Predição de pré-eclâmpsia no primeiro trimestre em gravidezes de baixo risco: determinação do cut-off numa amostra da população portuguesa
First trimester prediction of pre-eclampsia in low risk pregnancies: determining the cut-off in a portuguese group
Natacha Oliveira*, Bruno Carrilho*, Ana Carocha*, Ana Teresa Martins**, Álvaro Cohen**, Isabel Martins**, Jader Cruz**, Ana Campos**
Centro Hospitalar Lisboa Central - Maternidade Dr. Alfredo da Costa
*Interno de Ginecologia Obstetricia, Maternidade Dr. Alfredo da Costa, Centro Hospitalar Lisboa Central
**Especialista em Ginecologia Obstetrícia, Maternidade Dr. Alfredo da Costa, Centro Hospitalar Lisboa Central
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
]]> Objective: We aimed to identify the cut-off for risk of pre-eclampsia (PE) in Portuguese population by applying the first trimester prediction model from Fetal Medicine Foundation (FMF) in a prospective enrolled cohort of low risk pregnant women.Population and methods: A prospective cohort of low risk singleton pregnancies underwent routine first-trimester screening from 2011 through 2013. Maternal characteristics, blood pressure, uterine artery Doppler, levels of pregnancy-associated plasma protein-A (PAPP-A) and free b-human chorionic gonadotropin were evaluated. The prediction of PE in first trimester was calculated through software Astraia, the outcome obtained from medical records and the cutoff value was subsequently calculated.
Results: Of the 273 enrolled patients, 7 (2.6%) developed PE. In first trimester women who developed PE presented higher uterine arteries resistance, represented by higher values of lowest and mean uterine pulsatility index, p <0.005. There was no statistical significance among the remaining maternal characteristics, body mass index, blood pressure and PAPP-A.
Using the FMF first trimester PE algorithm, an ideal cut-off of 0.045 (1/22) would correctly detect 71% women who developed PE for a 12% false positive rate and a likelihood ratio of 12.98 (area under the curve: 0.69; confidence interval 95%: 0.39-0.99). By applying the reported cutoff to our cohort, we would obtain 71.4% true positives, 88.3% true negatives, 11.4% false positives and 28.6% false negatives.
Conclusion: By applying a first trimester PE prediction model to low risk pregnancies derived from a Portuguese population, a significant proportion of patients would have been predicted as high risk. New larger studies are required to confirm the present findings.
Keywords: Pre-eclampsia; First trimester; Algorithm; Screening.
Introdução
A pré-eclâmpsia afeta 2% das gravidezes e constitui uma causa major de morbilidade e mortalidade materno-fetal1. Apesar da sua baixa incidência, o facto de contribuir em 15% para a incidência de parto pré-termo e em 9%-42%2 para a mortalidade materna justifica a necessidade de estratificação precoce do risco de desenvolvimento subsequente. A aplicação de algoritmos preditivos de pré-eclâmpsia no primeiro trimestre permite a identificação de grupos de risco, a instituição atempada de medidas profiláticas e a individualização da vigilância obstétrica.
Nos últimos anos, vários modelos preditivos de pré-eclâmpsia foram desenvolvidos no sentido de determinar desde o primeiro trimestre quais as mulheres em risco de desenvolvimento subsequente de pré-eclâmpsia3-14. A pré-eclâmpsia é uma doença multifatorial, razão pela qual os algoritmos que incluem múltiplas variáveis demonstraram melhor performance na identificação de grupos de risco3-14. A história materna isoladamente associa-se a uma taxa de deteção de 30%; quando associada a parâmetros biofísicos (incluindo pressão arterial média e estudo doppler das artérias uterinas) e bioquímicos a taxa de deteção aumenta significativamente para os 46,7-100% para pré-eclâmpsia precoce (<34 semanas) e 29,4-71,1% posteriormente a esta idade gestacional3-14. No entanto, um estudo previamente publicado demonstrou que a maioria dos algoritmos para predição de pré-eclâmpsia apresentam uma pior performance comparativamente ao estudo original, quando aplicados numa população com diferentes características15.
