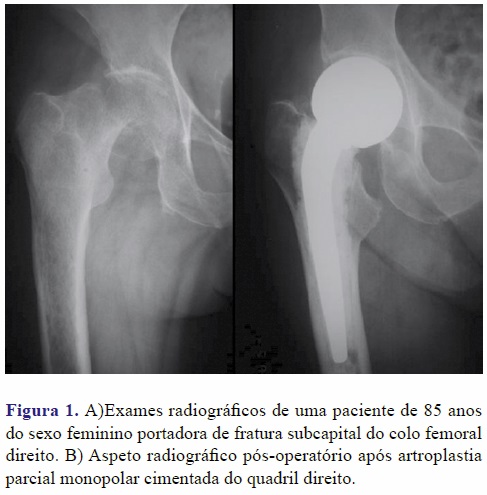
Resultado funcional após hemiartroplastia de quadril para tratamento de fraturas do colo femoral
Ademir SchuroffI; Mark DeekeI; Marco PedroniI; Josieano ValérioI; Fernando MielkeI; Renato LocksI
I. Serviço de Ortopedia e Traumatologia. Grupo do Quadril. Hospital Universitário Cajuru da Pontifícia Universidade Católica do Paraná. Curitiba . Brasil.
RESUMO
]]> Objetivo: Avaliação clínico-funcional e mortalidade de pacientes idosos com fraturas mediais instáveis do colo femoral submetidos à hemiartroplastia do quadril. Métodos: Foram avaliados prospectivamente 93 pacientes com seguimento mínimo de quatro meses, entre agosto de 2006 a maio de 2009, submetidos à artroplastia parcial de quadril cimentada após fratura instável do colo femoral. Analisaram-se status deambulatório, mortalidade pós-operatória, tempo decorrido entre a fratura e o tratamento cirúrgico, função cognitiva (Short Portable Mental Status Questionnaire-SPMSQ), além do nível de independência nas atividades da vida diária (método de Katz), nível de dor e impacto da fisioterapia na reabilitação desses pacientes.Palavras chave: Fraturas do colo femoral, artroplastia de quadril, mortalidade, morbidade, marcha.
ABSTRACT
Objetive: Clinical and functional avaliation and mortality of elderly patients with unstable fratures of the medial femoral neck underwent hemiarthroplasty of the hip.
Methods: We prospectively evaluated 93 patients followed at least four months between August 2006 and May 2009, submitted to partial cemented hemiarthroplasty of hip after unstable femoral neck frature. We analyzed ambulatory status, postoperative mortality, time between frature and surgery, cognitive function (Short Portable Mental Status Questionnaire-SPMSQ), beyond the level of independence in activities of daily living (Katz Method), level of pain and impact of physiotherapy on rehabilitation of these patients.
Results: Of the 93 patients evaluated, 20 died and 19 patients were lost to follow-up, leaving 54 patients to be evaluated. There was a mean age of 82.5 years with a predominance of females (79.63%). The follow-up was 21 months (4-37). The patients were operated on average at day 4 after frature. Before surgery, over 81% of patients could ambulate without assistance at home or in the community. After surgery, this percentage dropped to approximately 57% of patients. The mortality in the postoperative period was 21.50%. The rate of dislocation was 4.65%. Severe dementia was found in 22.2% of patients. Physical therapy was not significant for patients to bring the same level ambulatories before the frature.
Conclusion: Patients with frature of the femoral neck underwent partial hip prosthesis in our series show a loss of walking ability, a postoperative mortality around 20%, with a low rate of complications following short-term. We believe this to be a viable alternative treatment in elderly patients with poor walking ability and other uncontrolled medical comorbidity.
Key words: Hip neck fratures, hemiarthroplasty, mortality, morbidity, gait.
INTRODUÇÃO
A mortalidade após cirurgia por fratura do fêmur proximal em idosos é em torno de 26%, variando de 14-36%. Essa taxa de mortalidade é observada nos primeiros seis meses após o trauma, diminuindo progressivamente, até igualar-se a expectativa de vida da população da mesma faixa etária, somente depois de um ano[1].
Apesar do tratamento ideal para fraturas do colo do fêmur em idosos permanecer controverso, o número de casos vem crescendo, atualmente estimam-se 250 mil fraturas /ano nos EUA e há previsão de aumento de 100% até 2040.[2].
