Estabilização Rígida Percutânea em Fraturas Proximais do Úmero - Porquê, Quando e Como?
Sérgio AzevedoI; Manuel BrandãoI; Ana BiaI; Rodriguez de SousaI
I. Hospital Cuf Torres Vedras.
RESUMO
]]> Objetivo:Partilhar a nossa experiência no tratamento de fraturas proximais do úmero através de estabilização rígida com placa por via percutânea. Em alinhamento com a opinião de outros autores, as fraturas em 2 e 3 partes de Neer poderão beneficiar muito de uma osteossíntese rígida minimamente invasiva.
Material e métodos:
Análise retrospetiva de 48 doentes submetidos a osteossíntese rígida percutânea por fratura proximal do úmero em 2 e 3 partes de Neer, entre 2008 e 2016, com follow-up médio de 24,4 meses.
O protocolo cirúrgico e de reabilitação foi igual em todos os casos. Avaliámos os nossos resultados através do Score Quick Dash (QDS), Score de Constant (CS), avaliação radiográfica (falência de osteossíntese, perdas de redução, posição da placa, tempo de consolidação, incidência de necrose avascular), complicações neurológicas e infeciosas.
Resultados:
Avaliámos 48 doentes com idade média de 66 anos (desvio padrão ± 13,98). No QDS obtivemos uma média de 20 (desvio padrão ± 11,48). Obtivemos um Score Constant médio de 78 (desvio padrão ± 12,8). Não se registou nenhuma complicação grave.
Conclusões:
Neste tipo de fraturas, a osteossíntese rígida minimamente invasiva permite uma excelente redução anatómica, uma excelente fixação e uma baixa taxa de complicações.
Os nossos resultados vão ao encontro daqueles já previamente publicados em termos de resultado final.
]]> A ausência de estudo comparativo relativamente à via clássica delto-pectoral, é uma limitação deste trabalho.Palavras chave: Fraturas proximais do úmero, Estabilização rígida percutânea.
ABSTRACT
We intend to share our experience on percutaneous rigid stabilization of proximal humeral fractures. As mentioned by several authors, the 2 and 3 part fractures of Neer classification, could have a major benefit with this method.
Materials and methods:
Retrospective analysis of 48 patients submitted to percutaneous rigid stabilization of proximal humeral fracture (2 and 3 parts of Neer), between 2008 and 2016 with a mean follow-up of 24,4 months.
The surgical and rehabilitation protocol were the same at all cases.
Clinical evaluation by Quick Dash (QDS) and Constant Scores (CS), radiographic evaluation (implant failure, lost of reductions, plate positioning, consolidation time, avascular necrosis index), neurologic and infectious complications.
Results:
]]> Mean age of 66 years old (standard deviation ± 13,98).Mean QDS of 20 (standard deviation ± 11,48).
Mean CS of 78 (standard deviation ± 12,8).
Didn’t report any major complication.
Conclusions:
Regarding these type of fractures, the percutaneous rigid stabilization allows an excellent anatomical reduction, excellent fracture fixation and a low index of complications.
Our results are according those previously reported considering the final outcomes.
The absence of a comparative study with the classic delto-pectoral approach is a limitation of this study.
Key words: Proximal humeral fractures, Percutaneous rigid stabilization.
]]> INTRODUÇÃO
As fraturas proximais do úmero continuam a ser um desafio terapêutico importante.
A complexidade da fratura, a idade do paciente, o grau funcional pré-existente e expectativas de tratamento, a integridade da coifa, a panóplia de técnicas cirúrgicas disponíveis e a experiência do cirurgião, tornam a decisão terapêutica complexa1,2,5. O princípio fundamental no tratamento destas fraturas, quando avaliadas por imagem, além da competência da coifa dos rotadores que determina todo o resultado funcional final, é a possibilidade de reconstrução anatómica da fratura e uma reabilitação precoce.
Contudo, apesar da obtenção de uma reconstrução anatómica, o grau de estabilidade interfragmentária determina de forma decisiva o processo de reabilitação destes pacientes1,3,4,5.
A osteossíntese rígida com placas de estabilidade angular por via aberta delto-pectoral constitui a via clássica para o tratamento destas fraturas mas implicando maior diferenciação técnica da anatomia, maior disseção cirúrgica e maior tempo de exposição operatória. As complicações desta abordagem não são desprezíveis, nomeadamente a fibrose capsular e a consequente rigidez articular, o compromisso da artéria circunflexa anterior e a consequente necrose avascular da cabeça umeral, a pseudoartrose e a infeção4,5.