]]> O objetivo do presente estudo foi avaliar a performance do algoritmo da Fetal Medicine Foundation para predição de pré-eclâmpsia no primeiro trimestre em grávidas de baixo risco, numa amostra da população portuguesa e determinar qual o cut-off ideal para estratificação de risco de pré-eclâmpsia.Métodos
O presente estudo é um estudo prospetivo observacional, desenvolvido entre abril de 2011 e junho de 2013. Mulheres com gravidezes únicas de baixo risco com idades gestacionais compreendidas entre 11+0 e 13+6 semanas submetidas a rastreio combinado do primeiro trimestre, provenientes dos Centros de Saúde da área de referência da instituição, foram incluídas no estudo, após obtenção de consentimento informado. O presente estudo foi aprovado pela comissão de ética da instituição onde se realizou.
Um questionário foi aplicado presencialmente por dois investigadores treinados. Os dados avaliados foram: idade, altura, peso, raça, hábitos tabágicos, tipo de conceção (espontânea, procriação medicamente assistida), antecedentes pessoais (hipertensão arterial crónica, diabetes mellitus, doença renal crónica, trombofilia, síndrome de anticorpo anti-fosfolípido), medicação realizada (aspirina, anti-hipertensores), passado obstétrico (número de gravidezes anteriores, complicações hipertensivas, idade gestacional do diagnóstico da complicação, idade gestacional no parto, peso do recém-nascido) e antecedentes familiares (hipertensão arterial crónica em familiares 1º grau, história de pré-eclâmpsia na mãe ou irmã). O índice de massa corporal foi calculado com base na altura e peso referidos pela grávida. A pressão arterial (PA) foi avaliada com recurso a um dispositivo automático, com a grávida na posição sentada após 5 minutos de repouso, com os membros superiores ao nível do coração e utilizada uma braçadeira de acordo com a circunferência do braço. A PA foi avaliada duas vezes em ambos os membros superiores e calculada a pressão arterial média [pressão diastólica + 1/3 (pressão sistólica - pressão diastólica)]. Subsequentemente foi realizada uma ecografia por ecografistas certificados pela Fetal Medicine Foundation (www.fetalmedicine.com). Em cada ecografia foi confirmada a idade gestacional através da medição do comprimento crânio-caudal (CCC), confirmado o número de fetos, medida a translucência da nuca, estabelecida a corionicidade e excluídas anomalias fetais major ou alterações estruturais associadas a aneuploidias. O índice de pulsatilidade (IP) de ambas as artérias uterinas foi avaliado por ecografia Doppler transabdominal. Cada artéria uterina foi identificada através do mapeamento a cores do fluxo sanguíneo, a nível da crossa identificada a nível do púbis, tendo sido medida a onda de pulso após obtenção de 3 formatos de onda similares e calculado o IP para cada artéria uterina. O valor mínimo, médio e máximo do IP das duas artérias foram posteriormente determinados. Previamente à execução do rastreio ecográfico do primeiro trimestre ou posteriormente se não realizado antes, foi colhido sangue para doseamento da fração livre b da Hormona Gonadotrofina Coriónica (b-HCG) e Proteína A plasmática associada à gravidez (PAPP-A) para determinação do rastreio combinado de anomalias cromossómicas.
Após colheita de todos os parâmetros, estes foram incluídos no software Astraia e calculado o risco de pré-eclâmpsia total e pré-eclâmpsia precoce (<34 semanas). A fórmula utilizada para cálculo do risco de pré-eclâmpsia é a mesma disponibilizada pela Fetal Medicine Foundation (https://courses.fetalmedicine.com/calculator/pe). A fórmula descrita inclui o doseamento da hormona de crescimento placentar (PlGF), a qual não foi doseada no presente estudo, tendo o seu valor sido tratado como ausente.
