Gravidez na doença renal crónica: da diálise peritoneal à hemodiálise
Pregnancy in chronic kidney disease: from peritoneal dialysis to hemodialysis
Pedro Viana Pinto*, Ana Teresa Nunes*, Carla Santos**, Patricia Martins**, Ana Paula Machado***, Nuno Montenegro****
Serviço de Ginecologia/Obstetrícia, Centro Hospitalar São João
*Interno de Formacão Específica de Ginecologia e Obstetrícia, Centro Hospitalar de São João
**Interno de Formacão Específica de Nefrologia, Centro Hospitalar São João
***Assistente hospitalar, Serviço Nefrologia, Centro Hospitalar São João
****Assistente hospitalar, Serviço Ginecologia e Obstetrícia, Centro Hospitalar São João
*****Diretor do Serviço de Ginecologia e Obstetrícia, Centro Hospitalar de São João; Subdiretor da Faculdade de Medicina da Universidade do Porto
]]> Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Overview and Aims: pregnancy in women with chronic kidney disease (CKD), particularly in terminal CKD, remains a rare event. There are scarce reports of pregnancy in women undergoing peritoneal dialysis. Our study aims to evaluate the outcomes of pregnancies in women with CKD diagnosed at Hospital São João during the study period.
Study design: retrospective case series.
Population: pregnant women with chronic kidney disease diagnosed between January 2005 and December 2013.
Methods: pregnancies in women with severe CKD (GFR <30mL in/1.73m2) were identified by using hospital electronic platforms with evaluation of maternal and fetal outcomes.
Results: during the study period 4 cases of pregnancy in women with CKD were identified, including one of a woman in peritoneal dialysis prior to pregnancy - case 1. Case 1 progressed to hemodialysis at 17 weeks (due to haemoperitoneum subsequent to trauma by the peritoneal dialysis catheter) and had an eutocic late preterm delivery at 35 weeks. Case 2 began hemodialysis at 22 weeks, and was submitted to urgent cesarean section at 29 weeks. Case 3 started hemodialysis at 21 weeks, having also undergone urgent cesarean section at 31 weeks. Case 4 began hemodialysis at 21 weeks, presenting with an episode of hepatotoxicity secondary to darbopoietin at 26 weeks. Delivery occurred by Caesarean section at 32 weeks.
Conclusion: despite the high fetal morbidity documented, with the strategies adopted there was no fetal or neonatal mortality. The monitoring of these pregnant in specialized consultation favored the positive outcomes.
Palavras-chave: Pregnancy; Hemodialysis; Chronic Kidney Disease; Peritoneal Dialysis.
Introdução
Provavelmente nenhum outro insulto fisiológico causa alterações tão marcadas na função renal como a gravidez. O volume renal aumenta cerca de 30%, a taxa de filtração glomerular aumenta (não por alterações histológicas ou do número de nefrónios mas pelo aumento do débito cardíaco e do fluxo sanguíneo renal e por uma menor resposta a vasopressores como a angiotensina 2, noradrenalina e vasopressina)1-5, sendo que a alcalose respiratória própria da gravidez e as maiores necessidades de hemoglobina impõem, também, uma maior exigência aos rins maternos1. Contudo, na presença de doença renal crónica (DRC) estas adaptações fisiológicas ficam comprometidas ou até impossibilitadas, tornando a gravidez nestas situações um desafio extremamente complexo6.
Mais de 40 anos após o primeiro caso descrito de gravidez numa mulher em diálise, a gravidez em mulheres com DRC grave continua um evento raro. Há poucos dados sobre a taxa de concepção nestas mulheres, sendo a maioria provenientes de bases de dados antigas. No entanto, é descrito um aumento significativo na taxa de concepção de mulheres em diálise - 0,9% em 1980 para 2,4% em 1998 - embora este valor possa estar subestimado dado que a maioria das gravidezes é diagnosticada apenas no segundo trimestre, com perda dos casos de abortamentos precoces7, 8.
