Ulcerated infantile hemangioma
Hemangioma infantil ulcerado
Nídia BeloI, Patrícia MaioI, Susana GomesI, Carla CruzI, Maria João P. LopesII
I Pediatrics Department, Hospital do Espírito Santo de Évora. 7000-811 Évora, Portugal. nidia.belo@gmail.com; patriciaspmaio@gmail.com; susana_gomes@netcabo.pt; carla.cruz.aguiar@gmail.com
II Dermatology Department, Centro Hospitalar Lisboa Central. 1169-050 Lisboa, Portugal. mjfigueiroa@sapo.pt
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Infantile hemangiomas are the most frequent vascular tumors in pediatric age. Diagnostic can be challenging due to variable clinical presentation and natural history. Most cases have a favorable evolution. Treatment may be required according to tumor location, extension, and complications. Propranolol is an effective and safe treatment.
]]> The case of an infant with perianal ulcerated hemangiomas treated with propranolol with clinical improvement is reported.Keywords: infantile hemangioma; propranolol; ulceration
RESUMO
Os hemangiomas infantis são os tumores vasculares mais comuns em pediatria, mas o seu diagnóstico pode ser dificultado pela apresentação clínica e história natural variáveis. A maioria dos casos apresenta evolução favorável, porém a sua localização, extensão e complicações podem determinar necessidade terapêutica. O propranolol é uma terapêutica eficaz e segura.
É apresentado o caso de uma lactente com hemangioma perianal ulcerado tratado com propranolol com boa evolução clínica.
Palavras-chave: hemangioma infantil; propranolol; ulceração
Introduction
Infantile hemangioma (IH) is a benign vascular tumor affecting approximately 4−5% of children. It is more frequent in the Caucasian population, females, premature infants, low-birth-weight newborns, and twins. IH usually appears in the first weeks of life and may be preceded by a precursor lesion.1
]]> Natural history of IH has three phases.2 The proliferative phase is characterized by a rapid growth in the first months of life, often lasting three months. It is followed by a stabilization phase and a subsequent spontaneous gradual resolution (involutive) phase, lasting for two to six years. Complete resolution is usually attained by the age of ten. After involution, residual lesions as scarring, telangiectasia, or cutaneous atrophy may remain.2 Complete resolution of the condition seems to be related to the early onset of its involution.3IH diagnosis is clinical, based on history and clinical examination, but it can be challenging in cases of deep hemangiomas, atypical location, or when IH is associated with complications.4 Radiology may be useful in differential diagnosis, evaluation of size, type, and extension of IH, as well as in monitoring treatment response.3
Most IHs have a favorable evolution, hence an expectant attitude is recommended. Treatment should be considered according to patient’s age, size, number, and location of IH, associated symptoms, and evolutionary phase of the IH.3 Treatment is often required within the first months of life for cases associated with vital, organic, or esthetic commitment, or complicated IH, such as ulcerated hemangiomas.1
Classic therapeutic approach includes systemic or intralesional corticosteroids. In IH sensitive to steroids, a favorable response is observed one week after therapeutic initiation. However, adverse effects are not negligible and may include cushingoid facies, arterial hypertension, growth retardation, and an increased risk of fungal infections.5 After therapeutic suspension, rebound effect and IH relapse may occur.
Treatment with oral propranolol has emerged as an effective and safe option and is currently considered the first-line therapy in IH. Propranolol is a non-selective beta-blocker with a not fully clarified mechanism of action. Beneficial effects in the treatment of IH are attributed to its vasoconstriction action, inhibition of angiogenesis, and induction of apoptosis.1,6
A multidisciplinary approach is required, encompassing Pediatrics, Dermatology, Cardiology, and other medical specialties, when appropriate.7
Clinical case
The case of a female infant with irrelevant family history and prenatal background with no intercurrences is presented. At 15 days of age, she presented a perianal erythematous lesion that evolved to a flat ulcer (15mm) with marginal erythema and perilesional exsudate. The lesion was painful mainly during hygiene procedures and defecation. According to the mother, the child had a skin thickening at the lesion site since birth. She maintained a linear weight and length progression without other cutaneous or mucosal lesions and reported no episodes of infectious diseases or gastrointestinal alterations.
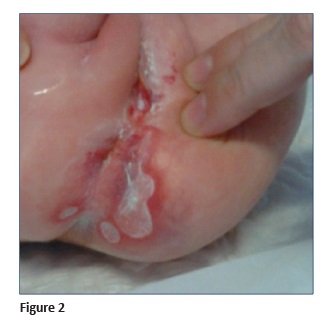
At the age of one month, the child was hospitalized to treat a presumed infected perianal ulcer and was medicated with systemic and topical antibiotics and topical antiseptic, with no improvement (Figure 1).
]]>
Laboratory tests revealed no indirect parameters of bacterial infection, and immunity study and determination of seric zinc were normal.
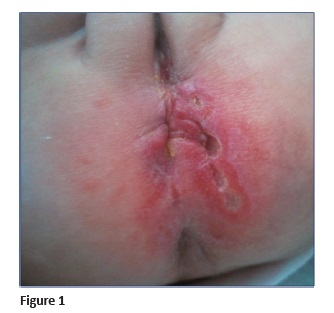
By two months old, she presented small-dimension vascular formations, perilesional and in the large left lip (Figure 2). At this time, a diagnostic hypothesis of ulcerative perianal hemangioma was raised. Abdominopelvic and lumbosacral nuclear magnetic resonance revealed an image compatible with vascular structure and excluded extension of the lesion to deep planes, organic invasion, and other structural anomalies.