É consenso que pacientes idosos com fratura do colo femoral desviada, deambuladores domiciliares e com comorbidades que levem a uma pequena expectativa de vida são melhor tratados com hemiartroplastia, possibilitando deambulação precoce e menor risco de nova intervenção cirúrgica[3] além do controle da dor[4].
Pacientes com demência submetidos à artroplastia parcial do quadril após fratura do colo do fêmur apresentam uma taxa de mortalidade maior no primeiro ano[5] além de maior índice de perda da independência para atividades da vida diária e marcha[2,5].
Os índices de mortalidade no primeiro ano após hemiartroplastia variam na literatura de 17-28%[6]. Os principais preditores de mortalidade são sexo feminino, idade maior que 80 anos e déficit cognitivo[7].
Estudo prévio mostra que a recuperação da função deambulatória dos pacientes submetidos à hemiartroplastia do quadril ocorre apenas nos primeiros quatro meses pós-operatórios[8].
O objetivo deste trabalho é avaliar a função deambulatória, o impacto da fisioterapia e a mortalidade dos pacientes com fratura do colo do fêmur submetidos à hemiartroplastia (artroplastia parcial) do quadril.
]]> MÉTODOS
Foram avaliados prospectivamente através de protocolo específico para o estudo, 93 pacientes que sofreram fraturas mediais instáveis do colo femoral, submetidos à artroplastia parcial de quadril cimentada tratados pelo grupo do quadril do Hospital Universitário Cajuru, na cidade de Curitiba, entre agosto de 2006 e maio de 2009. Consideramos neste estudo as avaliações feitas em 54 pacientes que cumpriram os critérios de inclusão em nosso estudo. Houve a perda do seguimento ambulatorial presencial de dezenove pacientes, não encontrados mesmo após contato telefônico. Vinte pacientes falecidos também foram excluídos, totalizando 39 pacientes não avaliados devido a óbito e perda de seguimento.
Foram incluídos na amostra pacientes com fratura desviada do colo femoral e que apresentavam-se com idade biológica avançada, baixa expectativa de vida, deambuladores comunitários com comorbidades clínicas descompensadas, deambuladores restritos domiciliares e pacientes não deambuladores com acompanhamento mínimo de seis meses. Foram excluídos pacientes submetidos à artroplastia parcial por seqüelas de fraturas já operadas da extremidade proximal do fêmur. Dividimos os pacientes de acordo com sua capacidade de deambulação em 5 grupos: Deambuladores comunitários com ou sem auxílio de muleta, bengala, andador; deambuladores domiciliares com ou sem auxílio e não deambuladores
Todos os pacientes foram submetidos à artroplastia parcial do quadril tipo modular céfalo-femoral cimentada (Figura 1), por via de acesso posterior sob anestesia raquidiana. Receberam analgesia, profilaxia pós-operatória com antibiótico por 48 horas (cefazolina) e anticoagulante por 14 dias (heparinas de baixo peso molecular). A descarga do peso corpóreo foi estimulada no 1º dia pós-operatório através da equipe de fisioterapia com auxílio de um andador, de acordo com demanda e condições clínicas dos pacientes.

Foram avaliados no pré-operatório: status deambulatório, grau de independência para atividades da vida diária (método de Katz)[9], número de comorbidades, o tempo decorrido entre a fratura e o tratamento cirúrgico e a função cognitiva (Short Portable Mental Status Questionnaire)[10]. Após serem submetidos ao tratamento cirúrgico e receberem alta hospitalar, os pacientes passam a receber acompanhamento ambulatorial neste Serviço de Ortopedia - Ambulatório do Quadril. Na alta, todos eram encaminhados também para fisioterapia. Um protocolo era aplicado nas consultas com 3, 6, 12, 24 meses de seguimento pós-operatório. Os pacientes eram questionados (entrevistados) nas consultas e fazíamos as seguintes perguntas:
RESULTADOS
Foram avaliados 54 pacientes entre 64 e 101 anos (idade média de 82,5 anos). O tempo médio entre a fratura e a cirurgia foi de 4,89(variando de 1 a 30) dias e o tempo de seguimento médio foi de 21,18 meses (variando de 6 a 37 meses). Pacientes do sexo feminino são mais freqüentes neste estudo (79,63%). O lado predominante da fratura é o esquerdo, com 59,26%. A classificação de Garden mais freqüente é a do tipo IV (51,85%). De acordo com o escore de Katz de independência das atividades de vida diária, 51,85% dos pacientes se apresentavam em condição independente e 12,86% eram considerados totalmente dependentes. Em relação ao Mini Mental, o escore mais freqüente obtido no teste mini-mental pré-operatório foi o 7, com 18,52% dos casos. O índice médio Mini-mental foi de 5,65 (variando de 0 a 10) enquanto que o índice Katz médio foi de 1,59 (variando de 0 a 6).
