Sinovite vilonodular pigmentada localizada
Eunice CarvalhoI; Luís SilvaI; Bruno MaiaI; Eduardo FerreiraI; Jorge CorreiaI
I. Serviço de Ortopedia. Unidade Local de Saúde da Guarda. Guarda. Portugal.
RESUMO
]]> A Sinovite Vilonodular Pigmentada (SVNP) é uma doença proliferativa da membrana sinovial, rara (estima-se uma incidência anual de 1.8 casos per million people (pmp) 8) e que geralmente afeta adultos jovens. Na maioria dos casos a doença é unilateral e envolve grandes articulações, sendo que em 80% dos casos reportados ocorre no joelho3. Pode manifestar-se sob a forma de doença localizada, Sinovite Vilonodular Pigmentada Localizada (SVNPL), ou difusa, Sinovite Vilonodular Pigmentada Difusa (SVNPD). A forma localizada é mais rara (25%3) e caracteriza-se pelo envolvimento focal da sinovial, podendo assumir uma forma nodular ou pediculada. Tem excelente prognóstico e baixa taxa de recidiva após a excisão. A forma difusa afeta virtualmente toda a sinovial e é localmente agressiva.Palavras chave: joelho, sinovite vilonodular pigmentada, forma localizada, tratamento.
ABSTRACT
Pigmented Villonodular Synovitis (PVNS) is a proliferative disorder of the synovium. It is rare (estimated an annual incidence of 1.8 cases per million people (pmp)8) and usually affects young adults. Most cases are unilateral and occur in large joints, with 80 % of reported cases affecting the knee3. May occur in localized form, Localized Pigmented Villonodular Synovitis (LPVNS), or diffuse, Diffuse Pigmented Villonodular Synovitis (DPVNS). The localized form is rare (25%3) and is characterized by focal involvement of the synovial, with either nodular or pedunculated masses and has an excellent prognosis and low rate of recurrence after excision. The diffuse form affects virtually all synovial and is locally aggressive.
The authors report a case of a female patient with a LPVNS knee injury. She underwent arthrotomy and excision of the lesion, with good clinical outcome, and remained asymptomatic after a 2 years follow-up. The authors wish to point out with this case that, although rare, LPVNS is a diagnosis to be considered in young patients with knee pain.
Key words: knee, pigmented villonodular synovitis, localized form, treatment outcome.
INTRODUÇÃO
A SVNP e os tumores de células gigantes das bainhas tendinosas (TCGBT) são doenças do mesmo espectro, com várias semelhanças histopatológicas. Ocorrem geralmente em adultos jovens, podendo também surgir em crianças e adolescentes2. Os sintomas são inespecíficos. A incidência anual estimada de TCGBT é de 9.2 casos pmp e de 1.8 pmp casos de SVNP8.
A Ressonância Magnética (RMN) é o exame complementar de diagnóstico com maior especificidade e sensibilidade para estas lesões4,9.
O tratamento de eleição é a ressecção cirúrgica. A ressecção completa é difícil nos casos de doença difusa, sendo este um dos fatores responsável pela elevada taxa de recidiva.
A SVNP é rara, principalmente na forma localizada, pelo que existe ainda pouca experiência na abordagem e tratamento destas lesões.
]]> CASO CLÍNICO
Paciente de 48 anos, género feminino, referenciada à consulta por dor na região anterior do joelho direito de carácter mecânico, sem episódios de derrame e sem relato de “falhas” ou bloqueios. Ao exame objetivo apresentava joelhos simétricos, sem desvios de eixos, sem cicatrizes ou atrofias musculares, com mobilidades ativas preservadas. Apresentava dor à palpação parapatelar interna. Estabilidade anteroposterior e varo/valgo mantidas e provas meniscais negativas.
