Tipos e vias de abordagem cirúrgica em histerectomia e sua relação com lesão do sistema urinário
Type and surgical approach in hysterectomy and lesions to the urinary tract
Joana Raquel Costa*, Antónia Costa*,**
Faculdade de Medicina do Porto
Departamento de Ginecologia e Obstetricia
*Estudante de Mestrado Integrado em Medicina da Faculdade de Medicina, Universidade do Porto, Porto
**Assistente Hospitalar do Serviço de Ginecologia e Obstetrícia, Centro Hospitalar de São João, E.P.E. Porto; Professora Auxiliar Convidada do Departamento de Ginecologia, Obstetrícia e Pediatria da FMUP; i3S Instituto de Inovação e Investigação em Saúde, Universidade do Porto
Endereço para correspondência | Dirección para correspondencia | Correspondence
]]> ABSTRACT
Hysterectomy is the second most frequently performed gynecological surgery. It is therefore relevant to perform an assessment of factors associated with urological surgical morbidity.
Hysterectomy is associated with injuries to the ureter (0-3.97%) and bladder (0-2.8%). The incidence of urologic complications has been declining, as well as the difference between surgical approaches. There are some studies that demonstrate an increased risk of urologic injuries with laparoscopic and radical hysterectomy. Controversy remains on which are the real benefits of subtotal hysterectomy. No differences were found between intrafascial and extrafascial techniques. Concomitant salpingophorectomy doesn’t lead to a greater risk of injuries.
Keywords: Hysterectomy; Urinary tract injury; Urologic morbidity.
Introdução
A histerectomia é, logo a seguir à cesariana, a segunda cirurgia ginecológica mais frequentemente realizada nos países desenvolvidos em mulheres em idade reprodutiva1. Em países como Israel, Espanha, Portugal, República Checa e Dinamarca a taxa é de menos de 200 por 100.000 mulheres por ano2.
Existem vários tipos de histerectomia, bem como diferentes vias de abordagem cirúrgica. A escolha do tipo e da via de histerectomia mais apropriado vai depender fundamentalmente de: indicação cirúrgica, comorbilidades da doente, cirurgias prévias abdominopélvicas, preferência da paciente, experiência do cirurgião e disponibilidade técnica institucional. Todas estas condicionantes são fatores com impacto na morbimortalidade cirúrgica desta intervenção.
As três principais vias de abordagem cirúrgica para a realização de uma histerectomia são: (1) via abdominal por laparotomia, (2) via vaginal e (3) via abdominal laparoscópica. De acordo com a extensão de disseção por via laparoscópica, esta pode ser ainda subclassificada em histerectomia vaginal assistida por laparoscopia e histerectomia laparoscópica supracervical3.
Existem vários tipos de histerectomia e todos eles envolvendo a remoção do corpo uterino. Numa histerectomia subtotal, também designada de supracervical ou parcial, não ocorre exérese do colo uterino. Uma histerectomia total envolve a remoção de corpo e colo4.
]]> A histerectomia total intrafascial implica uma disseção dos espaços vesicouterino e retouterino com preservação da fáscia pubovesicocervical. Esta fáscia contém vasos e nervos responsáveis pela irrigação e inervação da base da bexiga, do colo do útero e porção superior da vagina. A histerectomia total extrafascial não preserva a fáscia pubovesicocervical5.Denomina-se histerectomia radical, quando se procede à exérese do corpo e colo uterinos juntamente com paramétrios e porção superior da vagina4. Existem várias classificações de histerectomia radical, mas todas dependem da extensão da resseção cirúrgica relativamente aos paramétrios.
A histerectomia também pode envolver a remoção bilateral das trompas de Falópio (salpingectomia) e ovários (ooforectomia), designada salpingoforectomia6.
Objetivo
Identificar os diferentes riscos de lesão urológica (detetada no intraoperatório) associados aos diversos tipos de histerectomia (subtotal, total intrafascial, total extrafascial, radical, com ou sem salpingoforectomia), bem como às diversas vias de abordagem cirúrgica (laparotomia, vaginal e laparoscopia).
Material e métodos (fluxograma)
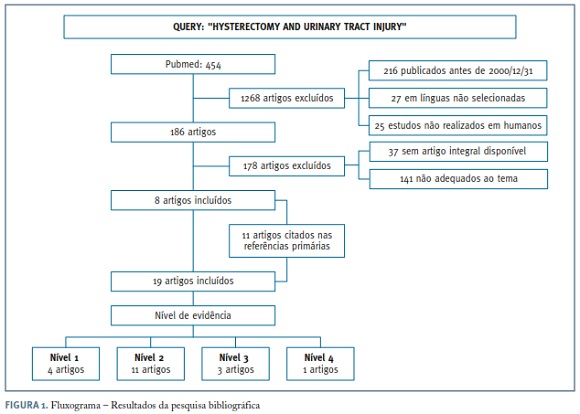
Pesquisa eletrónica nas bases de dados Pubmed/Medline COCHRANE, UPTODATE e Colégios de especialidade de ginecologia e obstetrícia britânico e americano, utilizando os termos MESH: «(hysterectomy) AND (urinary tract injury)». Os critérios de inclusão foram: estudos humanos, língua inglesa, publicados em 01/12/2000-31/07/2015 e níveis de evidência I a IV. Os critérios de exclusão foram: artigos publicados antes de 2000/31/12, em língua não inglesa, não realizados em humanos e estudos não disponíveis na íntegra. Foram encontrados 8 artigos na pesquisa electrónica e efetuou-se uma pesquisa adicional manual bibliográfica com inclusão de 11 artigos, perfazendo um total de 19 artigos.
