Necrose muscular paravertebral pós-cirúrgica
Bárbara CamposI; José Guimarães ConsciênciaI
I. Serviço de Ortopedia e Traumatologia. Centro Hospitalar de Lisboa Ocidental, E. P. E.Lisboa. Portugal.
RESUMO
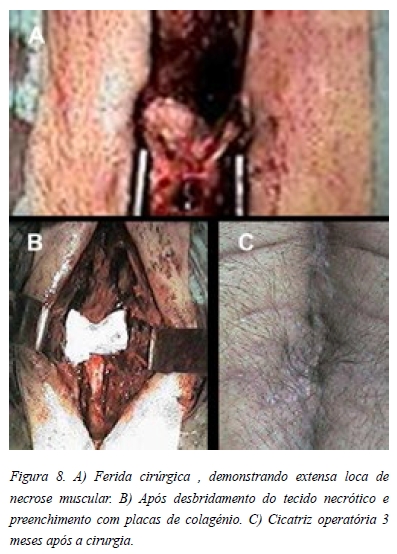
]]> Os autores apresentam dois casos clínicos, ambos do sexo masculino, de doentes com patologia degenerativa vertebral, com antecedentes pessoais médicos relevantes (diabetes, hiperlipidémia, Hipertensão ou policitémia), submetidos a uma abordagem posterior da sua coluna lombar, para tratamento cirúrgico no posicionamento de decúbito ventral.No período pós-operatório ambos os doentes desenvolveram alterações da cicatrização da ferida cirúrgica, posteriormente associadas a extensa necrose muscular paravertebral, devidamente documentada.
São discutidas as formas de tratamento e o envolvimento das patologias associadas, salientando a importância da prevenção cuidadosa desta complicação menos frequente.
Palavras chave: Necrose muscular, paravertebral, cirurgia da coluna lombar.
ABSTRACT
The authors present two case reports, both man, with lumbar degenerative disc disease and a positive personal medical history for diabetes, dyslipidemia, hypertension or polycythemia. They undergone a posterior approach to their lumbar spine, in a ventral decubitus position, for surgical treatment of the diagnosed disease.
In the post operative period both patients developed a wound dehiscence and seroma drainage related to an underlying muscular necrosis properly documented.
The treatment performed is discussed, along with the implicated medical diseases, stressing out the relevance of preventing measures in avoiding this less frequent complication.
Key words: Muscular necrosis, paravertebral, lumbar spine surgery.
]]>INTRODUÇÃO
Os músculos paravertebrais estão sujeitos a forças distractivas durante a abordagem posterior da coluna lombar1.
Sabe-se que a retração muscular necessária para a exposição das estruturas ósseas provoca, em termos histológicos, edema intersticial, acumulação intracelular de iões de Cálcio (Ca2+) no sarcolema, e finalmente necrose celular2.
O espectro de manifestações clínicas desta entidade patológica é variável, mas, depende habitualmente da gravidade da lesão nos músculos sacroespinalis e erector spinae. A variabilidade do quadro clínico oscila entre o doente com dor lombar, diminuição da força de extensão do tronco, e aquele que, tendo necrose muscular extensa, revela alterações graves da cicatrização normalmente associadas a uma panóplia de morbilidades. Várias publicações referem a possibilidade de documentação desta lesão através de estudos complementares de diagnóstico3, 4, 5, 6.
Apesar do traumatismo directo muscular ser a causa mais comum de necrose muscular, muitos outros factores foram identificados e a ela associados, como por exemplo a obesidade, a diabetes, a poliglobulia, ou até mesmo um posicionamento inadequado. No entanto, as lesões microvasculares e as alterações metabólicas relacionadas com a pressão exercida pelo garrote são bem conhecidas. Estudos histoquímicos, animais e humanos, que corelacionaram a pressão e o tempo da retração aplicada nos músculos paravertebrais, identificaram um valor superior a 10.000 g/cm2/min como sendo factor de risco elevado para o aparecimento de necrose muscular histológica, e, naturalmente também associado a piores resultados funcionais pós operatórios1, 2, 7, 8, 9. Existem também referências na literatura à associação entre piores resultados funcionais e lesões neuromusculares na sequência de extensas abordagens posteriores da coluna lombar, o que reforça a importância da sua prevenção10.
