Mudança de paradigma nas histerectomias - estudo retrospetivo comparativo
Paradigm shift in hysterectomies - a retrospective comparative study
Inês Gante*, Inês Coutinho**, Diana Vale**, Rita Medeiros**, Filipa Ferreira*, Maria João Fonseca**, Maria João Carvalho***, Fernanda Águas****
Centro Hospitalar e Universitário de Coimbra
*Interna Complementar de Ginecologia e Obstetrícia do Centro Hospitalar e Universitário de Coimbra; Assistente Convidada da Faculdade de Medicina da Universidade de Coimbra
** Interna Complementar de Ginecologia e Obstetrícia do Centro Hospitalar e Universitário de Coimbra
***Assistente Hospitalar de Ginecologia e Obstetrícia do Centro Hospitalar e Universitário de Coimbra; Assistente Convidada da Faculdade de Medicina da Universidade de Coimbra
**** Diretora dos serviços de Ginecologia do Centro Hospitalar e Universitário de Coimbra
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Overview: Despite the reduction in the rate of hysterectomies during the past years, it is still the second most common major surgical procedure performed among women. It has been common practice to counsel women who were planning hysterectomy, particularly in their mid-40s or older, to undergo concomitant bilateral salpingo-oophorectomy. However, this recommendation is now being replaced by consideration of ovarian conservation with bilateral salpingectomy (BS).
Aims: To describe the trends regarding hysterectomies and concomitant adnexal surgery.
Study Design: Single-center retrospective comparative study.
Population: Women who underwent hysterectomy (2004 versus 2014).
Methods: Data were analysed using STATA 13.1.
Results: The overall number of hysterectomies decreased 28.5% (n=916 versus n=656). There was a change in the pattern of indications for hysterectomy: benign pathology decreased [79.4% versus 64.5% (p<0.001)] (mainly due to uterine fibroids) with a corresponding increase in hysterectomies due to urogenital prolapse [13.7% versus 23.6% p<0.001)] and malignant pathology [7.0% versus 11.9% (p<0.01)]. Regarding the surgical approach, there was a decrease in laparotomic route (80.9% versus 57.4% (p <0.001) with an increase in the vaginal [12.6% versus 28.7% (p<0.001)] and laparoscopic routes [6.6% versus 13.9% (p<0.001)]. In women with benign pathology, the rate of bilateral adnexectomy decreased from 69.4% to 53.3% (p<0.001) and the rate of BS increased from 0.9% to 16.5% (p<0.001). There was a reduction in intraoperative complications [4.3% versus 1.8% (p=0.006)], immediate postoperative complications [11.6% versus 7.0% (p=0.003)] and duration of hospitalizations [5.6±3.0 versus 4.1±2.4 days (p<0.001)].
Conclusion: The rate of hysterectomies decreased in the last decade, mainly due to the reduction in hysterectomies for uterine fibroids. We verified a significant shift towards ovarian conservation with increasingly concomitant BS. Considering ovarian carcinogenesis, the increase in prophylactic BS may have future impact on the reduction of ovarian cancer.
Keywords: Hysterectomy; Prophylactic salpingectomy; Bilateral ovariectomy; Ovarian conservation.
Introdução
Embora a histerectomia permaneça uma das cirurgias mais frequentemente realizadas nas mulheres, as taxas anuais têm diminuído na última década1-5. Esta redução na taxa de histerectomias, embora multifatorial, deve-se particularmente ao aumento de tratamentos conservadores, médicos e cirúrgicos, para os miomas uterinos6-8.
Também as técnicas cirúrgicas têm evoluído ao longo das últimas décadas, a histerectomia começou por ser realizada por via vaginal, seguiu-se a via abdominal e a partir dos anos 90 assistiu-se ao desenvolvimento da via laparoscópica1,2,4. No entanto, a histerectomia é ainda um procedimento cirúrgico com morbilidade significativa, sendo a infeção a complicação mais frequente4.