As técnicas de estabilização percutânea não rígidas continuam a estar associadas a maior taxa de complicações, nomeadamente infeção, perda de redução, pseudoartrose e migração do material de osteossíntese6,7. Determinam uma estabilização das fraturas menos rígida com consequente necessidade de imobilização mais prolongada e maior probabilidade de rigidez articular.
Apesar da necessidade de redução aberta e osteossíntese/artroplastia em grande parte das fraturas proximais do úmero, no grupo específico das fraturas em 2 partes e em algumas em 3 partes de Neer, outra abordagem poderá ser preferencial. De facto, e de acordo com o que já foi descrito por vários autores8,9,10,11,12,13, considera-se que o tratamento por osteossíntese rígida via percutânea oferece todas as vantagens em termos de resultado funcional e evita todas as desvantagens da via aberta e/ou osteossínteses não rígidas.
Em alinhamento com estes autores, todas as fraturas passíveis de serem tratadas por redução incruenta, poderão beneficiar de uma osteossíntese rígida que permita uma recuperação funcional precoce com uma menor taxa de complicações.
Com base nestes pressupostos, procedemos a uma revisão retrospectiva de todos os pacientes tratados por osteossíntese rígida com placa PHILOS15 percutânea em fraturas em 2 partes de Neer (Troquiter descoaptado; Troquiter descoaptado e colo cirúrgico “in situ”; Troquiter coaptado e colo cirúrgico descoaptado passível de redução incruenta) e em 3 partes de Neer (Troquiter e colo cirúrgico descoaptados mas o último passível de redução incruenta).
]]> MATERIAL E MÉTODOS
Efetuou-se uma análise retrospetiva dos processos clínicos de todos os pacientes submetidos a tratamento cirúrgico por fratura proximal do úmero, entre 2008 e 2016.
Foram incluídos 48 doentes com fraturas documentadas por Tomografia Axial Computorizada e classificadas de acordo com a classificação de Neer, nos seguintes subtipos:
O tempo de demora média entre a fratura e a cirurgia foi de 3 dias (mínimo 0 dias, máximo 6 dias).
]]> Todos os pacientes foram operados por dois cirurgiões autores deste estudo.Em todos os casos a técnica cirúrgica foi realizada sob anestesia geral, com o paciente em posição semi-sentado e sob intensificador de imagem.
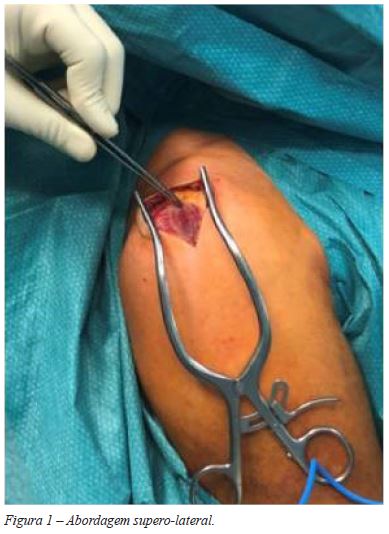
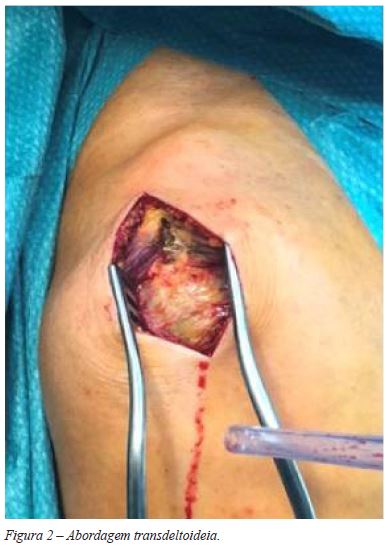
Em todos os casos preconizámos uma abordagem supero-lateral transdeltoideia (Figuras 1 e 2).