A disfunção reprodutiva feminina nesta população é complexa e multi-factorial, envolvendo fatores fisiológicos, condições médicas associadas e fatores psicossociais. Em mulheres com insuficiência renal avançada a secreção de GnRH encontra-se alterada, bem como o pico de LH, embora os níveis de LH basais tendam a ser mais elevados, com a consequente falha na ovulação9-11. Os níveis de prolactina e a sua actividade biológica encontram-se aumentados nestas mulheres, com consequente diminuição da libido, infertilidade, amenorreia ou oligomenorreia e galactorreia12. A amenorreia surge tipicamente com taxas de filtração glomerulares (TFGe) menores que 5mL inuto8. Alterações secundárias na morfologia endometrial (atrofia ou alterações proliferativas) são, também, comuns e podem dificultar a implantação do blastocisto9. O transplante renal bem-sucedido repõe, na maioria dos casos, o ambiente hormonal necessário à reprodução12.
Os enormes avanços nos cuidados materno-fetais bem como na frequência e eficiência das técnicas substitutivas da função renal permitiram um aumento da sobrevida fetal de 20-23 % em 1980 para 75-80% atualmente13-17. A concepção bem como o desfecho favorável da gravidez são muito mais frequentes em mulheres com menos tempo em diálise, com manutenção de função renal residual e quando a gravidez se inicia antes da necessidade de diálise11,17. O fator prognóstico mais importante para os desfechos materno e fetal é o grau de comprometimento da função renal no momento da concepção18.
Nestas mulheres é essencial um controlo adequado das complicações clínicas associadas à doença renal independentemente da etiologia da mesma6. Apesar de toda a evolução na vigilância destas grávidas, a maioria dos recém-nascidos são prematuros (idade gestacional média de 32 semanas)19,20 e complicações como a doença hipertensiva da gravidez, a anemia, o hidrâmnios e a restrição de crescimento fetal são também frequentes17,20,21.
A gravidez bem-sucedida é possível com ambas as técnicas substitutivas da função renal. São, no entanto, menos frequentes os casos descritos na literatura de gravidez em mulheres em diálise peritoneal (DP)22. Neste trabalho, descrevemos uma série de casos de gravidezes em mulheres com DRC grave acompanhadas entre 2005 e 2013 no Centro Hospitalar São João, incluindo um caso de uma gravidez numa mulher já em diálise peritoneal antes da concepção.
Métodos
Foi realizado uma pesquisa sistemática na nossa instituição de todas as grávidas portadoras de doença renal crónica. Todas as mulheres portadoras de doença renal crónica grave (TFGe <30mL/ min/1,73m2) e com parto na nossa instituição foram incluídas. As mulheres expostas foram identificadas com recurso a uma base de dados electrónica e ao sistema informático da nossa instituição (OBSCARE®, SCLINICO®). Foram consultados os processos clínicos individuais de forma a identificar as características particulares dos casos em estudo, nomeadamente a doença renal de base, presença de outras co-morbilidades maternas associadas, a idade gestacional (IG) de diagnóstico de gravidez, a técnica de substituição renal utilizada e com que IG foi iniciada, presença de doença hipertensiva da gravidez (HTA gestacional, pré-eclâmpsia/eclâmpsia, síndrome HELLP), restrição crescimento fetal, hidrâmnios ou anemia, IG do parto, peso do recém-nascido, via de parto e principais complicações puerperais e neonatais.
]]> ResultadosDurante o período em estudo houve 24.308 partos na nossa instituição, tendo sido detectados 4 casos de grávidas com DRC severa com necessidade de técnicas de substituição renal (incidência - 1/6.077 nascimentos).
Caso 1
Primigesta, 37 anos, DRC terminal em DP desde os 33 anos após glomerulosclerose segmentar e focal diagnosticada aos 24 anos de idade. Aos 36 anos apresenta episódio de neuropatia óptica isquémica anterior, tratado sem sequelas.