A anexectomia bilateral, que era habitualmente realizada no mesmo tempo cirúrgico da histerectomia por patologia benigna, com o objetivo de prevenir o cancro do ovário, é atualmente questionável, principalmente em mulheres pré-menopáusicas9-11. A evidência atual tem apontado um impacto negativo da ooforectomia bilateral em mulheres pré-menopáusicas, nomeadamente a nível cardiovascular e no maior risco de osteoporose10. Por outro lado, o potencial de prevenção de carcinoma do ovário associado à salpingectomia bilateral, poderá ter indicação em mulheres pré-menopáusicas submetidas a histerectomia por patologia não-oncológica9-18.
O objetivo deste estudo foi analisar a mudança de atitude em 10 anos em relação às histerectomias, considerando a indicação cirúrgica, via de abordagem, idade no momento da cirurgia, tempo operatório, intervenções cirúrgicas associadas (em particular, cirurgia anexial), complicações cirúrgicas, número de dias de internamento e estudo anatomopatológico.
Métodos
Estudo retrospetivo comparativo relativo aos anos de 2004 e de 2014 das mulheres submetidas a histerectomias por via laparotómica, vaginal e laparoscópica (códigos GDH 683, 6839, 684, 6849, 685, 6859, 6831, 6841, 6851, 686, 6861, 6869, 687, 6871, 6879 e 689). Os dados foram obtidos através da consulta dos processos clínicos de todas as mulheres submetidas a histerectomia nos serviços de Ginecologia do Centro Hospitalar e Universitário de Coimbra (CHUC) entre 1 de janeiro e 31 de dezembro de 2004 e 1 de janeiro e 31 de dezembro de 2014. Foram extraídos dados relativos às seguintes variáveis: tipo de histerectomia, indicação cirúrgica, sintomatologia, idade, dados biométricos, idade da menopausa, número de gestações, partos e tipos de parto, antecedentes pessoais e cirúrgicos, grau de prolapso urogenital, dados imagiológicos, citologia ao colo do útero, profilaxia antibiótica e tromboembólica, cirurgião principal (interno versus especialista), tempo operatório, intervenções cirúrgicas associadas, complicações intraoperatórias, complicações pós-operatórias, hemoglobina pré e pós-operatória, transfusão de concentrado de eritrócitos, número de dias de internamento e estudo histológico definitivo do útero e anexos. Subsequentemente, para garantir a total anonimidade e confidencialidade dos dados recolhidos, a identificação das doentes foi removida. O estudo seguiu os princípios expressos na Declaração de Helsínquia.
As variáveis categóricas foram analisadas pelo teste ÷2 e as médias das variáveis foram analisadas com o teste t de Student. A análise por regressão logística foi ajustada para os confounders idade, via de abordagem cirúrgica, peso, cirurgia oncológica, hemoglobina pré-operatória, antecedentes de cirúrgica abdominal e presença de comorbilidades. O nível de significância estatística foi de 0,05. Todos os cálculos foram efetuados com recurso ao programa estatístico STATA 13.1.
Resultados
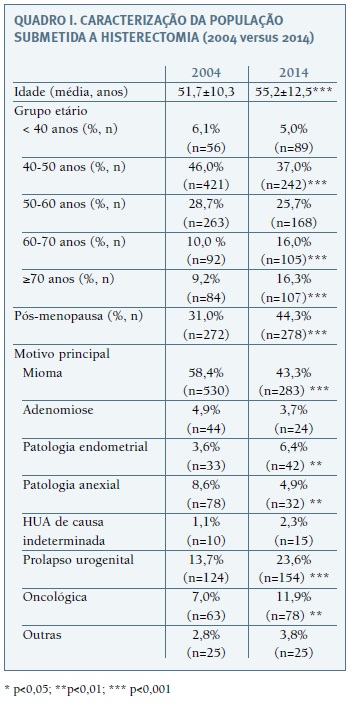
]]> No global, num intervalo de 10 anos (2004 versus 2014), o número de histerectomias reduziu 28,5% (n=916 versus n=656) no CHUC. Esta redução atingiu significado estatístico no grupo etário entre os 40 e os 50 anos, tendo neste grupo reduzido 42,5% (n=421 versus n=242). Do total de histerectomias realizadas, a proporção de histerectomias realizadas neste grupo etário (40-50 anos) reduziu de 46,0% (n=421) em 2004 para 37,0% (n=242) em 2014 (p<0,001) (Quadro I). Por outro lado, aumentou significativamente a proporção de histerectomias realizadas em mulheres com idade ≥60 anos: 10,0 % (n=92) versus 16,0% (n=105) (p<0,001) no grupo etário 60-70 anos e 9,2% (n=84) versus 16,3% (n=107) (p<0,001) no grupo etário ≥70 anos (Quadro I). Consequentemente, a proporção de mulheres pós-menopáusicas submetidas a histerectomia também aumentou: 31,0% (n=272) versus 44,3% (n=278) (p<0,001) (Quadro I).
