Lesão do Ligamento Cruzado Anterior: Apresentação Clínica, Diagnóstico e Tratamento
Ana PinheiroI; Cristina Varino SousaI
I. Serviço de Ortopedia e Traumatologia da Unidade Local de Saúde do Alto Minho, Viana do Castelo, Portugal. Viana do Castelo. Portugal.
RESUMO
]]> A lesão do ligamento cruzado anterior (LCA) é uma das lesões ligamentares do joelho mais comuns, daí a reconstrução do LCA ser uma das cirurgias mais frequentemente realizadas. O seu diagnóstico baseia-se na história e no exame clínico do joelho.As lesões do LCA ocorrem predominantemente em indivíduos jovens e activos, sobretudo durante a atividade física. As mulheres são mais afectadas que os homens. As lesões do LCA por mecanismo indirecto ocorrem através de uma complexa interacção de múltiplos factores de risco: ambientais, anatómicos, hormonais, neuro-musculares e familiares.
A evolução natural da lesão do LCA não está completamente decifrada e acredita-se que a instabilidade anterior possa progredir para lesões degenerativas.
O tratamento da lesão do LCA depende do tipo de lesão
O objetivo deste trabalho centrou-se na revisão bibliográfica da lesão do LCA a fim de adquirir os conhecimentos mais recentes nas várias dimensões desta patologia, nomeadamente a nível da epidemiologia, patogénese, apresentação clínica, diagnóstico e tratamento.
Foi realizada uma pesquisa na base de dados pubmed/medline com as palavras “Anterior Cruciate Ligament (ACL) Injury” e “ACL Injury Treatment”, selecionando sobretudo artigos publicados nos últimos 15 anos e em língua inglesa, incluindo artigos originais e de revisão.
Palavras chave: Lesão do Ligamento Cruzado Anterior, Tratamento da Lesão do LCA, Reconstrução do LCA.
ABSTRACT
Anterior cruciate ligament (ACL) injury is one of the most common knee ligament injuries, then ACL reconstruction be one of the most frequently performed surgeries. The diagnosis is based on history and clinical examination of the knee. The ACL injuries occur predominantly in young and active individuals, especially during physical activity. Women are more affected than men. The ACL injury by indirect mechanism occurs through a complex interaction of multiple risk factors: environmental, anatomical, hormonal, neuromuscular and family. The natural evolution of ACL injury is not completely deciphered and it is believed that the anterior instability can progress to degenerative disease.
]]> Treatment of ACL injuries depends on the type of injury. This study focused on literature review of ACL injury in order to acquire the latest knowledge in the various dimensions of this disease, particularly in terms of epidemiology, pathogenesis, clinical presentation, diagnosis and treatment. Research was carried out in the database Pubmed / Medline with the words “Anterior Cruciate Ligament (ACL) Injury” and “ACL Injury Treatment”, especially selecting articles published in the last 15 years and in English, including original and review articles.Key words: Anterior Cruciate Ligament Injury, ACL Injury Treatment, ACL Reconstruction.
INTRODUÇÃO
A lesão do ligamento cruzado anterior (LCA) é uma das lesões ligamentares do joelho mais comuns, daí a reconstrução do LCA ser uma das cirurgias mais frequentemente realizadas.1,2
Não é de estranhar, portanto, que existam mais de 2000 estudos publicados acerca deste ligamento, sendo este o ligamento mais estudado do corpo humano.2
Na Alemanha surgem cerca de 30/100000 rupturas do LCA na população geral e cerca de 70/100000 em desportistas.3
Nos EUA anualmente ocorrem cerca de 200000 lesões do LCA e são realizadas aproximadamente 100000 cirurgias de reconstrução deste mesmo ligamento.4,5
Estes dados enfatizam a elevada frequência deste tipo de lesões e a importância da necessidade de um tratamento adequado.