A recolha de dados face ao diagnóstico posterior de pré-eclâmpsia, idade gestacional do diagnóstico, morbilidade materna, dados relativos ao parto e peso do recém-nascido foram obtidos pela consulta dos respetivos processos clínicos. Pré-eclâmpsia foi definida como a presença de 2 medições de pressão arterial sistólica ≥140 mmHg e/ou pressão arterial diastólica ≥90 mmHg, com um intervalo mínimo de 4 horas, associadas a uma proteinúria ≥300 mg numa urina de 24h ou + de proteínas na urina numa amostra isolada, numa gravidez com idade gestacional superior a 20 semanas, na presença ou não de sintomatologia (cefaleias, escotomas ou epigastralgias)16. Hipertensão gestacional foi definida como a presença de 2 medições de pressão arterial sistólica ≥ 140 mmHg e/ou pressão arterial diastólica ≥ 90 mmHg, na ausência de proteinúria significativa, após as 20 semanas de gravidez16. Eclâmpsia foi definida como aparecimento de crises tónico-clónicas, na ausência de outro fator causal. Hipertensão arterial crónica com pré-eclâmpsia sobreposta foi definida na presença de proteinúria como descrita anteriormente após as 20 semanas de gravidez, numa mulher com o diagnóstico de hipertensão arterial antes das 20 semanas.
Foram excluídas gravidezes múltiplas, mulheres com CCC superior a 84 mm no momento do recrutamento da amostra, diagnóstico de anomalias fetais major (definidas como aquelas que são letais ou necessitam de cirurgia pré-natal ou pós-natal) ou aneuploidias, aborto espontâneo ou parto inferior a 23 semanas de gestação, incapacidade para o diagnóstico seguro de pré-eclâmpsia e ausência de dados sobre o desfecho da gravidez.
Para análise estatística foi utilizado o teste de Mann-Whitney para comparação de varáveis quantitativas e o teste do Qui quadrado de Pearson ou teste exato de Fisher, quando aplicável, para comparação de variáveis categóricas. A performance do teste de rastreio foi analisada com recurso a Área sob a Curva e o valor cut-off obtido pela aplicação do índice de Youden (maior especificidade e sensibilidade). O software estatístico SPSS 14.0 (SPSS Inc. Chicago, Il, USA) foi utilizado para análise estatística. Um valor p inferior a 0,05 foi considerado estatisticamente significativo.
Resultados
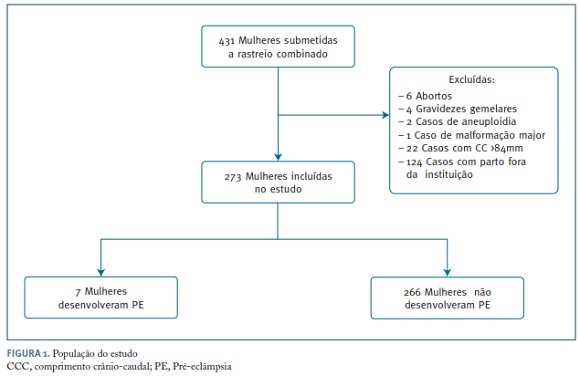
A população incluída no estudo encontra-se esquematizada na Figura 1. Das 273 mulheres que reuniram critérios de inclusão no estudo, 7 (2,6%) desenvolveram pré-eclâmpsia, tendo num dos casos o diagnóstico ocorrido antes das 34 semanas de gestação (incidência de pré-eclâmpsia precoce, 0,4%). As características demográficas da população encontram-se descritas no Quadro I. Não se observaram diferenças estatisticamente significativas relativamente à raça, paridade, antecedentes de hipertensão arterial crónica, antecedentes pessoais ou familiares de pré-eclâmpsia e índice de massa corporal entre o grupo que desenvolveu pré-eclâmpsia e o grupo controlo não afetado. O grupo que desenvolveu pré-eclâmpsia apresentou no primeiro trimestre maior resistência das artérias uterinas, traduzido em valores significativamente mais elevados de IP mínimos e médios das artérias uterinas e uma tendência para valores mais elevados de pressão arterial média e menores valores de PAPP-A, apesar de não estatisticamente significativo. Na Figura 2 encontram-se representados os diagramas referentes às variáveis contínuas pressão arterial média, IP mínimo e médio das artérias uterinas e PAPP-A.
