Que técnica paliativa para as sequelas gleno-umerais das lesões obstétricas do plexo braquial?
João VideI; Diogo GomesI; Marta SalgueiroI; Eduardo MatosI; Margarida HenriquesI
I. Serviço de Cirurgia Plástica e Reconstrutiva. Hospital S. Maria. Centro Hospitalar Lisboa Norte. Portugal.
RESUMO
]]> Objetivo: a lesão obstétrica do plexo braquial está presente em 1-4 em cada 1000 partos. Apesar da maioria recuperar, até 19% vão apresentar sequelas definitivas, mesmo após cirurgias de reparação primária do plexo braquial, sendo o ombro a região anatómica mais afetada. As cirurgias paliativas do ombro foram desenvolvidas para aumentar a função e qualidade de vida destes pacientes, no entanto não há consenso quanto ao timing cirúrgico e indicações de cada técnica. Avaliamos sistematicamente toda a evidência disponível nos últimos 10 anos com o objetivo de determinar quais as melhorias na função e quais os fatores que influenciam o resultado destas técnicas. Determinar a capacidade de remodelação gleno-umeral foi um objetivo secundário.Fonte: pesquisamos 5 bases de dados - Cochrane Review Library, TRIP, Pubmed, Web of Knowledge e Science Direct. Foram incluídos estudos de doentes com lesões obstétricas do plexo braquial submetidos a técnicas paliativas do ombro publicados nos últimos 10 anos (de janeiro de 2003 a dezembro de 2012). Avaliamos as mobilidades ativas e a classificação de Mallet pós-operatória. Numa análise post-hoc avaliamos o efeito das técnicas na remodelação glenóideia, através das alterações do ângulo de retroversão, percentagem de cobertura da cabeça umeral e da alteração morfológica. A avaliação da qualidade metodológica foi realizada independentemente por 2 autores, através de um formulário de revisão crítica.
Síntese dos dados: foram incluídos 1873 doentes num total de 42 estudos: 27 estudos com técnicas de partes moles, 12 estudos com procedimentos ósseos e 3 com combinação de ambas as técnicas. Todos os estudos têm baixo nível de evidência, sendo a maioria séries de casos, com múltiplos viéses e elevada heterogeneidade. A melhoria média da rotação externa foi de 58º e 61º na abdução. A melhoria média na classificação de Mallet foi 5,0 pontos e 1,5 no parâmetro da rotação externa. Observou-se melhoria da retroversão glenóideia entre 9 e 21º e percentagem de cobertura cefálica entre 4 e 25%.
Conclusões: considerando a qualidade metodológica dos estudos incluídos, a evidência parece apontar para um efeito benéfico das técnicas paliativas gleno-umerais na mobilidade, função e remodelação glenoumeral. No entanto, não é possível estabelecer indicações claras para as diferentes técnicas, o melhor timing para a cirurgia, nem se o benefício se mantêm após 10 anos da data da cirurgia. Para responder a estas questões é necessário investir em estudos com desenhos apropriados, de elevada qualidade metodológica e com estratégias de diminuição da heterogeneidade.
Palavras chave: Paralisia do plexo braquial, paralisia obstétrica do plexo braquial, procedimentos cirúrgicos, cirurgia paliativa.
ABSTRACT
Objectives: obstetric Brachial Plexus Palsy occurs in 1-4 in every 1000 births. Although most recover, up to 19% will present definitive sequelae, even after primary repair surgeries of the brachial plexus, being the shoulder the most commonly affected area. Palliative surgeries have been developed to increase function and quality of life of these patients, however there’s no agreement in regard to the surgical timing and indications of each technique. We evaluated all the available evidence published in the last 10 years with the goal to determine the improvement in function and the factors that have an influence on the result of these techniques. Determination of the gleno-umeral remodeling capacity was a secondary objective.
Source: we have researched 5 databases - Cochrane Review Library, TRIP, Pubmed, Web of Knowledge and Science Direct. We included studies that had obstetric brachial plexus palsy patients who were submitted to palliative techniques of the shoulder, published in the last 10 years (from January 2003 to December 2012). We evaluated the post-operative active range of motion and Mallet classification. In a post-hoc analysis, we evaluated the effect of the technique in glenoid remodelation, through retroversion angle, percentage of humeral head coverage and change in morphology.
The methodological quality was assessed independently by two reviewers, through a critical review form.
]]> Data syntheses: it was included 1873 patients from a total of 42 studies: 27 studies with soft tissues procedures, 12 studies with bony procedures and 3 with combination of techniques. All the studies have low evidence level, and the majority are case series with multiple biases and high heterogeneity. The main improvement in external rotation was 58º and 61º in abduction. The main improvement in Mallet score was 5,0 points and 1,5 in the parameter of external rotation. We observed improvement in glenoid retroversion between 9 and 21º and percentage of humeral head covereage between 4 and 25%.Conclusions: considering the methodological quality of the included studies, the evidence seems to show an improvement in range of motion, function and gleno-umeral remodelation with palliative techniques. However it’s not possible to establish clear indications to the different techniques, the better surgical timing, neither if the benefits withhold 10 years after surgery. To answer these questions it’s necessary to invest in studies with appropriate designs, of high methodological quality and with strategies to diminish heterogeneity.
Key words: Brachial plexus palsy, obstetric brachial plexus palsy, surgical procedures, palliative surgery.
INTRODUÇÃO
Estima-se que a prevalência internacional de lesão obstétrica do plexo braquial (LOPP) seja de 1-4/1,000 nados vivos[1-4], tendo-se verificado uma tendência para o aumento da frequência nos últimos anos. Até à data não existem estudos publicados que nos permitam conhecer a frequência desta patologia em Portugal.
O espectro de lesão nervosa pode variar desde neuropraxia até axonotemese ou avulsão da raiz nervosa. Embora a maior partes dos casos apresente recuperação completa, 5-19% dos casos vão apresentar alguma sequela[5]. Estão descritos padrões mais frequentes de lesão, sendo que 75% dos casos correspondem a lesões dos troncos superiores, C5-C6±C7 (paralisia de Erb)[6]. A classificação de Narakas[7] é a que melhor relaciona o tipo de lesão com a história natural: tipo I – lesão das raízes de C5-C6; tipo II – lesão das raízes de C5-C6-C7 (paralisia de Erb); tipo III – lesão completa de todo o plexo braquial, sem Síndrome de Horner; e tipo IV – lesão completa de todo o plexo braquial com Síndrome de Horner associado.
O tratamento inicial é de suporte, com preservação da mobilidade através da fisioterapia ou com uso de talas.
