Pseudaneurisma da artéria tibial anterior. Complicações na artroscopia anterior do tornozelo
André CarvalhoI; Francisco AgostinhoI; Joana RodriguesI; Joaquim NelasI; Manuel SousaI
I. Serviço de Ortopedia. Centro Hospitalar Tondela-Viseu.
RESUMO
]]> O desenvolvimento técnico da artroscopia do tornozelo permitiu uma notável evolução diagnóstica e terapêutica associada a baixa morbilidade.Encontra-se, contudo, descrita uma taxa de complicações variável dos 3 aos 17%.
Os autores apresentam um caso de pseudaneurisma da artéria tibial anterior após artroscopia anterior do tornozelo (sinovectomia e exostosectomia), uma complicação extremamente rara (<1%) com os portais standard anteromedial e anterolateral.
Após o diagnóstico a doente foi referenciada a Cirurgia Vascular tendo sido tratada com boa evolução clínica.
Discute-se a incidência das complicações da artroscopia do tornozelo, em particular do pseudaneurisma da artéria tibial anterior, intervenções subsequentes e opções de tratamento correntes.
Palavras chave: Artroscopia Tornozelo, artéria Tibial Anterior, Complicações, Pseudaneurisma.
ABSTRACT
The technical development of ankle arthroscopy has allowed remarkable advances in diagnostic and therapeutic procedures associated with low morbidity.
It is, however, described a rate of complications varying from 3 to 17%.
]]> The authors present a case of pseudaneurysm of anterior tibial artery after anterior ankle arthroscopy (synovectomy and exostosectomy), an extremely rare complication (<1%) with standard anteromedial and anterolateral portals.After diagnosis the patient was referred to vascular surgery and has been treated with good clinical outcome.
Discussion of the incidence of complications in ankle arthroscopy, particularly anterior tibial artery pseudaneurysm, subsequent interventions and current treatment options.
Key words: Ankle arthroscopy, anterior tibial artery, complications, pseudaneurysm.
INTRODUÇÃO
A artroscopia anterior do tornozelo (iniciada em 1930)1 é um procedimento considerado seguro e reprodutível para diagnóstico e tratamento de múltiplas afecções articulares.
As indicações major do procedimento são o tratamento do síndrome de impingement anterior, instabilidades e lesões osteocondrais (causas de bloqueio articular) mas também no diagnóstico de dor, edema, rigidez ou hemartrose inexplicadas2.
A artroscopia do tornozelo acarreta um baixo risco de complicações vasculares quando comparada com a do joelho3 sendo as principais complicações de origem neurológica (cerca de 50%)4,5.
Os pseudaneurimas são complicações raras da artroscopia do tornozelo6 mas podem conduzir a importante morbilidade com complicações severas se negligenciados.
]]> Existem 6 casos descritos na literatura de pseudaneurisma da artéria tibial anterior pós artroscopia do tornozelo3,7,8,9,10.
CASO CLÍNICO
Mulher caucasiana de 52 anos, sem antecedentes de relevo e com quadro de dor anterior do tornozelo direito e episódios de bloqueio oito meses após entorse.
O exame físico revelava edema difuso da articulação, tensão sobre a interlinha anterolateralmente e no ligamento talofibular anterior. A mobilidade activa estava limitada por dor a 2º dorsiflexão e 20º de flexão plantar.
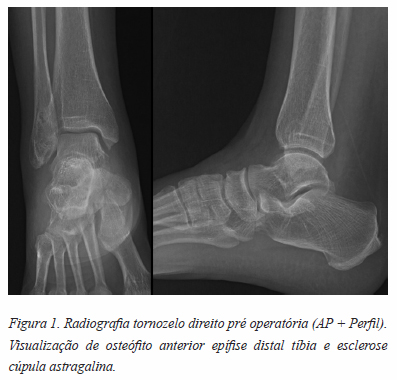
As radiografias demonstravam osteófitos face anterior epífise distal tíbia e esclerose cúpula astragalina (Figura 1).

]]> Após falência do tratamento conservador com analgesia e fisioterapia foi proposta artroscopia para sinovectomia e exostosectomia.
Foi realizada a técnica pelos portais standard (anteromedial e anterolateral), sem intercorrências.
Dez dias após a cirurgia foram removidos os pontos de sutura e iniciou reabilitação. Manteve-se em carga parcial durante 4 semanas.
Na consulta das 5 semanas a doente apresentou um quadro de edema, disestesias e dor tornozelo direito condicionando a marcha. Foi instruída nos cuidados - carga conforme tolerável - e orientada para fisioterapia.
Na consulta seguinte apresentava menor edema e uma massa pulsátil na face anterior do tornozelo. O diagnóstico diferencial no momento seria derrame articular, artrite tornozelo, sinovite adesiva ou pseudaneurisma.