]]> Resultados
Resultados da pesquisa bibliográfica
A pesquisa bibliográfica e electrónica resultou na seleção de um total de 19 artigos incluídos neste estudo: 4 de nível de evidência 1, 11 de nível de evidência 2, 3 de nível de evidência 3 e 1 de nível de evidência 4, segundo a classificação Oxford Centre for Evidence-Based Medicine - Levels of Evidence.
Setenta e cinco por cento das lesões do trato urinário de causa iatrogénica cirúrgica são atribuíveis a cirurgias ginecológicas e obstétricas7. A verdadeira incidência de lesões urinárias decorrentes de cirurgia ginecológica ou de outro foro é difícil de estimar, porque a maior parte dos casos reportados incluem apenas doentes com lesões detetadas intraoperatoriamente ou com necessidade de reintervenção cirúrgica.
Uma recente revisão sistemática com metanálise de 2015 (n=40.606) estimou uma incidência de lesões no ureter e na bexiga aquando da realização de uma histerectomia de 0,3% e 0,8%, respetivamente8.
Os principais fatores de risco que aumentam o risco de lesão urológica são cirurgias e aderências pélvicas prévias, hemorragia, endometriose, obesidade, neoplasias malignas e aumento das dimensões uterinas9,10.
(clique para ampliar ! click to enlarge)
]]>
]]>
1. Ureter:
Lesões ureterais no decorrer de cirurgias ginecológicas podem ocorrer ao longo de todo o trajeto ureteral. Os locais de vulnerabilidade por ordem decrescente são: ligamento infundíbulopélvico, artérias uterinas no ligamento cardinal, fossa pararretal e desembocadura na bexiga10. As lesões do ureter são mais frequentes justavesicais (75,6%), no terço médio (17,1%) e justarrenais (7,3%). O ureter esquerdo (59,8%) é o mais frequentemente lesado, seguido do ureter direito (36,6%) e em menor percentagem ambos os ureteres são lesados (3,6%)11.
2. Bexiga:
O trígono é o local onde ocorrem mais frequentemente as lesões na bexiga9,10. Lesões que ocorrem no trígono vesical podem ser mais graves pela possibilidade de estarem envolvidos os ureteres ou serem lesionados durante a reparação da lesão9,10.
3. Uretra:
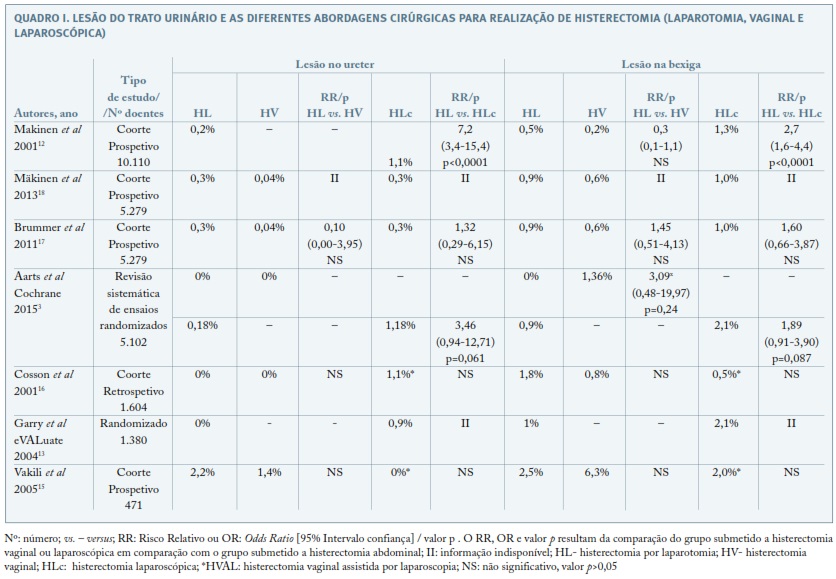
]]> Um terço das lesões ocorrem na porção proximal da uretra e as restantes na porção distal da uretra.Lesão do trato urinário e as diferentes vias de abordagem cirúrgicas para realização de histerectomia (laparotomia, vaginal e laparoscopia) - Quadro I3,12,13,15-18 e Quadro II3,14
Makinene et al, 2001, incluíram um total de 10.110 mulheres submetidas a histerectomia, (5.875 por via abdominal, 1.801 por via vaginal e 2.434 por via laparoscópica) e analisaram as morbilidades resultantes de histerectomia total de acordo com as diferentes abordagens cirúrgicas12. Comparativamente à abordagem padrão por laparotomia com uma incidência para ambas as lesões vesical e ureteral de 0,2%, a via vaginal apresenta a mesma morbilidade urinária, o que não se verifica com a via laparoscópica, em que as lesões ureteral e vesical se encontram significativamente aumentadas (Risco relativo (RR): 7,2, (Intervalo de confiança (IC) 95% 3,4-15,4) para o ureter e RR: 2,7 (IC 95% 1,6-4,4) para a bexiga)12. Foi demonstrada uma relação significativa entre o aumento da experiência dos cirurgiões em histerectomia laparoscópica e a diminuição de lesões no trato urinário: cirurgiões com mais de 30 cirurgias efetuadas têm uma incidência de de lesões no ureter de 0,50% e na bexiga de 2,0%. Quando realizadas menos de 30 cirurgias a incidência de lesões no ureter é de 2,2% e na bexiga de 0,8%12. Os mesmos resultados relativos à experiência dos cirurgiões não foram observados na abordagem por laparotomia ou vaginal, não existindo diferenças significativas. Este estudo apresenta como principais limitações tratar-se de um estudo retrospetivo e não corrigir possíveis fatores de confundimento, tal como viés de seleção, ou seja indicações para histerectomia, que são fatores de risco para morbilidade urológica, tais como endometriose e útero de dimensões significativas.