Após o seguimento médio de 21 meses, 46 (86%) pacientes relataram não sentir dor. Dor leve foi relatada por 7 pacientes e um paciente relatou dor moderada.
Em relação à capacidade de deambulação pré e pós-operatória, encontramos os seguintes resultados descritos na tabela 1.
]]>
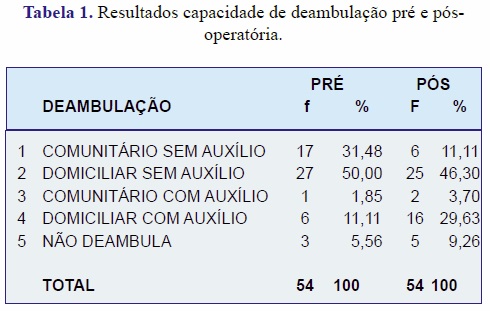
No pré-operatório, mais de 81% dos pacientes deambulavam sem auxílio no domicílio ou na comunidade. Após a cirurgia, este percentual caiu para aproximadamente 57% dos pacientes.
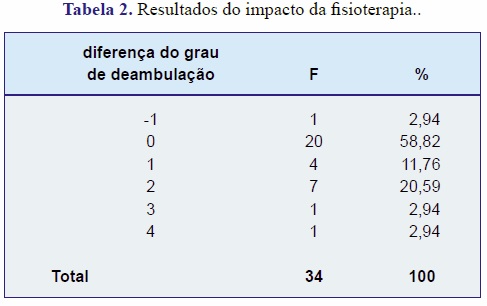
Pode-se notar que 58,82% dos pacientes continuou no mesmo grau de deambulação e apenas 1 paciente melhorou seu grau de deambulação. 13 pacientes pioraram (38,24%). Comparando os pacientes que fizeram fisioterapia com aqueles que não fizeram, obteve-se um p-valor=0,89, ou seja, não existe efeito significativo da fisioterapia.
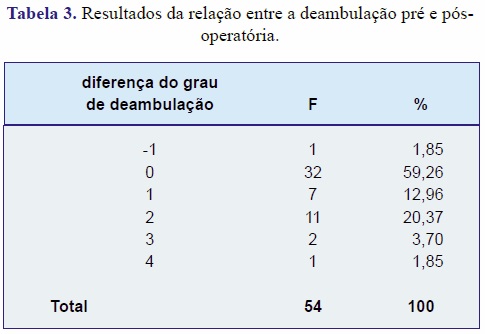
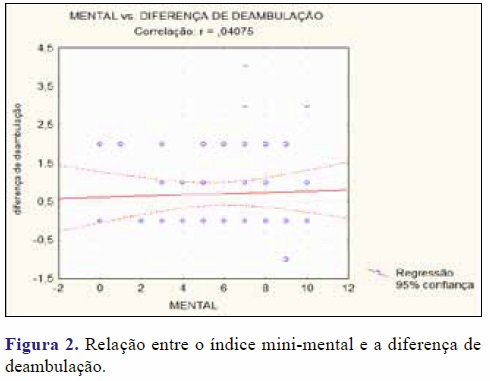
Na relação entre o índice Katz e o nível deambulatório pós-operatório, verificamos que aparentemente quanto maior o índice de Katz pior é o nível de deambulação no período pós-operatório. Aplicando o coeficiente de Spearman, obteve-se r = 0,285 (p=0,037), ou seja, existe associação significativa entre o índice de Katz e o nível de deambulação no pós-operatório. Portanto, aqueles pacientes mais dependentes no período pré-operatório terão piores resultados de deambulação após a cirurgia.

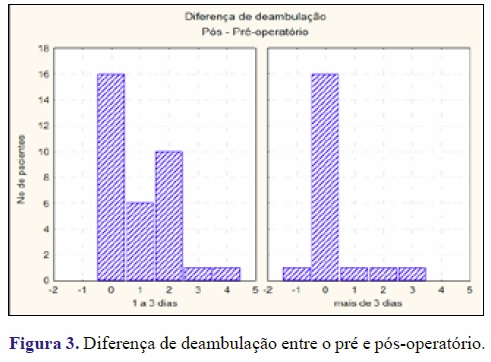
Existe diferença significativa entre os dois grupos (p=0,016). Curiosamente, os pacientes que foram operados mais tarde (mais de 3 dias entre a fratura e a cirurgia) tiveram uma recuperação significativamente melhor que os pacientes que foram operados mais cedo (1 a 3 dias) (Figura 3).