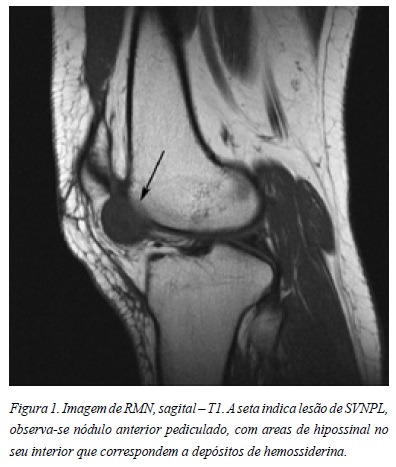
A radiografia simples do joelho nas incidências anteroposterior e perfil não apresentava alterações. A RMN do joelho revelou “lesão pediculada, sólida, vascularizada, com a dimensão 2.8x2.5x1.5 cm, sugestiva de SVNPL (…), sem outros focos suspeitos de sinovite vilonodular.” (Figura 1)

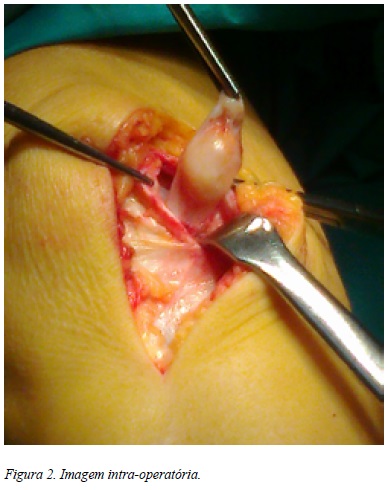
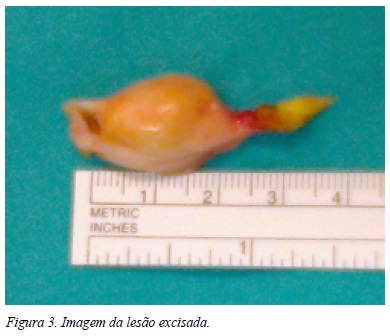
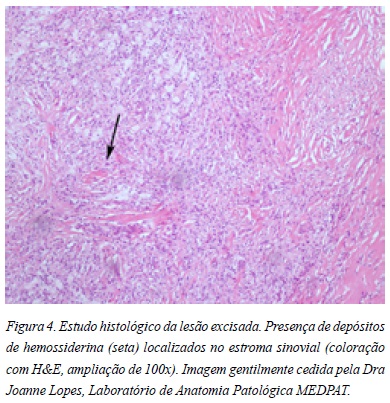
Foi submetida a excisão cirúrgica da lesão por mini-artrotomia (Figuras 2 e 3). O estudo anatomopatológico revelou trata-se de uma lesão de SVNPL (Figura 4).
]]>
O período pós-operatório decorreu sem intercorrências. Após 2 anos de seguimento, a doente permanece assintomática e a RMN de controlo não revelou recidiva da lesão.
DISCUSSÃO
Os tumores tenossinoviais de células gigantes pertencem a um espectro de lesões geralmente benignas, com características histológicas comuns, que podem ser intraarticulares ou de tecidos moles. Podem dividir-se em formas difusas e localizadas. Os tipos localizados incluem os tumores de células gigantes das bainhas tendinosas e a sinovite vilonodular pigmentada localizada, enquanto as formas difusas incluem a sinovite vilonodular pigmentada difusa e os tipos difusos de tumores de células gigantes. As formas localizadas são geralmente indolentes, mas as formas difusas podem ser localmente agressivas.
A sinovite vilonodular pigmentada pode ocorrer em qualquer articulação, bainha tendinosa ou bursa, tendo no entanto uma predileção pelo joelho.
Foi descrita pela primeira vez por Chassaignac em 1852, como uma proliferação sinovial anormal sarcoma-like nas bainhas tendinosas de tendões flexores dos dedos da mão11.
A forma localizada (SVNPL) foi descrita em 1865 por Simon como um nódulo pediculado no joelho11.
A designação sinovite vilonodular pigmentada foi pela primeira vez usada por Jaffe em 1941, na descrição de 20 lesões sinoviais que envolviam em bainhas tendinosas, articulações e bursas.
A etiologia da SVNP é desconhecida. Apesar de alguns autores sugerirem que pode ser resultado de um traumatismo e subsequente hemorragia local recorrente, outros defendem que é um processo neoplásico, existindo casos reportados de transformação maligna e metastização em doentes previamente diagnosticados com SVNP. Não existem, no entanto, dados com validade científica que corroborem uma etiologia tumoral.
A SVNP e os TCGBT ocorrem geralmente em adultos jovens com idades entre os 20 e os 40 anos, verificando-se um ligeiro predomínio de indivíduos do género feminino. Existem poucos casos publicados em crianças e adolescentes2.