Resultados idênticos foram observados no estudo eVAluate, Garry et al, 2004, um estudo com dois ensaios simultâneos randomizados, multicêntricos, em que se avaliou a realização de histerectomias em mulheres com patologias benignas13. Um braço do estudo comparou mulheres submetidas a histerectomia total por laparotomia (n=292) com a laparoscopica (n=584). O outro braço do estudo comparou a via vaginal com a laparoscópica. A incidência de lesões uretrais foi de 0,9% e na bexiga 2,1% por via laparoscópica comparativamente a 0,0 % e 1,0 %, respetivamente, para a histerectomia por laparotomia13. Os resultados mostraram que a via laparoscópica se associou a um número significativamente maior das seguintes complicações graves: hemorragias graves, lesões na bexiga, problemas anestésicos graves, com uma incidência de 11,1% por via laparoscópica e 6,2% por laparotomia (Odds ratio (OR) = 1,91 (IC 95% 0,9-9,1), p=0,02))13.
Em 2005, Johnson et al, (n=3643), publicaram uma metanálise de ensaios randomizados, concluindo que as complicações do trato urinário (quando avaliados em conjunto bexiga e ureter) parecem ser superiores por via laparoscópica (OR= 2,61 (IC 95% 1,22-5,60)), comparativamente à laparotomia e via vaginal, apesar das diferenças nas lesões do ureter e bexiga, quando analisadas separadamente, não serem significativas14.
Vakili et al., 2005, avaliaram num ensaio prospetivo, multicêntrico, a incidência de lesão do trato urinário em 471 histerectomias totais por indicação benigna15. Em relação às lesões no ureter não foram encontradas diferenças significativas nas diferentes vias de histerectomia total (2,2% por laparotomia, 1,4% por via vaginal e 0,0% por via laparoscópica; p= 0,527)15. As mulheres com mais de 50 anos apresentam significativamente maior probabilidade de lesão do ureter (4,7% versus (vs.) 1,0%, p=0,04) 15. Em relação a lesões na bexiga, não foram encontradas diferenças significativas entre as diferentes vias de abordagem (2,5% por laparotomia, 6,3% por via vaginal e 2,0% por via laparoscópica; p=0,123)15. As histerectomias associadas a correção simultânea de prolapsos pélvicos, independentemente da via de realização, aumentaram o risco de lesão do ureter de 1,2% para 7,3%, (p=0,025)15.
Cosson et al, 2001 (n= 1.604, retrospetivo)16 e Brummer 2011 (n=5.279, prospetivo)17, mostraram que não existe qualquer diferença estatisticamente significativa ou tendência para maior número de lesões no trato urinário qualquer que seja a via de abordagem cirúrgica adotada para realização de histerectomia (laparotomia, vaginal ou laparoscópica). Brummer et al, mostraram ainda que a maioria das lesões da bexiga (88%) são detetadas intraoperatoriamente, contrariamente às do ureter (10%)17. No primeiro estudo referido os pacientes com cirurgias prévias ou cesarianas, assim como úteros com mais de 500g são consistentemente incluídas no grupo de histerectomia por laparotomia, o que pode influenciar os resultados. No estudo de Brummer et al participantes com aderências pélvicas foram incluídas em menor número no grupo de doentes submetidas a histerectomia vaginal. Por sua vez, úteros de maiores dimensões (>500g) estão presentes mais frequentemente no grupo de mulheres submetidas a histerectomia por laparotomia.
A mais recente revisão da Cochrane de 2015 acerca desta temática incluiu 47 ensaios randomizados controlados (ERC) (n= 5.102)3. Quando comparada a laparotomia com a via vaginal, existem três vezes mais lesões no trato urinário após uma histerectomia vaginal, embora não haja evidência de diferença estatisticamente significativa (OR=3,09 (IC 95% 0,48-19,97), 4 ERC, 439 mulheres)3. Comparando a via laparoscópica com a laparotomia, apesar de não ser provada uma diferença significativa, existe uma tendência para um maior número de lesões no ureter (OR= 3,46 IC 95% 0,94-12,71), 7 ERC, 1417 mulheres) e bexiga (OR 1,89 (IC 95% 0,91-3,90), 12 ECR, 2.038 mulheres) por via laparoscópica3. Quando as lesões no ureter e bexiga são agrupadas, existe uma evidência estatisticamente significativa de maior número de lesões pela via laparoscópica (OR= 2,44 (IC 95% 1,24-4,80), 13 ERC, 2.140 mulheres)3. A principal limitação deste estudo é a reduzida informação acerca da metodologia dos estudos e a número da amostra, que acarreta amplos intervalos de confiança em torno das estimativas feitas.