O objetivo deste trabalho centrou-se na revisão bibliográfica da lesão do LCA a fim de adquirir os conhecimentos mais recentes nas várias dimensões desta patologia, nomeadamente a nível da epidemiologia, patogénese, apresentação clínica, diagnóstico e tratamento.
]]>ANATOMIA
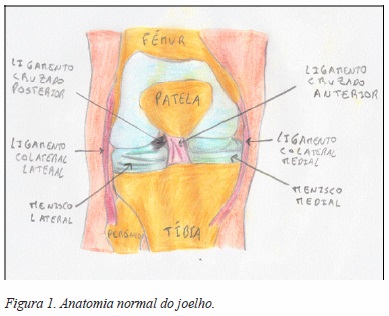
O joelho é constituído por três ossos (fémur, tíbia e patela) que originam duas articulações, a fémuro-tibial e a fémuro-patelar (Figura 1). O joelho é uma articulação complexa, sendo estabilizado por ligamentos, músculos e pela cápsula articular.6,7,8

Os ligamentos conectam os ossos, contribuindo assim para a estabilidade do joelho.8 De referir que existem 4 ligamentos a ligar o fémur e a tíbia: dois colaterais que estabilizam o joelho latero-medialmente (ligamentos colaterais medial e lateral) e dois intra-articulares (os ligamentos cruzados anterior e posterior) que controlam o movimento do joelho anteroposteriormente.7,8
De uma forma geral, todos os componentes do joelho trabalham em conjunto para manter a estabilidade do mesmo.
O LCA é um dos principais ligamentos que une o fémur à tíbia, não permitindo que a tíbia deslize anteriormente em relação ao fémur e proporcionando estabilidade rotacional ao joelho.6-9
]]> Esta harmonia pode, contudo, ser interrompida pelo desgaste ou lesões deste ligamento, causando dor, fraqueza ou perda de função.6,9
FISIOPATOLOGIA DA LESÃO DO LCA
A lesão do LCA ocorre quando o ligamento é forçado além da sua aptidão elástica, podendo ocorrer uma ruptura parcial ou total.
As lesões ligamentares podem classificar-se em grau I, II e III. Na lesão de grau I existe uma lesão ligamentar ligeira, um estiramento, mantendo-se a estabilidade da articulação. Na lesão de grau II ocorre já uma ruptura parcial das fibras do ligamento, originando um ligamento frouxo. Por último, as lesões de grau III caracterizam-se por uma ruptura total do ligamento, causando assim instabilidade articular.10
Apesar da evolução natural da lesão do LCA ainda não estar determinada, acredita-se que a instabilidade anterior progrida para lesões degenerativas meniscais e comprometa o desempenho dos indivíduos durante a atividade física.9
A lesão do LCA pode ocorrer por traumatismo directo ou indirecto, ocorrendo habitualmente perante uma mudança súbita de direção, paragem repentina, queda incorrecta de um salto ou então por contacto directo.6 Estas lesões ocorrem maioritariamente por trauma indireto e podem ocorrer através de vários mecanismos: rotação externa, abdução e forças anteriores aplicadas na tíbia, rotação interna do fémur sobre a tíbia e hiperextensão do joelho.11
O mecanismo de lesão por trauma direto ocorre habitualmente num traumatismo em que o fémur é puxado posteriormente quando o joelho se encontra a 90 graus de flexão e a tíbia está fixa. Por sua vez, a lesão por trauma indireto acontece perante paragem brusca e saltos sem qualquer contato físico, provocando lesões isoladas do LCA seguidas de hemartrose.10 A hiperflexão forçada do joelho, flexão forçada, extensão completa do joelho e hiperextensão forçada do joelho são os mecanismos mais comuns nas lesões isoladas do LCA.10