Com base neste pressuposto, Kawaguchi et al7 estudaram a necessidade de alívio da pressão exercida nos músculos paravertebrais, e concluíram que no decorrer de uma cirurgia com duração entre 40 min a 1 hora, a interrupção durante 5 min da acção dos afastadores, constituía medida eficaz na prevenção da necrose muscular.
CASO CLÍNICO 1
Paciente do sexo masculino, com 79 anos de idade, IMC 29, e antecedentes pessoais de hemilaminectomia esquerda há 10 anos, Diabetes Mellitus tipo II e Hipertensão arterial, ambas medicadas. Recorre à consulta de coluna por lombalgia com irradiação ao membro inferior direito, e marcha claudicante neurogénica.
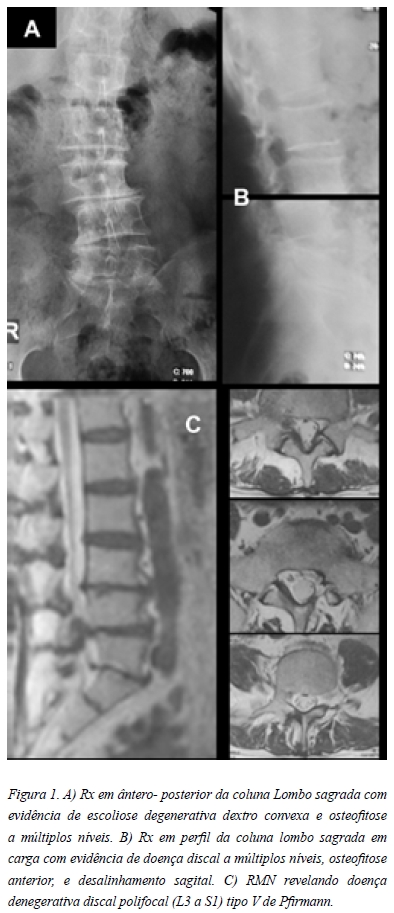
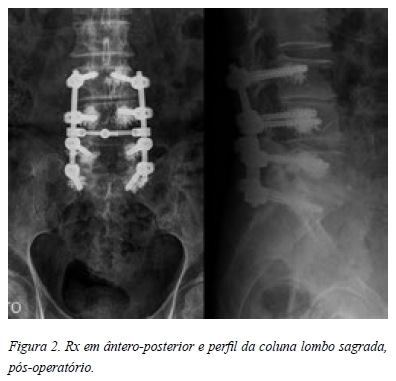
Apresentava uma doença degenerativa discal polifocal (L3-S1) tipo V de Pfirmann, com estenose canalar central/ lateral, escoliose degenerativa e atrofia muscular (Figura 1).

CASO CLÍNICO 2
Paciente do sexo masculino, com 68 anos de idade, IMC 27, e antecedentes pessoais de Policitémia vera ( HB 19g/dl), Hipertensão arterial e Hiperlipidémia medicada com Sinvastatina. Recorre à consulta de coluna por lombalgia de carácter renitente, e evolução arrastada de aproximadamente 5 anos.
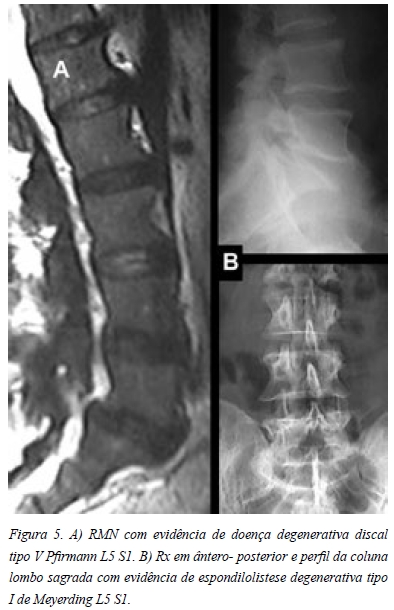
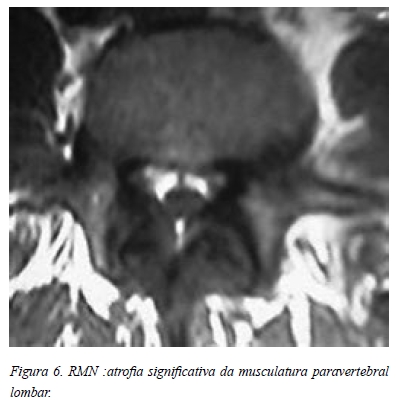
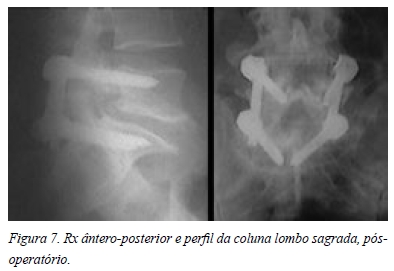
Apresentava uma doença degenerativa discal L5-S1 tipo V de Pfirmann e uma espondilolistese degenerativa tipo I de Meyerding (Figura 5) no mesmo nível. Era ainda evidente uma atrofia muscular lombar generalizada (Figura 6).