Makienen et al, 2013 (n=5.279), observaram uma diminuição do número de complicações decorrentes da histerectomia com uma diminuição de 17,5% em 1996 para 14,7% em 200618. As lesões no ureter mais frequentemente associadas à cirurgia laparoscópica diminuíram de 1,1% em 1996 para 0,3% em 2006 alcançando o valor observado na histerectomia por via vaginal. As lesões na bexiga diminuíram de 1,3% para 1%18.
Assim, das 7 publicações, apenas um estudo mostrou uma diferença estatisticamente significativa entre laparotomia e a via laparoscópica a favor da histerectomia por laparotomia em relação a lesões no ureter. Dois estudos mostraram risco significativamente superior de lesões urinárias globais na via laparoscópica, comparativamente à laparotomia. As principais limitações dos estudos consistem na presença de viéses de seleção e o mau/não controlo de importantes variáveis de confundimento, nomeadamente experiência do cirurgião e fatores de risco para lesão urológica.
]]> II. Lesões no trato urinário e diferentes tipos de histerectomiaIIA . Histerectomia subtotal versus total e lesão do trato urinário - Quadro III20-25
A histerectomia total dominou desde os anos 60 até meados dos anos 90. Em 1997 a histerectomia subtotal voltou a ser popular, ressurgimento coincidente com a expansão da cirurgia laparoscópica19.
A remoção do colo do útero e controlo da hemorragia na sutura vaginal constituem duas etapas importantes do decorrer de uma histerectomia e que podem propiciar o aparecimento de complicações, procedimentos estes evitados pela histerectomia subtotal19.
Harmanli et al, 2009 (estudo retrospetivo, n=1.016), analisaram as lesões do trato urinário em conjunto e mostraram um aumento significativo da incidência de lesões urológicas na histerectomia laparoscópica total (2,2%) quando comparada com a histerectomia laparoscópica subtotal (0,5%), (OR= 4,75 (IC 95% 1,21-18,56))20.
Kiran et al, 2015 (estudo coorte retrospetivo, n= 377 073) referem que existe associação entre lesão urinária e a remoção total ou parcial do útero21. Existe um risco duas vezes superior de lesões no ureter na histerectomia total por laparotomia (3,97%) quando comparada com a histerectomia subtotal por laparotomia (1,94%) (p=0,028)21. Estes resultados são obtidos num grupo de mulheres submetido a histerectomia por cancro no ovário, neoplasia esta que pode condicionar alterações na morfologia e fixação do ureter, tornando mais suscetivel a sua lesão, podendo contribuir para uma maior incidência de lesões no ureter, em comparação com as incidências reportadas nos restantes estudos incluídos.
Cupillo et al, 2003 (estudo coorte retrospetivo, n= 314) observaram uma incidência de lesões no ureter e bexiga de 0,6% e 1,3%, respetivamente, na histerectomia laparoscópica total e nenhuma lesão foi observada na histerectomia laparoscópica subtotal22. As diferenças encontradas não foram estatisticamente significativas para lesão no ureter (p=0,319) e na bexiga (p=0,158), tendo em conta os dois tipos de histerectomia laparoscópica22. Neste estudo existe uma diferença significativa em relação ao número de cirurgias prévias realizadas pelas participantes entre os dois grupos em estudo, com um maior número de intervenções prévias no grupo de doentes submetidas a histerectomia subtotal.
Learman et al, 2003 num estudo randomizado (n=135)23 e Wallwiener et al, 2013, estudo prospetivo (n=1 952)24 concluíram que a lesão do trato urinário durante a histerectomia abdominal, no primeiro estudo, e laparoscópica, no segundo estudo, é incomum e sem diferença estatisticamente significativa, quando usada a abordagem total ou subtotal. Este último estudo concluiu ainda que as complicações intraoperatórias (hemorragia; lesão do retosigmoide, do ureter e/ou bexiga; lesão da artéria epigástrica) na histerectomia laparoscópica subtotal e total não revelam diferença significativa (0,2% e 0,7%, respetivamente, p=0,225)24. Neste estudo foi encontrada uma diferença entre as participantes incluídas em cada grupo, sendo que o grupo de pacientes submetidas a histerectomia subtotal apresenta uma média inferior de cirurgias prévias por laparoscopia/laparotomia ou cesarianas, o que pode interferir nos melhores resultados encontrados na abordagem subtotal, uma vez que as variáveis referidas interferem no risco de lesão no trato urinário.