O timing para a intervenção primária, que consiste na tentativa de reparação nervosa através de diversas técnicas (neurólise, enxerto nervoso e neurotização, conforme o grau e tipo de lesão), ainda é controverso. Vários estudos procuraram estabelecer marcos na recuperação motora que permitissem identificar os doentes que beneficiariam com a cirurgia primária, baseados na recuperação de um único músculo[8,9], em vários scores[10-12] ou na recuperação muscular com outros fatores prognósticos[13,14]. O marco criado por Gilbert[8] - ausência de recuperação do bicípite braquial ao 3º mês, ainda hoje é aceite como indicação de exploração e cirurgia primária do plexo, quer por ter sido pioneiro, quer pela simplicidade da indicação. Em relação à história natural, verificou-se que os casos com recuperação motora antigravitacional até aos 2 meses, vão evoluir para a recuperação completa dentro de 1-2 anos. Os restantes casos, submetidos ou não a reparação primária, cursam com o desenvolvimento de sequelas ao nível do ombro, cotovelo e mão[15].
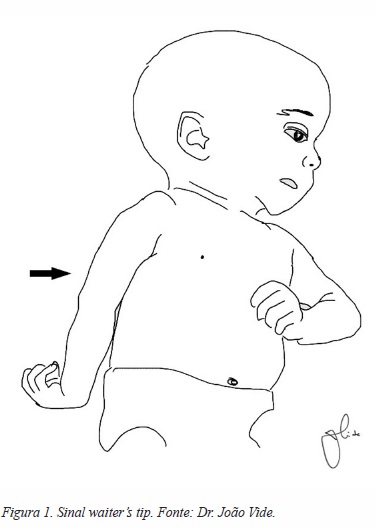
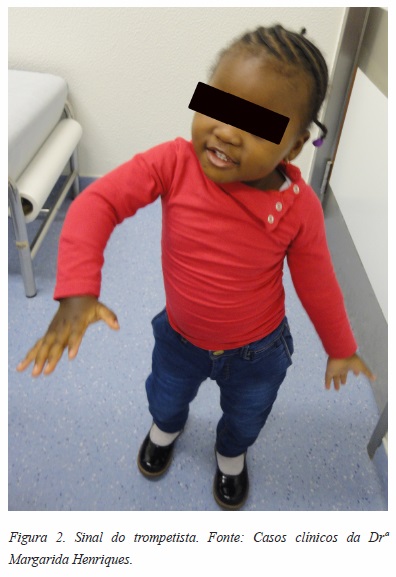
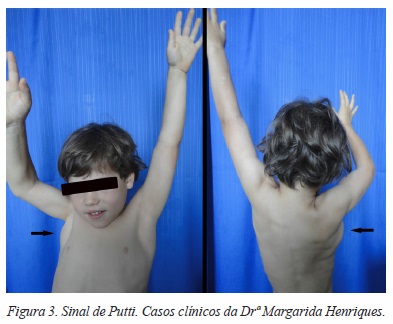
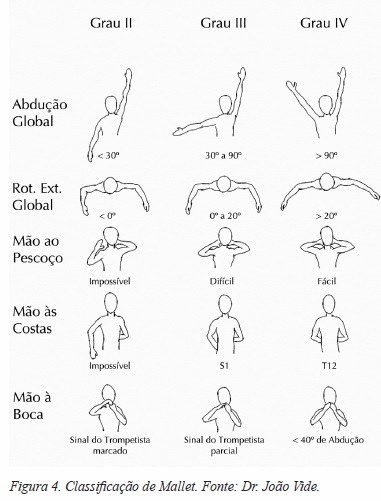
No ombro, a sequela mais frequente é a contractura em rotação interna e adução (CORI), originada pela recuperação mais rápida dos músculos subescapular e grande peitoral, que vão condicionar a recuperação do rotadores externos e abdutores[15] (Figura 1). Frequentemente esta contractura é um fator major na limitação funcional, impedindo a elevação da mão até à boca numa posição normal (Figura 2) e forçando o movimento de abdução ao nível de articulação escapulo-torácica, visível clinicamente quando está presente o sinal de Putti[15] (Figura 3). Estas alterações são alvo de valorização na classificação funcional proposta por Mallet (Figura 4). É o desequilíbrio das forças musculares e a limitação da mobilidade a nível gleno-umeral que vão dar origem a deformidades ósseo-ligamentares, que habitualmente se manifestam logo após os primeiros 5 meses de vida[16]. Em 1998, Waters et al[17] descreve e classifica estas alterações articulares em 7 tipos (Figura 5), e propõe a orientação da cirurgia paliativa do ombro considerando estas alterações.
]]>

]]>
As técnicas cirúrgicas paliativas, ou secundárias, preconizadas para o tratamento das sequelas glenoumerais das LOPB, objeto de estudo desta revisão, têm a sua indicação guiada pela idade do paciente, pelas mobilidades passivas e ativas do ombro, pela força dos músculos escapulares e periescapulares e pelas alterações ósseas encontradas. Embora não exista consenso, habitualmente pacientes mais novos, com deformidades ósseas ligeiras são preferencialmente tratados com procedimentos de partes moles, enquanto os procedimentos ósseos são reservados para doentes com mais idade, deformidades marcadas ou falências de técnicas de partes moles. A avaliação clínica das mobilidades passivas e ativas devem guiar as libertações ligamentares e tendinosas assim como os grupos musculares a serem transferidos e sua posição de inserção. A avaliação da força muscular permite estabelecer a viabilidade das transferências tendinosas.
Objetivos
Avaliamos de modo sistematizado os resultados dos procedimentos paliativos para as sequelas glenoumerais das LOPB com o objetivo de responder às questões:
1) Quais as intervenções que obtêm melhores resultados funcionais? Estes resultados mantêm-se a longo prazo?
]]> 2) Que fatores influenciam o resultado funcional? Idade, grau da lesão, cirurgia primária, alterações morfológicas ou da estabilidade glenoumeral?Um objetivo secundário foi determinar o impacto das intervenções na remodelação glenóideia.
MÉTODO DE REVISÃO
Critérios de Inclusão
Tipos de Estudo
Selecionamos todos os estudos com avaliações da mobilidade e/ou função após técnicas paliativas para sequelas gleno-umerais das LOPB. Poderiam ser incluídos ensaios clínicos randomizados, estudos comparativos prospetivos ou retrospetivos ou séries de casos. Não se incluíram casos clínicos pelos viéses a que estão sujeitos[18]. Limitamos a inclusão a publicações redigidas em Inglês, Italiano, Espanhol ou Português, publicadas nos últimos 10 anos (de 1 de janeiro de 2003 até 31 de dezembro de 2012).
Tipos de Paciente
Incluímos bebés, crianças e adolescentes até aos 20 anos de idade, na data do último procedimento paliativo gleno-umeral, sujeitos ou não a reparação nervosa primária.
Tipos de Intervenção
]]> As intervenções paliativas para sequelas glenoumerais de LOPB incluem procedimentos de partes moles: libertações capsulares por via aberta ou artroscópica, secção, alongamento ou transferências tendinosas; ou procedimentos ósseos: osteotomias de desrotação umeral externa (OTM desrot.) e interna (OTM RI), glenoplastias e osteotomias com rotação escapular (tilt triangular). Poderiam ser incluídos na revisão estudos que avaliassem e documentassem o efeito de qualquer destas intervenções cirúrgicas, isolada ou utilizada em combinação.Tipos de Medida de Outcome
Os outcomes primários foram as alterações nas mobilidades ativas, na escala de Mallet global[19] e/ou dos seus parâmetros de rotação externa (RE) e rotação interna (RI). As medidas de outcome secundárias foram as alterações do ângulo de retroversão glenoide (RG) e percentagem de cobertura da cabeça umeral (PHHA), do tipo de deformidade glenoide e/ou congruência da articulação gleno-umeral, descritiva ou através da utilização da classificação de Waters ou Glenoid Deformity Scale (GDS)[20].