Em Abril de 2013, apresentando um quadro de náuseas e vómitos recorre a urgência hospitalar tendo sido diagnosticada gravidez de 10 semanas. Nesta data apresentava-se com uma estratégia de DP de 3 permutas/dias (com 2L de dialisante Physioneal®), com boa adequação dialítica e diurese residual de 1000mL. A sua medicação crónica prévia ao diagnóstico de gravidez incluía rosuvastatina 20mg/d, alopurinol 100mg/d, sertralina 50mg/d, amitriptilina 10mg/d, darbopoietina, sulfato ferroso, ácido fólico e complexo multivitamínico do grupo B. Após diagnóstico de gravidez manteve apenas a sertralina 50mg/d, darbopoietina, sulfato ferroso, ácido fólico 5mg/d e complexo multivitamínico do grupo B, aos quais acrescentou o ácido acetilsalicílico 100mg/d, tendo sido aumentadas as permutas de DP para 4 vezes/dia. Foi orientada para vigilância em consulta multidisciplinar envolvendo Nefrologia, Obstetrícia e Nutrição.
Durante o primeiro trimestre apresentou duas infeções urinárias baixas não complicadas. Às 15 semanas de gestação apresentou um episódio de hemoperitoneu sem evidência de trauma pelo catéter de DP e com culturas de líquido peritoneal negativas. Fez amniocentese às 16 semanas por rastreio combinado de 1º trimestre positivo, sem intercorrências (cariótipo 46, XY).
Devido a queixas de distensão abdominal foi reduzido o volume de dialisante (1700ml) mas aumentada a frequência (5 vezes/dia) de modo a manter eficácia dialítica adequada. Às 17 semanas de gestação apresenta novo hemoperitoneu com documentação ecográfica de contacto entre catéter de DP com a serosa uterina. Neste contexto procedeu-se à remoção urgente do catéter de DP e iniciada hemodiálise por catéter tunelizado no mesmo dia. Duas semanas após o inicio de hemodiálise foi possível o início de punção da fistula arterio-venosa, já previamente intervencionada durante a gravidez na perspetiva de eventual necessidade de transição de diálise peritoneal para hemodiálise. A estratégia adotada consistiu em 24h/semana de diálise (4h/6 vezes por semana). Foi estimado um aumento de peso de 450g/semana, com controlo do mesmo com recurso a avaliação clínica regular, avaliações seriadas de BNP, bioimpedância e índices de volémia ecocardiográficos. O controlo tensional foi efetuado sem recurso a medicação anti-hipertensora até às 27 semanas, altura em que iniciou metildopa (750mg/d). Necessitou de aumento progressivo da dose de estimulador da eritropoiese (doses de darbopoietina de 100 mcg/semana no final da gravidez) de modo a que os níveis de hemoglobina (Hb) se mantivessem estáveis (Hb ~10g/ /dL). Durante o período em que realizou hemodiálise os níveis sanguíneos de ureia mantiveram-se <60mg/ /dL.
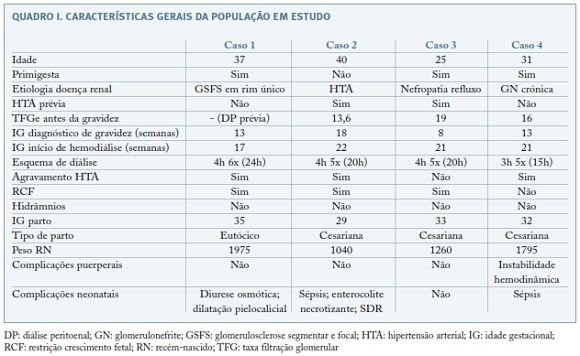
Às 27 semanas de gestação foi internada no serviço de Medicina Materno-Fetal no contexto de ameaça de parto pré-termo, tendo iniciado tocólise com nifedipina e ciclo de maturação pulmonar fetal com betametasona. Diagnosticada restrição de crescimento fetal às 32 semanas (percentil 5), com fluxometria umbilical e da artéria cerebral média normais. Às 35 semanas por HTA grave (apesar da terapêutica com metildopa 1500mg/d) com traçado cardiotocográfico suspeito (variabilidade longa reduzida sustentada) foi induzido o trabalho de parto, tendo tido um parto eutócico, com recém-nascido (RN) do sexo masculino com 1975g e índice de Apgar de 7/8 ao 1º/5º minutos (Quadro I). O RN apresentou diurese osmótica na dependência de azotemia materna, bem como uma dilatação pielocalicial ligeira à esquerda (5mm), tendo tido alta ao 18º dia de vida.