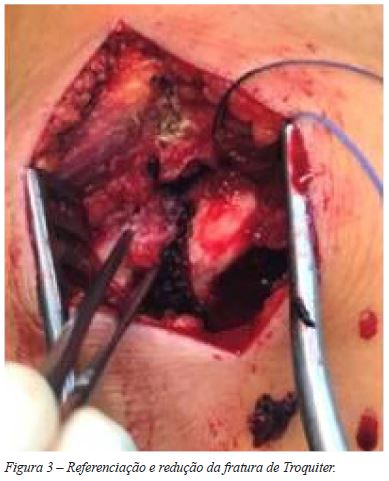
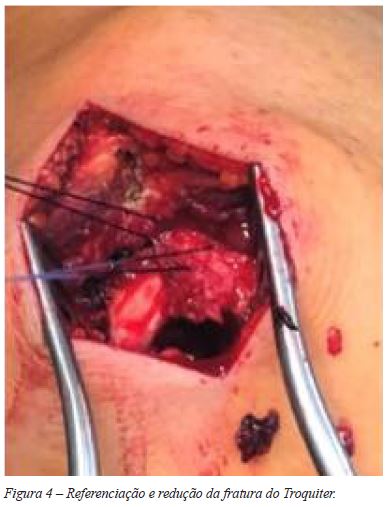
]]> Quando necessária, a fratura do Troquiter foi reduzida e fixada de forma direta, com suturas transósseas e fios de Kirschner (Figuras 3, 4 e 5).
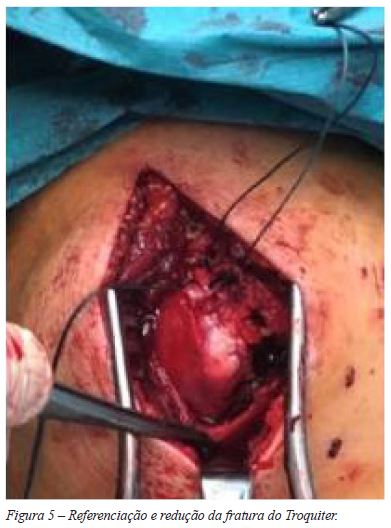
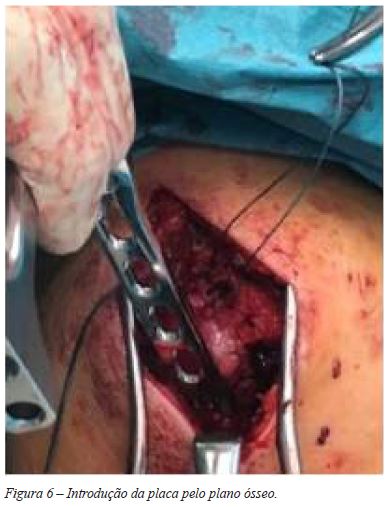
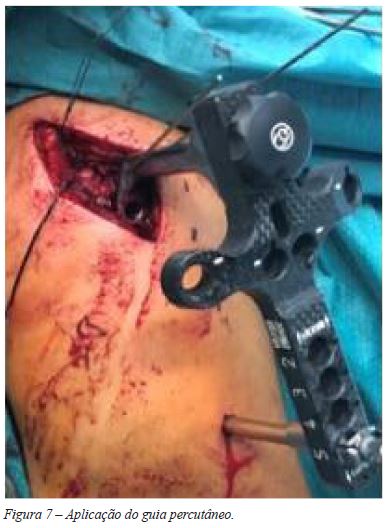
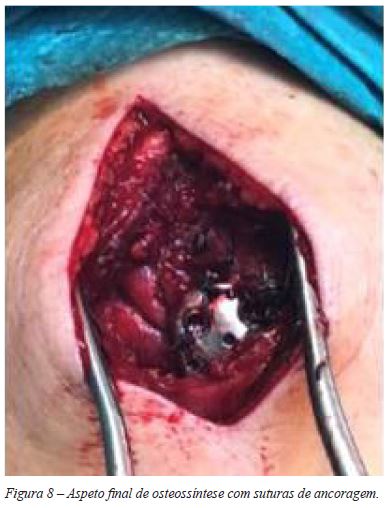
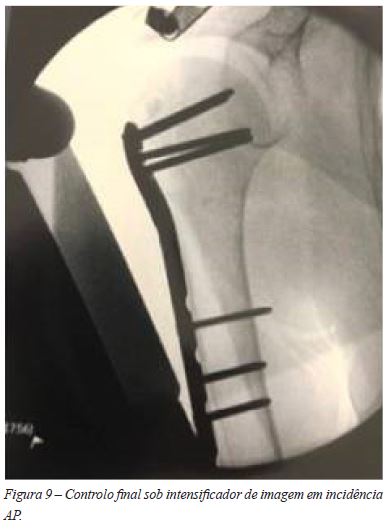
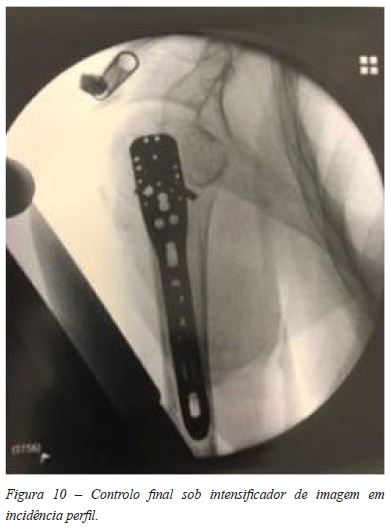
A aplicação da placa por via percutânea foi executada pelo plano ósseo e centrada nos 2 planos (Figura 6). Usámos em todos os casos uma placa PHILOS Depuy-Synthes15 de 5 orifícios distais ( 4 parafusos epifisários proximais e 3 parafusos diafisários distais) aplicada com guia percutâneo. (Figuras 7, 8, 9 e 10).
]]>
O protocolo de reabilitação foi o mesmo em todos os casos:
Todos os casos foram avaliados por uma Ortopedista que não participou diretamente no tratamento destes pacientes, tendo sido feito um follow-up médio de 24,4 meses(mínimo de 12 meses e máximo de 36 meses) Avaliámos os nossos resultados através de:
2.1 CS < 30 considerado insatisfatório
2.2 CS entre 30-39 considerado razoável
2.3 CS entre 40-59 considerado bom
2.4 CS entre 60-69 considerado muito bom
2.5 CS >70 considerado excelente
3. Avaliação radiográfica com foco em:
3.1. Falências da osteossíntese (fraturada placa, migração de parafusos);
3.2. Perdas de redução (perda de redução do Troquiter pela distância cabeça-tuberosidade e nas fraturas com envolvimento do colo cirúrgico potenciais alterações do angulo diáfise-cabeça entre o controlo radiográfico ao primeiro dia e aos 3 meses após a cirurgia).