The girl was submitted to a pre-therapeutic evaluation which included electrocardiogram, blood pressure, and blood glucose. She initiated propranolol therapy at three months of age. Treatment was started in elective hospitalization under monitoring according to the national protocol, with oral propranolol up to a target dose of 3mg/ kg/day, tid.9
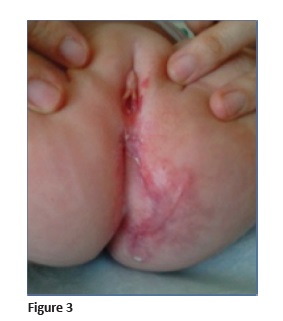
The infant had a regular follow-up. A rapid and favorable response was observed, with ulcer healing one month after treatment initiation and progressive involution of IH with formation of fibrotic scar tissue (Figure 3−4). Therapy was well tolerated, with no complications or adverse events observed.
]]>
The child underwent a total of 16 months of therapy, with progressive reduction of propranolol dose until suspension.
At 24 months of age, corresponding to the fifth month post- treatment suspension, she presented residual fibrosis, with no relapses (Figure 4). No evidence of other hemangiomas was observed.
Discussion
The variable natural evolution and clinical presentation of IH complicate the diagnosis, especially when angiomatous lesion is preceded by complications. Ulceration is the most common complication, occurring mainly in the proliferative phase. This complication causes intense pain and discomfort, especially when ulceration affects the lips, perianal, and genital regions.2-4 Consideration of IH diagnosis is essential to avoid unnecessary testing and treatment.
Most IHs evolve with spontaneous regression, and an expectant attitude can be adopted. When treatment is indicated, propranolol should be started as soon as possible.
In this clinical case, given IH location, local ulceration, and intense pain, decision to start propranolol was made. An excellent initial response was observed during the proliferative IH phase, with progressive involution of the hemangioma, probably due to the early therapeutic institution. As a consequence, a good analgesic response was observed.
]]> Although safe, propranolol is not free of adverse effects. They are, however, uncommon, and include bradycardia, hypotension, hypoglycemia, wheezing, and sleep disorders.8 Their monitoring is essential, especially during the therapeutic induction phase.Protocols for induction, maintenance, dose, and duration of propranolol therapy are variable. The recommended target dose is 1 to 3 mg/kg/day in three doses after an initial period of therapeutic induction. Treatment should be maintained up to 12−16 months of age.8-9
Rate of relapse after therapeutic withdrawal is estimated at 19−25%, especially if propranolol suspension occurs before the age of nine months.10
Further studies are required to develop consensual guidelines.
IH with lumbosacral or anogenital location may be associated with medullar dysraphism or anogenital anomalies. Magnetic resonance is the gold standard examination for this investigation. In the present case, imaging allowed to evaluate lesion extent and to exclude associated anomalies.
Key messages
1. Diagnosis of infantile hemangioma can be difficult, especially when complicated.
2. Early diagnosis is essential to avoid unnecessary testing and treatment.
3. Propranolol initiated in an early stage allows a good response.
4. The lumbosacral or anogenital location imposes investigation of spinal cord dysraphism or anogenital anomalies.
]]>REFERENCES
1. Ravenscroft J. Management of infantile haemangioma. Paediatrics and Child Health. 2014; 25:2. [ Links ]
2. Nina BID, Oliveira ZNP, Machado MCMR, Macea JM. Apresentação, evolução e tratamento dos hemangiomas cutâneos - experiência do Ambulatório de Dermatologia Infantil do Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo. An Bras Dermatol. 2006; 81: 323-7. [ Links ]
3. Gontijo B, Silva CMR, Pereira LB. Hemangioma da infância. An Bras Dermatol. 2003; 78: 651-73. [ Links ]
4. Lanoel A, Tosi V, Bocian M, Lubieniecki F, Poblete SB, García HO, et al. Úlceras perianales sobre hemangioma con crecimiento mínimo o detenido segmentário. Actas Dermosifiliogr. 2012; 103: 820-3. [ Links ]
]]>5. Bonini FK, Bellodi FS, Souza EM. Hemangioma infantil tratado com propranolol. An Bras Dermatol. 2011; 86:763-6. [ Links ]
6. Hiraki PY, Goldenberg DC. Diagnóstico e tratamento do hemangioma infantil. Rev Bras Cir Plást. 2010; 25:388-97. [ Links ]
7. Melo IS, Gonçalves V, Anjos R. Propranolol nos hemangiomas infantis: casuística nacional com 30 doentes. Acta Pediatr Port 2012; 43:190-4. [ Links ]
8. Drolet BA, Frommelt PC, Chamlin SL, Haggstrom A, Bauman NM, Chiu YE, et al. Initiation and use of propranolol for infantile hemangioma: Report of a Consensus Conference. Pediatrics. 2013; 131:128- 40. [ Links ]
9. Lawley LP. Siegfried E, Todd JL. Propranolol treatment for hemangioma of infancy: risks and recomendations. Pediatr Dermatol. 2009; 26:610-4. [ Links ]
]]>10. Shah SD, Baselga E, McCuaig C, Pope E, Coulie J, Boon LM. Rebound growth of infantile hemangiomas after propranolol therapy. Pediatrics. 2016; 137:1-8. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Nídia Belo
Pediatrics Department
Hospital do Espírito Santo de Évora Largo Sr. da Pobreza
7000-811 Évora
Email: nidia.belo@gmail.com
]]> Received for publication: 17.01.2018
Accepted in revised form: 05.09.2018
]]>