(clique para ampliar ! click to enlarge)
Psychological repercussions after stroke: a literature review
Catiele Reis1 & André Faro1
1Universidade Federal de Sergipe; Centro Universitário Ages, São Cristóvão - SE, Brasil, catiele.reis@gmail.com
2Universidade Federal de Sergipe, São Cristóvão - SE, Brasil; CAPES, Brasil, andre.faro.ufs@gmail.com
RESUMO
Este estudo apresenta uma revisão integrativa de literatura acerca das principais repercussões psicológicas relacionadas à adaptação da vítima após um Acidente Vascular Cerebral (AVC). Foram utilizadas quatro bases de dados: Scopus, Science Direct, PEPSIC e SCIELO. Ao final do processo de seleção, 40 artigos foram selecionados e analisados a partir de seus métodos e principais resultados. Percebeu-se que o AVC traz repercussões psicológicas ligadas a adaptação, afetando a Qualidade de Vida (QV), o que facilita o desencadeamento de transtornos psicológicos, principalmente nos seis primeiros meses da doença. É possível notar também que o primeiro semestre da doença é considerado o período mais crítico com relação ao aparecimento dos sintomas ansiosos e rebaixamento no nível de QV. Finalmente, foi possível perceber que recuperação da funcionalidade, assim como o uso de estratégias de enfrentamento funcionais, auxiliar na promoção da QV em pacientes que sofreram um AVC.
Palavras-chave: acidente vascular cerebral, adaptação, revisão de literatura
]]> ABSTRACT
This study performed an integrative literature review about the main psychological repercussions related to the adaptation of the victim after a Stroke. Four databases were used: Scopus, Science Direct, PEPSIC and SCIELO. At the end of the selection process, 33 articles were selected and analyzed based on their methods and main results. It was observed that stroke has psychological repercussions related to adaptation, affecting Quality of Life (QoL). This facilitates the triggering of psychological disorders, especially in the first six months of the disease. It is also possible to note that the first half of the disease is considered the most critical period in relation to the appearance of anxious symptoms and lowering in the level of QoL. On the other hand, after the sixth month is the appearance of depressive symptoms. Finally, it was noted that facing a stroke, victims are compelled to activate adaptive resources that may aid in the adjustment to the disease.
Keywords: stroke, adaptation, literature review
Repercussões psicológicas após um avc
Apontado como um problema de saúde pública mundial, o Acidente Vascular Cerebral (AVC) é causa de 27% das internações em todo o mundo (Steiner et al., 2014) e a terceira causa de morte mundial (World Health Organization [WHO], 2014). No entanto, o montante de pessoas com sequelas após o AVC é maior que o número de mortes, pois a principal característica da doença são as limitações físicas e cognitivas que atingem até 80% das vítimas. Por vezes, isso torna a vítima altamente dependente de cuidadores, até mesmo para atividades corriqueiras como comer e tomar banho (Brasil, 2013).
Pode-se caracterizar o AVC como uma deficiência neurológica que ocorre em virtude de uma lesão aguda ocorrida na área vascular do sistema nervoso central, incluindo infarto cerebral, hemorragia intracerebral e hemorragia subaracnóide (Sacco et al., 2013). As alterações físicas do AVC repercutem no âmbito social e financeiro ocasionando limitações, tais como a impossibilidade de exercer atividade remunerada e aumento de gastos decorrentes da doença (Araujo, Silva, Santana, Conceição, & Vasconcelos, 2011). Todos esses fatores contribuem para que ele seja considerado um severo evento estressor para a vítima e seus cuidadores (Hilari, Northcott, Roy, & Marshal, 2010), o que tem um impacto direto sobre alguns componentes psicológicos, a exemplo do rebaixamento da qualidade de vida das vítimas (Castellanos-Pinedo et al., 2011).
As modificações na vida da vítima pós-AVC contam com um elevado número de publicações acerca das repercussões que o AVC causa, a exemplo dos trabalhos de Oliveira e Silveira (2012); Tsutsumi, Kayaba e Ishikawa (2011) e White et al. (2012) que discutem algumas sequelas físicas e/ou psicológicas decorrentes do AVC. Porém, de modo geral, esses estudos priorizaram a análise de facetas específicas do pós-AVC (a exemplo da análise do estresse, proposto por Huang (2016) ou até mesmo fatores associados às limitações impostas pela condição (ver Liu et al., 2015; Matsuzaki et al., 2015). Por outro lado, não se encontrou um estudo que tenha como proposta a realização de uma síntese das modificações psicossociais decorrentes do AVC, que é o que constitui a principal proposta neste estudo.
É relevante destacar que estudos de revisão são essenciais pela síntese que fazem a respeito de um determinado tema e por permitir avaliar o que vem sendo estudado na área, trazendo novas possibilidades de estudos (Pais-Ribeiro, 2014). Além disso, estudos desse tipo permitem incorporar um espectro maior de resultados relevantes, ao invés de limitar as conclusões ao estudo de alguns artigos (Sampaio & Mancini, 2007). Diante disso, julgou-se pertinente tentar reunir as principais repercussões psicológicas em um único trabalho, visto que tal ato pode vir a favorecer a uma maior compreensão do processo de ajustamento diante de um quadro de AVC, bem como o papel do psicólogo no acompanhamento desses indivíduos. Adicionalmente, tal contribuição também pode auxiliar na elaboração de estratégias de prevenção ou mesmo tratamento de transtornos psicológicos no processo de enfrentamento após a ocorrência de um AVC.