]]> DISCUSSÃO
A cicatrização tecidual é um processo biológico complexo que requer uma sucessão coordenada de hemóstase, inflamação, proliferação, revascularização e remodelação.
As alterações no processo de cicatrização constituem um problema comum no âmbito hospitalar e ambulatório.
Dentro dos vários factores que influenciam este processo biológico existem alguns, como a técnica cirúrgica, que são passíveis de ser controlados pelo cirurgião.
O posicionamento adequado do doente, bem como a dissecção cuidadosa são factores bem conhecidos e que devem ser sempre respeitados. Na cirurgia de coluna em particular, a abordagem para vertebral de Wiltse, utilizando um plano natural de clivagem existente entre o multifidus e o longissimus (sacroespinalis), permite o acesso às apófises transversas e maciços articulares através duma dissecção quase atraumática. No entanto, esta abordagem nem sempre se torna possível considerando a necessidade de descompressão central alargada e re-intervenção.
A técnica MISS (minimally invasive surgery), foi desenvolvida na tentativa de minimizar a morbilidade associada à cirurgia aberta. As vantagens demonstradas em estudos clínicos incluem redução do tecido cicatricial e da dor, bem como menor tempo de recuperação no pós-operatório. Mais ainda, demonstrou-se que utilizando técnicas minimamente invasivas, as enzimas relacionadas com a lesão muscular (CK e aldolase), bem como as citoquinas pró inflamatórias (IL-6, IL-8), atingiam níveis bastante inferiores aos obtidos durante a cirurgia convencional.
Apesar destas vantagens, é uma técnica com curva de aprendizagem relativamente longa, e que, por razões anatómicas e especificas de cada caso clinico não pode ser sistematicamente utilizada.
Na abordagem mediana da coluna, as lesões microvasculares e necrose subsequente parecem poder ser em parte evitadas pela diminuição do tempo de aplicação da força exercida pelo afastador. Assim, a abertura desse mesmo afastador durante 5 minutos a cada 40 minutos de cirurgia tem sido sugerida como medida eficaz na prevenção de lesão da musculatura paravertebral, e constitui procedimento de rotina no nosso serviço1,2,7,8,9,11.
Por outro lado, existem também fatores determinantes mas relacionados com a situação médica do próprio doente. Nos casos apresentados a idade avançada, IMC elevado, Diabetes Mellitus, Hipertensão arterial, Poliglobulia, Hiperlipidémia e até a medicação (estatina) poderão ter tido um papel preponderante na instalação da lesão muscular.
A este propósito importa salientar a Diabetes, uma doença sistémica com diversas complicações associadas e bem documentadas, nomeadamente a alteração da cicatrização. Na base desta, e para além das lesões microvasculares, está a própria alteração do metabolismo da glicose. Estudos experimentais demonstraram que a ferida do doente diabético revela um fenótipo pró inflamatório com consequências importantes no processo de cicatrização. Em acréscimo, e do ponto de vista biomecânico, a inflamação induz uma degradação da matriz extracelular, com invasão de células produtoras deste tecido. Por outro lado, o TNF ( Tumor Necrosis Factor) activa genes pró apoptose, perpétua esta inflamação, e impede a correcta re-epitelização do tecido. No despoletar de todo este processo de pró inflamação está então a hiperglicémia, como activador de proteínas de fase aguda, e elevação de radicais livres de oxigénio e nitrogénio.