Relativamente à indicação cirúrgica, embora a patologia benigna se mantenha o motivo mais frequente para histerectomia, a proporção de histerectomias realizadas por patologia benigna reduziu de 79,4% (n=720) para 64,5% (n=421) (p<0,001), com o correspondente aumento nas histerectomias por prolapso urogenital [13,7% (n=124) versus 23,6% (n=154) (p<0,001)] e por patologia oncológica [7,0% (n=63) versus 11,9% (n=78) (p<0,01)] (Quadro I). A redução nas histerectomias por patologia benigna foi principalmente devido à redução das histerectomias por mioma uterino [58,4% (n=530) versus 43,3% (n=283) (p<0,001)] (Quadro I). De realçar que, no grupo de mulheres na perimenopausa (idade ≥ 45 anos, não menopáusicas), o número de histerectomias por miomas uterinos teve a maior redução (51,3%), tendo passado de 76,1% do total de histerectomias (n=308) em 2004 para 65,8% (n=150) em 2014.
Quanto à via de abordagem cirúrgica, verificou-se um decréscimo das histerectomias por laparotomia [80,9% (n=741) versus 57,4% (n=376) (p<0,001), com um aumento das histerectomias por via vaginal [12,6% (n=115) versus 28,7% (n=188) (p<0,001)] e laparoscópica [6,6% (n=60) versus 13,9% (n=91) (p<0,001)] (Quadro II).
No que diz respeito às intervenções associadas, em mulheres submetidas a histerectomia por patologia benigna (excluindo patologia oncológica e histerectomias por prolapso urogenital), a taxa de anexectomia bilateral reduziu de 69,4% (n=488) para 53,3% (n=210) (p<0,001) e, por outro lado, a taxa de salpingectomia bilateral aumentou de 0,9% (n=6) para 16,5% (n=65) (p<0,001)] (Figura 1). Nas mulheres em que se optou por preservar os ovários (n=327), a taxa de salpingectomia bilateral aumentou de 3,0% (n=6) em 2004 para 50,8% (n=65) em 2014 (p<0,001). Comparando o grupo de mulheres com patologia benigna em que se efetuou preservação dos ovários versus anexectomia bilateral, verifica-se que a média de idades é inferior no grupo que realizou preservação dos ovários [43,8±5,3 versus 50,8±7,2 anos (p<0,001)] (Quadro III). Perante a opção pela preservação dos ovários, a via laparoscópica esteve mais frequentemente associada a realização profilática de salpingectomia bilateral [40,7% (n=24) versus 17,5% (n=47) (p<0,001)]. A realização de salpingectomia bilateral profilática condiciona, em média, um aumento do tempo operatório de 16 minutos em relação à manutenção das trompas e ovários [122,3±42,6 versus 106,1±25,1 minutos (p<0,001)]. Nem a anexectomia bilateral nem a salpingectomia bilateral estiveram associadas a aumento da taxa de complicações (per e pós-operatórias) nem à redução de hemoglobina em relação com a perda hemática (Quadro III).
]]>
Relativamente a outras intervenções associadas, nas mulheres submetidas a histerectomia por motivos não oncológicos (patologia benigna e prolapso), entre 2004 e 2014, a taxa de correção de incontinência urinária manteve-se [8,9% (n=72) versus 11,1% (n=54) (p>0,05)] e a taxa de colpoplastias aumentou [14,9% (n=120) versus 28,9% (n=140) (p<0,001)].
O tempo operatório da histerectomia, per se, manteve-se constante [101,1±23,1 versus 102,9±24,4 minutos (p>0,05)]. No entanto, o tempo operatório total (histerectomia e intervenções associadas) aumentou [108,2±28,4 versus 117,2±53,6 minutos (p<0,001)]. No global, a via associada a menor tempo cirúrgico é a vaginal (87,7±25,9 minutos), seguida da via laparotómica (107,4±39,8 minutos) e sendo a laparoscópica a de maior duração (127,6±36,9 minutos) (p<0,001).