Apesar de histologicamente similares, a SVNPL e a SVNPD diferem na apresentação clinica, no prognóstico e na resposta ao tratamento.
A forma localizada caracteriza-se por uma lesão pediculada e lobular, localizada no tecido sinovial. No joelho, as lesões de SVNPL geralmente ocorrem no compartimento anterior, na junção menisco-capsular. Outras localizações descritas incluem a gordura de Hoffa, o fundo de saco supra-patelar e os recessos laterais.
A forma localizada da doença tem bom prognóstico após a excisão, com baixas taxas de recidiva. Se não for tratada cirurgicamente perpetuam-se as manifestações de dor e desconforto, com limitação da atividade e função. A maioria dos autores considera a excisão marginal destas lesões o tratamento de eleição, com um excelente resultado clinico.
Numa revisão da literatura, Granowitz et al encontraram apenas 2 casos de recidiva em 24 casos reportados de SVNPL do joelho6.
A forma difusa caracteriza-se pelo envolvimento de toda a articulação e é a forma mais comum de SVNP (75%). Os sintomas, de início insidioso, incluem dor generalizada, derrame articular e rigidez. Esta forma tem um padrão destrutivo e associa-se a um pior prognóstico, com elevadas taxas de recidiva.
O diagnóstico de SVNP nem sempre é clínico, uma vez que os sintomas são inespecíficos, o que condiciona um atraso no diagnóstico.
O estudo imagiológico é importante no diagnóstico diferencial. A radiografia articular é um exame pouco específico e sensível para o diagnóstico de SVNP. As alterações que caracterizam a SVNP são as erosões ósseas periarticulares, as lesões articulares isoladas com a restante articulação preservada e, numa fase tardia, o estreitamento da interlinha articular. Estes sinais são no entanto comuns a outras doenças articulares.
O estudo do líquido sinovial é também um exame com fraca especificidade e sensibilidade.
A RMN é o exame imagiológico de escolha para o diagnóstico da SVNP. É um método não invasivo e com elevada sensibilidade e especificidade. É útil na diferenciação entre as formas difusas e localizadas e na avaliação da extensão da doença (envolvimento intra e extraarticular).
O diagnóstico final obtido pelo exame histológico do tecido sinovial10. Microscopicamente, a SNVP é caracterizada pela presença de um infiltrado histiocitário mononuclear subsinovial com ocasionais células gigantes multinucleadas (Figura 4), células ovóides ou fusiformes, macrófagos e plexos vasculares1. Depósitos extracelulares de hemossiderina são um achado comum.
À medida que a doença progride, o aumento da celularidade e vascularização é substituído por tecido fibrótico.
O diagnóstico diferencial da SVNP inclui outras doenças proliferativas da sinovial como a artrite reumatoide, sarcoma sinovial, condromatose sinovial e artropatias inflamatórias.
O tratamento da SVNP tem variado e evoluído à medida que também evoluem as técnicas cirúrgicas, nomeadamente a artroscopia. Pretende-se a redução da dor e rigidez, evitando a destruição articular e protelando a necessidade da substituição artroplástica.
Atualmente não existe lugar para o tratamento conservador na SVNP, excetuando-se casos recorrentes diagnosticados por estudos de imagem mas sem sinovite progressiva, podendo nestas situações optar-se por uma atitude expectante em vez da re-operação.
A radioterapia (RT) é uma opção terapêutica que tem evoluído nos últimos anos. Se por um lado a radioterapia externa não mostrou ser eficaz como terapêutica adjuvante à sinovectomia, ultimamente tem crescido o interesse pela radioterapaia intraarticular tem sido crescente. Apesar de não existirem estudos que comprovem a superioridade da radioterapia intraarticular adjuvante relativamente à sinovectomia isolada, alguns autores sugerem que pode ter interesse em doentes com doença sinovial documentada pós sinovectomia12. Ex istem contudo algumas preocupações relacionadas com as complicações da radioterapia intraarticular, nomeadamente a radionecrose sinovial.
A excisão cirúrgica é o método gold standard no tratamento da SVNP, podendo esta ser artroscópica ou por via aberta.