Estratégia de Pesquisa
Pesquisamos cinco bases de dados: Cochrane Review Library, TRIP, Pubmed, Web of Knowledge e Science Direct.
A estratégia de pesquisa consistiu na introdução dos termos: "Obstetric Brachial Plexus Palsy Shoulder". Em todas as bases de dados, exceto na Cochrane Review Library, limitamos os resultados aos estudos publicados nos últimos 10 anos.
A seleção inicial, de acordo com os critérios de inclusão (Quadro I), foi realizada através do título e resumo. Quando não foi possível obter todos os dados para inclusão através do resumo, obtivemos o texto integral para avaliação. Realizamos ainda uma pesquisa secundária, através da revisão das referências dos artigos incluídos.

Avaliação da Qualidade Metodológica
Os estudos resultantes da pesquisa foram avaliados e selecionados independentemente por dois autores: JV e DG. Quando todos os critérios de inclusão foram cumpridos, o texto completo foi obtido.
Introduzimos todas as referências numa folha de cálculo do Microsoft® Excel para Mac 2011, v. 14.1.
Para cada estudo determinamos:
- O Nível de Evidência da NHMRC[18];
- A qualidade metodológica, através de um formulário de revisão crítica para estudos quantitativos por Law et al[21]. Esta ferramenta avalia a validade interna e externa de um estudo e os seus achados através da avaliação sistematizada dos seus items. Nas questões fechadas do formulário é atribuída a pontuação de 1 ponto, quando o critério é satisfeito, ou 0, quando o critério não é completamente satisfeito. Assim, a pontuação máxima de 16 pontos indica um estudo de excelente qualidade.
Avaliação dos Estudos
Realizamos uma descrição dos estudos incluídos, apresentando os dados através da percentagem dos estudos, da apresentação dos mínimos e máximos, ou do cálculo das médias ponderadas (considerando o número de participantes em cada estudo), em relação
a diversos parâmetros:
- Número, idade, cirurgias prévias, diagnósticos, classificação de Narakas, alterações gleno-umerais prévias, utilização de outras classificações e tempo de follow-up;
]]> - Descrição das cirurgias e resultados principais: efeito na mobilidade (rotação externa e abdução), função (alteração na classificação de Mallet) e na remodelação óssea (quando aplicável);- Complicações decorrentes do uso das técnicas cirúrgicas;
- Conclusões principais.
RESULTADOS
Descrição dos Estudos
Da estratégia de pesquisa resultaram um total de 941 estudos das cinco bases de dados pesquisadas, dos quais 75 foram selecionados para elegibilidade. Destes, 34 foram excluídos por não cumprirem todos os critérios de inclusão. Da pesquisa secundária dos artigos selecionados resultou a inclusão de 1 novo artigo[58]. Assim, esta revisão é uma síntese de 42 estudos que decorreram em 6 regiões: África (Egito), América do Norte (EUA, Canadá), América do Sul (Brasil), Ásia (Índia, Japão), Europa (França, Grécia, Holanda, Polónia, Reino Unido, Turquia) e Médio Oriente (Arabia Saudita, Irão). Incluímos estudos diferentes do mesmo grupo de investigação (Aydin, Kozin, Nath, Waters e Zoppi filho) em que não houve sobreposição de resultados. Houve concordância de 100% nos estudos incluídos.
Avaliação Crítica
Nível de Evidência
Cinco dos 42 estudos (12%) são comparativos, e apenas 2 comparam resultados de diferentes técnicas cirúrgicas: Abdel-Ghani et al[22] compara a transferência do grande dorsal (GD) com a do GD em conjunto com o redondo maior (RM); enquanto Abdelaziz et al[23] comparou a transferência do RM com a transferência do trapézio em conjunto com o RM. Como não houve randomização à atribuição dos grupos, ambos os estudos foram classificados como III-b (nível de evidência NHMRC). Os restantes 37 estudos são séries de casos, com avaliação pré e pósoperatória dos resultados. Todos os estudos contém um número considerável de viéses, pelo que os resultados devem ser interpretados com precaução.
]]> Qualidade MetodológicaA qualidade dos estudos foi razoável, sendo o score médio 10,6 (IC95 10,1 – 11,1) em 16 pontos. O estudo com maior qualidade metodológica, score 13, foi de Dodwell et al[33] em 2012. Os estudo com menor qualidade, score 7, foram os de Abid et al[24] e Al Qattan et al[26] em 2012 e 2003, respetivamente.
Os critérios de qualidade cumpridos foram variáveis. Em 10 destes a maioria dos estudos cumpriu: declaração do objetivo dos estudo, revisão da literatura relevante, desenho do estudo apropriado ao objetivo, descrição da amostra estudada e intervenção realizada em detalhe, medidas de outcome válidas e confiáveis, análise apropriada dos resultados e a sua implicação na atividade clínica. Dois critérios foram cumpridos em cerca de 50% dos estudos: reportagem do significado estatístico e limitações do estudo. Os critérios que poucos ou nenhuns estudos cumpriram foram 4: ausência de viéses, escolha justificada do tamanho da amostra, declaração de preenchimento do consentimento informado e a importância clínica das diferenças encontradas. Foram encontradis vários tipos de viéses: de seleção, de performance, de deteção e de relato.
Resultados da Pesquisa
Participantes
Foram incluídos um total de 1873 doentes, de estudos com amostras entre 6 e 203 doentes. A maioria incluiu pequenas amostras (57% com amostras = 30 doentes), enquanto seis estudos apresentaram resultados de grandes amostras[29,34,36,45,52,56].
A idade média ponderada na altura na data da cirurgia foi 4,3 anos (entre 0,3 e 19,8 anos). A maioria dos estudos avaliou os resultados de uma técnica cirúrgica em doentes com um espectro de idades alargado.
Os diagnósticos mais frequentes foram a CORI, défice de abdução e/ou rotação externa e, por último, instabilidade/incongruência gleno-umeral (66,7%, 23,8% e 9,5%, respetivamente).
Em 76% dos estudos foi avaliada a gravidade da lesão segundo a classificação de Narakas: 8 estudos[27,34,38,39,50,53,63,59] não incluíram doentes com parésias completas (GIII ou IV de Narakas) e num estudo[22] apenas se incluíram doentes parésias completas.