]]>
Em relação a mortalidade,houve 20 óbitos entre os 93 pacientes do estudo (21,5%). Desses pacientes, 14 pacientes (70%) vieram a óbito com 3 meses ou menos de pós-operatório, 4 pacientes com 3 meses a 1 ano de pós-operatório (20%) e 2 pacientes com mais de 1 anos de pós-operatório (10%). Além disso, deve-se lembrar que outros 19 pacientes tiveram perda de seguimento (20,43%) e assim não se pode estimar corretamente a taxa de mortalidade. Mas se considerarmos apenas os pacientes que tiveram mais de 4 meses de seguimento, a taxa de mortalidade vai para 27,03%, sendo desses, 70% antes do 3º mês de pós-operatório, ou seja, 18,91%.
DISCUSSÃO
A artroplastia parcial do quadril é um procedimento seguro, simples e rápido que permite ao paciente mobilização precoce[11], sendo o método de escolha para tratamento de fraturas mediais instáveis do colo femoral nos pacientes idosos com pobre estado de saúde geral, baixa capacidade mental, pouca demanda funcional e baixa expectativa de vida[12].
Dos 54 pacientes submetidos à artroplastia parcial do quadril encontramos uma idade média de 82,5 anos e o sexo feminino foi predominante (79,63%). Norish et al acompanhando 500 próteses parciais com seguimento de 7 anos relatou idade média de 82 anos e 85% eram mulheres[6].
A taxa de mortalidade geral do presente estudo foi de 21,5% em quatro meses de acompanhamento mínimo, semelhante às taxas de mortalidade encontradas na literatura: Sipila et al[13], 12% em quatro meses, Jalovaara[14] , 19% em um ano,e Norish et al, 23% em 1 ano de seguimento[6]. Shah[7] et al verificou que a mortalidade intra-hospitalar pós-operatória após hemiartroplastia era de 3.1% e os principais fatores associados eram idade maior que 85 anos, sexo feminino, 3 ou mais comorbidades e que a principal causa de óbito era pneumonia.
Alguns autores acreditam que a hemiartroplastia pode ser dolorosa devido à lesão na cartilagem acetabular provocada pela cabeça metálica da prótese e isto pode evoluir para protusão acetabular[8,15,16] . Em nossa casuística, 86% pacientes não relataram dor após o seguimento médio de 21 meses.
Na avaliação do estado mental dos pacientes no pré-operatório através do Short Portable Mental Status Questionnaire encontramos 22,2% dos pacientes com déficit cognitivo importante(SPMSQ<3). Soderqvist et al comprovou que pacientes com SPMSQ < 3 (demência) submetidos a prótese parcial de quadril possuem uma maior mortalidade no 1° ano[5]. Nosso trabalho mostrou que a demência não interfere na capacidade de deambulação pós-operatória.
Sipila et al indicou que a maior parcela de recuperação funcional dos pacientes submetidos à cirurgia do quadril ocorre nos primeiros 4 meses[13]. Ceder et al demonstrou haver pouca ou nenhuma recuperação adicional, no que se refere às atividades da vida diária e grau de independência, entre quatro meses e 1 ano após a fratura[17]. Borgquist et al concluiu que a dependência para atividades de vida diária e a capacidade deambulatória permanecem constantes após quatro meses da fratura, até 10 anos de acompanhamento[18]. Por essa razão, incluímos somente pacientes com seguimento mínimo de 4 meses. Nossa casuística mostrou que pacientes previamente dependentes pelo Método de Katz tiveram pior resultado funcional em relação a capacidade de deambulação pós-operatória.
O momento ideal para operar fraturas do quadril em pacientes idosos é crucial. Vários trabalhos sugerem um melhor resultado clínico, menor tempo de internação, diminuição de mortalidade e complicações naqueles pacientes operados precocemente[1,19,20,21], especialmente num período menor de 48 horas, segundo metanálise envolvendo 16 estudos prospetivos e observacionais[21]. Isso pode ser difícil em pacientes idosos, com múltiplas comorbidades, especialmente as cardiovasculares. Em nosso trabalho, curiosamente, não encontramos esta relação.