]]> O doente diabético é, portanto, um doente com risco elevado de cicatrização inadequada e consequentemente favorecedora de maus resultados cirúrgicos. Porém, estes estão não só relacionados com a alteração de cicatrização da ferida cirúrgica mas também com as restantes complicações inerentes à diabetes (nefropatia, aterosclerose e neuropatia), e até mesmo a eventual infecção.A Policitémia, com a inerente poliglobulia, constitui um fator de aumento da viscosidade sanguínea e diminuição da correcta oxigenação dos tecidos.
Estão descritos eventos trombóticos em cerca de 20 a 50% nos doentes com esta doença, envolvendo não só a microcirculação mas também os grandes vasos.
As úlceras relacionadas com o comprometimento da microcirculação dos membros inferiores são as mais frequentes, sendo normalmente dolorosas, inflamatórias e necróticas.
Embora o doente em questão fosse seguido na consulta de Hematologia e a sua patologia estivesse controlada, é possível que na base da deiscência da ferida cirúrgica se registem cumulativamente mecanismos relacionados com a referida microtrombose e consequente necrose tecidular.
A idade avançada e hipertensão arterial, ambas relacionadas com o processo de aterosclerose hialina, afectam a microcirculação sanguínea, e desse modo correcta vascularização e cicatrização tecidual12.
Mais ainda, a hipertensão arterial como factor condicionante de alterações da perfusão sanguínea da pele e resposta à isquémia, sendo objecto de estudos recentes, animais e humanos, parece estar associada a alterações tanto nos indivíduos hipertensos como nos que apenas revelam uma certa predisposição familiar13,14.
As Estatinas, utilizadas para o controlo da Hiperlipidémia estão amplamente instituída na população em geral e são habitualmente bem toleradas. São usadas na prevenção da aterosclerose e doença cardíaca isquémica e têm sido reconhecidas como potencial factor de agravamento da rabdomiólise, e até possivelmente da necrose muscular. Têm sido associadas a uma variedade de miopatias inflamatórias, incluindo polimiosite, dermatomisite e miopatia necrosante15.
Por outro lado, dados publicados em estudos animais e humanos, mostram que este grupo de fármacos, em particular a atorvastatina e pravastatina podem acelerar o processo de cicatrização da pele. No entanto são ainda necessários mais estudos clínicos randomizados para definir dose, modo de administração, duração de tratamento e, em última análise determinar a correlação entre os efeitos pleotrópicos das estatinas e o seu efeito clínico previsível15-19.
Estas incertezas fazem-nos pensar que, no caso em questão, permanece a dúvida da relação desta mediação com a necrose muscular diagnosticada.
]]> Sumarizando, a micro irculação da pele é controlada por uma combinação de factores metabólicos como: óxido nítrico (produzido em resposta à tensão de cisalhamento nas células endoteliais); actividade do músculo liso vascular (proporcional ás necessidades de oxigénio do tecido); flutuações nas concentrações iónicas (através da membrana das células do músculo liso dos vasos)20,21,22. Qualquer mecanismo, para além dos acima mencionados, que perturbe este equilíbrio pode, eventualmente, também alterar a correcta oxigenação dos tecidos e consequentemente a sua cicatrização.
CONCLUSÃO
A aplicação rigorosa das técnicas de preservação da oxigenação tecidular constitui uma medida indispensável da abordagem cirúrgica da coluna vertebral.
Por outro lado, o despiste criterioso e exaustivo de todos os factores de risco para necrose muscular, pode e deve orientar o cirurgião na tomada de medidas adicionais necessárias a cada situação clínica.