A avaliação das alterações da morfologia da glenoide e congruência articular foi realizada de vários modos: em 12 estudos[2,7,11,12,20,21,29,30,39,40,41,43] foi utilizada a classificação de Waters; a descrição em congruente/não congruente foi realizada em 10 estudos[26,31,36,40,43,49,52,53,54,59]; a descrição morfológica foi realizada em 10 estudos[24,31,35,37,40,44,48,49,57,58]; e dois estudos[38,39] fizeram a avaliação segundo a GDS. Seis estudos incluíram doentes sem alterações ou com alterações morfológicas ligeiras e ombros estáveis[26,28,35,37,52,63] (todos utilizaram técnicas de partes moles) enquanto 9 estudos incluíram doentes com alterações moderadas a graves da morfologia e/ou instabilidade gleno-umeral (2 com técnicas de partes moles[45,49], 6 com técnicas ósseas[42,43,48,59,61,58] e um[33] com combinação de transferências tendinosas com glenoplastia). Os restantes estudos incluíram doentes com vários tipos de displasia e instabilidade gleno-umeral.
]]> Outras avaliações foram utilizadas - classificação de Gilbert[22,52], MRC[23,30,37,50,51,55,63], AMS[33,60], avaliação da morfologia da cintura escapular[43] e distância coracoumeral[47]; que apesar de serem instrumentos válidos, são pouco utilizados, o que limita o valor comparativo da sua utilização.Em relação à inclusão de doentes submetidos a reparação primária prévia, 50% dos estudos não refere se incluiu ou excluiu estes doentes. Sete estudos[22,34,35,37,49,50,63] não incluíram doentes submetidos a qualquer tipo de cirurgia de reparação primária do plexo braquial, enquanto 14 estudos[24,27,29,33,36,38,39,42,44,45,48,52,55,56] incluíram.
O tempo médio de follow-up foi 3,9 meses (1,1[39]-30[37]).
Tipos de Intervenções
As cirurgias paliativas do ombro nas LOPB incluídas nesta revisão foram classificadas em 3 grupos: procedimentos de partes moles - 27 estudos (1266 doentes); procedimentos ósseos – 12 estudos (482 doentes); procedimentos ósseos e transferências musculares associadas – 3 estudos (125 doentes) (Quadro II).
Eficácia das Intervenções
]]> MobilidadesTodos os estudos mostraram melhoria na rotação externa, sendo o ganho médio ponderado de 58,4º (26,8[58] - 104º[22]). A média da rotação externa final foi de 65,1º. Apenas um estudo não apresentou melhoria na abdução[25], sendo que o ganho na abdução foi de 60,8º (-7º[25] – 117º[45]). A média da abdução final nos estudos foi de 137,8º.
Relativamente à rotação externa final, as cirurgias de partes moles apresentaram 69,3º (ganho 56,5º), as cirurgias ósseas 55,5º (ganho 55,5º) e as cirurgias combinadas 45º (ganho 78,8º). As mobilidades por técnica cirúrgica estão representadas na figura 6.
Na abdução final, as cirurgias de partes moles apresentaram 140,4º (ganho 61,0º), as cirurgias ósseas 124,2º (ganho 62,8º) e as cirurgias combinadas 123,6º (ganho 54,9º). As mobilidades por técnica cirúrgica estão representadas na figura 7.
]]>
Figura 7
Escala de Mallet
Todos os estudos mostraram melhoria no classificação de Mallet total, sendo o ganho médio ponderado de 5,0 (1,639 – 8,0[56,60]). O Mallet total final médio foi 16,3 (12,0[40] – 20,7[55]). O parâmetro da rotação externa do Mallet melhorou 1,5 (0,6[39] – 2,0[26,56,59-61]), sendo a média ponderada final de 3,6 (2,1[33] – 4,0[26,56,59-61]). O parâmetro da rotação interna teve um ganho médio de 0,2 (-2,1[31] – 1,0[48,60]), sendo a média final 2,5 (2,0[60] – 3,3[44]).
Relativamente ao Mallet final, as cirurgias de partes moles apresentaram 16,3 (ganho 5,1), as cirurgias ósseas 15,7 (ganho 4,5) e as cirurgias combinadas 18,7 (ganho 6,6). O Mallet final por técnica cirúrgica está representado na figura 8.
Relativamente aos parâmetros de rotação externa e interna da classificação de Mallet, as cirurgias de partes moles apresentaram 3,8 (ganho 1,6) e 2,4 (ganho 0,1), as cirurgias ósseas 3,5 (ganho 1,2) e as cirurgias combinadas 2,1 (ganho 1,8) e 2,1 (ganho -0,8), respetivamente. Os parâmetros de rotação externa e interna por técnica cirúrgica estão representados na figura 9.
]]>
Remodelação da glenoide
Apesar de 76% dos estudos realizarem avaliação da deformidade pré-operatória, apenas 48% consideram o grau de alteração morfológica nas indicações cirúrgicas e apenas 41% avaliam o efeito destas na remodelação gleno-umeral. Quer as técnicas em partes moles, quer os procedimentos ósseos têm evidência a favor e contra a capacidade remodelativa destas técnicas. Nas primeiras, Kozin et al[39] num estudo com 23 crianças com 5,1 anos de idade média, com followup de um ano, mostra melhoria clínica e funcional, embora sem alterações da morfologia e estabilidade gleno-umeral, enquanto Waters et al[62], refere que estas técnicas têm a capacidade de parar a evolução das alterações, e observou uma melhoria marginal, que atribuiu a um possível resultado do crescimento normal. A evidência restante[24,31,32,38,41,50,53,57,60] apoia a capacidade de remodelação óssea, com melhoria da versão glenóideia entre 9 e 21º e a PHHA entre 4 e 25%. Nos procedimentos ósseos, Waters e Bae[61] num estudo com OTM de desrotação umeral, demonstrou que esta técnica não tem capacidade de remodelar a morfologia óssea. No entanto, as técnicas - tilt triangular[43], glenoplastia[33] e OTM de rotação interna[58,59], parecem ter um efeito benéfico na estabilidade e morfologia da articulação gleno-umeral (Quadro III).
]]> Complicações
Apenas 23 estudos (54,8%) reportaram as complicações. Em 2 estudos[24,27] não ocorreram complicações. A complicação mais frequentemente reportada, e que por vezes necessitou de correção cirúrgica, foi a contractura em rotação externa (CORE) / limitação da rotação externa, presente em 10 estudos[22,30,32,33,40,41,49,53,54,57] (em 4[22,30,49,54] estudos verificou-se em mais de 50% dos pacientes). Em 8 estudos ocorreram casos de falência do tratamento: 4 estudos com técnicas de partes moles[26,31,34,52 e 4] estudos com procedimentos ósseos[25,36,59,58]. Outras complicações reportadas foram neuropraxias transitórias[25], secção nervosa[33], e problemas relacionados com a incisão como seromas[26], queloides[34] e deiscência de sutura[63].
DISCUSSÃO
A nossa estratégia de pesquisa foi minuciosa e sistemática, o que permite a sua replicação posterior. Foi realizada uma pesquisa abrangente em várias bases de dados, com pesquisa secundária através das referências de cada artigo selecionado. Embora a exclusão de artigos escritos em Francês e os limites da pesquisa até 10 anos possam representar a exclusão de alguns artigos importantes, estamos confiantes que a maioria da evidência relevante sobre este tópico foi incluída. Outra limitação da nossa revisão foi a ausência de ocultação do autor e fonte do artigo.