Este estudo objetivou realizar uma revisão integrativa literatura sobre as repercussões psicológicas associadas à adaptação de vítimas do AVC, descritas na literatura entre os anos de 2005 a 2018. Para tanto, organizaram-se os achados sob dois tópicos distintos: a) análise metodológica, que compreendeu identificar local de estudo, método e sujeitos das pesquisas selecionadas, e b) principais resultados dos estudos selecionados, visando à compreensão das principais consequências psicológicas decorrentes das limitações pós-AVC.
]]> MétodoA coleta de dados foi feita em Dezembro de 2018, utilizando como base a seguinte pergunta norteadora: Quais as principais repercussões psicológicas relacionadas à adaptação ao AVC?. No campo assunto das bases de dados utilizados foram inseridas as seguintes palavras-chave: psicológicos AND Acidente Vascular Cerebral e seus respectivos descritores em inglês, limitando-se a artigos que contivessem esses termos nos títulos. Antes da escolha dessas palavras-chave, realizou-se uma busca preliminar utilizando outros descritores, a saber: coping, adaptação, saúde mental e reabilitação, sempre usando o conectivo and. Porém, os resultados encontrados não diferiram dos apresentados na revisão ora apresentada.
Adotaram-se os seguintes critérios de inclusão: apenas artigos que englobassem ao menos um aspecto psicológico relacionado do AVC (por exemplo, depressão, qualidade de vida, entre outros) e pesquisas em português, inglês ou espanhol indexadas à Scientific Electronic Library Online (SCIELO), Elsevier's Scopus (Scopus), Science Direct e ao Portal de Periódicos Eletrônicos de Psicologia (PEPSIC). Os critérios de exclusão foram: estudos nas áreas de neurociência, genética, farmacologia, toxicologia e engenharia, os trabalhos repetidos entre as bases de dados, bem como aqueles que não abordaram o enfoque proposto nesta revisão.
A busca inicial apresentou um total de 118 artigos, dispostos da seguinte forma: 74 artigos no Scopus (62,7%), 39 no Science Direct (33,0%), 4 artigos no SCIELO (3,3%) e 1 no PEPSIC (0,8%). Após a leitura minuciosa dos títulos e dos resumos foram excluídos 76 artigos pelos seguintes motivos: serem repetidos (n = 25), focarem em aspectos médico-farmacológico (n = 12), não focarem no AVC, focarem nos cuidadores e/ou analisarem unicamente o tratamento psicoterápico e outras formas de terapia (n = 39). Chegou-se, então, aos 40 artigos que compuseram esta revisão.
Os artigos foram apresentados e discutidos através de dois tópicos distintos: tópicos metodológicos e análise descritiva dos principais resultados. O primeiro tópico foi composto pela análise de dados metodológicos e sociodemográficos (idioma de publicação do estudo, país de publicação, perfil da amostra e abordagem metodológica utilizado). O segundo tópico de análise, que foi voltado aos principais resultados, foi classificado em três categorias com base na proximidade de assunto e objetivos abordados em cada um deles: a) Impacto do AVC sobre a Qualidade de vida (25%; n = 10), b) Ocorrência de ansiedade e depressão pós-AVC (50%; n = 20), e c) Estresse e adaptação ao AVC (25%; n = 10). Cada artigo (unidade de análise) foi incluído unicamente em uma dessas categorias.
Resultados
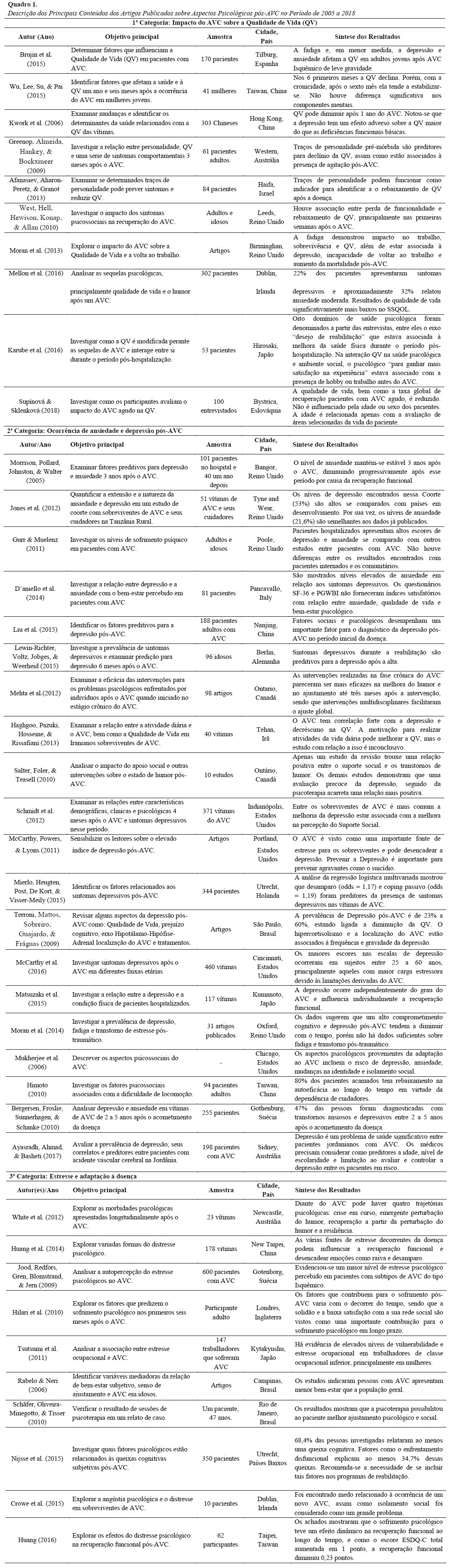
A síntese das informações em relação a objetivos, amostra, local da pesquisa e síntese dos resultados está apresentada no Quadro 1.