]]>
A) Pressão arterial média, B) Índice de pulsatilidade mínimo e médio das artérias uterinas, C) Proteína A associada à gravidez em múltiplos da mediana; PE, Pré-eclâmpsia
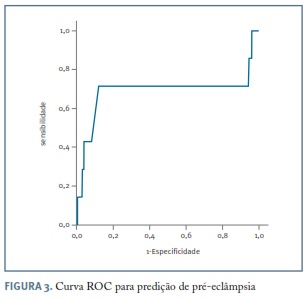
Na Figura 3 encontra-se representada a curva ROC referente à performance do algoritmo da FMF para predição de pré-eclâmpsia no 1º trimestre. A aplicação do algoritmo da FMF no 1º trimestre na população estudada resultou numa área sob a curva de 0,69 (intervalo de confiança a 95%, 0,39-0,99). Utilizando o cut-off obtido a partir da curva ROC baseado no índice de Youden, umcut-off de 1/22 (0,045) demonstrou uma sensibilidade de 71% para uma taxa de falsos positivos de 12%, uma razão de verosimilhança ( likelihood ratio - LR) positiva de 6,11 (IC 95%, 3,44-10,84) e negativa de 0,32 (IC 95%, 0,10-1,04), Quadro II. Aplicando o cut-off de 1/22, 36 doentes seriam consideradas em risco de desenvolvimento posterior de pré-eclâmpsia, das quais 71,4% seriam corretamente identificadas (verdadeiros positivos), 88,3% seriam corretamente identificadas como baixo risco (verdadeiros negativos), 11,4% não desenvolveram pré-eclâmpsia apesar de inicialmente consideradas de risco (falsos positivos) e 28,6% desenvolveram pré-eclâmpsia apesar de consideradas inicialmente de baixo risco (falsos negativos). Reduzindo os falsos positivos para 10% utilizado um cut-off de 1/18, obter-se-ia uma sensibilidade de 55%, um LR positivo de 5,41 (IC 95%, 2,09-13,97) e negativo de 0,62 (IC 95%, 0,33-1,18), Quadro II. Utilizando ambos os valores de cut-off, o caso de pré-eclâmpsia que ocorreu antes das 34 semanas seria corretamente previsto como alto risco.
]]>
Discussão
No presente estudo procurámos avaliar a performance do algoritmo do primeiro trimestre para predição de pré-eclâmpsia da Fetal Medicine Foundation numa amostra da população portuguesa e determinar qual o cut-off de risco associado a uma melhor sensibilidade e especificidade. Ao aplicarmos o algoritmo disponível no software Astraia para predição de pré-eclâmpsia no primeiro trimestre, em grávidas de baixo risco, seria possível detetar 71% dos casos de pré-eclâmpsia para uma taxa de falsos positivos de 12%, enquanto reduzindo a taxa de falsos positivos para 8%, a taxa de deteção seria de 45%.