3.3. posição da placa segundo os princípios da AO Foundation (entre 2-4mm posterior à goteira bicipital e entre 5-7mm distal ao topo do Troquiter);
3.4. tempo de consolidação da fractura (avaliada por critérios radiográficos e incidência AP + axilar)
5. Complicações neurológicas (avaliação clínica).
6. Complicações infeciosas.
7. Rigidez
RESULTADOS
Avaliámos 48 doentes com idade média de 66 anos (desvio padrão ± 13,98).
No QDS obtivemos uma média de 20 (desvio padrão ± 11,48).
Obtivemos um score Constant médio de 78 (desvio padrão ± 12,8).
Destes 48 casos, 62,5% (30 casos) foram considerados excelentes, 20,8% (10 casos) considerados muito bons, 12,5% (6 casos) considerados bons e 4,1% (2 casos) considerados razoáveis.
]]> O tempo médio de consolidação das fraturas foi de 10 semanas (desvio padrão ± 11,69).Não se registou nenhum caso de falência da osteossíntese nem de perda de redução pósosteossíntese.
Em todos os casos a posição da placa foi dentro dos parâmetros exigidos, não se tendo reportado nenhum caso de Conflito Subacromial.
Não se registou nenhum caso de protusão dos parafusos na cabeça umeral.
Não procedemos à remoção do material de osteossíntese em nenhum caso.
Não se verificou nenhuma complicação neurológica nem de necrose asséptica capital.
Registámos 2 casos de infeção superficial da ferida operatória, que resolveram de forma conservadora através de antiobioterapia oral.
Apenas um caso desenvolveu quadro álgico intenso às 2 semanas de operado, clinicamente compatível com quadro de Capsulite em fase inflamatória aguda, que reverteu completamente em 3 dias após a administração de Betametasona 14mg por via intra-muscular.