]]>
Teve alta ao 7º dia de puerpério em programa regular de hemodiálise 4 vezes/semana, tendo reiniciado DP 2 meses após o parto. Atualmente mantém DP com controlo adequado de volume e diurese residual de 1000mL.
Caso 2
Paciente de 40 anos de idade, gesta 7, 6 partos eutócicos, seguida por Nefrologia por DRC no contexto de nefroangiosclerose hipertensiva - suspeita de estenose da artéria renal (TFGe antes da gravidez de 13,6ml/ in/1,73m2). Em ecografia (Novembro de 2005) realizada para estudo da doença renal foi-lhe diagnosticada gravidez (cerca de 18 semanas). Foi alterada a medicação anti- hipertensora (suspendeu Enalapril) e orientada para consulta multidisciplinar de Obstetrícia e Nefrologia para acompanhamento especializado. Às 21 semanas foi internada por HTA crónica agravada (com agravamento da função renal), sem outras alterações analíticas. Apresentava anemia grave com necessidade de suporte transfusional. Foi conseguido controlo tensional satisfatório mas não se verificou recuperação da função renal tendo iniciado hemodiálise às 22 semanas - estratégia de 20h/semana (4h/5 vezes semana). Apesar da medicação anti-hipertensora (metildopa 1500g/d) e estratégia dialítica frequente apresentou controlo tensional sub-ótimo procedendo-se a internamento às 27 semanas para realização de ciclo de maturação pulmonar fetal com betametasona. Às 29 semanas tem parto por cesariana eletiva por mau controlo tensional associado a restrição crescimento fetal grave com alterações da fluxometria umbilical, com RN do sexo masculino, 1040g e índice de Apgar 8/9 ao 1º/5º minutos (Quadro I). O RN apresentou várias complicações no contexto de prematuridade, apresentando atualmente desenvolvimento psicomotor adequado. A mãe tem alta ao 6º dia de puerpério, medicada com lisinopril. Foi submetida a transplante renal em 2011 e transplectomizada um mês depois por infeção de hematoma (hemorragia no pós-transplante imediato), com segundo transplante, bem sucedido, em 2013.
Caso 3
Primigesta de 25 anos, com DRC secundária a nefropatia de refluxo, nefrectomia direita em 1996 e HTA. Gravidez diagnosticada às 8 semanas (Outubro de 2009), tendo sido encaminhada para consulta multidisciplinar de Obstetrícia e Nefrologia. Prevendo-se a necessidade de início de diálise a curto prazo (à data de diagnóstico de gravidez TFGe 19ml in/1,72m2) é construída fístula arterio-venosa, com falência primária desta. Às 20 semanas de gestação é internada por hipervolémia e agravamento da função renal com início de hemodiálise por catéter venoso central tunelizado. Tem alta às 22 semanas de gravidez, medicada com ácido acetilsalicílico (AAS) 100mg e metildopa 1500mg/d, com estratégia de diálise 20h/semana (4h/5 vezes semana), visando-se um aumento de peso seco de cerca 250-300g/semana. Às 29 semanas apresenta pielonefrite aguda por Escherichia coli com resolução com antibioterapia (ceftriaxone seguido de amoxicilina/ ácido clavulânico), sendo re-internada às 31 semanas por restrição de crescimento fetal com alterações fluxométricas. Faz ciclo de maturação pulmonar fetal com betametasona sendo submetida a cesariana emergente por estado fetal não tranquilizador às 31 semanas, com RN do sexo feminino, 1250g e índice de Apgar 8/9 ao 1º/5º minutos. O período neonatal evoluiu sem intercorrências. A mãe teve alta ao 5º dia de puerpério, tendo optado por iniciar diálise peritoneal (Quadro I). Foi transplantada 2 anos depois e apresenta boa função do aloenxerto.