APRESENTAÇÃO CLÍNICA E DIAGNÓSTICO
]]> O diagnóstico baseia-se na história e no exame clínico do joelho.Habitualmente, os pacientes portadores de lesão do LCA costumam apresentar dor, edema, sensação de instabilidade no joelho, sensibilidade ao longo da interlinha articular, desconforto ao caminhar e perda da amplitude de movimentos.8
A suspeita de lesão no LCA deve levar o clínico a realizar um exame físico completo do joelho, testando todas as estruturas do joelho lesionado e comparando com o joelho saudável, podendo assim diagnosticar a maioria das lesões ligamentares.12
A laxidez ligamentar pode ser avaliada através de vários testes específicos tais como: teste de Lachman, Pivot Shift, Mac-Intosh e Gaveta Anterior. A positividade nos testes de Mac-Intosh, Gaveta Anterior e Lachman apontam para uma lesão do LCA.13
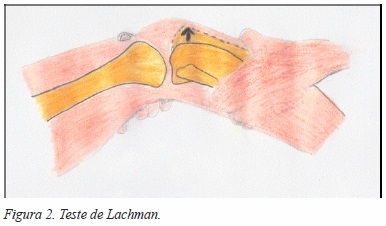
Nos testes de Mac-Intosh ou Pivot Shift o paciente fica em decúbito dorsal, com o joelho em extensão e a tíbia subluxada anteriormente13. A flexão do joelho começa calmamente quando, perto dos 30 a 50 graus, logo se percebe a redução da subluxação anterior. O teste da gaveta anterior é realizado com o paciente em decúbito dorsal e o joelho fletido a 80 ou 90 graus. O teste de Lachman, por sua vez, permite o melhor diagnóstico de uma lesão do LCA. Este evidencia-se do teste de gaveta anterior somente na angulação da flexão do joelho, tal como se pode observar nas Figuras 2 e 3. É de realçar, contudo, que por vezes, estes testes não fornecem resultados exactos.13
]]>

O Raio-X, a Tomografia axial computorizada (TAC) e a Ressonância Magnética (RM) constituem os exames complementares de diagnóstico importantes no estudo do joelho. O Raio-X apesar de não demonstrar as lesões ligamentares pode evidenciar fraturas ósseas associadas, pois ao detectar a fratura de Segond, aponta para a avulsão óssea ocasionada pela rutura do ligamento colateral lateral e fornece-nos pistas para outras lesões associadas.13
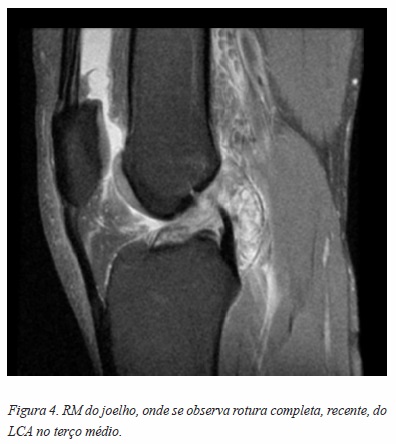
A TAC é utilizada na impossibilidade de realizar a RM, pois a RM permite uma melhor visualização dos ligamentos, cartilagem e dos outros componentes do joelho. A RM é pois muito útil no pré-operatório, pois indica o tipo e a gravidade da lesão (Figura 4).13,14
PATOGÉNESE
]]> As lesões do LCA ocorrem predominantemente em indivíduos jovens (16-45 anos) e activos, sobretudo durante a atividade física.15,16 As mulheres são mais afectadas do que os homens, não existindo ainda consenso para este facto, mas são apontadas razões anatómicas, hormonais e técnicas de treino. No futebol e basquetebol as lesões ocorrem cerca de 3 vezes mais em mulheres do que em homens.15-18Segundo a “Hunt Valley II Consensus Conference on the prevention of non-contact LCA injuries” realizada em Janeiro de 2005, as lesões do LCA por mecanismo indirecto ocorrem através de uma complexa interacção de múltiplos factores de risco: ambientais, anatómicos, hormonais, neuro-musculares e familiares.19 No que toca aos factores ambientais a informação é obscura, podendo ocorrer maior número de lesões do LCA em condições meteorológicas solares; sabe-se que o uso de joelheiras diminui a percentagem de lesões e que o tipo de superfície e o calçado também influenciam o risco deste tipo de lesões.19