Consideramos ainda que o controlo prévio rigoroso e sistemático de toda a medicação e patologia se assume como primeiro passo na prevenção desta complicação.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Kawaguchi Y. Back Muscle Injury after posterior lumbar spine surgery Part I. Spine. 1994; 19 [ Links ]
2. Kawaguchi Y. Back Muscle Injury after posterior lumbar spine surgery Part II. Spine. 1994; 19 [ Links ]
3. Laasonen EM. Atrophy of sacrospinal muscle groups in patients with chronic, diffusely radiating lumbar back pain. Neuroradiology. 1984; 26: 9-13 [ Links ]
4. Mayer TG, Vanharanta H, Gatchel RJ, Mooney V, Barnes D, Juddge L, et al. Comparison of CT scan muscle measurements and isokinetic trunk strength in postoperative patients. Spine. 1989; 14: 33-36
5. Johnson EW, Burkhart JA, Earl WC. Electromyography in postlaminectomy patients. Arch Phys Med Rehabil. 1972; 53: 407-409 [ Links ]
6. Macnab I, Cuthbert H, Godfrey CM. The incidence of denervation of the sacrospinalis muscles following spinal surgery. Spine. 1977; 2: 294-298 [ Links ]
7. Kawaguchi Y. Preventive measures of back muscle injury after posterior lumbar spine surgery in rats. Spine. 1998; 23 [ Links ]
8. Kawaguchi Y. Back Muscle Injury after posterior lumbar spine surgery. A histologic and enzymatic analysis. Spine. 1996; 21 [ Links ]
9. Kawaguchi Y. Back muscle injury after posterior lumbar spine surgery. Topographic evaluation of intramuscular pressure and blood flow in the porcine back muscle during surgery. Spine. 1996; 21 [ Links ]
10. Airaksinen O, Herno A, Kaukanen E, Saari T, Sihvonen T, Suomalainen O. Density of lumbar muscles 4 years after decompressive spinal surgery. Eur Spine J. 1996; 5 (3): 193-197 [ Links ]
11. Smilanich RP, Bonnet I, Kirkpatrick JR. Contaminated wounds: the effect of initial management on outcome. Am Surg. 1995; 61: 427-430 [ Links ]
12. Kumar V. Robbins and Cotran Pathologic Basis of Disease. 8th. Professional Edition; [ Links ]
13. Gryglewska B. Neurogenic and myogenic resting skin blood flowmotion in subjects with masked hypertension. J Physiol Pharmacol. 2010 Oct 1; 61 (5): 551-558
14. Gryglewska B. Fractal dimensions of skin microcirculation flow in subjects with familial predisposition or newly diagnosed hypertension. Cardiol J. 2011; 18 (1): 26-32 [ Links ]
15. Cooper A. Clinical guidelines and evidence review for lipid modification: cardiovascular risk assessment and the primary and secondary prevention of cardiovascular disease. National Collaborating Centre for Primary Care and Royal College of General Practitioners. National Institute of Clinical Excellence Guidance. 2008; [ Links ]
16. Schneider Philip J.. Will cholesterol lowering therapy increase the risk of muscle injury?. The journal for Nurse Practicioners JNP. 2013 Fev; 9
17. Bruckert E, Hayem G, Dejager S. Mild to moderate muscular symptoms with high-dosage statin therapy in hyperlipidemic patients: the PRIMO study. Cardiovasc Drugs Ther. 2005; 19: 403-414 [ Links ]
18. Graham DJ, Staffa JA, Shatin D. Incidence of hospitalized rhabdomyolysis in patients treated with lipid-lowering drugs. JAMA. 2004; 292: 2582-2590 [ Links ]
19. Krishnan GM, Thompson PD. The effects of statins on skeletal muscle strength and exercise performance. Curr Opin Lipidol. 2010; 21: 324-328 [ Links ]
20. Nilsson H, Aalkjaer C. Vasomotion: Mechanisms and physiological importance. Mol Interv. 2003; 3: 79-89 [ Links ]
21. Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985; 28: 412-419 [ Links ]
22. Lamboley M, Schuster A, Bény JL, Meister JJ. Recruitment of smooth muscle cells and arterial vasomotion. Am J Physiol Heart Circ Physiol. 2003; 285: 562-569 [ Links ]
Bárbara Campos
Serviço de Ortopedia e Traumatologia
Centro Hospitalar de Lisboa Ocidental
Estrada Forte do Alto Duque
1449-005 Lisboa ]]>
Portugal
babinha2001@hotmail.com
Data de Submissão: 2013-11-18
Data de Revisão: 2014-03-03
Data de Aceitação: 2014-03-03
]]>