(clique para ampliar ! click to enlarge)
]]> Principais aspectos metodológicos
Com base nos artigos selecionados, percebeu-se que o número de publicações em português acerca da temática foi reduzido, dado que 92,5% (n = 37) dos artigos estavam escritos em inglês e apenas 7,5% (n = 3) escritos em Português. Notou-se ainda que as pesquisas selecionadas foram realizadas em diferentes países, com destaque para: China com 15% (n = 6), Japão também com 12,5% (n = 5), Reino Unido com 15% (n = 6), Estados Unidos e Canadá 15,7% (n = 6) cada e Brasil, Alemanha e Holanda, com 7,8% dos artigos por localidade (n = 3 por país).
Outro indicador utilizado para esta pesquisa diz respeito à metodologia adotada pelos autores na composição dos estudos. Observou-se que 30 publicações (75%) utilizaram a metodologia quantitativa, com destaque para as pesquisas longitudinais (36,8%), sendo que as do tipo Coorte foram as mais utilizadas pelos pesquisadores (21%, n = 8). A aplicação de escalas, principalmente as relativas aos transtornos de ansiedade e depressão, foi o instrumental escolhido por grande parte dos pesquisadores, principalmente aqueles cujo objetivo foi verificar a incidência de transtornos psicológicos (a exemplo de D'aniello et al., 2014; Gurr & Muellenz, 2011; Matsuzaki et al., 2015). Constatou-se, ainda, que poucos estudos tiv+eram abordagem qualitativa (n = 2).
É importante ressaltar o número de estudos selecionados que utilizaram a revisão de literatura (n= 7). Destes, quatro investigaram a depressão após AVC sobre as diferentes perspectivas: Terroni et al. (2009) e Moran et al. (2013) dissertaram acerca das consequências psicológicas da depressão pós-AVC, McCarthy, Powers, & Lyons (2011) reuniram dados sobre o retorno ao trabalho de pessoas com sintomas depressivos e, finalmente, o estudo de Salter et al. (2010) analisou o papel do suporte social em pessoas com depressão decorrente do AVC. As outras três revisões tiveram como foco o ajustamento, porém cada uma delas enfatizou um fator específico: Rabelo e Neri (2006) evidenciaram o bem-estar subjetivo, Moran et al. (2014) o rebaixamento da Qualidade de Vida e Mehta et al. (2012) avaliaram práticas que visam melhorar o ajustamento das vítimas de AVC, a exemplo da psicoterapia.
Principais resultados
Ocorrência de ansiedade e depressão pós-AVC (50,0%; 20 artigos)
Acerca da incidência de transtornos mentais comuns, tais como ansiedade e depressão, a pesquisa de Bergersen et al. (2010) sugeriu que cerca de 50% dos pacientes que sofreram AVC desenvolvem algum tipo de distúrbio psicológico. Doze dos 20 artigos selecionados abordaram a ocorrência de depressão após o AVC. Sete artigos buscaram analisar quais aspectos podem atuar de forma positiva na prevenção da depressão pós-AVC, sendo que esses fatores foram: estratégias de enfrentamento com foco no problema, tais como a busca por informação (Haghgoo et al, 2013; Mehta et al., 2012), obtenção de um suporte social positivo (Salter et al., 2010; Schmidt et al., 2012) e o acompanhamento psicológico (Laurie & Lyons, 2010; Lewin-Richter et al., 2015; Terroni et al., 2009). Por sua vez, quatro dos 19 artigos selecionados focaram especificamente na ansiedade como o objeto de estudo.
Impacto do AVC sobre a Qualidade de Vida (25,0%; 10 artigos)
Esta classe buscou investigar de que modo a faceta psicológica da Qualidade de Vida (QV) é modificada após o AVC. Este fator foi mostrado em 9 artigos, compondo 25,0% do total de artigos. A maioria deles buscou comprovar que há um rebaixamento da QV após um AVC. Ressalta-se aqui o artigo de Afasisev et al. (2013), que buscou, para além do rebaixamento da QV, analisar os aspectos da personalidade que podem contribuir para a modificação da percepção acerca da QV após o AVC. Em contraposição ao já falado acima, o artigo de Wu et al. (2015) analisou uma coorte a respeito do restabelecimento da QV em sujeitos com AVC, após a cronicidade das repercussões do quadro clínico.
Estresse e adaptação à doença (25,0%; 10 artigos)
]]> Esta classe buscou reforçar a visão de que o AVC se constitui como um evento estressor em virtude não só das limitações físicas e cognitivas, mas também devido ao prologado período de recuperação que caracteriza tal condição. Dentre as principais limitações derivadas do AVC, destacou-se a afasia, que na pesquisa realizada por Hilari et al. (2010), foi vista como um importante preditor para o distresse (82% da amostra de adultos possuíam um alto índice de distresse 6 meses após o evento).Os estudos mostraram que, independentemente do tipo diagnosticado (Isquêmico ou Hemorrágico), o AVC, por si só, pode ser considerado um evento adverso. Todavia, a pesquisa de Jood et al. (2009) sugere que há um maior grau de estresse psicológico em pessoas com AVC do tipo Isquêmico, pois as limitações físicas são maiores nesse subtipo, a exemplo de afasia, paresia e agrafia. White et al. (2012) também ressaltaram que, em um primeiro momento, o AVC ocasiona uma crise marcada pelas constantes mudanças de humor devido à insegurança quanto ao futuro e da possibilidade de não reversão das sequelas. Tal quadro pode ser modificado a partir da recuperação funcional e da capacidade de resiliência da vítima. Os autores ainda destacam que a alteração do humor é uma das possíveis causas de transtornos como a depressão, mas que isso pode ser atenuado por meio da mobilização de estratégias de enfrentamento funcionais.