Os factores de risco anatómicos encontrados estão associados a um aumento do risco de lesão, e são mais difíceis de modificar do que os ambientais, hormonais ou neuromusculares. A literatura aponta que a magnitude do ângulo Q, o grau de valgização do joelho estático e dinâmico, o índice de massa corporal (IMC), a largura do entalhe femoral e a geometria do LCA são factores de risco para esta lesão.16,19
Apesar de não existir unanimidade, alguns trabalhos constataram que as hormonas medeiam os aumentos cíclicos na frouxidão do joelho ao longo do ciclo menstrual e que ocorrem mais lesões no início e no fim das fases foliculares.16,19
No que toca aos fatores de risco neuromusculares sabe-se que as mulheres possuem um desequilíbrio entre a força muscular, flexibilidade e coordenação das extremidades inferiores, e que estes desequilíbrios estão associados a um maior risco de lesão.
Apesar de existirem ainda poucos estudos a abordar este assunto, acredita-se que possa existir uma predisposição familiar para lesões por mecanismos indiretos do LCA.19
TRATAMENTO
O tratamento da lesão do LCA depende do tipo de lesão, pois podemos deparar-nos com um ligamento estirado, uma ruptura ligamentar parcial ou uma ruptura completa do ligamento.20
De uma forma geral, o tratamento conservador é utilizado nas rupturas parciais, sendo que nas rupturas totais opta-se pelo método cirúrgico ou conservador.20
]]> Assim, o doente e o médico podem optar por um tratamento cirúrgico ou não-cirúrgico/conservador, dependendo de vários factores como: idade, extensão das lesões associadas, a disponibilidade para realizar um programa de reabilitação e o estilo de vida do paciente.3, 9 Num estudo com 4355 joelhos com lesão do LCA a maioria dos pacientes (94%) foram submetidos à reconstrução do LCA, sendo os restantes tratados conservadoramente. Este estudo evidenciou que ambos os tratamentos são eficazes se tiverem em conta as características particulares de cada paciente.21Tratamento Não Cirúrgico
O tratamento conservador visa a analgesia e a estabilização da dinâmica do joelho, através do reforço muscular e do treino proprioceptivo.10,13,20
Este tipo de tratamento consiste no uso de ortóteses para proteger o joelho de instabilidades, fisioterapia (através de exercícios específicos para fortalecer o joelho e os músculos) e mudanças no estilo de vida ou atividades, recomendando-se exercícios físicos que coloquem menos carga sobre o joelho.
O tratamento conservador está indicado nas seguintes situações: ruptura parcial e sem sintomas de instabilidade; ruptura completa e sem sintomas de instabilidade durante a actividade desportiva de baixo risco em pacientes dispostos a abdicar de actividades físicas exigentes; indivíduo que têm estilos de vida sedentário ou que executam trabalho manual leve, e nas crianças por apresentarem as placas de crescimento abertas.6,20
Tratamento Cirúrgico
O objetivo do tratamento cirúrgico é evitar a instabilidade do joelho e promover a restauração da função do ligamento.