A profilaxia antibiótica associada à histerectomia aumentou de 96,4% (n=866) para 99,5% (n=651) (p<0,001) bem como a profilaxia tromboembólica [97,1% (n=872) versus 99,7% (n=652) (p<0,001).
Reduziram as complicações intraoperatórias [4,3% (n=39) versus 1,8% (n=12) (p=0,006)] e pós-operatórias imediatas [11,6% (n=104) versus 7,0% (n=46) (p=0,003)]. Por regressão logística ajustada verificou-se que a profilaxia antibiótica esteve associada a uma redução nas complicações pós-operatórias ocorridas antes da alta hospitalar [ORa= 0,24 (IC 95% 0,10-0,56; p=0,001)], não se verificando associação com a profilaxia tromboembólica
Numa década a duração de internamento associado a histerectomia reduziu 1,5 dias [5,6±3,0 versus 4,1±2,4 dias (p<0,001)]. Analisando por via de abordagem cirúrgica, verifica-se que a redução no tempo de internamento foi estatisticamente significativa nas vias abdominal [5,8±3,2 versus 4,7±2,8 dias (p<0,001)] e vaginal [5,6±2,4 versus 3,2±1,1 dias (p<0,001)], não se verificando diferenças significativas na via laparoscópica [3,3±1,0 versus 3,7±1,4 dias].
]]> Por último, relativamente aos achados anátomo-patológicos, verificou-se que, apesar da redução, os miomas uterinos se mantiveram o achado mais frequente [71,7% (n=645) versus 59,7% (n=391) (p<0,001)], seguidos da adenomiose [28,8% (n=259) versus 26,1% (n=171) (p>0,05)] e da patologia oncológica [8,6% (n=79) versus 14,7% (n=96) (p<0,001)].Discussão
O número de histerectomias reduziu significativamente no CHUC entre 2004 e 2014, particularmente nas mulheres pré e peri menopáusicas. Esta redução pode ser explicada pela disponibilidade de opções terapêuticas menos invasivas na patologia ginecológica benigna, em particular no tratamento de miomas uterinos (através do desenvolvimento das técnicas de miomectomia e do surgimento de novas possibilidades de tratamento médico)6-8.
A via cirúrgica atualmente considerada como 1ª linha na patologia benigna é a vaginal, no entanto, se esta não for exequível, a via laparoscópica poderá evitar a necessidade de laparotomia19. A evidência de menor tempo de recuperação e dias de hospitalização das vias vaginal e laparoscópica condicionaram uma diminuição na taxa de histerectomias por laparotomia na maioria dos países1,2,20-25. Neste estudo verificou-se que a proporção de histerectomias por técnicas menos invasivas (vaginal e laparoscópica) mais do que duplicou, o que está de acordo com outros estudos e recomendações internacionais1,2,19.
Tendo em consideração os atuais conhecimentos relativos à carcinogénese do ovário, verificou-se um aumento na taxa de salpingectomia bilateral em mulheres pré-menopáusicas contrariando o aumento da taxa de anexectomia bilateral que se verificava no final do século XX em mulheres pré-menopáusicas com mais de 45 anos26,27. De realçar que, a salpingectomia bilateral condicionou um aumento do tempo operatório em cerca de 12 minutos (comparando com a anexectomia bilateral) e de 16 minutos (comparando com a preservação dos ovários sem salpingectomia bilateral) mas sem aumento no número de complicações intra ou pós-operatórias nem diferenças na perda hemática associada, o que está em concordância com outros estudos16,18. Assim, dado que a preservação das trompas durante a histerectomia não possui qualquer benefício e poderá condicionar patologia futura, tanto intrínseca (como hidrossalpinge) como associada à carcinogénese do ovário, a salpingectomia bilateral profilática deverá ser ponderada em todas as mulheres pré-menopáusicas sem indicação para anexectomia bilateral13,14,16,18,28.