Discussão
Nesta investigação se conduziu a revisão de literatura dos principais aspectos psicológicos do AVC. A partir de pesquisas publicadas entre os anos de 2005 e 2018, realizou-se a análise de aspectos metodológicos e dos principais resultados de 33 publicações selecionadas para esta revisão. Para fins didáticos, a seção discussão será subdividida em dois eixos, assim como feito na seção de resultados.
Aspectos Metodológicos
Os aspectos metodológicos analisados se referiram ao idioma, local da pesquisa e a abordagem metodológica dos artigos analisados. Quanto ao idioma, a constatação de mais trabalhos em língua inglesa parece se sustentar na tendência à internacionalização da ciência, o que justificaria a escrita predominante nesse idioma, mesmo que os dados não tenham sido coletados em países que tenham o Inglês como língua oficial, a exemplo dos trabalhos realizados na China (Himoto, 2010; Huang et al., 2014) ou Alemanha (Ayasrah, Hamad, & Basheti, 2017; White et al., 2012). Mesmo assim, a localidade dos estudos vem corroborar a carência de estudos em países de língua portuguesa, um dado destoante tendo em vista o alto grau de incidência e mortalidade por AVC, sobretudo no Brasil (Brasil, 2013).
Os estudos aqui avaliados trouxeram, em sua maioria, sujeitos adultos, contrapondo os dados estatísticos que comprovam que o AVC acomete mais idosos (Brasil, 2013). Talvez isso tenha ocorrido porque a chance de sobrevivência na terceira idade são menores do que em outras faixas etárias (Rolim & Martins, 2011). Além disso, as limitações da doença tornam a adaptação mais difícil em pessoas na idade produtiva, o que favorece a identificação de repercussões psicológicas e/ou sociais, a exemplo do impacto sobre a qualidade de vida (Brujin et al., 2015), e aumentam a incidência de transtornos mentais comuns, tais como depressão e ansiedade (Himoto, 2010; Levin, & Moran et al., 2014; McCarthy et al., 2016).
Os métodos longitudinais utilizados pela maioria das pesquisas possibilitou a compreensão das repercussões do AVC tanto no período agudo da doença quanto no crônico da doença. Assim, foi possível observar a incidência de transtornos psicológicos à medida que a doença adquira um caráter crônico. Por outro lado, os poucos os dados qualitativos não foram suficientes para que as vivências de pessoas com AVC pudessem ser conhecidas a fundo. Enfim, considerando que as pesquisas qualitativas possibilitam conhecer as particularidades ao conviver com o AVC, salienta-se a importância de mais estudos com este delineamento metodológico.
Principais Resultados
A primeira das três categorias criadas no estudo tratou da ocorrência de ansiedade e depressão em pessoas com AVC. Nesse sentido, Matsuzaki et al. (2015) apontou que a depressão pode atingir cerca de 25% das vítimas de AVC em idade produtiva, podendo estar associada a falta de recuperação funcional das mesmas. Esses autores relataram que as limitações causadas pela doença tendem a afastar do trabalho as pessoas que sofreram AVC, ocasionando impacto financeiro e, com isso, podem facilitar o surgimento de um quadro clinico de depressão. Consistente com essa expectativa, o estudo de coorte realizado por Lewin-Richter et al. (2015) apontou que, após 6 meses, 44% das pessoas estudadas (96 ao todo) foram diagnosticadas com depressão.
]]> A respeito da ansiedade, as pesquisas de D'aniello et al. (2014) e Gurr e Mullenz (2011) abordaram os transtornos de ansiedade como um sofrimento recorrente entre as vítimas de AVC, estando atrelada, principalmente, à percepção do paciente acerca de seu estado de saúde, ou seja, a percepção da pessoa quanto às sequelas e limitações. Os autores notaram que os primeiros sintomas ansiosos são identificados nas primeiras duas semanas após o AVC, período de tempo na qual as pessoas começam a perceber que disfunções físicas existentes persistem. Esses sintomas permanecem estáveis em mais de 50% da amostra por até três anos após o acometimento da doença. Em termos de predição para a ansiedade, Morrison et al. (2005) obtiveram resultados significativos ao comparar sintomas ansiosos entre sexos, encontrando que os sintomas ansiosos foram mais comuns entre as mulheres em três anos após o AVC.Pode-se dizer, em suma, que a ansiedade e a depressão temática tendem a ter um impacto direto sobre a QV das pessoas que são acometidas pelo AVC. A dimensão psicológica da QV pode ser conceituada como a percepção individual que cada pessoa tem acerca de sua posição na vida, incluindo o contexto cultural em que ela está inserida, o sistema de valores na qual vive, além de seus interesses e expectativas pessoais (Urzúa, 2012). Com isso, pode-se dizer que, após um AVC, a QV da vítima sofre um rebaixamento significativo, pois tende a ocorrer limitações importantes derivadas do quadro clínico (Brujin et al., 2015) ou mesmo pelo alto índice de estresse psicológico, principalmente nos três primeiros meses após o acometimento pela doença (West et al., 2010). Logo, o estresse psicológico está associado não apenas às limitações que a pessoa tem, mas também à intensa atividade de reabilitação, estratégias de enfrentamento e a percepção que a pessoa tem de seu suporte social (Rabelo & Neri, 2006).