Uma das principais preocupações com a artroplastia no paciente idoso é a estabilidade do implante. A luxação é complicação freqüente nestes pacientes que até então tinham mobilidade normal do quadril e apresentam maior insuficiëncia de partes moles[22]. Sua incidência varia de 1-15%[23,24]. Em nossa série, tivemos um indice de luxação em torno de 4,65% no total de 93 submetidos a cirurgia. A luxação precoce pode aumentar a mortalidade em 65-75% nos primeiros seis meses pós-operatórios[22]. Fatores de risco para a luxação incluem ressecção insuficiente do colo, insuficiência de partes moles, impacto por restituição ineficaz de offset horizontal, dimensionamento inadequado da cabeça femoral protética[25] Nihn et al concluíram que a presença de um pequeno ângulo centro-borda de Wiberg, semelhante as displasias acetabulares, é fator de risco para luxação em artroplastias parciais unipolares[26]. Doenças neurológicas progressivas como demência e Mal de Parkinson também são consideradas em alguns estudos como fator de risco para instabilidade[27,28,29]. Em relação
à via de acesso, utilizamos como rotina em artroplastias parciais e totais o acesso posterior, mesmo ela sendo considerado uma via de acesso com maior incidência de luxação em alguns trabalhos[30,31,32] . Outros autores publicaram trabalhos mostrando não haver diferença nos índices de luxação pela via de acesso utilizada[33,34]. Em nossa série, em alguns casos, quando possível, procuramos preservar piriforme, mas não temos idéia de quanto a preservação deste tendão pode influenciar na estabilidade do implante.
Nenhum paciente nesses três anos de seguimento precisou realizar conversão para artroplastia total de quadril. A revisão da artroplastia parcial e conversão para artroplastia total foi avaliada e mostrou ser procedimento com bons resultados clínicos e funcionais e com índice de complicações semelhante aos de uma cirurgia de revisão(35,36). Segundo o Registro Norueguês que avaliou 595 revisões, o risco de falha na conversão de artroplastia parcial para total aumenta quando se preserva a haste femoral(37) . Sah et al avaliou o risco de luxações após conversão de artroplastia parcial para total, comparando a um grupo de revisões de prótese total. Encontraram o dobro de luxações de prótese e atribuíram essa complicação ao menor número de cabeça femoral protética e ao balanço inadequado de partes moles(38).
Em nosso Serviço utilizamos a hemiartroplastia parcial com prótese unipolar, com haste cimentada polida e cabe ça intercambiável. Consideramos esta opção mais simples e de menor custo. Raia et al, em estudo prospetivo randomizado, comparou os dois grupos em pacientes acima de 65 anos e concluiu não haver diferença no status deambulatório, mortalidade, índice de luxações, tempo de internação hospitalar, sangramento, complicações pós-operatórias e qualidade de vida pelo questionário SF-36 em seguimento mínimo de 1 ano (37). Calder et al randomizou 141 pacientes com mais de 80 anos e constatou que a mortalidade, complicações e Harris Hip escores foram idênticos nos dois grupos. Erosão acetabular foi observada em 3 pacientes no grupo unipolar, mas não no grupo bipolar, não foram necessárias revisões e que a diferença não foi estatisticamente significativa(40). Bhattacharyya em revisão de literatura conclui que os custos iniciais mais elevados da hemiartroplastia bipolar não justificam seu uso(41).