Conclusões
O número de histerectomias reduziu na última década, sobretudo à custa da redução de histerectomias por mioma uterino. No entanto, miomas ainda são o motivo mais frequente para histerectomia na pré-menopausa. Por outro lado, verificou-se um aumento da proporção de histerectomias por prolapso urogenital e patologia oncológica. Relativamente à via de abordagem cirúrgica, houve um aumento das histerectomias por via vaginal e laparoscópica, o que se traduziu numa redução dos dias de internamento hospitalar e das complicações cirúrgicas. Em mulheres pré-menopáusicas, aumentou a opção pela preservação ovárica associada a salpingectomia bilateral profilática, o que, de acordo com os atuais conhecimentos relativos à carcinogénese do ovário, poderá ter impacto futuro na redução do cancro do ovário.
REFERÊNCIAS BIBLIOGRÁFICAS
1. Wright JD, Herzog TJ, Tsui J, Ananth C V, Lewin SN, Lu YS, et al. Nationwide trends in the performance of inpatient hysterectomy in the United States. Obs Gynecol. 2013;122(2 Pt 1):233-241. [ Links ]
2. Lykke R, Blaakaer J, Ottesen B, Gimbel H. Hysterectomy in Denmark 1977-2011: changes in rate, indications, and hospitalization. Eur J Obs Gynecol Reprod Biol. 2013;171(2):333-338. [ Links ]
3. Hilton P, Cromwell DA. The risk of vesicovaginal and urethrovaginal fistula after hysterectomy performed in the English National Health Service-a retrospective cohort study examining patterns of care between 2000 and 2008. BJOG. 2012;119(12): 1447-1454. [ Links ]
4. Makinen J, Brummer T, Jalkanen J, Heikkinen AM, Fraser J, Tomas E, et al. Ten years of progress-improved hysterectomy outcomes in Finland 1996-2006: a longitudinal observation study. BMJ Open. 2013;3(10):e003169. [ Links ]
5. Gante I, Medeiros-Borges C, Águas F. Hysterectomies in Portugal (2000-2014): What has changed? Eur J Obstet Gynecol Reprod Biol. 2017;208:97-102. [ Links ]
6. Roberts TE, Tsourapas A, Middleton LJ, Champaneria R, Daniels JP, Cooper KG, et al. Hysterectomy, endometrial ablation, and levonorgestrel releasing intrauterine system (Mirena) for treatment of heavy menstrual bleeding: cost effectiveness analysis. BMJ. 2011;342:d2202. [ Links ]
7. Olejek A, Olszak-Wasik K, Czerwinska-Bednarska A. Long-term intermittent pharmacological therapy of uterine fibroids - a possibility to avoid hysterectomy and its negative consequences. Prz Menopauzalny. 2016;15(1):48-51. [ Links ]
8. Corona LE, Swenson CW, Sheetz KH, Shelby G, Berger MB, Pearlman MD, et al. Use of other treatments before hysterectomy for benign conditions in a statewide hospital collaborative. Am J Obs Gynecol. 2015;212(3):304.e1-7. [ Links ]
9. Nunes E, Águas F, Pereira-da-Silva D. Determinants for prophylactic oophorectomy at the time of hysterectomy for benign disease. Acta Obs Ginecol Port. 2014;8(3):292-296. [ Links ]
10. Orozco LJ, Tristan M, Vreugdenhil MM, Salazar A. Hysterectomy versus hysterectomy plus oophorectomy for premenopausal women. Cochrane Database Syst Rev. 2014;(7):Cd005638. [ Links ]
11. Parker WH, Feskanich D, Broder MS, Chang E, Shoupe D, Farquhar CM, et al. Long-term mortality associated with oophorectomy compared with ovarian conservation in the nurses' health study. Obs Gynecol. 2013;121(4):709-716. [ Links ]
12. Parker WH, Broder MS, Chang E, Feskanich D, Farquhar C, Liu Z, et al. Ovarian conservation at the time of hysterectomy and long-term health outcomes in the nurses' health study. Obs Gynecol. 2009;113(5):1027-1037. [ Links ]