Caso 4
Primigesta com 31 anos, com DRC secundária a glomerulopatia crónica não especificada, com uma TFGe antes da gravidez de 16ml in/1,72m2. Encaminhada para consulta multidisciplinar de Obstetrícia e Nefrologia às 13 semanas de gestação (Julho de 2010), sendo medicada com metildopa 500mg/d, suplementação de ferro, AAS 100mg id, ácido fólico 5mg id e darbopoietina 10µg/sem. Às 21 semanas de gestação, por agravamento da função renal, inicia hemodiálise por fístula arterio-venosa (15h - 3h/ 5 vezes semana) com um aumento de peso seco previsto de 500g/semana. Às 26 semanas é detectada citólise hepática com hiperbilirrubinemia, tendo sido internada para estudo. Realizou biópsia hepática que revelou apenas siderose nas células de Kupfer e, dada a melhoria analítica após suspensão de darbopoietina, foi presumida hepatite tóxica secundária este fármaco. Teve necessidade de suporte transfusional (6U de glóbulos rubros) durante a gravidez. Às 31 semanas foi reinternada por hipervolémia associada a infeção respiratória e agravamento do controlo tensional tendo sido medicada com amlodipina. Às 32 semanas, após completar maturação pulmonar fetal com betametasona, no contexto de hipervolémia e HTA graves e insuficiência respiratória, foi submetida a cesariana urgente com recém-nascido do sexo feminino, 1705g e índice de Apgar 8/8 ao 1º/5º minutos (Quadro I). O RN desenvolveu uma sépsis no período neonatal com posterior melhoria e recuperação. A doente permaneceu 24 horas em Unidade de Cuidados Intensivos, com alta hospitalar ao 11º dia de puerpério, após remoção de elevado volume de ultrafiltrado (13 L em 3 dias). Atualmente mantém-se em programa regular de hemodiálise, em lista de espera para transplante renal.
Discussão
Esta série de casos permite constatar que, apesar da elevada morbilidade associada, a gravidez em mulheres com DRC grave é possível, com desfecho materno-fetal aceitável. Apesar da alta incidência de complicações observadas na nossa série (parto pré-termo, doença hipertensiva da gravidez, agravamento da função renal, complicações infeciosas, hipersensibilidade medicamentosa) com as estratégias adotadas não existiu mortalidade fetal ou neonatal.
]]> O agravamento da função renal é mais frequente nas grávidas com DRC avançada e deve-se em particular às alterações hemodinâmicas típicas da gravidez com uma importante sobrecarga de volume materno, a maior incidência de HTA e síndromes obstétricos associados e às complicações infeciosas, particularmente do tracto genito-urinário17. Os três casos que iniciaram diálise durante a gravidez apresentavam já doença renal crónica avançada e iniciaram diálise no contexto de hipertensão não controlada, hipervolémia e agravamento da função renal.O caso 1 reporta a única gravidez numa mulher já em tratamento de substituição renal, em diálise peritoneal. Esta situação é relativamente rara, com poucos casos descritos na literatura22. A diálise peritoneal permite trocas dialíticas contínuas, com controlo metabólico mais suave, e alterações menos abruptas no volume intravascular materno, possivelmente diminuindo as alterações hemodinâmicas na circulação utero-placentária e minimizando as flutuações na pressão arterial materna. Por outro lado, traz também o benefício de não ser necessária anti-coagulação, com menor risco hemorrágico8,22. Contudo, as alterações de volume intra-abdominal causadas pelo aumento das dimensões uterinas podem obrigar à diminuição dos volumes de dialisante e necessidade de aumento da frequência das permutas de modo a manter uma eficácia dialítica adequada23. Outras complicações diretamente associadas à diálise peritoneal são a dor abdominal, o hemoperitoneu ou peritonite22. No caso em questão foi necessário transitar para hemodiálise às 17 semanas após um segundo episódio de hemoperitoneu comprovadamente associado a lesão uterina pelo catéter de diálise.