Outra controvérsia diz respeito à indicação de artroplastia parcial ou total nos pacientes idosos com fratura de colo femoral. Alguns trabalhos consideram que a hemiartroplastia não é a melhor opção de tratamento em fraturas do colo femoral em idosos[42,43,44,45]. Uma metanálise publicada em 2009 incluiu 407 pacientes e 3 estudos clínicos relevantes randomizados controlados. No acompanhamento de longo prazo, verificou-se que na Artroplastia Total os pacientes foram capazes de deambular melhor, tinham melhores resultados em escores que avaliavam qualidade de vida e relataram menos dor em comparação com os pacientes submetidos à hemiartroplastia, além de serem menos propensos a sofrer uma nova cirurgia do quadril. Considerando os resultados de longo prazo mais favoráveis em pacientes com prótese total de quadril, concluíram os autores que esta deve ser indicada em pacientes com boas condições de saúde, sem doenças cardiovasculares descompensadas, com maior expectativa de vida e que vão se beneficiar dos resultados mais duradouros da artroplastia total(47). Um estudo que avaliou a relação custo X efetividade das opções de artroplastia em pacientes idosos saudáveis com fraturas desviadas de colo de fêmur concluiu que a prótese total, apesar do custo inicial mais elevado, tem melhor aplicação neste grupo de pacientes, em virtude dos resultados mais duradouros e melhor qualidade de vida(48). Alguns trabalhos mostram uma piora da qualidade de vida e do status deambulatório após fratura da extremidade proximal do fêmur tratada com osteossíntese ou artroplastia(49,50). Nesta série, observamos uma perda da capacidade deambulatória em mais da metade dos pacientes, ou seja, muitos pacientes que antes deambulavam sem auxílio passaram a necessitar de bengalas ou andador para sua locomoção. A fisioterapia ajudou certamente na reabilitação, mas não se mostrou capaz de trazer aos pacientes níveis deambulatórios semelhantes àqueles antes da fratura. Obviamente outros fatores como idade avançada e descompensação de comorbidades clínicas também podem influenciar nesses resultados.
CONCLUSÃO
Pacientes com fratura do colo do fêmur submetidos à prótese parcial de quadril apresentam em nossa série uma perda de capacidade deambulatória, uma mortalidade pós-operatória em torno de 20%, com baixo índice de complicações em seguimento de curto prazo. Acreditamos esta ser uma alternativa viável de tratamento em pacientes idosos, com pouca capacidade deambulatória e com outras comorbidades clínicas descompensadas.
]]> REFERÊNCIAS BIBLIOGRÁFICAS
1. Casaletto JA, Gatt R. Post-operative mortality related to waiting time for hip surgery. Injury. 2004; 35: 114-120 [ Links ]
2. Robertson BD, Robertson TJ. Postoperative delirium after hip frature. J Bone Joint Surg Am. 2006; 88A (9): 2060-2068 [ Links ]
3. Bhandari M, Devereaux PM, Swiontkowski MF, Tornetta P, Obremski W, Kowal KJ. Internal fixation compared with arthroplasty for displaced fratures of the femoral neck. J Bone Joint Surg Am. 2003; 85A (9): 1674-1681 [ Links ]
4. Faraj S, French G, McAuslan A. Hemiarthroplasty for frature neck of femur, was it the right option?. J Bone Joint Surg Br. 2005; 87B (1): 30-31 [ Links ]
5. Soderqvist A, Miedel R, Ponzer S, Tidermark J. The influence of cognitive function after hip frature. J Bone Joint Surg Am. 2006; 88A (10): 2115-2123 [ Links ]
6. Norrish AR, Rao J, Parker MJ. Prosthesis survivorship and clinical outcome of the Austin Moore hemiarthroplasty: an 8-year mean follow-up of a consecutive series of 500 patients. Injury. 2006; 37: 734-739 [ Links ]
7. Shah Steven N, Wainess Reid M, Karunakar Madhav A. Hemiarthroplasty for Femoral Neck Frature in the Elderly Surgeon and Hospital Volume - Related Outcomes. J Arthroplasty. 2005; 20 (4): 503-508 [ Links ]
8. Kaltsas DS, Klugman DJ. Acetabular erosion: a comparison between the Austin Moore and Monk hard top prostheses. Injurs. 1986; 17: 230-236 [ Links ]