Um achado importante deste artigo é que os estudos que avaliam os resultados das técnicas paliativas nas sequelas gleno-umerais de LOPB são de natureza heterogénea e diferem em variados parâmetros como a idade na data da cirurgia, a extensão das lesões pré-operatórias, o tempo de seguimento, entre outros. Esta heterogeneidade deve-se em parte à ausência de consenso nas indicações e timing destas técnicas. Procuramos realizar uma análise post-hoc simples destas variáveis, para observar eventuais diferenças de resultados. Assim, os resultados desta revisão devem de ser interpretados com cautela pois, embora a qualidade metodológica dos estudo incluídos seja aceitável, o nível de evidência é baixo, estão presentes vários viéses e as populações têm muita heterogeneidade intra e interestudos.
Mobilidade e Função:
As técnicas de partes moles e ósseas apresentam ganhos na RE ativa na ordem dos 55º. Os procedimentos combinados, embora com poucos estudos disponíveis, parecem obter ganhos de quase 80º, o que aponta para um eventual benefício cumulativo das intervenções. Na abdução, observouse melhoria perto dos 60º para qualquer grupo de técnicas. As cirurgias de partes moles genericamente apresentam os maiores valores de mobilidades finais, porque são estes doentes que têm maior mobilidade prévia à intervenção. A recuperação funcional, avaliada pela classificação de Mallet, é menor com procedimentos ósseos, observando-se um ganho médio de 4,5 pontos, enquanto as cirurgias de partes moles e combinadas obtêm 5,1 e 6,6, respetivamente.
Considerando as cirurgias de partes moles, há autores que defendem a utilização sistemática de transferências tendinosas com as libertações articulares, por garantirem ganhos superiores na rotação externa, abdução, função e capacidade de manutenção da redução articular, em oposição aos que defendem procedimentos faseados, para evitarem perda de força da RI e contracturas em RE. No entanto, em alguns estudos com transferências, há menor limitação funcional na rotação interna, em comparação a libertações articulares: Waters e Bae[60] mostra um ganho médio de 1 ponto no parâmetro de rotação interna da classificação de Mallet enquanto Van Slujis et al[57] e Breton et al[31] mostram limitação entre 0,6 e 2,1, respetivamente. Para tal pode justificar o recurso a libertações excessivas nos casos mais severos numa tentativa de estabilização gleno-umeral, sem recurso a transferência tendinosas para reequilíbrio muscular.
Embora não tenha sido realizado nenhum estudo comparativo entre a transferência do trapézio e do GD±RM, o último é capaz de aumentar a abdução, por aumentar a força de acoplagem, que permite maior eficácia do deltoide[29,34,51], e a rotação externa é inferior com a transferência do trapézio.
]]> Os resultados desta revisão mostram vantagem na utilização de transferências, em particular do GD±RM, para aumentar as libertações articulares, com resultados consistentemente superiores na mobilidade e função, e com perdas mínimas na RI que, na maioria das situações, não influenciam as AVDs[22,53,57]. A libertação articular isolada deve ser ponderada precocemente na criança sem alterações ósseas, que inicia o desenvolvimento da CORI.Com procedimentos ósseos, os resultados são muito variáveis: a OTM de RI para recentragem da cabeça umeral, embora com recuperações modestas na mobilidade articular (RE +26,8º e Abd +46,8º), permite um ganho funcional excelente (+5,2 na escala de Mallet); a Osteotomia de desrotação umeral permite colocar o membro superior na posição ideal, apresentando assim bons resultados na melhoria da mobilidade (RE +58º e Abd +64,1º) e função (+3,6 pontos); a Glenoplastia permitiu obter os ganhos mais elevados de RE (+72º), mas com discreta melhoria da abdução (+25º); o Tilt Triangular é uma técnica com resultados apenas descritos pelo seu autor - R. Nath, e embora sem resultados publicados para a mobilidade, tem uma excelente recuperação funcional, com ganho de 5,4 pontos no Mallet global.
Genericamente todas as técnicas têm bons resultados, quer na mobilidade ativa, quer na classificação funcional de Mallet. Embora não exista consenso em relação às indicações de cada técnica, a idade não parece representar um limite para as técnicas de partes moles: pacientes mais velhos podem ter resultados inferiores[34,50,55], mas verificase sempre benefício. Não se demonstrou um limite de deformidade óssea para o qual as técnicas de partes moles deixem de ter benefício, mas nas situações graves (= Waters V), é preferida a utilização de procedimentos ósseos. A técnica mais citada é a OTM de desrotação umeral externa, que apenas coloca o membro numa posição mais funcional, mas faltam estudos que esclareçam quais as melhores indicações de cada técnica: as OTM de RI, bem como o Tilt Triangular, parecem ter mais eficácia em doentes novos, onde tiram partido do potencial de remodelação ósseo. São estas técnicas que apresentam as maiores recuperações funcionais. A Glenoplastia permite bons ganhos de RE e uma excelente estabilidade gleno-umeral, embora tecnicamente exigente. A OTM de desrotação é uma técnica simples, que permite um ganho significativo de mobilidade e função, independentemente da idade e alterações ósseas. Ainda não se sabe qual a tendência destas técnicas para complicações tardias como artrose e dor, bem como perda de benefício, além da eventual vantagem de combinação destas técnicas com transferências tendinosas.
Remodelação Gleno-umeral:
A maior parte da evidência parece apontar para um efeito benéfico das cirurgias de partes moles, na remodelação e estabilidade gleno-umeral: 8 estudos[24,31,32,38,41,50,53,60] são concordantes no efeito benéfico destas técnicas, mostrando melhoria da retroversão da glenoide entre 9 e 21º, da PHHA entre 4 e 25%, bem como da congruência e morfologia (Quadro III). Apenas 2 estudos não observaram capacidade de reverter deformidades ósseas: Waters e Bae[62] referem que as cirurgias de partes moles têm, pelo menos, a capacidade de terminar as alterações displásicas, sendo a melhoria marginal verificada o resultado eventual da maturação esquelética normal; enquanto Kozin et al[39], num estudo com 23 doentes de idade média na data da cirurgia de 5,1 anos e com um ano de seguimento, não mostrou alteração da morfologia óssea. Para estes resultados podem ter contribuído a idade avançada dos pacientes e um tempo curto de follow-up.
Dos procedimentos ósseos apenas a OTM de desrotação umeral externa não demonstrou capacidade para alterar a configuração óssea, uma vez que não tem efeito a nível articular. Tanto a Glenoplastia[33], como o tilt triangular[45] ou a OTM de RI[58,59] apresentam resultados positivos na morfologia e congruência articular, embora sejam escassos os dados que suportam estas afirmações.