O mesmo foi observado num estudo mais recente de Tan-Kim et al, 2015 (n=3 523), que comparou a histerectomia total e subtotal por via laparoscópica, obtendo uma incidência de lesões no ureter na histerectomia laparoscópica total de 0,5% e na histerectomia laparoscópica subtotal de 0,7%, sem diferença significativa (p=0,32)25. O mesmo se observou em relação a lesões na bexiga, com uma incidência de 0,6% na abordagem total e de 1,0% na abordagem subtotal (p=0,24)25.
Uma revisão da Cochrane realizada em 2012, que incluiu 9 ensaios randomizados, (n=1.553), comparou os resultados a curto e longo prazo da histerectomia subtotal com a histerectomia total em doentes com patologias benignas, por via abdominal e laparoscópica26. Mostraram que apenas houve uma diferença significativa no intraoperatório em relação à hemorragia intraoperatória e tempo operatório, sendo estes menores na histerectomia subtotal. Em relação a lesão de estruturas adjacentes, incluindo o trato urinário, não foram encontradas diferenças26. A maior parte dos ensaios incluídos nesta revisão são pequenos (máximo n=279 e mínimo n=63) e com algumas falhas metodológicas (falha nos métodos de alocação dos doentes nos grupo de comparação, perda de seguimento dos doentes, fatores de confundimento não controlados, entre outros).
]]> Parece evidente em alguns estudos que a histerectomia subtotal apresenta vantagens em relação às complicações no período intra e pós-operatório a curto prazo27. A diminuição significativa da lesão do trato urinário, na histerectomia subtotal, só foi verificada em dois dos seis ensaios.Os resultados dos estudos são frequentemente contraditórios, dificilmente comparáveis entre si, pois verifica-se heterogeneidade nos estudos no controlo de fatores de confundimento, o que vai limitar as conclusões extrapoláveis, nomeadamente as vantagens reais da histerectomia subtotal em relação à histerectomia total.
IIB. Histerectomia total intrafascial versus hiterectomia total extrafascial e lesões no trato urinário - Quadro IV5,29
Em 1950 Aldridge e Meredith descrevem a técnica intrafascial durante uma histerectomia total por laparotomia para o tratamento de patologias benignas do colo do útero com preservação da fáscia pubovesicocervical28.
No estudo de A.Conde Aguedelo, 2000, ensaio prospetivo (n=867), os autores defendem que a remoção do colo do útero é um risco acrescido para lesões do trato urinário, uma vez que muitas lesões ocorrem nos 3 cm inferiores do ureter, junto à bexiga e, com a técnica intrafascial, reduz-se a incidência de lesões do colo do útero29. Neste estudo prospetivo, em 267 histerectomias abdominais realizadas pela técnica cirúrgica intrafascial a lesão de órgãos adjacentes (0,4 % na bexiga, 0,1% no ureter e 0% retosigmóide) foi de 0,5%, comparando com 2% de lesões de órgãos adjacentes na histerectomia extrafascial por laparotomia descrita na literatura29. A maior limitação neste estudo consiste no facto de se tratar de um ensaio experimental não controlado, onde todos os participantes foram submetidos à intervenção cirúrgica (histerectomia total com técnica intrafascial) sem grupo de comparação.
No estudo, Kaya et al, 2004 (estudo prospetivo, n=80) foi observada uma incidência de 2,6% de lesões na bexiga nas histerectomias por laparotomia realizadas com o uso da técnica extrafascial (n=38) e nenhuma lesão foi observada na histerectomia com o uso da técnica intrafascial (n=42)5. Contudo, a diferença não era estatisticamente significativa.
A técnica intrafascial é classicamente referida como uma técnica de menor risco de lesão de estruturas adjacentes, especialmente ureter, bexiga e retosigmóide. No entanto, na evidência científica pesquisada não foram encontradas diferenças significativas entre a técnica intrafascial e extrafascial. A robustez científica não é grande, pois os estudos nesta área incluem amostras diminutas, mau controlo das variáveis de confundimento e nível de qualidade baixo.
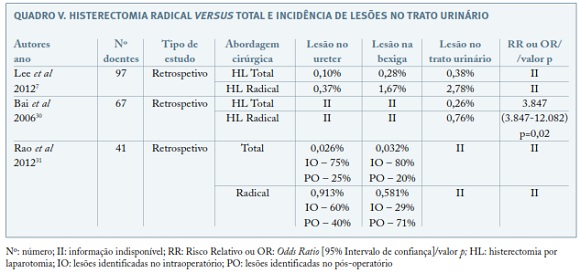
IIC. Histerectomia radical versus total e lesão do trato urinário - Quadro V7,30,31
O estudo retrospetivo (n=67) de Bai, SW et al, 2006, mostrou que a incidência de lesões do trato urinário é de 0,76%, quando realizada uma histerectomia radical por laparotomia, incidência esta superior à observada na histerectomia total por laparotomia de 0,26% (OR 3,847 (1,225-12,082), p=0,021)30. Os autores acreditam que estes valores podem ser justificados pelo facto de durante este procedimento cirúrgico ser necessária uma disseção e recessão cirúrgica mais extensa dos órgãos pélvicos30. Este estudo apresenta como principal limitação um reduzido número de participantes com complicações no trato urinário, não permitindo a obtenção de comparações com elevado poder estatístico.