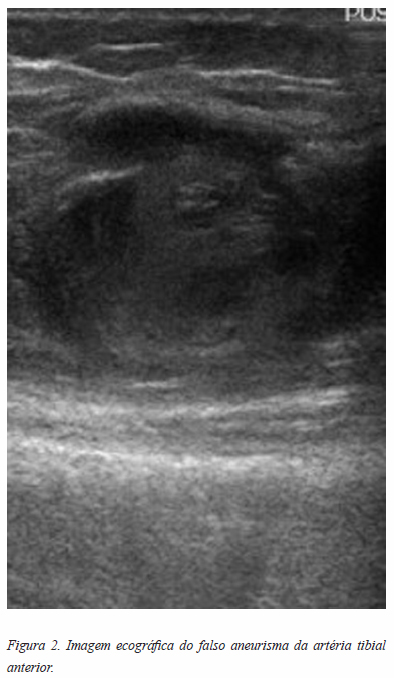
Foi pedido uma ecografia com Doppler para esclarecimento diagnóstico, vindo a confirmar-se um pseudaneurisma da artéria tibial anterior ao nível da articulação com 2cm maior eixo (Figura 2).
]]> Referenciada a Cirurgia Vascular tendo sido operada aos 2 meses pós artroscopia: Operação de O’Farrel (excisão do saco aneurismático da artéria tibial anterior direita e anastomose topo-a-topo) (Figuras 3 a 6).
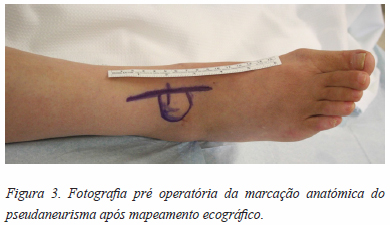
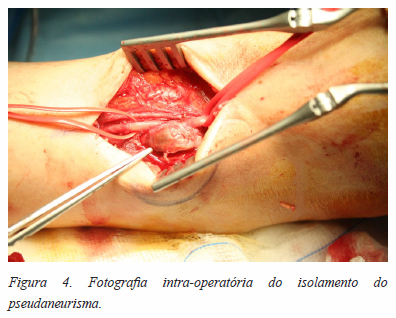
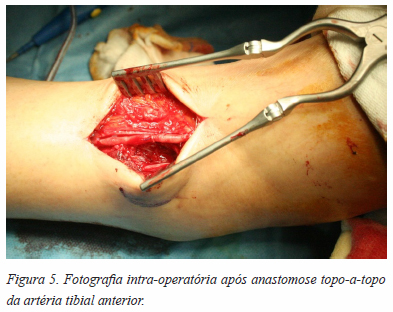
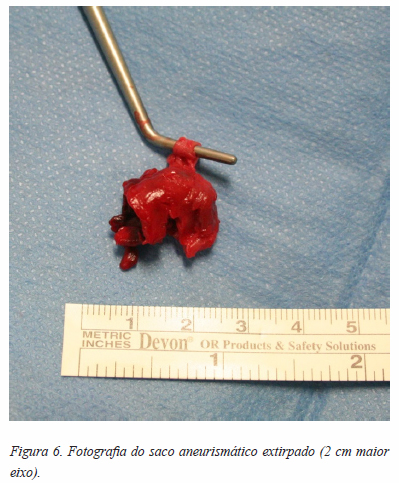
Prosseguiu com um programa de reabilitação pós cirúrgica apresentando boa evolução clínica em follow up aos 6 meses (marcha autónoma sem restrição nas AVDs, sem queixas, KOFOED ankle score 81; controlo com ecodoppler normal – “permeabilidade da artéria tibial anterior, sem recidiva de falso aneurisma”).
DISCUSSÃO
Os pseudaneurismas são uma complicação iatrogénica pouco frequente da cirurgia artroscópica do tornozelo sendo a sua incidência de 0,008%11.
O pseudaneurisma, também conhecido como “falso aneurisma”, é consequência do traumatismo das três camadas histológicas arteriais condicionando hemorragia e a formação de uma cápsula fibrosa com uma neo-circulação externamente ao lúmen lesado.
Esta estrutura fibrosa ao não apresentar a arquitectura típica do vaso expande-se até ficar confinada nos limites das estruturas adjacentes e tem maior potencial de rotura do que os verdadeiros aneurismas.
]]> Parece evidente que a hemorragia e a remodelação do hematoma estarão na origem do falso aneurisma.O mecanismo etiológico e os factores de risco não são claros podendo surgir a lesão na execução dos portais (considerando as variações anatómicas da artéria 3 nomeadamente o desvio lateral (5,5%) ou medial (3,5%)12, durante a instrumentação cirúrgica (distensão capsular insuficiente, instrumentação agressiva, sinovectomia alargada ou exérese de osteófitos ou corpos livres) ou associado a condições médicas como coagulopatias7,8.
O período pós-operatório para desenvolvimento do pseudaneurisma é variável existindo descrições da apresentação desde uma semana3,8 até dois meses10,11.
A lesão vascular passa frequentemente despercebida no peri-operatório podendo a sua apresentação estar diferida meses ou anos num quadro injustificável caracterizado por dor e/ou edema e uma massa pulsátil.