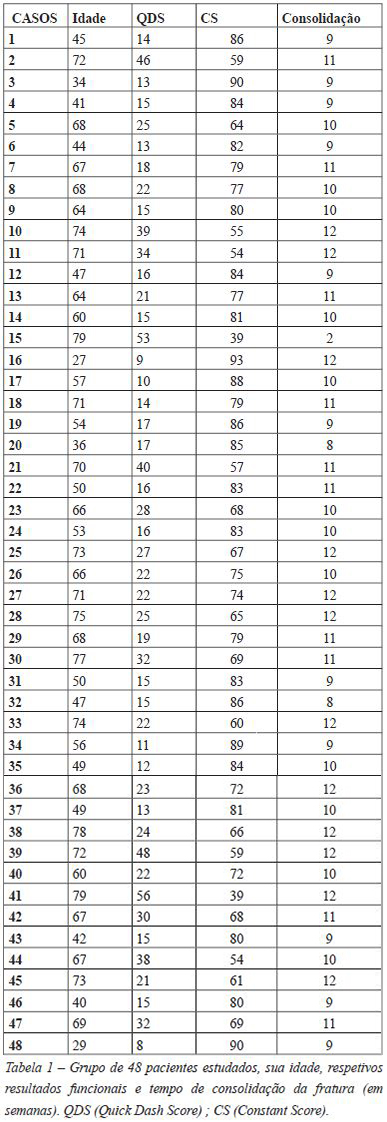
Na Tabela 1, encontram-se discriminados os resultados considerados mais importantes nesta série de doentes estudada.
]]>
DISCUSSÃO
A osteossíntese rígida com placa de estabilidade angular das fraturas proximais do úmero continua a ser o “gold standard” nos casos passíveis de reconstrução, não associados a alterações degenerativas gleno-umerais e com coifa íntegra1,3,4,5.
A possibilidade de associar esta filosofia a um método minimamente invasivo, faz, na nossa opinião e em alinhamento com a experiência de outros autores8,9,10,11,12,13, todo o sentido de forma a permitir todas as vantagens da osteossíntese rígida evitando todas as complicações de uma dissecção cirúrgica mais invasiva10,13.
Na nossa experiência, a abordagem minimamente invasiva é exigente mas de fácil execução, permitindo uma exposição proximal adequada ao tratamento deste tipo de fraturas. Na nossa opinião a abordagem das fraturas do troquiter é extremamente facilitada por se tratar de uma via direta, facilitando a sua referenciação e redução. Por outro lado, a colocação da placa é muito facilitada por esta via superior transdeltoideia.
O uso de placas com 5 orifícios permitiu, na população estudada, a sua fixação distal longe da zona de passagem do nervo axilar e dos seus ramos, não se tendo verificado complicações neurológicas nos doentes operados8.
Apesar da idade não ser um fator decisivo neste tipo de abordagem, verificámos que os resultados bons e razoáveis ocorreram em doentes com idade média de 73 anos (67-79) que relacionamos com alterações degenerativas da coifa dos rotadores.
]]>CONCLUSÃO
Acumulando uma experiência longa no tratamento de fraturas proximais do úmero, fomos percebendo que esta técnica minimamente invasiva poderia oferecer benefícios importantes neste grupo particular da classificação de Neer.
Os nossos resultados vão ao encontro daqueles já previamente publicados em termos de resultado final8,9,10,11,12,13.
Perante as fraturas descoaptadas do Troquiter e aquelas associadas a fratura do Colo Cirúrgico (coaptada ou passível de redução incruenta), a técnica minimamente invasiva permite uma redução anatómica sobreponível àquele obtido por via aberta8,9,11.
Trata-se de uma técnica cirúrgica simples que unifica todas as vantagens de uma osteossíntese rígida proporcionadas por uma abordagem menos agressiva e implicando uma menor disseção de partes moles e menor risco de necrose avascular da cabeça umeral9,10,11.
A idade e a correspondente qualidade da coifa parecem ter um papel determinante no resultado funcional final, independentemente do tipo de via de abordagem.
Na nossa experiência, o tempo de Bloco Operatório consumido é inferior quando comparado com a via aberta, embora não tenhamos dados estatísticos para assim o inferir. De facto, uma maior rentabilização do tempo de utilização da Sala Operatória constitui um critério interessante já mencionado por vários autores13.
Da mesma forma, não obstante os resultados claramente positivos encontrados na população estudada, a ausência de estudo comparativo relativamente à via clássica delto-pectoral, é uma limitação deste trabalho.