Resultados idênticos foram também observados no estudo retrospetivo (n=41) de Rao, Dapang et al, 2012, onde a incidência de lesões no ureter foi de 0,913% na histerectomia radical por laparotomia e 0,026% na histerectomia total por laparotomia31. Nas lesões da bexiga a incidência foi de 0,581% na histerectomia radical por laparotomia e 0,032% na histerectomia total por laparotomia31. Um aspeto a ter em conta neste estudo é que, perante patologias pélvicas graves, para as quais se esperava a realização de procedimentos mais difíceis, foi colocado um cateter ureteral bilateralmente no pré-operatório (sem critérios definidos para a sua colocação, dependendo apenas da preferência do cirurgião), o que pode reduzir o número de lesões no ureter.
]]> O estudo retrospetivo (n=97) de Lee et al, 2012, foi de encontro aos resultados observados nos estudos anteriores7. A incidência de lesões no trato urinário foi de 2,78% na histerectomia radical e 0,38% na histerectomia total por laparotomia. Particularizando, a incidência de lesões na bexiga e ureter foi de 1,67% e 0,37%, respetivamente, na histerectomia radical. Já na histerectomia por laparotomia a incidência de lesões na bexiga foi de 0,28% e no ureter de 0,10%. Das doentes com lesão no trato urinário, 71,8% apresentaram lesão na bexiga e 23,9% lesão no ureter7.Uma das indicações mais frequentes para histerectomia radical é o cancro invasor do colo do útero. Nestas situações, o estadio da doença parece ser o principal fator de risco para lesões no trato urinário, sendo que em estadios mais avançados (maior dimensão tumoral, maior grau de invasão linfovascular e perineural, maior grau de neovascularização pericervical, aderências pélvicas com alteração anatomia normal da pelve, entre outros fatores) é mais difícil a identificação das estruturas, aumentando assim a probabilidade de lesão do trato urinário. Cirurgia oncoginecológica implica um grau de resseção mais radical, especificamente no que respeita à extensão da exérese dos paramétrios32.
Pelo fato da histerectomia total e histerectomia radical possuírem geralmente diferentes indicações (sendo a histerectomia radical indicada em situações específicas de cancro do colo do útero, do endométrio, da porção superior da vagina, entre outras), torna-se difícil encontrar estudos com resultados comparáveis, com variáveis de confundimento devidamente controladas e sem viéses de seleção. A leitura dos resultados no que respeita a comparação da morbilidade urológica entre dois tipos de histerectomias referidos é assim limitada.
A maioria dos estudos supramencionados apenas evidencia uma maior tendência, não estatisticamente significativa, para lesões do trato urinário durante a realização de uma histerectomia radical comparativamente aos restantes tipos de histerectomia. Apenas um ensaio mostrou uma diferença significativa, com maior número de lesões no trato urinário na histerectomia radical por laparotomia.
IID. Histerectomia com ou sem salpingoforectomia e lesões no trato urinário - Quadro VI15,25
A histerectomia com concomitante salpingoforectomia pode tornar o procedimento cirúrgico tecnicamente mais difícil com subsequente aumento da incidência de complicações intraoperatórias33.
No estudo de Vakili et al, 2005, (n=471) foi observada uma maior tendência de lesões no ureter e bexiga, com incidência de 2,5% e 3,9%, respetivamente, quando realizada histerectomia com salpingoforectomia bilateral, comparativamente à histerectomia sem salpingoforectomia, que apresenta uma incidência de lesão no ureter de 1,1% e na bexiga de 3,4%15. Neste estudo, a salpingoforectomia foi realizada em 62,5% das participantes nas quais foi detetada lesão no ureter e em 43,0% das participantes onde não se verificou lesão no ureter (p=0,301)15. Em relação às lesões na bexiga, 41,2% das participantes com lesão da bexiga realizaram salpingoforectomia e 43,4% das participantes sem lesão na bexiga realizaram este procedimento concomitante durante a histerectomia (p=0,856)15.
Resultados semelhantes foram obtidos num estudo mais recente, de Tan-Kim et al (estudo retrospetivo, n=3523), 201525. As lesões no ureter durante a histerectomia ocorrem com uma incidência de 0,64% sem salpingoforectomia concomitante, 0,82% se salpingoforectomia unilateral e 0,53% se bilateral25. Em relação às lesões na bexiga, 0,83% das lesões ocorrem sem salpingoforectomia, 0,81% na salpingoforectomia unilateral e 0,70% se bilateral25. Os autores avaliaram que estas diferenças entre histerectomia com e sem salpingoforectomia bilateral não são estatisticamente significativas.
Os estudos incluídos nesta análise não mostraram diferença significativa em relação a lesões no trato urinário, quando realizada histerectomia com ou sem salpingooforectomia. Contudo, muitas lesões que ocorrem são classificadas como lesões associadas à histerectomia, uma vez que não é especificado nos registos ou não é possível a distinção do momento exato em que a lesão ocorre. Deste modo, a atribuição das lesões no trato urinário à histerectomia ou à salpingoforectomia, quando estes procedimentos são realizados concomitantemente, é difícil.