9. Katz S, Ford AB, Moskowitz RW, BA Jacson, Jaffe MW. Studies of illness in the aged. The index of ADL: a standardized measure of biological and psychosocial function. JAMA. 1963; 185: 914-919 [ Links ]
10. Pfeiffer E. A short portable mental status questionnaire for the assessment of organic brain deficit in elderly patients. J Am Geriatr Soc. 1975; 23: 433-441 [ Links ]
11. Harris WH. Traumatic arthritis of the hip after dislocation and acetabular fratures: treatment by mold arthroplasty. An end result study using a new method of result evaluation. J Bone Joint Surg Am. 1969; 51A: 737-755 [ Links ]
12. Albuquerque H, Albuquerque PCVC. Hemiartroplastia bipolar do quadril como tratamento primário das fraturas do colo do fêmur, graus III e IV de Garden. Rev Bras Ortop. 1993; 28 (3): 144-148 [ Links ]
13. Sipila J, Hyvönen P, Partanen J, Ristiniemi J, Jalovaara P. Early revision after hemiathroplasty and osteosynthesis of cervical hip frature. Ata Orthop Scand. 2004; 75 (4): 402-407 [ Links ]
14. Jalovaara P, Virkunnen H. Quality of life after primary hemiarthroplasty for femoral neck frature.6-year follow-up of 185 patients. Ata Orthop Scand. 1991 Jun; 62 (3): 208-217
15. Kim YH. The reaction of the acetabular articular cartilage to bipolar hemiarthroplasty. Yonsei Med. J.. 1986; 27: 234-238 [ Links ]
16. Kofoed H, Kofod J. Moore prosthesis in the treatment of fresh femoral neck fratures. A critical review with special attention to secondary acetabular degeneration. Injury. 1983; 14: 531-540 [ Links ]
17. Ceder L, Thorngren KG, Wallden B. Prognostic indicators and early home rehabilitation in elderly patients with hip fratures. Clin Orthop Relat Res. 1980 Oct; 152: 173-184
18. Bjorguist K, Reikeras O. Hemiarthroplasty in worst cases is better than internal fixation in best cases of displaced femoral neck fratures. Ata Orthopaedica. 2006; 77 (3): 368-374 [ Links ]
19. Casaletto JA, Gatt R. Post-operative mortality related to waiting time for hip frature surgery. Injury. 2004 Fev; 35 (2): 114-120
]]> 20. Moran CG, Wenn RT, Sikand M, Taylor AM. Early mortality after hip frature: is delay before surgery important?. J Bone Joint Surg Am. 2005 Mar; 87 (3): 483-48921. Shiga T, Wajima Z, Ohe Y. Is operative delay associated with increased mortality of hip frature patients? Systematic review, meta-analysis, and meta-regression. Can J Anaesth. 2008 Mar; 55 (3): 146-154
22. Blewitt N, Mortimore S. Outcome of dislocation after hemiarthroplasty for fractured neck of the femur. Injury. 1992; 23: 320 [ Links ]
23. Chan RN, Hoskinson J. Thompson prosthesis for fractured neck of femur. A comparison of surgical approaches. J Bone Joint Surg Br. 1975; 57: 437 [ Links ]
24. D'Arcy J, Devas M. Treatment of fratures of the femoral neck by replacement with the Thompson prosthesis. J Bone Joint Surg Br. 1976; 58 (3): 279 [ Links ]
25. Pajarinen J, Savolainen V, Tulikoura I. Factors predisposing to dislocation of the Thompson hemiarthroplasty: dislocations in 338 patients. Ata Orthop Scand. 2003; 74: 45 [ Links ]
26. Ninh Christopher C, Sethi Anil, Hatahet Mohammed, Les Clifford, Morandi Massimo, Vaidya Rahul. Hip Dislocation After Modular Unipolar Hemiarthroplasty. The Journal of Arthroplasty. 2009; 24 (5): 768-774 [ Links ]
27. Lu-Yao GL, Keller RB, Littenberg B. Outcomes after displaced fratures of the femoral neck. A metaanalysis of one hundred and six published reports. J Bone Joint Surg Am. 1994; 76: 15 [ Links ]
28. Garcia Jr A, Neer II CS, Ambrose GB. Displaced intracapsular fratures of the neck of the femur. 1. Mortality and morbidity. J Trauma. 1961; 1: 128 [ Links ]
29. Rothermel JE, Garcia A. Treatment of hip fratures in patients with Parkinson's syndrome on levodopa therapy. J Bone Joint Surg Am. 1972; 54: 1251 [ Links ]
31. Keene GS, Parker MJ. Hemiarthroplasty of the hip - the anterior or posterior approach? A comparison of surgical approaches. Injury. 1993; 24: 611 [ Links ]
32. Unwin AJ, Thomas M. Dislocation after hemiarthroplasty of the hip: a comparison of the dislocation rate after posterior and lateral approaches to the hip. Ann R Coll Surg Engl. 1994; 76: 327 [ Links ]