Considera-se que as estratégias de enfrentamento podem atuar de uma forma a diminuir o rebaixamento da QV de pessoas com AVC (Nijsse et al., 2015). De maneira semelhante, fatores internos como traços de personalidade podem ser vistos como fator impeditivo para o rebaixamento da QV, como por exemplo a extroversão. De modo contrário, traços como o neuroticismo (Greenop et al., 2009), dependência de recompensa, busca de novidades e esquiva de danos (Afanasisev, Aharon-Peretz, & Granot, 2013) pode atuar de forma negativa para a busca por uma mais saudável QV em pessoas que sofreram AVC, sobretudo na fase aguda da doença, aumentando a incidência de depressão e ansiedade nas vítimas (Moran et al., 2013), além da redução da interação social das vítimas (Kwork et al., 2006).
De modo complementar, a pesquisa de coorte realizada por Wu et al. (2015) debateu o reestabelecimento dos níveis de QV. Para eles, à medida que a doença adquire o estágio crônico, ou seja, após 6 meses, a funcionalidade da vítima é, em partes, reestabelecida. O retorno às atividades cotidianas pode ser visto como um fator que eleva os níveis bem-estar, o que, associado à presença de suporte social positivo, contribui para o aumento da QV. Por outro lado, foi possível perceber que, como consequência da redução da QV, há uma maior probabilidade de surgir ou agravar transtornos psicológicos, podendo também prolongar o afastamento de atividades laborais (Moran et al., 2013). É importante ressaltar que mesmo com a manutenção das sequelas limitantes, o acompanhamento psicológico durante a reabilitação da doença pode manter os escores de QV mais elevados do que aqueles que não tinham acompanhamento psicológico. Destaca-se, então, a importância do trabalho do psicólogo nas equipes de reabilitação do AVC, o que já fora apontado por Huang (2016) e Schãfer, Oliveira-Minegotto, & Tisser (2010).
A terceira e última categoria abordou o estresse e as estratégias utilizadas pelas pessoas para lidar com o período pós-AVC. Detectou-se que estratégias de enfrentamento eficazes podem diminuir a percepção do estresse e, assim, contribuir positivamente para a saúde mental. Percebeu- se que as pessoas que mais sofrem o impacto da doença e, consequentemente, do estresse, são aquelas compelidas a afastarem-se de suas atividades laborais em virtude dessas sequelas (Tsutsumi et al. 2011). Contudo, a carga estressora tende a diminuir ao passo que o indivíduo vai recuperando sua funcionalidade, mesmo que minimamente (Huang et al., 2014). Outro fator que tende a diminuir a carga estressora é a percepção benéfica do apoio de família, amigos, companheiro de trabalho, entre outros, o que caracteriza o suporte social positivo (Hilari et al., 2010).
Ao analisar o estresse em vítimas de AVC, Schãfer et. (2010) relataram que pessoas em atendimento psicoterápico, se comparado a pessoas sem esse tipo de suporte, relatam menor carga estressora. Isso possivelmente ocorre porque o psicólogo auxilia a vítima no desenvolvimento de estratégias de enfrentamento positivas e, assim, minimiza a probabilidade de possíveis transtornos decorrentes de um ajustamento psicológico insuficiente para lidar com os desafios adaptativos impostos pela situação clínica (Schãfer et al. 2010). Destacou-se aqui a ativação de estratégias de enfrentamento como um recurso que pode ser positivo, caso as estratégias utilizadas sirvam como atenuante ao estresse. Porém, se essas estratégias empreendidas forem vistas como disfuncionais, a exemplo, o Suporte Social com caráter negativo (Rabelo & Neri, 2006), pode haver o aumento da crise que surge após o acometimento da doença e elevar a possibilidade de transtornos psicológicos ao longo do tempo.
Em resumo, notou-se que as limitações cognitivas, físicas e sociais advindas do AVC atuam como estressores, levando o indivíduo a ativar estratégias cognitivas e comportamentais para minimizar seus efeitos. Lazarus e Folkman (1984) relatam que se as estratégias de enfrentamento forem positivas, o estresse advindo pela mudança de vida trazida pela doença é reduzido. Por outro lado, quando os recursos ativados forem considerados como mal adaptativos, eleva-se a chance de ocorrência de transtornos mentais, tais como os transtornos de ansiedade e depressão. Tal explicação sobre enfrentamento assinalado acima se mostrou como plausível e funciona também no processo de ajustamento pós-AVC.