Em mulheres com DRC o diagnóstico de gravidez frequentemente é tardio, dada a irregularidade menstrual própria das mulheres com doença renal e a não valorização de sintomas como náuseas e vómitos, tradicionalmente associados a uremia. Após o diagnóstico de gravidez, é determinante a vigilância por equipa multidisciplinar, que inclua especialistas em Obstetrícia, Nefrologia e Nutrição, adaptados às características particulares do acompanhamento destas doentes. Apesar de na nossa casuística 3 dos casos terem sido diagnosticados no 1º trimestre, é desejável que a intervenção multidisciplinar seja o mais precoce possível.
Os melhores desfechos obstétricos descritos são obtidos com hemodiálise intensiva com aumento da frequência das trocas semanais (>24h/semana)11,24. É indispensável um controlo adequado do ganho de peso e da tensão arterial (todos os nossos casos se acompanharam de HTA), devendo haver um limiar baixo de suspeição de doenças como pré-eclâmpsia e síndrome HELLP cujo diagnóstico por vezes pode ser complicado nestas pacientes. O controlo da tensão arterial deve ser conseguido pelo controlo da volémia e, quando necessário, pelo recurso a medicação anti-hipertensora. Não existe um valor alvo consensual de tensão arterial nas grávidas com DRC, no entanto são sugeridos valores <140/90mmHg, não sendo recomendadas valores de TA diastólica inferiores a 75mmHg de modo a não comprometer a perfusão placentar18,25.
É fundamental o controlo dos níveis de hemoglobina que diminuem por aumento das necessidades de síntese de eritrócitos, perdas de ferro e eritrócitos durante a diálise, bem como aumento da resistência à eritropoietina por citocinas circulantes. As grávidas com doença renal apresentam frequentemente necessidades muito elevadas de estimuladores da eritropoietina e de suplementação de ferro para manutenção de níveis de hemoglobina entre 10-11g/dL8,18,25. Um adequado aporte nutricional é promovido através de liberalização da dieta, aumento de ingestão proteica (1,5-1,8g/ kg/dia) e suplementação com vitaminas hidrossolúveis com destaque para o acido fólico8,11. É essencial a vigilância regular dos níveis de cálcio e fósforo, uma vez que a hipercalcemia materna pode causar hipocalcemia e hiperfosfatemia no recém-nascido e afetar o seu desenvolvimento esquelético25.
Uma das principais complicações da gravidez em mulheres com DRC é a prematuridade, na maioria dos casos iatrogénica, com uma prevalência que varia entre os 67-100% em mulheres em diálise16. A prematuridade é o determinante isolado mais importante de desfecho adverso infantil, quer em termos de morbilidade quer em termos de mortalidade26. Apesar do número limitado de casos na nossa série salienta-se que o caso 1, em que a concepção decorreu em doente em diálise, submetido a uma estratégia de diálise mais intensiva, obteve o melhor desfecho obstétrico com parto às 35 semanas (pré-termo tardio).
Outra complicação muito frequente nestas grávidas é a restrição de crescimento fetal (cerca de 36% dos casos)27, que deve ser orientada de acordo com os padrões obstétricos habituais com ecografias seriadas, avaliação da fluxometria Doppler das artérias umbilical28 e cerebral média29 e cardiotocografia. Por último, referência ao hidrâmnios, secundário a diurese osmótica fetal pelo aumento da ureia na urina25. A decisão quanto à via de parto deve ser individualizada, tendo sempre o parto vaginal como via preferencial. A opção por uma cesariana deverá estar de acordo com as indicações obstétricas habituais.