33. Salvati EA, Wilson Jr PD. Long-term results of femoral-head replacement. J Bone Joint Surg Am. 1973; 55: 516 [ Links ]
34. Wood MR. Femoral head replacement following frature: an analysis of the surgical approach. Injury. 1980; 11: 317 [ Links ]
35. Pankaj A, Malhotra R, Bhan S. Conversion of failed hemiarthroplasty to total hip arthroplasty: A short to mid-term follow-up study. Indian J Orthop. 2008 Jul; 42 (3): 294-300
36. Diwanji SR, Kim SK, Seon JK, Park SJ, Yoon TR. Clinical results of conversion total hip arthroplasty after failed bipolar hemiarthroplasty. J Arthroplasty. 2008 Oct; 23 (7): 1009-1015
37. Figved W, Dybvik E, Frihagen F, Furnes O, Madsen JE, Havelin LI, et al. Conversion from failed hemiarthroplasty to total hip arthroplasty: a Norwegian Arthroplasty Register analysis of 595 hips with previous femoral neck fratures. Ata Orthop. 2007 Dec; 78 (6): 711-718
38. Sah AP, Estok DM. Dislocation rate after conversion from hip hemiarthroplasty to total hip arthroplasty. J Bone Joint Surg Am. 2008 Mar; 90 (3): 506-516
39. Raia F, Chapman C, Herrera M, Schweppe M, Michelsen C, Rosenwasser M. Unipolar versus bipolar hemiarthroplasty for femoral neck fratures in elderly patients?. Clinical Orthopaedics and related Research. 2003; 414: 259-265 [ Links ]
40. Calder SJ, Anderson GH, Jagger C. Unipolar or bipolar prosthesis for displaced intracapsular hip frature in octogenarians: a randomized prospective study. J Bone Joint Surg Br. 1996; 78: 391-394 [ Links ]
41. Bhattacharyya T, Koval K. Unipolar Versus Bipolar Hemiarthroplasty for Femoral Neck Fratures: Is There a Difference?. J Orthop Trauma. 2009; 23: 426-427 [ Links ]
41. Keating J, Grant A, Masson M. Randomized comparison of reduction and fixation, bipolar hemiarthroplasty, and total hip arthroplasty. Treatment of displaced intracapsular hip fratures in healthy older patients. JBJS. 2006; 88A: 249 [ Links ]
43. Baker R, Squires B, Gargan MF. Total hip arthroplasty and hemiarthroplasty in mobile, independent patients with a displaced intracapsular frature of the femoral neck. JBJS. 2006; 88A: 2583 [ Links ]
44. Iorio R, Schwartz B, Macaulay W. Surgical treatment of displaced femoral neck fratures in the elderly: A survey of the American Association of Hip and Knee Surgeons. J Arthroplasty. 2006; 21: 1124 [ Links ]
45. Blomfeldt R, Tornkvist H, Eriksson K. A randomised controlled trial comparing bipolar hemiarthroplasty with total hip replacement for displaced intracapsular fratures of the femoral neck in elderly patients. JBJS. 2007; 89B: 160 [ Links ]
46. Healy W, Iorio R. Total hip arthroplasty: optimal treatment for displaced femoral neck fratures in elderly patients. Clin Orthop. 2004; 429: 42 [ Links ]
47. Seo-Kiat Goh, Miny Samuel, Su David Hsien Ching, Chan Edwin Shih-Yen, Yeo Seng-Jin. Meta-analysis Comparing Total Hip Arthroplasty With Hemiarthroplasty in the Treatment of Displaced Neck of Femur Frature. The Journal of Arthroplasty. 2009; 24 (3): 400-406 [ Links ]
48. Lover J, Hoffman M, Malchau H, Tosteson A, Koval K. A Cost-effectiveness Analysis of the Arthroplasty Options for Displaced Femoral Neck Fractures in the Active, Healthy, Elderly Population. The Journal of Arthroplasty. 2009; 24 (6): 854-860 [ Links ]
49. Boonen S, Autier P, Barette M, Vanderschueren D, Lips P, Haentjens P. Functional outcome and quality of life following hip frature in elderly women: a prospective controlled study. Osteoporos Int. 2004 Fev; 15 (2): 87-94
50. Randell AG, Nguyen TV, Bhajerao N, Silverman SL, Sambrook SL, Sambrook PN, et al. Deterioration in quality of life following hip frature: a prospective study. Osteoporos Int. 11 (5): 460-466
]]>Conflito de interesse:
Nada a declara
Fernando Rossi Mielke
Rua Atanásio Belmonte 175, torre 07,
apto 527
Bairro Boa Vista
Porto Alegre ]]>
Rio Grande do Sul
Brasil
CEP 90520550
frmielke@hotmail.com
Data de Submissão: 2012-12-12
Data de Revisão: 2013-05-02
Data de Aceitação: 2013-06-03
]]>