Conclusão
]]> No que diz respeito às diferentes abordagens cirúrgicas da histerectomia, alguns estudos recentes ainda associam a histerectomia laparoscópica a um maior risco de lesão do trato urinário, comparativamente à laparotomia e via vaginal. Contudo, cada vez mais aproxima os seus resultados às restantes vias de abordagem cirúrgica, corroborado pelo fato de a maioria dos estudos recentes já mostrarem não existir diferença significativa entre as diversas vias e a morbilidade urológica.Em relação aos diferentes tipos de histerectomia, apenas dois estudos mostraram que a histerectomia total (quer por laparotomia, quer por laparoscopia) apresenta um risco significativamente maior de lesões no ureter (o mesmo não se verificou em relação a lesões na bexiga), quando comparada com a histerectomia subtotal.
A histerectomia intrafascial está descrita na literatura como sendo uma técnica que confere uma proteção maior das estruturas pélvicas adjacentes, especialmente do ureter, da bexiga e do retosigmóide, no entanto, a evidência científica não revela diferença significativa entre estas duas técnicas.
Em relação à histerectomia radical, esta encontra-se associada a maior resseção cirúrgica, acarretando maior risco teórico de lesão, que é evidenciado significativamente em lesões urológicas avaliadas no conjunto, mas não isoladamente da bexiga ou do ureter.
A histerectomia com salpingoforectomia não adiciona risco significativo de lesões urinárias.
As principais limitações da evidência científica residem na heterogeneidade dos estudos: tamanho amostral geralmente diminuto associado a um número reduzido de complicações urológicas com subsequente grande amplitude dos intervalos de confiança e baixo poder estatístico; desenho dos estudos com reduzido número de ensaios randomizados; discrepância na metodologia de diagnóstico de lesão urológica e ausência de controlo de fatores de confundimento e viéses de seleção, tais como: fatores de risco para lesão urológica e experiência do cirurgião.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Wu JM, Wechter ME, Geller EJ, Nguyen TV, Visco AG. Hysterectomy rates in the United States, 2003. Obstet Gynecol, 2007;110:1091-1095. [ Links ]
]]>2. OECD. Geographic Variations in Health Care: What Do We Know and What Can We Done to Improve Health System Performance?, OECD Health Policy Studies, 2014. OECD Publishing. [ Links ]
3. Aarts JWM, Nieboer TE, Johnson N, Tavender E, Garry R, Mol BWJ, Kluivers KB. Surgical approach to hysterectomy for benign gynaecological disease. Cochrane Database of Systematic Reviews, 2015, Issue 8. Art. No.: CD003677. DOI: 10.1002/ /14651858.CD003677.pub5.
4. Kives S, Lefebvre G, Wolfman W, Leyland N, Allaire C, Awadalla A, Best C, Leroux N, Potestio F, Rittenberg D, Soucy R, Singh S. Supracervical hysterectomy. J Obstet Gynaecol Can, 2010;32:62-68. [ Links ]
5. Kaya H, Sezik M, Ozbasar D, Ozkaya O, Sahiner H. Intrafascial versus extrafascial abdominal hysterectomy: effects on urinary urge incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2994; 15:171. [ Links ]
6. Orozco LJ, Tristan M, Vreugdenhil MMT, Salazar A. Hysterectomy versus hysterectomy plus oophorectomy for premenopausal women. Cochrane Database of Systematic Reviews 2014, Issue 7. Art. No.: CD005638. DOI:10.1002/14651858.CD005638. pub3.
7. Lee JS, Choe JH, Lee HS, Seo JT. Urologic complications following obstetric and gynecologic surgery. Korean J Urol. 2012;53:795-799. [ Links ]
]]>8. Teeluckdharry B, Gilmour D, Flowerdew G. Urinary tract injury at benign gynecologic surgery and the role of cystoscopy: a systematic review and meta-analysis. Obstetrics & Gynecology 126.6, 2015: 1161-1169. [ Links ]
9. Hodges KR, Davis BR, Swaim LS. Prevention and management of hysterectomy complications. Clin. Obstet. Gynecol., 57 (1) , Mar 2014, pp. 43-57.
10. Clarke-Pearson DL, Geller EJ. Complicatons of hysterectomy. Obstet Gynecol, 121, 2013, pp. 654-673.
11. Chalya PL, Massinde AN, Kihunrwa A, Simbila S. Iatrogenic ureteric injuries following abdomino-pelvic operations: a 10-year tertiary care hospital experience in Tanzania. World Journal of Emergency Surgery, 2015, 10.1: 17. [ Links ]
12. Mäkinen J, Johansson J, Tomás C, Tomás E, Heinonen PK, Laatikainen T, et al. Morbidity of 10 110 hysterectomies by type of approach. Hum Reprod 2001;16:1473-1478. [ Links ]
13. Garry R, Fountain J, Mason S, Hawe J, Napp V, Abbott J, et al. The eVALuate study: two parallel randomised trials, one comparing laparoscopic with abdominal hysterectomy, the other comparing laparoscopic with vaginal hysterectomy. BMJ, 2004;328: 129-138. [ Links ]
]]>14. Johnson N, Barlow D, Lethaby A, Tavender E, Curr L, Garry R. Methods of hysterectomy: systematic review and meta-analysis of randomized controlled trials. Br Med J 2005;330: 1478-1481. [ Links ]
15. Vakili B, Chesson RR, Kyle BL, Shobeiri SA, Echols KT, Gist R, et al. The incidence of urinary tract injury during hysterectomy: a prospective analysis based on universal cystoscopy. Am J Obstet Gynecol 2005;192:1599-1604. [ Links ]
16. Cosson M, Lambaudie E, Boukerroum M, Querleu D, Crepin G. Vaginal, laparoscopic or abdominal hysterectomy for benign disorders immediate and early postoperative complications. Eur J Obstet Gynecol Reprod Biol 2001;98: 231-236. [ Links ]
17. Brummer TH, Jalkanen J, Fraser J, Heikkinen AM, Kauko M, Mäkinen J, et al. FINHYST, a prospective study of 5279 hysterectomies: complications and their risk factors. Hum Reprod. 2011; 26:1741-1751. [ Links ]
18. Mäkinen J, Brummer T, Jalkanen J, Heikkinem A, Fraser J, Tómas E, et al. Ten years of progress- improved hysterectomy outcomes in Finland 1996-2006: a longitudinal observation study. BMJ Open, 2013;3:e003169. doi:10.1136/bmjopen-2013- 003169.