]]> REFERÊNCIAS BIBLIOGRÁFICAS
1. Karataglis D, Stavridis SI, Petsatodis G. New trends in fixation of proximal humeral fractures: a review. Injury. 2011; 42 (4): 330-338 [ Links ]
2. Gradl G, Knobe M, Pape HC. Decision making in displaced fractures of the proximal humerus: fracture or surgeon based? . Int Orthop. 2015; 39 (2): 329-334 [ Links ]
3. Chudik SC, Weinhold P, Dahners LE. Fixed-angle plate fixation in simulated fractures of the proximal humerus: a biomechanical study of a new device. J Shoulder Elbow Surg. 2003; 12 (6): 578-588 [ Links ]
4. Bjorkenheim JM, Pajarinen J, Savolainen V. Internal fixation of proximal humeral fractures with a locking compression plate: a retrospective evaluation of 72 patients followed for a minimum of 1 year. Acta Orthop Scand. 2004; 75 (6): 741-745 [ Links ]
5. Sturzenegger M, Fornaro E, Jakob RP. Results of surgical tratment of multifragmented fractures of the humeral head. Arch Orthop Trauma Surg. 1982; 100 (4): 249-259 [ Links ]
6. Wong J, Newman JM, Gruson KI. Outcomes of intramedullary nailing for acute proximal umerus fractures: a systematic review. J Orthop Traumatol. 2016 Jun; 17 (2): 113-122
7. Wang G, Mao Z, Zhang L. Meta-analysis of locking plate versus intramedullary nail for treatment of proximal humeral fractures. J Orthop Surg Res. 2015; 10: 122 [ Links ]
8. Acklin YP, Stoffel K, Sommer C. A prospective analysis of the functional and radiologic outcomes of minimally invasive plating in proximal humerus fractures. Injury. 2013; 44 (4): 456-460 [ Links ]
9. Falez F, Papalia M, Greco A. Minimally invasive plate osteosynthesis in proximal humeral fractures:1- year results of a prospective multicenter study. Int Orthop. 2016 Mar; 40 (3): 579-585
]]>10. Lin T, Xiao B, Ma X. Minimally invasive plate osteosynthesis with a locking compression plate is superior to open reduction and internal fixation in the management of the proximal humerus fractures. BMC Musculoskelet Disord. 2014; 15: 206 [ Links ]
11. Sohn HS, Shin SJ. Minimally invasive plate osteosynthesis for proximal humeral fractures: clinical and radiologic outcomes according to fracture type. J Shoulder Elbow Surg. 2014; 23 (9): 1334-1340 [ Links ]
12. Koljonen PA, Fang C, Lau TW, Leung F, Cheung NW. Minimally invasive plate osteosynthesis for proximal humeral fractures. J Orthop Surg. 2015 Aug; 23 (2): 160-163
13. Zhao W, Zhang Y, Johansson D, Chen X, Zheng F, Li L. Comparison of minimally invasive percutaneous plate osteosynthesisand open reduction internal fixation on proximal humeral fracture in eldery patients: A systematic review and meta-analysis. Hindawi Biomed Research International. 2017; 2017: 3431609 [ Links ]
14. Booker S, Alfahad N, Scott M, Gooding B, Wallace WA. Use of scoring systems for assessing and reporting the outcome results from shoulder surgery and arthroplasty. World J Orthop. 2015 Mar; 6 (2): 244-251
15. Placa anatómica para osteossíntese de fraturas do úmero proximal desenvolvida e comercializada pela empresa Depuy-Synthes. 2019; [ Links ]
16. The Dash and Quick Dash. Disabilities of the arm, shoulder and hand. Outcome measures e-bulletin. Fall. 2012; [ Links ]
17. Vrotsou K, Ávila M, Machón M, Mateo-Abad M, Pardo Y, Garin O, et al. Constant-Murley score: systematic review and standardized evaluation in different shoulder pathologies. Quality of Life Research. 2018 Sep; 27 (9): 2217-2226
]]>Conflito de interesse:
Nada a declarar
Sérgio Azevedo
Urbanização das Portelinhas, Rua Além Mar nº2, 2560-401 Silveira
Telefone: 966959968
azevedo.sg@gmail.com
]]> Data de Submissão: 2018-04-05
Data de Revisão: 2018-11-28
Data de Aceitação: 2018-11-28
]]>