Existem limitações neste estudo que merecem ser destacadas. Primeiramente, não foi possível fazer comparações em questões importantes a respeito da adaptação ao AVC, por exemplo, quanto às diferenças da repercussão por sexo (Morrison et al., 2005) ou status socioeconômico da vítima e de sua família (Rabelo & Neri, 2006). Tais análise seriam importantes pois poderiam evidenciar diferenças na relação entre essas especificidades. Além disso, não se fez a análise da repercussão psicológica na vida dos cuidadores e familiares mais próximos, uma vez que já se sabe que o impacto tende a ser severo e causar notável mobilização da dinâmica familiar (Lutz, Young, Cox, Martz, & Creasy, 2011; Ostwald, Bernal, Cron, & Godwin, 2015), o que também afeta, por sua vez, a própria vítima do AVC. Ademais, espera-se que futuras pesquisas se voltem às repercussões psicológicas pós-AVC priorizem a análise qualitativa dos achados e temáticas como o Suporte Social e autoestima, visto que foram aspectos considerados escassos na literatura então avaliada.
Finalmente, espera-se com este trabalho contribuir com profissionais da área da saúde, de modo que possam entender a vítima de AVC com mais completude e prestar assistência cada vez mais integral ao paciente. Além disso, crê-se que ao compreender os processos psicológicos decorrentes do ajustamento ao AVC, torna-se possível traçar diretrizes para melhorar a QV e minimizar a ocorrência de transtornos psicológicos nesse público.
]]> REFERÊNCIAS
Afanasiev, S., Aharon-Peretz, J., & Granot, M. (2013). Personality type as a predictor for depressive symptoms and reduction in quality of life among stroke survivals. The American Journal of Geriatric Psychiatry, 21(9), 832-839. doi: 10.1016/j.jagp.2013.04.012. [ Links ]
Araujo, J. S., Silva, S. E. D. da., Santana, M. E. de., Conceição, V. M. da., & Vasconcelos, E. V. (2011). O processo do cuidar/cuidado nas representações sociais de cuidadores de pacientes sequelados por acidente vascular cerebral. Enfermagem em Foco, 2(4), 235-238. [ Links ]
Ayasrah, S.M., Ahmad, M.M., & Basheti, I.A. (2017). Post-Stroke depression in Jordan: Prevalence Correlates and Predictors. Jornal of Stroke Cerebrovascular Diseases, 27(5), 1134-1142. doi: 10.1016/j.jstrokecerebrovasdis.2017.1. [ Links ]
Bergersen, H., Froslie, K.F., Sunneshagen, K.S., & Schonke, A. (2010). Anxiety, depression, and well-being 2 to 5 years post-stroke. Stroke, 19(5), 364-360. doi: 10.1016/j.jstrokecerebrovasdis.2009.06.005. [ Links ]
Brasil. Ministério da Saúde. (2013). Vigilância epidemiológica da doença cerebrovascular. Brasília, DF: Goulart.
]]>Brujin, M., Synhaeve, N.E., Rijsbergen, M.W., Leew, F.E., Mark, R.E., Jansen, B.P., & Kort, P.L. (2015). Quality of life after young isquemic stroke of mild severity is mainly influencied by psychological factors. Journal of Stroke and Cerebrovascular Diseases, 24(10), 2183-2188. doi: 10.1016/j.jstrokecerebrovasdis.2015.04.040. [ Links ]
Castellanos-Pinedo, F., Hernández-Perez, J.M., Zurdo, M., Rodríguez-Fúnez, B., Hernández-Bayo, J.M., Gárcia-Fernández, C., ... & Castro-Posada, J.A. (2011). Influence of premorbid psychopatology and lesion location on affective and behavioral disorders after Isquemic stroke. Journal Neuropsychiatry Clinic Neuroscience, 23(3), 340-347. doi: 10.1176/jnp.23.3.jnp340. [ Links ]
Crowe, C., Coen, R., Kidd, N., Hevey, D., Cooney, J., & Harbison, J. (2015). A qualitative study of the experience of psychological distress post-stroke. Journal of Health Psychology, 21(11), 1-8. doi: 10.1177/1359105315581067. [ Links ]
D'aniello, G., Scarpina, F., Mauro, A., Mori, J., Castelnuovo, G., Bigoni, M., ... & Molinari, E. (2014). Characteristics of anxiety and psychological well-being in chronic post stroke patients. Journal of Neurological Sciences, 338, 191-196. doi: 10.1016/jns2017.01.005. [ Links ]
Greenop, K., Almeida, O., Hankey, G., & Bockxmeer, F. (2009). Premorbid personality traits are associated with post-stroke behavioral and psychological symptons: A 3-month follow-up study in Perth, Western, Australia. International Psychogeriatrics, 21(6), 1068-1071. doi: 10.1017/S104161020999457. [ Links ]
]]>Gurr, B., & Mielenz, C. (2011). A follow-up study of psychological problems after stroke. Top Stroke Rehabilitation, 18(5), 461-169. doi: 101310/tsr180s.461. [ Links ]
Haghgoo, H.A., Pazuki, E.S., Hosseine, A.S., & Rissafiani, M. (2013). Depression, activities of daily living and quality of life in patients with Stroke. Journal Neurological Sciences, 328, 87- 91. doi: 10.1016/j.jns.2013.02.027. [ Links ]
Hilari, K., Northcott, R., Coy, P., Marshall, J., Wiggins, R., Chataway, J., & Ames, D. (2010). Psychological distress after stroke and aphasia: The first six months. Clinical Rehabilitation, 24, 181-190. doi: 10.1177/0269215509346090. [ Links ]
Himoto, Y. (2010). An examination of the physical, psychological and social factors associated with post stroke people arrested at home in a community. Journal of Physical Therapy. Science, 14, 239-245. [ Links ]
Huang, H., Huang, L., Hu, C., Chang, C., Lee, H., Chi, N. Chang, H. (2014). The mediating effect of psychological distress on functional dependence in Stroke patients. Journal of Clinical Nursing, 23, 3533-3543. doi: 10.1111/jocn.12606. [ Links ]
]]>Huang, H.C. (2016). Time-varying effects of psychological distress on the functional recovery of stroke patients. Archives of Physical Medicine and Rehabilitation, 3(16), 31145-31150. doi: 10.1016/j.apmr.2016.09.120. [ Links ]
Jones, M., Howitt, S., Jusabani, A., Gray, W., Mugusi, F., Swai, M., & Walker, R. (2012). Anxiety and depression in incident survivors and their caregivers in Rural Tanzania: A case control follow-up over five years. Neurology, Psychiatry, and Brain Research, 18, I22-I28. doi: 10.1016/j.npbr.2012.01.003.