No presente estudo, a incidência de pré-eclâmpsia foi de 2,6%, o que está de acordo com a incidência reportada na literatura 1,2. Vários estudos previamente realizados demonstraram que características maternas como a presença de hipertensão arterial crónica, diabetes mellitus, raça africana, peso materno aumentado, lúpus eritematoso sistémico ou síndrome de anticorpo anti-fosfolípido, antecedentes pessoais e familiares de pré-eclâmpsia se encontram associados a um risco acrescido de pré-eclâmpsia2-15. No presente estudo não se observaram diferenças estatisticamente significativas relativamente às características maternas previamente descritas, entre as doentes que desenvolveram pré-eclâmpsia comparativamente ao grupo controlo não afetado. Uma das razões para a baixa representatividade de fatores de risco entre os grupos, tais como hipertensão arterial crónica ou diabetes, deve-se ao facto das gravidezes incluídas no estudo serem de baixo risco. A ausência de diferença estatisticamente significativa para as diversas características em foco muito provavelmente deve-se à reduzida dimensão da amostra e baixa representatividade das mesmas nos dois grupos, não podendo ser concluída uma ausência de associação. De forma similar, vários estudos demostraram que o desenvolvimento posterior de pré-eclâmpsia se associa a valores mais elevados de pressão arterial média e maior resistência das artérias uterinas, traduzida num maior índice de pulsatilidade, bem como menores valores de PAPP-A no primeiro trimestre 3-9,11,12,17-19. O presente estudo corroborou os achados para as variáveis contínuas já previamente demonstrados, observando-se uma maior resistência das artérias uterinas, com valores mínimos e médios mais elevados do IP das artérias uterinas, tendo este resultado sido estatisticamente significativo. Apesar de ausência de poder estatístico, justificável pela reduzida dimensão da amostra, observou-se igualmente uma maior pressão arterial média e menores valores de PAPP-A no primeiro trimestre no grupo que veio a desenvolver pré-eclâmpsia comparativamente ao grupo controlo não afetado.
Em 2013 Akolekar et al4 através da aplicação de um algoritmo no primeiro trimestre para predição de pré-eclâmpsia incluíndo características maternas, biofísicas (pressão arterial média e doppler das artérias uterinas) e PAPP-A obteve uma taxa de deteção de 92,5% (cut-off 1:216) e 59,9% (cut-off 1:12) para pré-eclâmpsia precoce e total, respetivamente, para uma taxa de falsos positivos de 10%. Do mesmo grupo de estudo, Poon et al12 pela utilização dos mesmos parâmetros obteve uma taxa de deteção no primeiro trimestre de 94,6 (área sob a curva 0,96, 95% IC, 81,8-99,2) para pré-eclâmpsia precoce. Neste estudo a utilização de PAPP-A não se associou a uma maior taxa de deteção de pré-eclâmpsia tardia, tendo a maior predição resultado da combinação de fatores maternos e biofísicos, traduzida numa sensibilidade de 57% para uma especificidade de 90% (área sob a curva 0,86, 95% IC, 48,0-65,7). Scazzocchio et al9, numa população diferente, pela utilização dos mesmos parâmetros no primeiro trimestre, mas através da aplicação de um algoritmo diferente obteve uma taxa de deteção de 80,8% para predição de pré-eclâmpsia precoce (cut-off 1/178; área sob a curva 0,95; 95% IC, 0,94-0,98) e 39,6% para predição de pré-eclâmpsia tardia (cut-off; 1/18; área sob a curva 0,71, 95% IC 0,66-0,76), para uma taxa de falsos positivos de 10%. A taxa de deteção obtida no presente estudo para predição de pré-eclâmpsia total foi de 71% para uma especificidade de 88%, mas considerando os valores de referência próximos dos utilizados nos diversos estudos da FMF, a obtenção de uma taxa de deteção de 43% encontra-se próximo dos valores reportados4,12. No entanto, a área sob a curva obtida foi de 0,69 (intervalo de confiança a 95%, 0,39-0,99), inferior às reportadas4,12.