Na década de 70 desenvolveram-se técnicas de reconstrução não-anatómicas extra-articulares do LCA, surgindo mais tarde a reconstrução do LCA através do uso dos tendões da pata de ganso. Posteriormente emergiu um novo avanço no que toca aos métodos de fixação, destacando-se o uso de parafusos de interferência metálicos. Desde então novos métodos de fixação têm sido desenvolvidos.22 O tratamento cirúrgico é geralmente realizado em pacientes jovens e desportistas , mesmo naqueles com lesões combinadas, como por exemplo no caso da “tríade infeliz” (lesão do LCA, ligamento colateral lateral e menisco medial) frequentemente presente em esquiadores e jogadores de futebol.21,23 O período mais apropriado para a realização do tratamento cirúrgico é ainda controverso, mas no caso de lesão aguda a cirurgia é realizada após um período de 4 a 6 semanas.22
A reconstrução do LCA em crianças e adolescentes pode lesionar a placa de crescimento, gerando problemas no crescimento ósseo. Nestes casos o cirurgião pode atrasar acirurgia até que a criança atinja a maturidade esquelética ou então deve modificar a técnica cirúrgica.20
O tratamento cirúrgico mais utilizado consiste na reconstrução intra-articular por via artroscópica através de enxertos autólogos, com um substituto de tendão que éidêntico ao tecido ligamentar. Os enxertos mais vulgares provêm do tendão patelar e dos isquiotibiais (semitendinoso e gracil). Por vezes, são utilizados aloenxertos provenientes de cadáveres.24,25
]]> A técnica cirúrgica osso-tendão-osso que utiliza o tendão patelar é a mais popular. Nesta técnica o enxerto é retirado do tendão patelar e é utilizado um processo de fixação no osso através da produção de um canal onde o ligamento se insere para ser efetivamente fixado por um parafuso. A dor patelar e o risco aumentado de rigidez pós-operatória constituem algumas das complicações associadas a esta técnica cirúrgica.23,25,26A técnica mais recente de fixação com duplo feixe é realizada através do uso de 2 enxertos, o tendão gracílis e semitendinoso.
A escolha relativa ao método cirúrgico a utilizar deve ser discutida pelo médico e pelo paciente, pois sendo o enxerto do tendão patelar e dos isquiotibiais os mais utilizados, e dado ambos apresentarem bons resultados, alguns estudos associam uma menor taxa de complicações ao enxerto dos tendões isquiotibiais.
Estudos comparativos dos resultados obtidos com o enxerto com tendão patelar e dos isquiotibiais demonstraram que o enxerto dos tendões da pata de ganso apresenta melhores resultados: menor incisão, recuperação mais rápida, menor dor rotuliana pós-operatória, menor osteoartrose radiológica e menor risco de rigidez pós-operatória.24
Num estudo com 100 rupturas completas do LCA e que foram aleatoriamente submetidas a enxertos do tendão patelar ou dos isquiotibiais, registaram-se diferenças significativas na flexão do joelho e na força de extensão no 3º mês do pós-operatório.25
Um outro estudo com 120 pacientes encontrou nos enxertos do tendão patelar uma maior prevalência de desconforto pós-operatório na região do joelho, maior área de diminuição da sensibilidade da pele, menor taxa de osteoartrose e maior prevalência de alargamento no túnel femoral.23, 26
Um trabalho semelhante com 41 pacientes demonstrou que a reconstrução do LCA independentemente do método cirúrgico e da escolha do enxerto apresenta bons resultados clínicos, com retorno a um nível razoável da atividade desportiva e satisfação do paciente.27
Em outros trabalhos idênticos aos acima referenciados, constatou-se não haver resultados suficientes para tirar conclusões acerca das diferenças entre os dois enxertos no que toca ao resultado funcional a longo prazo e que o enxerto do tendão semitendinoso é pelo menos uma opção equivalente ao enxerto do tendão patelar para reconstrução do ligamento cruzado anterior, recomendando-se a sua utilização.22, 28, 29
Como todas as cirurgias, a ligamentoplastia apresenta riscos associados, tais como: infecção (é um risco inerente a qualquer cirurgia), rigidez (o tecido da cicatriz restringe a capacidade de dobrar e esticar o joelho), instabilidade do joelho e recidiva da lesão (a instabilidade pode dever-se à ruptura ou alongamento do LCA reconstruido) e hemorragias (a hemartrose é um dos problemas mais comuns mas menos graves).23,24,25,26,29
A cirurgia aberta de reconstrução ligamentar só é realizada se surgirem complicações no decurso da cirurgia artroscópica.24
CONCLUSÃO
A lesão do LCA constitui uma das lesões ligamentares do joelho mais comuns e é por isso também muito estudada.