Jood, K., Redfors, P., Rosengren, A., Blomstrand, C., & Jurn, C. (2009). Self-perceived psychological stress and ischemic Stroke: A case control study. Biomed Central, 7(53), 1741- 1751.doi:10.1186/1741-7015-7-53. [ Links ]
Karube. N., Sasaki, A., Hondoh, F., Odagiri, C., Hagii, J., Seino, S., ... & Osanai, T. (2016). Quality of life in physical and psychological health and social environment at post-hospitalization period in patients with stroke. Journal of Stroke Cerebrovascular Disease, 25(10), 2482-2487. doi: 10.1016/j.jstrokecerebrovasdis.2016.06.022. [ Links ]
Kwork, T., Lo, R., Wong, E., Wai-Kwong, T., Mok, V., & Kai-Sing, W. (2006). Quality of life of stroke suvivors: A 1-year follow-up study. Archives of Physical Medical Rehabilitation, 87, 1177-1182. doi: 10.1016/j.apnr.2006.05.015. [ Links ]
Lazarus, R., & Folkman, S. (1984). Stress, Appaisal and Coping (1ª Ed.). New York: Springer Publisher company. [ Links ]
Lewin-Richter, A., Voltz, M., Jobges, M., & Werheid, K. (2015). Predictivity of early depressive symptoms for post-stroke depression. Journal of Nursing Health Aging, 19(7), 754-758. [ Links ]
Liu, R., Yue, Y., Jiang, J., Lu, Y., Yuan, G., & Wang, Q. (2015). A risk prediction model of PSD in stroke survivors. European Psychiatry, 30(1), 28-31. doi: 10.1016/S0924-9338(15)30562-9. [ Links ]
Lutz, B. J., Young, M. E., Cox, K. J., Martz, C., & Creasy, K. R. (2011). The crisis of stroke: Experiences of patients and their family caregivers. Topics in Stroke Rehabilitation, 18(6), 786- 97. doi:10.1310/tsr1806-786. [ Links ]
Matsuzaki, S., Hashimoto, M., Yuki, S., Koyama, A., Hirata, Y. & Ikeda, M. (2015). The relationship between post-stroke depression and physical recovery. Journal of Affective Disorders, 176, 56-60. doi: 10.1016/j.jad.2015.01.020. [ Links ]
McCarthy, M., Sucharew, H., Alwell, K., Moomaw, C., Woo, D., Flaherty, M Kissela, B. (2016). Age, subjective stress, and depression after ischemic stroke. Journal Behavioral Medical, 39, 55- 64. doi: 10.1007/s10865-015-9663-0. [ Links ]
McCarthy, M.J.M., Powers, L.E., & Lyons, K.S. (2011). Depression post-Stroke: Worker's role in addressing an under recognized psychological problem for couples who have experienced Stroke. Health and Social Work, 36(2), 139-147. [ Links ]
Mehta, S., Pereira, S., Janzen, S., McIntyre, A., McClure, A., & Teasel, R. (2012). Effectiveness of psychological interventions in chronic stage of stroke: A systematic Review. Top Stroke Rehabilitation, 19(6), 536-544. doi: 10.1310/tsr1906-536. [ Links ]
Mellon, L., Willians, D., Brewer, P., Hall, P., Horgan, F., Dolan, E. Hickey, A. (2016). Psychological symptoms and quality of life post-stroke. A profile of Irish stroke survivors from the ASPIRE-S cohort. Journal of Psychosomatic Research, 85, 74-84. doi: 10.1016/j.jpsychores.2016.03.182. [ Links ]
Mierlo, M. L., Heugten, C. M., Post, M. W., De Kort, P. L., & Visser-Meily, J. M. (2015). Psychological factors determine depressive symptomatology after stroke. Archives of Physical Medicine and Rehabilitation, 96(6), 1064-1070. doi: 10.1016/j.apmr.2015.01.022. [ Links ]
Moran, G., Fletcher, B., Feltham, M., Calvert, M., Sackley, C., & Marshal, T. (2014). Fatigue psychological and cognitive impairment following transient ischaemic attack and minor stroke: A sistematic review. European Journal Neurologic, 21(10), 1258-1267. doi: 10.1111/ene.12469. [ Links ]
Moran, G., Fletcher, B., Calvert, M., Feltham, M., Sackley, C., & Marshal, T. (2013). A systematic review investigating fatigue, psychological and cognitive impairment following TIA and minor stroke: Protocol paper. Journal Systematic Reviews, 2(72), 2-7. doi: 10.1186/2046-4053-2-72 [ Links ]
Morrison, V., Pollard, B., Johnston, M., & Walter, R. (2005). Anxiety and depression 3 years following Stroke: Demographic, clinical and psychological predictors. Journal of Psychosomatic Research, 59, 209-213. doi: 10.1016/j.jpsychores.2005.02.019. [ Links ]
Mukherjee, D., Levin, R., & Heller, W. (2006). The cognitive, emotional, and social sequelae of stroke: Psychological and ethical concerns in post-stroke adaptation. Stroke, 13(4), 26-35. doi: 10.1310/tsr1304-26. [ Links ]
