a todos os que colaboraram na angariação de potenciais participantes.
Apêndice. Material adicional
Pode consultar o material adicional para este artigo na sua versão eletrónica disponível em doi:10.1016/j.rpsp.2013.05.002.
1 Rothes I, Henriques M, Leal J, Lemos M. Facing a patient who seeks help after a suicide attempt: difficulties of health professionals. Crisis. 2013. Manuscript under review.
]]>Recebido 10 Abril 2012. Aceito 23 Maio 2013
*Autor para correspondência. irothes@gmail.com
]]>