Fatores que condicionam o prognóstico
Não há consenso sobre a influência da idade[37] nos outcomes dos pacientes: a favor da ausência de influência da idade, Pearl[20] refere que as transferências tendinosas podem ter benefício mesmo após os 9/10 anos na ausência de alterações ósseas e incongruência gleno-umeral; Hui concluiu que a idade não altera o outcome num estudo com idades médias dos pacientes de 2,5 anos; e Newman[49] não encontrou diferenças significativas na mobilidade em grupos de diferentes idades. Outros autores apresentam diferenças de resultados com diferentes idades: Javid[35] com transferências tendinosas e Nath[46] com Tilt Triangular concluíram que são obtidos resultados superiores na remodelação se as cirurgias forem realizadas em idade precoce; El Gammal[34], Ozben[50] e Terzis[55] mostram benefícios em todas as idades, embora menores nos doentes com idades mais avançadas. Nesta revisão a análise por idade não foi possível devido a uma grande heterogeneidade das amostras dos estudos.
Poucos autores avaliaram a influencia do grau de lesão (Narakas) ou da mobilidade pré-operatória. Pagnotta[52] no seu estudo com 203 doentes encontrou melhores resultados nas lesões Narakas I e piores nos Narakas III /IV. Terzis[55] encontrou resultados similares - Narakas III/IV apenas recuperam em RE. Comparando os resultados dos estudos que incluíram apenas doentes com lesões parciais, Narakas I/II, com estudos que incluíram todos o espectro de lesões observamos resultados superiores no último grupo. No entanto, estes resultados parecem ser enviesados por amostras menores e aplicação de técnicas que obtêm resultados inferiores, como as libertações articulares simples, nos estudos unicamente com pacientes Narakas I/II. Ainda, o facto de não ser possível uma comparação direta de resultados entre lesões parciais e completas pode alterar significativamente os resultados.
Parece haver consenso que as transferências devem ser de músculos com força = M3 (MRC), mesmo que seja o resultado de uma cirurgia primária prévia. A maioria dos estudos incluiu doentes com algum tipo de cirurgia de reinervação/reparação do plexo braquial, e são estes que apresentam melhor mobilidade e Mallet global. É assim sugerido que a utilização de cirurgias primárias nos casos estão indicadas, poderá ser benéfica para a função final do membro.
]]> Em relação à morfologia e estabilidade glenoumeral foram encontrados resultados semelhantes: nos estudos onde foram incluídos apenas doentes com sem alterações ou alterações ligeiras (equivalente a Waters 2), ou ombros estavéis, observaram-se resultados superiores. Nenhum estudo com técnicas ósseas incluiu apenas doentes com alterações ligeiras ou ombros estáveis.Apenas 3 estudos[32,37,52] apresentaram resultados de seguimentos superiores a 10 anos de cirurgia. Todos utilizaram técnicas de partes moles e todos demonstram perda dos ganhos iniciais, especialmente da abdução, sendo que os ganhos de rotação externa se mantêm em algum grau. Entre os 5 e os 10 anos após cirurgia é que se observam os maiores ganhos, independentemente da técnica. Desconhece-se a razão para a perda tardia de função - Kirkos[37] refere uma eventual relação com a degeneração do músculo devido à tensão da tenodese e compressão pela musculatura adjacente na nova posição, enquanto Pagnotta[52] refere que o abandono da reabilitação e desuso do membro afetado na altura da adolescência poderão ser as causas da diminuição dos resultados.
CONCLUSÃO
Implicações para a prática clínica
As cirurgias paliativas para tratamento de sequelas de LOPB no ombro estão bem documentadas e difundidas a nível internacional. Todas a técnicas têm capacidade para aumentar as mobilidades ativas e a função do membro superior, sendo a complicação mais frequente uma perda de mobilidade em RI, habitualmente sem impacto funcional. Não há ainda um consenso claro sobre as indicações, sendo que as libertações articulares são importantes precocemente para manter a congruência e melhorar a morfologia articular, as transferências tendinosas têm um benefício em quase todos os doentes, independentemente da idade e alterações ósseas, podendo mesmo utilizarse de forma combinada com procedimentos ósseos, embora haja evidência da perda de efeito 10 anos após a cirurgia. As cirurgias ósseas, geralmente consideradas procedimentos de salvação em alterações displásicas graves e idades avançadas, têm agora técnicas que parecem ser benéficas quando aplicadas cedo, como o tilt triangular ou a OTM de RI, embora a evidência seja muito limitada.
Implicações para a investigação futura:
Os resultados desta revisão sistemática revelam a necessidade de mais investigação para que possam ser determinados protocolos assertivos de atuação, em relação aos critérios e timing cirúrgicos. Para alcançar estes objetivos é necessário a realização de estudos comparativos prospetivos, com tempos de seguimento elevados para se concluir quais as técnicas mais eficazes e a causa da diminuição dos ganhos. Estas considerações podem ser de difícil aplicação pela baixa frequência e elevada heterogeneidade da população em causa. No entanto, devem-se desenvolver diferentes subgrupos pelas variáveis que podem influenciar o prognóstico e que aqui foram apresentadas. Os benefícios de desenhar estudos rigorosos e de alta qualidade ultrapassam largamente as dificuldades, pelo potencial que têm de fornecer os cuidados mais adequados às crianças com LOPB melhorando assim a sua qualidade de vida.
REFERÊNCIAS BIBLIOGRÁFICAS
]]>1. Greenwald AG, Shute PC, Shiveley JL. Brachial plexus palsy: a 10 year report on the incidence and prognosis. J Pediatr Orthop. 1984; 4: 689-692 [ Links ]
2. Hardy AE. Birth injuries of the brachial plexus: incidence and prognosis. J Bone Joint Surg Br. 1981; 63: 98-101 [ Links ]
3. Levine MG, Holroyde J, Woods JR Jr. Birthtrauma: incidence and predisposing factors. Obstet Gynecol. 1984; 63: 792-795 [ Links ]
4. Kay SP. Obstetrical brachial palsy. Br J Plast Surg. 1998; 51: 43-50 [ Links ]
5. Beischer AD, Simmons TD, Torode IP. Glenoid version in children with obstetric brachial plexus palsy. J Pediatr Orthop. 1999; 19: 359-361 [ Links ]
6. Brandt KE, Mackinnon SE. A technique for maximizing biceps recovery in brachial plexus reconstruction. J Hand Surg Am. 1993; 18: 726-733 [ Links ]
7. Narakas AO. Injuries to the brachial plexus. In Bora FW, editors. Diagnosis and Management. Philadelphia: WB Saunders; 1986. p. 247.