Pela primeira vez um estudo procurou determinar a performance numa amostra da população portuguesa de um algoritmo criado para predição de pré-eclâmpsia no primeiro trimestre. Um aspeto positivo do nosso estudo prende-se com o facto da metodologia utilizada ter sido a mesma da utilizada pela Fetal Medicine Foundation no estudo que teve como base o algoritmo em análise, permitindo assim verificar corretamente a sua performance e limitando erros de colheita de dados. Por outro lado, utilizando o valor de risco obtido para cada doente através da introdução dos dados no software Astraia, minimizou o erro de cálculo que poderia surgir pela aplicação do algoritmo da FMF para predição de pré-eclâmpsia, o qual apresenta várias fórmulas intermédias para cálculo de cada variável.
A reduzida dimensão da amostra constitui uma limitação ao presente estudo. A amostra final representa apenas 63,3% dos casos inicialmente incluídos, sendo justificável em parte por em 28,8% dos casos o parto ter ocorrido fora da instituição. Tal facto deveu-se a uma restruturação das áreas de referenciação aos hospitais e consequentemente uma parte significativa das doentes inicialmente referenciadas para realização de rastreio combinado do primeiro trimestre na instituição onde se realizou o estudo, terem sido posteriormente referenciadas para outra instituição no momento do parto. Por outro lado, dada a baixa prevalência de pré-eclâmpsia precoce e dado o tamanho amostral reduzido, não foi possível avaliar a performance do algoritmo da FMF na predição de pré-eclâmpsia precoce. Por outro lado, o valor de PlGF não foi incluído no cálculo, como publicado originalmente no estudo da FMF, por o doseamento do mesmo não se encontrar disponível na instituição no momento da realização do estudo. A ausência da inclusão do doseamento de PlGF no cálculo de predição de pré-eclâmpsia pode ter influenciado negativamente a performance do algoritmo.
]]> O presente estudo sugere que a aplicação de um algoritmo no primeiro trimestre para predição de pré-eclâmpsia, utilizando variáveis facilmente obtidas numa avaliação obstétrica de rotina e no rastreio combinado do primeiro trimestre, permite uma deteção significativa de casos de risco (71%) para uma taxa de falsos positivos de 12%. Estudos subsequentes, de maiores dimensões e incluindo gravidezes de risco são necessários para comprovar os presentes resultados.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Scazzocchio E, Figueras F. Contemporary prediction of preeclampsia. Curr Opin Obstet Gynecol 2011. 23:65-71. [ Links ]
2. Steegers EAP, Dadelszen Pv, Duvekot JJ, Pijnenborg R. 2010. Pre-eclampsia. Lancet 2010;376:631-44.
3. Akolekar R, Syngelaki A, Sarquis R, Zvanca M, Nicolaides K. Prediction of early, intermediate and late pre-eclampsia from maternal factors, biophysical and biochemical markers at 11-13 weeks. Prenat Diagn 2011; 31: 66-74. [ Links ]
4. Akolekar R, Syngelaki A, Poon L, Wright D, Nicolaides K. Competing Risks Model in Early Screening for Preeclampsia by Biophysical and Biochemical Markers. Fetal Diagn Ther 2013; 33: 8-15. [ Links ]
]]>5. Audibert F, Boucoiran I, An N, Aleksandrov N, Delvin E, Bujold E, Rey E. Screening for preeclampsia using first-trimester serum markers and uterine artery Doppler in nulliparous women. Am J Obstet Gynecol 2010; 203: 383.e1-8. [ Links ]