Nijsse, B., van Heughten, V., van Mierlo, M., Post, M., de Kort, P., & Visser-Meily, J. (2015). Psychological factors are associated with subjective cognitive complaints 2 months post-stroke. Neuropsychological Rehabilitation: An international Journal, 27(1), 99-115. doi: 10.1080/09602011.2015.1065280. [ Links ]
Ostwald, S. K., Bernal, M. P., Cron, S. G., & Godwin, K. M. (2015). Stress experienced by stroke survivors and spousal caregivers during the first year after discharge from inpatient rehabilitation. Topics in Stroke Rehabilitation, 16(2), 93-104. doi: 10.1310/tsr1602-93. [ Links ]
]]>Pais-Ribeiro, J.L. (2014). Revisão de investigação e evidência científica. Psicologia Saúde & Doenças, 15(3), 631-682. doi: 10.15309/14psd150309. [ Links ]
Rabelo, D.F., & Néri, A.L. (2006). Bem-estar subjetivo e senso de ajustamento psicológico em idosos que sofreram AVC: Uma revisão. Estudos de Psicologia, 11(3), 169-177. [ Links ]
Rolim, C., & Martins, M. (2011). Qualidade do cuidado ao acidente vascular cerebral isquêmico no SUS. Caderno de Saúde Pública, 27(11), 2106-2116. [ Links ]
Sacco, R. L., Kasner, S. E., Broderick, J. P., Caplan, L. R., Connors, J. J., Culebras, A., & Vinters, H. V. (2013). An updated definition of stroke for the 21st century: A statement for healthcare professionals from the American heart association/American stroke association. Stroke, 44(7), 2064-2089. doi: 10.1161/STR.0b013e318296aeca. [ Links ]
Salter, K., Foley, N., & Teasell, R. (2010). Social support interventions a mood status post-Stroke: A review. International Journal of Nursing Studies, 47, 616-625. doi: 10.1016/j.ijnurstu.2009.12.002. [ Links ]
]]>Sampaio, R.F., & Mancini, M.C. (2007). Estudos de revisão sistemática: Um guia para síntese criteriosa da evidência científica. Revista Brasileira de Fisioterapia, 11(1), 83-89. [ Links ]
Schãfer, P.S., Oliveira-Minegotto, L., & Tisser. L. (2010). AVC: As repercussões psíquicas a partir de um relato de caso. Ciência e Cognição, 15(2), 202-215. [ Links ]
Schmidt, A., Damush, T., Tu, W., Bakas, T., Kroenke, K., Hendrie, H., & Williams, L. (2012). Depression Improvement is related to social role functioning after Stroke. Archives of Physical Medical Rehabilitation, 93, 978-982. [ Links ]
Supínová, M., & Sklenková, G. (2018). The Quality of Life of patients after an acute Stroke. Kontakt, 20(2), 153-159. doi:10.1016/j.kontakt.2018.02.001. [ Links ]
Steiner, T., Al-Sashi, R., Beer, R., Christensen, H., Cordonnier, C., Csiba, L. Wagner, M. (2014). Europe Stroke Organization (ESO): Guidelines for the management of Spontaneous Intracerebral Hemorrhage. Internacional. Journal Stroke, 9(7),840-855. doi: 10.1111/ijs.12309. [ Links ]
]]>Terroni, L., Mattos, P., Sobreiro, M., Guajardo, V., & Fráguas, R. (2009). Depressão pós-AVC: Aspectos psicológicos, neurológicos, eixo HHA, correlato neuro-anatômico e tratamento. Revista de Psiquiatria Clínica, 36(3), 100-108. [ Links ]
Tsutsumi, A., Kayoba, K., & Ishukawa, S. (2011). Impact occupational stress on stroke across occupational classes and genders. Societal, Science, and Medicine, 72, 1652-1658. doi: 10.1016/j.socscimed.2011.03.026 . [ Links ]
Urzúa, A. (2012). Calidad de vida: Una revisión teórica del concepto. Terapia Psicológica, 30(1), 718-4808. doi: 10.4067/S0718-48082012000100006. [ Links ]
West, R., Hell, K., Hewisson, J., Knapp, P., & House, A. (2010). Psychological disorders after stroke are an important influence on functional outcomes. Stroke, 41, 1723-1727. doi: 10.11611/strokeaha.110.583351. [ Links ]
White, J., Magin, P., Attia, J., Sturm, J., Carter, G., & Pollack, M. (2012). Trajectories of psychological distress after stroke. Annals of Family Medicine, 10(5), 435-442. doi: 10.1370/afm.1374. [ Links ]
]]>World Health Organization. (2014). World health statistics 2014. Geneva: Word Health Organization [ Links ]
Wu, M., Lee, S., Su, H., & Pai, H. (2015). The effect of cognitive appraisal in middle-aged women stroke survivors and psychological health of their caregivers: A follow-up study. Journal of Clinical Nursing, 24, 3155-3164. doi: 10.1111/jocn.12926. [ Links ]
Recebido em 07 de Fevereiro de 2017/ Aceite em 04 de Setembro de 2018
]]>