As potenciais complicações dos pseudaneurismas da artéria tibial anterior são a hemartrose do tornozelo13, síndrome compartimental14 e rotura vascular (a mais severa e que poderá conduzir a instabilidade hemodinâmica)
Nesse contexto, um diagnóstico precoce e tratamento específico são fundamentais.
Estão descritos vários métodos de tratamento desde o conservador – terapia compressiva ecoguiada três horas/dia com intervalo de três a quatro dias entre tratamentos (4 sessões por Jang et al 2008)– ao cirúrgico – excisão falso aneurisma com anastomose topo-a-topo (O’Farrel 1997), excisão e bypass com enxerto venoso (Mariani et al 2001), laqueação do falso aneurisma (Darwish et al 2004) e resseção com interposição veia safena (Kotwal et al 2007).
A prevenção de complicações passará pré-operatoriamente por uma identificação percutânea da anatomia (principalmente do nervo peroneal superficial), mapeamento vascular com EcoDoppler e uma cuidadosa dissecção e desbridamento dos tecidos durante a cirurgia.
Na presença de osteófitos, alguns autores defendem o procedimento aberto em detrimento da artroscopia para diminuição do risco de lesão vascular.
]]> CONCLUSÕES
Os pseudaneurismas resultantes de dano vascular são uma complicação rara da artroscopia do tornozelo.
A dificuldade do diagnóstico inicial deve-se à evolução insidiosa do quadro importando manter um elevado grau de suspeita clínica dado que o tratamento imediato é fundamental na evolução evitando potenciais sequelas importantes.
O tratamento é função do local da lesão e das dimensões do pseudaneurisma sendo o tratamento preferencial cirúrgico.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Burman MS. Arthroscopy or the direct visualization of joints: An experimental cadaver study. J Bone Joint Surg Am. 1931; 13: 669-695 [ Links ]
2. van Dijk CN, van Bergen CJ. Advancements in ankle arthroscopy. J Am Acad Orthop Surg. 2008; 16: 635-646 [ Links ]
3. Mariani PP, Mancini L, Giorgini TL. Pseudoaneurysm as a complication of ankle arthroscopy. Arthroscopy. 2001; 17: 400-402 [ Links ]
4. Ferkel RD, Heath DD, Guhl JF. Neurological complications of ankle arthroscopy. Arthroscopy. 1996; 12: 200-208 [ Links ]
5. Barber FA, Click J, Britt BT. Complications of ankle arthroscopy. Foot Ankle. 1990; 10: 263-266 [ Links ]
6. Bernard JP, Ramavath AL, Cornish JA, Ganapathi M, Williams DT. Missed diagnosis of ankle pseudaneurysm following ankle arthroscopy: a case report. Cases Journal. 2009; 2: 162 [ Links ]
7. Kotwal RS, Acharya A, O?Doherty D. Anterior tibial artery pseudoaneurysm in a patient with hemophilia: a complication of ankle arthroscopy. J Foot Ankle Surg. 2007; 46: 314-316 [ Links ]
8. Darwish A, Ehsan O, Marynissen H, Al-Khaffaf H. Pseudoaneurysm of the anterior tibial artery after ankle arthroscopy. Arthroscopy. 2004; 20: 63-64 [ Links ]
9. O?Farrell D, Dudeney S, McNally S, Moran R. Pseudoaneurysm formation after ankle arthroscopy. Foot Ankle Int. 1997; 18: 578-579 [ Links ]
10. Salgado CJ, Mukherjee D, Quist MA, Cero S. Anterior tibial artery pseudoaneurysm after ankle arthroscopy. Cardiovasc Surg. 1998; 6: 604-606 [ Links ]
11. Jang EC, Kwak BK, Song KS, Jung HJ, Lee JS, Yang JJ. Pseudoaneurysm of the Anterior Tibial Artery after Ankle Arthroscopy treated with Ultrasound-Guided Compression Therapy: A Case Report. JBJS Am. 2008; 90 (10): 2235-2239 [ Links ]
12. Huber JF. Anatomy of the foot and ankle. Anatomy of the foot. Philadelphia: JB Lippincott; 1993. p. 294-300. [ Links ]
13. Ris HB, Klaiber C. Hemarthrosis of the ankle secondary to false aneurysm caused by impingement from an osteophyte: A case report. J Bone Joint Surg Am. 1989; 71: 935-937 [ Links ]
14. Ward NJ, Wilde GP, Jackson WF, Walker N. Compartment syndrome following ankle sprain. J Bone Joint Surg Br. 2007; 89: 953-955 [ Links ]
15. Ferkel RD, Small HN, Gittins JE. Complications in foot and ankle arthroscopy. Clin Orthop Relat Res. 2001; 391: 89-104 [ Links ]
Conflito de interesse:
Nada a declarar
Joaquim Soares do Brito
Centro Hospitalar Lisboa Norte
Hospital de Santa Maria ]]>
Avenida Professor Egas Moniz
1649-035 Lisboa
Portugal
joaquimsoaresdobrito@gmail.com
Data de Submissão: 2014-11-18
Data de Revisão: 2015-01-02
Data de Aceitação: 2015-01-02
]]>