6. Parra-Cordero M, Rodrigo R, Barja P, Bosco C, Rencoret G, Sepúlveda-Martinez A, Quezada S. Prediction of early and late pre-eclampsia from maternal characteristics, uterine artery Doppler and markers of vasculogenesis during first trimester of pregnancy. Ultrasound Obstet Gynecol 2013; 41: 538-44. [ Links ]
7. Poon L, Karagiannis G, Leal A, Romero X, Nicolaides K. Hypertensive disorders in pregnancy: screening by uterine artery Doppler imaging and blood pressure at 11-13 weeks. Ultrasound Obstet Gynecol 2009; 34: 497-02 [ Links ]
8. Herraiz I, Arbués J, Camaño I, Gómez-Montes E, Grañeras A, Galindo A. Application of a first-trimester prediction model for pre-eclampsia based on uterine arteries and maternal history in high-risk pregnancies. Prenat Diagn 2009; 29: 1123-29 [ Links ]
9. Scazzocchio E, Figueras F, Crispi F, Meler E, Masoller N, Mula R, Gratacos E. Performance of a first-trimester screening of preeclampsia in a routine care low-risk setting. Am J Obstet Gynecol 2013; 208: 203e.1-10 [ Links ]
10. Park F, Leung C, Poon L, Williams P, Rothwell S, Hyett J. Clinical evaluation of a first trimester algorithm predicting the risk of hypertensive disease of pregnancy. Australian and New Zealand Journal of Obstetrics and Gynecology 2013; 53: 532-39. [ Links ]
11. Odibo A, Zhong Y, Goetzinger K, Odibo L, Bick J, Bower C, Nelson D. First-trimester placental protein-13, PAPP-A, uterine artery Doppler and maternal characteristics in the prediction of pre-eclampsia. Placenta 2011; 32:598-02. [ Links ]
12. Poon L, Stratieva V, Piras S, Piri S, Nicolaides K. Hypertensive disorders in pregnancy: combined screening by uterine artery Doppler, blood pressure and serum PAPP-A at 11-13 weeks. Prenat Diagn 2010; 30: 216-23. [ Links ]
13. Kuc S, Koster M, Franx A, Schielen P, Visser G. Maternal Characteristics. Mean Arterial Pressure and Serum Markers in Early Prediction of Preeclampsia. Plos ONE 2013; 8: e63546. [ Links ]
14. Caradeux J, Serra R, Nien JK, Pérez-Sepulveda A, Schepeler M, Guerra F, Gutiérrez J, Martínez J, Cabrera C, Figueroa-Diesel H, Soothil P, Illanes SE. First trimester prediction of early onset preeclampsia using demographic, clinical, and sonographic data: a cohort study. Prenat Diagn 2013; 33: 732-6. [ Links ]
15. Oliveira N, Magder LS, Blitzer MG, Baschat AA. First Trimester Prediction of Preeclampsia: External validity of algorithms in a prospectively enrolled cohort. Ultrasound Obstet Gynecol 2014; 44: 286-92. [ Links ]
16. Brown MA, Lindheimer MD, de Swiet M, Van Assche A, Moutquin Jm. The classification and diagnosis of the hypertensive disorders of pregnancy: statement from the International Society for the Study of Hypertension in Pregnancy (ISSHP). Hypertens Pregnancy 2011; 20: IX-XIV. [ Links ]
17. Poon LC, Maiz N, Valencia C, Nicolaides KH. First-trimester maternal serum pregnancy-associated plasma protein-A and pre-eclampsia. Ultrasound Obstet Gynecol 2009; 33: 22-33. [ Links ]
18. Poon LC, Staboulidou I, Maiz N, Plasencia W, Nicolaides KH. Hypertensive disorders in pregnancy: screening by uterine artery Doppler at 11-13 weeks. Ultrasound Obstet Gynecol 2009; 34: 142-48. [ Links ]
19. Poon LC, Kametas NA, Pandeva I, Valencia C, Nicolaides KH. Mean arterial blood pressure at 11+0 to 13+6 Weeks in the Prediction of Preeclampsia. Hypertension 2008; 51: 1027-33. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Natacha Oliveira
]]> Centro Hospitalar de Lisboa CentralMaternidade Dr. Alfredo da Costa
Rua Viriato
1069-089 Lisboa
E-mail: natacha_oliveira@hotmail.com
Recebido em: 02-10-2014
Aceite para publicação: 25-05-2015
]]>