Esta pequena série de casos demonstra que, apesar da gravidez em pacientes com doença renal crónica avançada apresentar elevada morbilidade, a monitorização fetal frequente e o controlo intensivo dos parâmetros bioquímicos e físicos maternos, sob a supervisão de uma equipa multidisciplinar especializada tornam possíveis desfechos positivos. O ajuste das técnicas dialíticas, em particular os esquemas de diálise intensiva e interação frequente entre os profissionais permite otimizar a saúde materna sem comprometimento fetal e obter melhores desfechos obstétricos.
REFERÊNCIAS BIBLIOGRÁFICAS
]]>1. Christensen T, Klebe JG, Bertelsen V, Hansen HE. Changes in renal volume during normal pregnancy. Acta Obstet Gynecol Scand. 1989;68:541-543. [ Links ]
2. Baylis C. Glomerular filtration and volume regulation in gravid animal models. Baillieres Clin Obstet Gynaecol. 1994;8:235- -264. [ Links ]
3. Baylis C. Glomerular filtration rate in normal and abnormal pregnancies. Semin Nephrol. 1999;19:133-139. [ Links ]
4. Conrad KP, Novak J, Danielson LA, Kerchner LJ, Jeyabalan A. Mechanisms of renal vasodilation and hyperfiltration during pregnancy: current perspectives and potential implications for preeclampsia. Endothelium. 2005;12:57-62. [ Links ]
5. Odutayo A, Hladunewich M. Obstetric nephrology: renal hemodynamic and metabolic physiology in normal pregnancy. Clin J Am Soc Nephrol. 2012;7:2073-2080. [ Links ]
]]>6. Williams D, Davison J. Chronic kidney disease in pregnancy. BMJ. 2008;336:211-215. [ Links ]
7. Tuot D, Gibson S, Caughey AB, Frassetto LA. Intradialytic hyperalimentation as adjuvant support in pregnant hemodialysis patients: case report and review of the literature. Int Urol Nephrol. 2010;42:233-237. [ Links ]
8. Hladunewich M, Hercz AE, Keunen J, Chan C, Pierratos A. Pregnancy in end stage renal disease. Semin Dial. 2011;24:634- -639. [ Links ]
9. Matuszkiewicz-Rowinska J, Skorzewska K, Radowicki S, Niemczyk S, Sokalski A, Przedlacki J, Puka J, Switalski M, Wardyn K, Grochowski J, Ostrowski K. Endometrial morphology and pituitary-gonadal axis dysfunction in women of reproductive age undergoing chronic haemodialysis-a multicentre study. Nephrol Dial Transplant. 2004;19:2074-2077. [ Links ]
10. Holley JL, Schmidt RJ. Changes in fertility and hormone replacement therapy in kidney disease. Adv Chronic Kidney Dis. 2013;20:240-245. [ Links ]
]]>11. Nadeau-Fredette AC, Hladunewich M, Hui D, Keunen J, Chan CT. End-stage renal disease and pregnancy. Adv Chronic Kidney Dis. 2013;20:246-252. [ Links ]
12. Framarino Dei Malatesta M, Rossi M, Rocca B, Iappelli M, Poli L, Piccioni MG, Gentile T, Landucci L, Berloco P. Fertility following solid organ transplantation. Transplant Proc. 2007;39:2001-2004. [ Links ]
13. Successful pregnancies in women treated by dialysis and kidney transplantation. Report from the Registration Committee of the European Dialysis and Transplant Association. Br J Obstet Gynaecol. 1980;87:839-845. [ Links ]
14. Romao JE, Jr., Luders C, Kahhale S, Pascoal IJ, Abensur H, Sabbaga E, Zugaib M, Marcondes M. Pregnancy in women on chronic dialysis. A single-center experience with 17 cases. Nephron. 1998;78:416-422.