19. Baggish MS. Total and subtotal abdominal hysterectomy. Best Practice and Research: Clinical Obstetrics and Gynaecology. 2005;19(3):333-356. [ Links ]
20. Harmanli OH, Tunitsky E, Esin S, Citil A, Knee A. A comparison of short-term outcomes between laparoscopic supracervical and total hysterectomy. Am J Obstet Gynecol 2009;201:536.e1-7. [ Links ]
21. Kiran A, Hilton P, Cromwell DA. The risk of ureteric injury associated with hysterectomy: a 10-year retrospective cohort study. BJOG 2015; DOI: 10.1111/1471-0528.13576. [ Links ]
22. Cipullo L, De Paoli S, Fasolino L, Fasolino A. Laparoscopic supracervical hysterectomy compared to total hysterectomy. JSLS, Journal of the Society of Laparoendoscopic Surgeons, 13(3), 2009, 370-375.
23. Learman LA, Summitt RL Jr, Varner RE, McNeeley SG, Goodman-Gruen D, Richter HE, et al. Total or Supracervical Hysterectomy (TOSH) Research Group. A randomized comparison of total or supracervical hysterectomy: surgical complications and clinical outcomes. Obstet Gynecol, 102 (3), 2003, pp. 453-462.
24. Wallwiener M, Taran FA, Rothmund R, Kasperkowiak A, Auwärter G, Ganz A, et al. Laparoscopic supracervical hysterectomy (LSH) versus total laparoscopic hysterectomy (TLH): an implementation study in 1,952 patients with an analysis of risk factors for conversion to laparotomy and complications, and of procedure-specific re-operations. Archives of gynecology and obstetrics 288.6 (2013): 1329-1339.
25. Tan-Kim J, Menefee SA, Reinsch CS, O’Day CH, Bebchuk J, Kennedy JS, et al. Laparoscopic hysterectomy and urinary tract injury: experience in a health maintenance organization, The Journal of Minimally Invasive Gynecology, 2015, doi: 10.1016/j.jmig.2015.07.016.
26. Lethaby A, Ivanova V, Johnson NP. Total versus subtotal hysterectomy for benign gynaecological conditions. Cochrane Database of Systematic Reviews 2012, Issue 4. (DOI: 10.1002/ /14651858.CD004993.pub3).
]]>27. Garry R. The place of subtotal/supracervical hysterectomy in current practice. BJOG 2008;115:1597-1600. [ Links ]
28. Aldridge AH, Meredith RS. Complete abdominal hysterectomy. AM J Obstet Gynecol 1950;59:748-752. [ Links ]
29. Conde-Agudelo A. Intrafascial abdominal hysterectomy: outcomes and complications of 867 operations. International Journal of Gynecology & Obstetrics 68, 2000, 233-239.
30. Bai SW, Huh EH, Jung AJ, Park JH, Rha KH, Kim SK, et al. Urinary tract injuries during pelvic surgery: incidence rates and predisposing factores. International Urogynecol Journal (2006) 17: 360-364. [ Links ] DOI 10.1007/s00192-005-0015-4.
31. Rao D, Yu H, Zhu H, Duan P. The diagnosis and treatment of iatrogenic ureteral and bladder injury caused by traditional gynaecology and obstetrics operation. Arch Gynecol Obstet (2012) 285:763-765. DOI 10.1007/s00404-011-2075-2077. [ Links ]
32. Likic IS, Kadija S, Ladjevic NG, Stefanovic A, Jeremic K, Petkovic S, et al. Analysis of urologic complications after radical hysterectomy. Am J Obstet Gynecol 2008;199:644.e1-644.e3. [ Links ]
33. Camanni M, Mistrangelo E, Febo G, Ferrero B, Deltetto F. Prophylactic bilateral oophorectomy during vaginal hysterectomy for benign pathology. Arch Gynecol Obstet ,2009, 280:87-90. DOI 10.1007/s004-008-0879-x. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Joana Raquel Correia Carvalho Costa
E-mail: joana_cccosta@hotmail.com
Recebido em: 10/04/2016
Aceite para publicação: 4/09/2016
]]>