8. Gilbert A, Razaboni R, Amar-Khodja S. Indications and results of brachial plexus surgery in obstetric palsy. Orthop Clin North Am. 1988; 19: 91-105 [ Links ]
9. Al-Qattan MM. The outcome of Erb?s palsy when the decision to operate is made at 4 months of age. Plast Reconstr Surg. 2000; 106: 1461-1465 [ Links ]
10. Michelow B, Clarke HM, Curtis CG. The natural history of obstetrical brachial plexus palsy. Plast Reconstr Surg. 1994; 93: 675-680 [ Links ]
11. Zancolli EA, Zancolli ER. Palliative surgical procedures in sequelae of obstetrical palsy. Hand Clin. 1988; 4: 643-669 [ Links ]
12. Laurent JP, Lee R, Shenag S. Neurosurgical correction of the upper brachial plexus birth injuries. J Neurosurg. 1993; 79: 197-203 [ Links ]
13. Nehme A, Kany J, Gauzy JS DE. Obstetrical brachial plexus palsy. Prediction of outcome in upper root injuries. J Hand Surg. 2002; 278: 9-12 [ Links ]
14. Chuang DCC, Ma HS, Wei FC. A new evaluation system to predict the sequelae of late obstetric brachial plexus palsy. Plast Reconstr Surg. 1998; 101: 673-685 [ Links ]
15. Waters PM. Update on Management of Pediatric Brachial Plexus Palsy. J Pediatr Orthop. 2005; 25: 116-126 [ Links ]
16. van der Sluijs JA, van Ouwerkerk WJ, Gast A de, Wuisman PI, Nollet F, Manoliu RA. Deformities of the shoulder in infants younger than 12 months with an obstetric lesion of the brachial plexus. J Bone Joint Surg Br. 2001; 83: 551-555 [ Links ]
17. Waters PM. Glenohumeral Deformity Secondary to Brachial Plexus Birth Palsy. J Bone Joint Surg Am. 1998 May; 80-A (5)
18. How to Use the Evidence: Assessment and Application of Scientific Evidence. National Health and Medical Research Council; Canberra: National Health and Medical Research Council; 2000.
19. Mallet J. Paralysie obstetrical du plexus brachial. Traitement des sequelles. Primaute du traitment de l'epaule -methode d'expression des resultats. Rev Chir Orthop. 1972; 58 (1): 166-170 [ Links ]
20. Pearl ML, Edgerton BW. Glenoid deformity secondary to brachial plexus birth palsy. J Bone Joint Surg Am. 1998; 80: 659-667 [ Links ]
21. Law M, Stewart D, Pollock N, Letts L, Bosch J, Westmorland M. Critical Review Form - Quantitative Studies (McMaster University). 1998; [ Links ]
22. Abdel-Ghani H, Hamdy KA, Basha N, Tarraf YN. Tendon transfer for treatment of internal rotation contracture of the shoulder in brachial plexus birth palsy. J Hand Surg Eur. 2012; 37: 781 [ Links ]
23. Abdelaziz TH, Samir S, Magdy W. Restoring shoulder abduction in children with Erb's palsy - When to add trapezius transfer to a teres major transfer. J Bone Joint Surg Br. 2012 Nov; 94-b (11)
24. Abid A, Accadbled F, Louis D, Kany J, Knorr J, Cahuzac JP, et al. Arthroscopic release for shoulder internal rotation contracture secondary to brachial plexus birth palsy: clinical and magnetic resonance imaging results on glenohumeral dysplasia. J Pediatr Orthop. 2012; 21: 305-309
25. Abzug JM, Chafetz RS, Gaughan JP, Ashworth S, Kozin SH. Shoulder Function After Medial Approach and Derotational Humeral Osteotomy in Patients With Brachial Plexus Birth Palsy. J Pediatr Orthop. 2010; 30: 469-474 [ Links ]
26. Al-Qattan MM. Latissimus Dorsi Transfer for External Rotation Weakness of the Shoulder in Obstetric Brachial Plexus Palsy. J Hand Surg Br & Eur. 2003; 28b (5): 487-490 [ Links ]
27. Armangil M, Akan B, Kerem B, Bilgin SS, Gurcan S, Demirtas M. Arthroscopic release of the subscapularis for shoulder contracture of obstetric palsy. Eur J Orthop Surg Traumatol. 2012; 22: 25-28 [ Links ]
28. Aydin A, Ozkan T, Onel D. Does preoperative abduction value affect functional outcome of combined muscle transfer and release procedures in obstetrical palsy patients with shoulder involvement?. BMC Musculoskeletal Disorders. 2004; 5: 25 [ Links ]
29. Aydin A, Biçer A, Ozkan T, Mersa B, Ozkan S, Yildirim ZH. Does primary brachial plexus surgery alter palliative tendon transfer surgery outcomes in children with obstetric paralysis?. BMC Musculoskeletal Disorders. 2011; 12: 74 [ Links ]
30. Bertelli JA. Lengthening of the subscapularis and transfer of the lower trapezius in the correction of recurrent internal rotation contracture following obstetric brachial plexus palsy. J Bone Joint Surg Br. 2009 Jul; 91b (7): 943-948
31. Breton A, Mainard L, Gaspéri M, Barbary S, Maurice E, Dautel G. Arthroscopic release of shoulder contracture secondary to obstetric brachial plexus palsy: Retrospective study of 18 children with an average follow-up of 4.5 years. Orthop Traumatol Surg Res. 2012; 98: 638-644 [ Links ]
32. Cohen G, Rampal V, Aubart-Cohen F, Seringe R, Wicart P. Brachial plexus birth palsy shoulder deformity treatment using subscapularis release combined to tendons transfer. Orthop Traumatol Surg Res. 2010; 96: 334-339 [ Links ]
33. Dodwell E, O'Callaghan J, Anthony A, Jellicoe P, Shah M, Curtis C, et al. Combined Glenoid Anteversion Osteotomy and Tendon Transfers for Brachial Plexus Birth Palsy - Early Outcomes. J Bone Joint Surg Am. 2012; 94: 2145-2152
34. El-Gammal TA, Saleh WR, El-Sayed A, Kotb MM, Imam HM, Fathi NA. Tendon Transfer Around the Shoulder in Obstetric Brachial Plexus Paralysis: Clinical and Computed Tomographic Study. J Pediatr Orthop. 2006; 26 (5): 641-646 [ Links ]
35. Javid M, Shahcheraghi GH. Shoulder reconstruction in obstetric brachial plexus palsy in older children via a one-stage release and tendon transfers. J Shoulder Elbow Surg. 2009; 18: 107-113 [ Links ]
36. Kambhampati SB, Birch R, Cobiella C, Chen L. Posterior subluxation and dislocation of the shoulder in obstetric brachial plexus palsy. J Bone Joint Surg. 2006 Fev; 88-B: 213-219
37. Kirkos JM, Kyrkos MJ, Kapetanos GA, Haritidis JH. Brachial plexus palsy secondary to birth injuries - Long-term results of anterior release and tendon transfers around the shoulder. J Bone Joint Surg Br. 2005 Fev; 87-B (2): 231-235