15. Barua M, Hladunewich M, Keunen J, Pierratos A, McFarlane P, Sood M, Chan CT. Successful pregnancies on nocturnal home hemodialysis. Clin J Am Soc Nephrol. 2008;3:392-396. [ Links ]
16. Piccoli GB, Conijn A, Consiglio V, Vasario E, Attini R, Deagostini MC, Bontempo S, Todros T. Pregnancy in dialysis patients: is the evidence strong enough to lead us to change our counseling policy? Clin J Am Soc Nephrol. 2010;5:62-71. [ Links ]
17. Castellano G, Losappio V, Gesualdo L. Update on pregnancy in chronic kidney disease. Kidney Blood Press Res. 2011;34: 253-260. [ Links ]
18. Bili E, Tsolakidis D, Stangou S, Tarlatzis B. Pregnancy management and outcome in women with chronic kidney disease. Hippokratia. 2013;17:163-168. [ Links ]
19. Chao AS, Huang JY, Lien R, Kung FT, Chen PJ, Hsieh PC. Pregnancy in women who undergo long-term hemodialysis. Am J Obstet Gynecol. 2002;187:152-156. [ Links ]
20. Chou CY, Ting IW, Lin TH, Lee CN. Pregnancy in patients on chronic dialysis: a single center experience and combined analysis of reported results. Eur J Obstet Gynecol Reprod Biol. 2008;136:165-170. [ Links ]
21. Davison JM, Lindheimer MD. Pregnancy and chronic kidney disease. Semin Nephrol. 2011;31:86-99. [ Links ]
22. Jefferys A, Wyburn K, Chow J, Cleland B, Hennessy A. Peritoneal dialysis in pregnancy: a case series. Nephrology (Carlton). 2008;13:380-383. [ Links ]
23. Bolignano D, Coppolino G, Crasci E, Campo S, Aloisi C, Buemi M. Pregnancy in uremic patients: an eventful journey. J Obstet Gynaecol Res. 2008;34:137-143. [ Links ]
24. Hladunewich MA, Hou S, Odutayo A, Cornelis T, Pierratos A, Goldstein M, Tennankore K, Keunen J, Hui D, Chan CT. Intensive hemodialysis associates with improved pregnancy outcomes: a Canadian and United States cohort comparison. J Am Soc Nephrol. 2014;25:1103-1109. [ Links ]
25. Furaz-Czerpak KR, Fernandez-Juarez G, Moreno-de la Higuera MA, Corchete-Prats E, Puente-Garcia A, Martin-Hernandez R. Pregnancy in women on chronic dialysis: a review. Nefrologia. 2012;32:287-294.
26. Chang HH, Larson J, Blencowe H, Spong CY, Howson CP, Cairns-Smith S, Lackritz EM, Lee SK, Mason E, Serazin AC, Walani S, Simpson JL, Lawn JE, Born Too Soon preterm prevention analysis g. Preventing preterm births: analysis of trends and potential reductions with interventions in 39 countries with very high human development index. Lancet. 2013;381:223-234. [ Links ]
]]>27. Manisco G, Poti M, Maggiulli G, Di Tullio M, Losappio V, Vernaglione L. Pregnancy in end- stage renal disease patients on dialysis: how to achieve a successful delivery. Clin Kidney J. 2015;8: 293-299. [ Links ]
28. Alfirevic Z, Stampalija T, Gyte GM. Fetal and umbilical Doppler ultrasound in high-risk pregnancies. Cochrane Database Syst Rev. 2013;11:CD007529. [ Links ]
29. Prior T, Mullins E, Bennett P, Kumar S. Prediction of intrapartum fetal compromise using the cerebroumbilical ratio: a prospective observational study. Am J Obstet Gynecol. 2013;208:124 e1-6. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Pedro Viana Pinto
Centro Hospitalar São João
]]> E-mail: pedrovianapinto@gmail.com
Conflitos de interesse
Os autores declaram não haver qualquer conflito de interesses.
Recebido em: 20/4/2015
Aceite para publicação: 3/12/2015
]]>