13. Nezhat FR, Apostol R, Nezhat C, Pejovic T. New insights in the pathophysiology of ovarian cancer and implications for screening and prevention. Am J Obs Gynecol. 2015;213(3):262-267. [ Links ]
14. Reade CJ, McVey RM, Tone AA, Finlayson SJ, McAlpine JN, Fung-Kee-Fung M, et al. The fallopian tube as the origin of high grade serous ovarian cancer: review of a paradigm shift. J Obs Gynaecol Can. 2014;36(2):133-140. [ Links ]
15. Chene G, Lamblin G, Le Bail-Carval K, Chabert P, Golfier F, Dauplat J, et al. Prophylactic salpingectomy or salpingo-oophorectomy as an ovarian cancer prevention?. Press Med. 2015;44(3): 317-323. [ Links ]
16. Hanley GE, McAlpine JN, Kwon JS, Mitchell G. Opportunistic salpingectomy for ovarian cancer prevention. Gynecol Oncol Res Pr. 2015;2:5. [ Links ]
17. Yoon SH, Kim SN, Shim SH, Kang SB, Lee SJ. Bilateral salpingectomy can reduce the risk of ovarian cancer in the general population: A meta-analysis. Eur J Cancer. 2016;55:38-46. [ Links ]
18. Morelli M, Venturella R, Mocciaro R, Di Cello A, Rania E, Lico D, et al. Prophylactic salpingectomy in premenopausal low-risk women for ovarian cancer: primum non nocere. Gynecol Oncol. 2013;129(3):448-451. [ Links ]
19. Aarts JW, Nieboer TE, Johnson N, Tavender E, Garry R, Mol BW, et al. Surgical approach to hysterectomy for benign gynaecological disease. Cochrane Database Syst Rev. 2015;(8):Cd003677. [ Links ]
20. Veerus P, Lang K, Toompere K, Kirss F. Hysterectomy types in Estonia are still different from the Nordic countries. Acta Obs Gynecol Scand. 2015;94(5):489-493. [ Links ]
21. Yusuf F, Leeder S, Wilson A. Recent estimates of the incidence of hysterectomy in New South Wales and trends over the past 30 years. Aust N Z J Obs Gynaecol. 2016;56: 420-425. [ Links ]
22. Stang A, Merrill RM, Kuss O. Hysterectomy in Germany: a DRG-based nationwide analysis, 2005-2006. Dtsch Arztebl Int. 2011;108(30):508-514. [ Links ]
23. Jokinen E, Brummer T, Jalkanen J, Fraser J, Heikkinen AM, Makinen J, et al. Hysterectomies in Finland in 1990-2012: comparison of outcomes between trainees and specialists. Acta Obs Gynecol Scand. 2015;94(7):701-707. [ Links ]
24. Lee J, Jennings K, Borahay MA, Rodriguez AM, Kilic GS, Snyder RR, et al. Trends in the national distribution of laparoscopic hysterectomies from 2003 to 2010. J Minim Invasive Gynecol. 2014;21(4):656-661. [ Links ]
25. Nogueira-Silva C, Santos-Ribeiro S, Barata S, Alho C, Osorio F, Calhaz-Jorge C. Total laparoscopic hysterectomy: Retrospective analysis of 262 cases. Acta Med Port. 2014;27(1):73-81. [ Links ]
26. Dias AC; Oliveira, CF; Almeida-Santos, A; Oliveira, HM ML. Évaluation des 3400 hystérectomies par voie abdominale réalisées dans le service de gynécologie des hôpitaux de l´Université de Coimbra. Rev Fr Gynécol Obs. 1996;91(1-2):14-19. [ Links ]
27. Mikhail E, Salemi JL, Mogos MF, Hart S, Salihu HM, Imudia AN. National trends of adnexal surgeries at the time of hysterectomy for benign indication, United States, 1998-2011. Am J Obs Gynecol. 2015;213(5):713.e1-13. [ Links ]
28. Morse AN, Hammer RA, Walter AJ, Baker S, Magtibay PM. Does hysterectomy without adnexectomy in patients with prior tubal interruption increase the risk of subsequent hydrosalpinx? Am J Obstet Gynecol. 2002;187(6):1483-5-6.
Endereço para correspondência | Dirección para correspondencia | Correspondence
Inês Gante
Centro Hospitalar e Universitario de Coimbra EPE
Coimbra, Portugal
E-mail: inesrcgante@gmail.com
]]>Recebido em: 25/06/2017
Aceite para publicação: 24/07/2017
]]>