38. Kozin SH, Boardman MJ, Chafetz RS, Williams GR, Hanlon A. Arthroscopic treatment of internal rotation contracture and glenohumeral dysplasia in children with brachial plexus birth palsy. J Shoulder Elbow Surg. 2010; 19: 102-110 [ Links ]
39. Kozin SH, Chafetz RS, Barus D, Filipone L. Magnetic resonance imaging and clinical findings before and after tendon transfers about the shoulder in children with residual brachial plexus birth palsy. J Shoulder Elbow Surg. 2006; 15 (5): 554-561 [ Links ]
40. Mascio L Di, Chin KF, Fox M, Sinisi M. Glenoplasty for complex shoulder subluxation and dislocation in children with obstetric brachial plexus palsy. J Bone Joint Surg Br. 2011; 93-B: 102-107 [ Links ]
41. Mehlman CT, DeVoe WB, Lippert WC, Michaud LJ, Allgier AJ, Foad SL. Arthroscopically Assisted Sever-L'Episcopo Procedure Improves Clinical and Radiographic Outcomes in Neonatal Brachial Plexus Palsy Patients. J Pediatr Orthop. 2011; 31: 341-351 [ Links ]
42. Nath RK, Lyons AB, Melcher SE, Paizi M. Surgical correction of the medial rotation contracture in obstetric brachial plexus palsy. J Bone Joint Surg Br. 2007; 89-B: 1638-1644 [ Links ]
43. Nath RK, Karicherla P, Mahmooduddin F. Shoulder function and anatomy in complete obstetric brachial plexus palsy: longterm improvement after triangle tilt surgery. Childs Nerv Syst. 2010; 26: 1009-1019 [ Links ]
44. Nath RK, Liu X, Melcher SE, Fan J. Long-term outcomes of triangle tilt surgery for obstetric brachial plexus injury. Pediatr Surg Int. 2010; 26: 393-399 [ Links ]
45. Nath RK, Paizi M. Improvement in abduction of the shoulder after reconstructive soft-tissue procedures in obstetric brachial plexus palsy. J Bone Joint Surg Br. 2007; 89-B: 620-626 [ Links ]
46. Nath RK, Somasundaram C, Mahmooduddin F. Comparing Functional Outcome of Triangle Tilt Surgery Performed Before Versus After Two Years of Age. Open Orthop J. 2011; 5: 59-62 [ Links ]
47. Nath RK, Mahmooduddin F. Triangle Tilt Surgery: Effect on Coracohumeral Distance and External Rotation of the Glenohumeral Joint. Open Acess J Plastic Surg. 2010 Nov; 560-567
48. Nath RK, Somasundaram C, Melcher SE, Bala M, Wentz MJ. Arm rotated medially with supination - the ARMS variant: description of its surgical correction. BMC Musculoskeletal Disorders. 2009; 10: 32 [ Links ]
49. Newman CJ, Morrison L, Lynch B, Hynes D. Outcome of Subscapularis Muscle Release for Shoulder Contracture Secondary to Brachial Plexus Palsy at Birth. J Pediatr Orthop. 2006; 26: 647-651 [ Links ]
50. Ozben H, Atalar AC, Bilsel K, Demirhan M. Transfer of latissmus dorsi and teres major tendons without subscapularis release for the treatment of obstetrical brachial plexus palsy sequela. J Shoulder Elbow Surg. 2011; 20: 1265-1274 [ Links ]
51. Özturk K, Bulbul M, Demir BB, Buyukkurt CD, Ayanoglu S, Esenyel CZ. Reconstruction of shoulder abduction and external rotation with latissimus dorsi and teres major transfer in obstetric brachial plexus palsy. Acta Orthop Traumatol Turc. 2010; 44 (3): 186-193 [ Links ]
52. Pagnotta A, Haerle M, Gilbert A. Long-term Results on Abduction and External Rotation of the Shoulder after Latissimus Dorsi Transfer for Sequelae of Obstetric Palsy. Clin Orthop Relat Res. 2004; 426: 199-205 [ Links ]
53. Pearl ML, Edgerton BW, Kazimiroff PA, Burchette RJ, Wong K. Arthroscopic Release and Latissimus Dorsi Transfer for Shoulder Internal Rotation Contractures and Glenohumeral Deformity Secondary to Brachial Plexus Birth Palsy. J Bone Joint Surg Am. 2006 Mar; 88-A (3): 564-574
54. Sibinski M, Synder M. Soft tissue rebalancing procedures with and without internal rotation osteotomy for shoulder deformity in children with persistent obstetric brachial plexus palsy. Arch Orthop Trauma Surg. 2010; 130: 1499-1504 [ Links ]
55. Terzis JK, Kokkalis ZT. Outcomes of Secondary Shoulder Reconstruction in Obstetrical Brachial Plexus Palsy. Plast Reconstr Surg. 2008 Dec; 122 (6): 1812-1822
56. Thatte MR, Agashe MV, Rao A, Rathod CM, Metha R. Clinical outcome of shoulder muscle transfer for shoulder deformities in obstetric brachial plexus palsy: a study of 150 cases. Indian J Plast Surg. 2011; 44 (1): 21-28 [ Links ]
57. van der Sluijs JA, Van Ouwerkerkb WJ, Gasta A DE, Nolletc F, Wintersd H, Wuismana P. Treatment of internal rotation contracture of the shoulder in obstetric brachial plexus lesions by subscapular tendon lengthening and open reduction: early results and complications. J Pediatr Orthop B. 2004; 13: 218-224 [ Links ]
58. Vieira LA, Poderoso MA, Gonçalves MC, Hissadomi MI, Benegas E, Neto AA, et al. Humeral head centering osteotomy for posterior shoulder dislocation due to obstetric palsy. Rev Bras Ortop. 39; 39: 661-669
59. Vilaça Jr PA, Uezumib MK, Filho A Zoppi. Centering osteotomy for treatment of posterior shoulder dislocation in obstetrical palsy. Orthop Traumatol Surg Res. 2012; 98: 199-205 [ Links ]
60. Waters PM, Bae DS. The Early Effects of Tendon Transfers and Open Capsulorrhaphy on Glenohumeral Deformity in Brachial Plexus Birth Palsy. J Bone Joint Surg Am. 2008; 90: 2171-2179 [ Links ]
61. Waters PM, Bae DS. The Effect of Derotational Humeral Osteotomy on Global Shoulder Function in Brachial Plexus Birth Palsy. J Bone Joint Surg Am. 2006; 88-A (5): 1035-1042 [ Links ]
62. Waters PM, Bae DS. Effect of Tendon Transfers and Extra-Articular Soft-Tissue Balancing on Glenohumeral Development in Brachial Plexus Birth Palsy. J Bone Joint Surg Am. 2005; 87-A (2): 320-325 [ Links ]
63. Özkan T, Aydin A, Önel D, Özkan S. Reconstruction of shoulder abduction and external rotation in obstetric brachial plexus palsy. Acta Orthop Traumatol Turc. 2004; 38 (3): 161-169 [ Links ]
Conflito de interesse:
Nada a declarar.
João Vide ]]>
Urb. Parque das Amoreiras, Lt 8/9
Bloco A, 8ºD
8500-546 Faro
Portugal
joaovide@gmail.com
Data de Submissão: 2013-08-27
Data de Revisão: 2013-11-26
Data de Aceitação: 2013-11-26
]]>