O tratamento da lesão do LCA depende do tipo de lesão. De uma forma geral, o tratamento conservador é utilizado nas rupturas parciais, sendo que nas rupturas completas opta-se pelo método cirúrgico ou conservador, dependendo das características do paciente. Ambos os tratamentos são eficazes e apresentam bons resultados dependendo do tipo de lesão. A nível do tratamento cirúrgico utilizam-se diferentes técnicas sendo o enxerto do tendão patelar e dos isquiotibiais as mais utilizadas. Ambas apresentam bons resultados, no entanto alguns estudos associam menos complicações ao enxerto dos tendões isquiotibiais.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Ritchie JR, Parker RD. Graft selection in anterior cruciate ligament revision surgery. Clin Orthop. 1996; 325: 65-77 [ Links ]
2. Frobell RB, Roos EM, Roos HP, Ranstam J. A randomized trial of treatment for acute anterior cruciate ligament tears. N English J Med. 2010; 363 (4): 331-342 [ Links ]
3. Voigt C, Schonaich M, Lill H. Anterior Cruciate Ligament Reconstruction: State of art. European Journal of Trauma. 2006; 32: 332-3339 [ Links ]
4. McDaniel WJ Jr, Dameron TB Jr. The untreated anterior cruciate ligament rupture. Clin Ortho Relat Res. 1983; 172: 158-163 [ Links ]
5. Duthon VB, Barea C, Abrassart S, Fasel JH, Fristchy D, Menetrey J. Anatomy of the anterior cruciate ligament.. Knee Surg Sports Traumatol ARthrosc. 2007; 14 (3): 204-213 [ Links ]
6. Han HS, Seong SC, Lee S, Lee MC. Anterior Cruciate Ligament Reconstruction.. Clinical Orthopaedics and Related Research. 2008; 466 (1): 198-204 [ Links ]
7. Kapandji A. Fisiologia articular. São Paulo: Panamericana; 200. [ Links ]
8. Kjaer M. Compêndio de medicina desportiva. Ciência básica e aspectos clínicos da lesão desportiva e da actividade física. Instituto Piaget; 2003. [ Links ]
9. Romano VM, Graf BK, Keene JS, Lange RH. Anterior cruciate ligament reconstruction. The American Journal of Sports Medicine. 1993; 21 (3): 415-418 [ Links ]
10. Gould JA. Fisioterapia na Ortopedia e na medicina do Esporte. São Paulo: Manole; 1993. [ Links ]
11. Tureck S. Ortopedia: Princípios e suas Aplicações. São Paulo: Manole; 1991. [ Links ]
12. Proença A. Ortopedia traumatologia: noções essenciais. Imprensa da Universidade; 2008. [ Links ]
13. Hall CM, Brody LT, Taranto G. Exercício terapêutico:na busca da função. Guanabara Koogan; 2007. [ Links ]
14. Stefanowski J. Application of rule induction and rough sets to verification of magnetic resonance diagnosis. Fundamental Informatics. 2002; 53: 345-363 [ Links ]
15. Huston LJ, Greenfield ML, Wojtys EM. Anterior cruciate ligament injuries in the female athlete:Potential risk factors. Clin Orthop. 2000; 372: 50-63 [ Links ]
16. Griffin LY. Noncontact anterior cruciate ligament injuries risk factors and prevention strategies. J Am Acad Orthop Surg. 2000; 8 (3): 141-150 [ Links ]
17. Prodromos CC, Han Y, Rogowski J, Joyce B, Shi K. A meta-analysis of the incidence of anterior cruciate ligament tears as a function of gender, sport, and a knee injury-reduction regimen. Arthroscopy. 2007; 23: 1320-1325 [ Links ]