Quanto ao tratamento artroscópico da SVNPL, os estudos publicados são praticamente limitados ao joelho. A artroscopia do joelho permite visualizar facilmente o compartimento anterior, onde se localiza a maioria das lesões de SVNPL, bem como os recessos lateral e medial. A sinovectomia parcial por artroscopia tem apresentado baixas taxas de recidiva, sendo importante uma ressecção alargada ao tecido saudável.
O papel da artroscopia no tratamento da forma difusa da SVNP é discutível, já que está afetada uma maior área de sinovial, e as lesões localizam-se predominante no compartimento posterior, local de mais difícil acesso.
Elevadas taxas de sucesso tem sido reportadas por vários autores6,7,9 relativamente à sinovectomia aberta no tratamento da SVNPL. Johansson et al não encontraram recidivas em 11 doentes submetidos à excisão por artrotomia7.
A artroplastia total deve ser considerada nos casos de recidivas persistentes e osteoartrose avançada.
Os autores consideram que, no caso apresentado, a excisão da lesão por artrotomia foi eficaz e não apresentou complicações (nomeadamente retração fibrótica e perda de amplitude articular). Permitiu a visualização adequada da lesão e a sua excisão de forma alargada. No entanto, parece-nos que em lesões localizadas e de pequena dimensão a ressecção artroscópica é a opção.
A SNVP é um desafio diagnóstico devido à pouca especificidade dos seus sintomas e às características radiológicas subtis, constituindo uma patologia que deve ser considerada na abordagem da gonalgia, principalmente em adultos jovens.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Bouali H, Deppert E, Leventhal L, Reeves B, Pope T. Pigmented villonodular synovitis: a disease in evolution. The Journal of Rheumatology. 2004; 31: 1659-1662 [ Links ]
2. Bruns J, Schubert T, Eggers-Stroeder G. Pigmented villonodular synovitis in children. A case report. Arch Orthop Trauma Surg. 1993; 112: 148-151 [ Links ]
3. Dorwart R, Genant H, Johnston W, Morris J. Pigmented villonodular synovitis of synovial joints: Clinical, pathologic, and radiologic features. Am J Roentgenol. 1984; 143: 877-885 [ Links ]
4. Flandry F, Hughston J, McCann S, Kurtz D. Diagnostic features of diffuse pigmented villonodular synovitis of the knee. Clin Orthop Relat Res. 1994; 300: 212-220 [ Links ]
5. Friedman M, Schwartz E. Irradiation therapy of pigmented villonodular synovitis. Buli Hosp Joint Dis. 1957; 18: 19-32 [ Links ]
6. Granowitz S, D'Antonio L, Mankin H. The pathogenesis and long-term end results of pigmented villonodular synovitis. Clin Otthop Relat Res. 1976; 114: 335-351 [ Links ]
7. Johansson J, Ajjoub S, Coughlin L, Wener J, Cruess R. Pigmented villonodular synovitis of joints. Clin Orthop Relat Res. 1982; 163: 159-166 [ Links ]
8. Myers B, Masi A. Pigmented villonodular synovitis and tenosynovitis: A clinical epidemiologic study of 166 cases and literature review. Medicine (Baltimore). 1980; 59: 223-238 [ Links ]
9. Kim S, Shin S, Choi N, Choo E. Arthroscopic treatment for localized pigmented villonodular synovitis of the knee. Clin Orthop Relat Res. 2000; 379: 224-230 [ Links ]
10. Klompmaker J, Veth R, Robinson P, Molenaar W, Nielsen H. Pigmented villonodular synovitis. Arch Orthop Trauma Surg. 1990; 109: 205-210 [ Links ]
11. Kramer D, Frassica F, Frassica D, Cosgarea A. Pigmented Villonodular Synovitis of the Knee Diagnosis and Treatment. Journal of Knee Surg. 2009; 22: 243-254 [ Links ]
12. Wiss D. Recurrent villonodular synovitis of the knee: Successful treatment with Yttrium-90. Clinical Orthop Relat Res. 1982; 169: 139-144 [ Links ]
Eunice Carvalho
Serviço de Ortopedia e Traumatologia
Unidade Local de Saúde da Guarda ]]>
Av. Rainha D. Amélia
6301-857 Guarda
Portugal
eunice.tavares@gmail.com
Conflito de interesse:
Nada a declarar.
Data de Submissão: 2014-06-29
Data de Revisão: 2014-08-20
]]> Data de Aceitação: 2014-08-20 ]]>