18. Brophy R, Silvers HJ, Gonzales T, Mandelbaum BR. Gender influences: the role of leg dominance in ACL injury among soccer players. Br J Sports Med. 2010; 44: 694-697 [ Links ]
19. Griffin LY. Understanding and Preventing Noncontact Anterior Cruciate Ligament Injuries: A Review of the Hunt Valley II Meeting, January 2005. Am J Sports Med. 2006 Sep; 34 (9): 1512-1532
20. Arliani G, Astur D, Kanas M, Kaleka C, Cohen M. Lesão do ligamento cruzado anterior: tratamento e reabilitação. Perspetivas e tendências atuais. Rev. bras. Ortop. 2012; 47 (2) [ Links ]
21. Mey Y. Clinical characteristics of 4355 patients with anterior cruciate ligament injury. Chin Med J (Engl). 2013; 126 (23): 4487-4492 [ Links ]
22. Ejerhed L, Kartus J, Sernert N, Köhler K, Karlsson J. Patellar tendon or semitendinosus tendon autografts for anterior cruciate ligament reconstruction? A prospective randomized study with a two-year follow-up. Am J Sports Med. 2003; 31 (1): 19-25 [ Links ]
23. Aglietti P, Giron F, Buzzi R, Biddau F, Sasso F. Anterior cruciate ligament reconstruction: bone-patellar tendon-bone compared with double semitendinosus and gracilis tendon grafts. A prospective, randomized clinical trial. J Bone Joint Surg Am. 2004; 86 (10): 2143-2155 [ Links ]
24. Boschin LC, Schuck GF, Oliveira G, Schmiedt I, Schwartsmann CR. Artrotomia “versus” artroscopia: avaliação pós-operatória da reconstrução do ligamento cruzado anterior. Rev Bras Ortop. 37 (1/2): 23-30 [ Links ]
25. McRae S, Leiter J, McCormack R, Old J, Macdonald P. Ipsilateral versus contralateral hamstring grafts in anterior cruciate ligament reconstruction: a prospective randomized trial. J Sports Med. 2013; 41 (11): 2492-2499 [ Links ]
26. Leys T, Salmon L, Waller A, Linklater J, Pinczewski L. Clinical results and risk factors for reinjury 15 years after anterior cruciate ligament reconstruction: a prospective study of hamstring and patellar tendon grafts. Am J Sports Med. 2012; 40 (3): 595-605 [ Links ]
27. Struewer J, Ziring E, Oberkircher L, Schüttler KF, Efe T. Isolated anterior cruciate ligament reconstruction in patients aged fifty years: comparison of hamstring graft versus bone-patellar tendon-bone graft. Int Orthop. 2013; 37 (5): 809-817 [ Links ]
28. Mohtadi NG, Chan DS, Dainty KN, Whelan DB. Patellar tendon versus hamstring tendon autograft for anterior cruciate ligament rupture in adults. Cochrane Database Syst Rev. 2011; 7 (9): 5960-5974 [ Links ]
29. Wipfler B, Donner S, Zechmann CM, Springer J, Siebold R, Paessler HH. Anterior cruciate ligament reconstruction using patellar tendon versus hamstring tendon: a prospective comparative study with 9-year follow-up. Arthroscopy. 2011; 27 (5): 653-665 [ Links ]
Conflito de interesse:
Nada a declarar
Ana Alexandra da Costa Pinheiro,
Serviço de Ortopedia e Traumatologia da Unidade Local de Saúde do Alto Minho
Estrada de Santa Luzia
4901-858 Viana do Castelo ]]>
Telefone: 258802100
ana.alexandra.pinheiro@gmail.com
Data de Submissão: 2015-03-15
Data de Revisão: 2015-09-15
Data de Aceitação: 2016-03-25
]]>