Cirurgia de varizes em Portugal: que outcomes interessa avaliar?
Varicose veins surgery in Portugal: which outcomes to assess?
Ricardo Castro-Ferreiraa,b,*, Alberto Freitasc, José Oliveira-Pintoa,b, Dalila Rolima, José Vidoedod, Emanuel Alves Silvae, André Marinhof, Rodolfo Abreug, Andreia Coelhoh, Paulo Gonçalves Diasa, Adelino Leite-Moreirab, Sérgio Sampaioa,c, Armando Mansilhaa,b e José Fernando Teixeiraa
a Serviço de Angiologia e Cirurgia Vascular, Centro Hospitalar de São João, Porto, Portugal
b Departamento de Fisiologia e Cirurgia Cardiotorácica, Unidade de Investigação e Desenvolvimento Cardiovascular, Faculdade de Medicina da Universidade do Porto, Porto, Portugal
c Centro de Investigação e Tecnologia de Informação em Sistemas de Saúde (CINTESIS), Departamento de Ciências da Informação e da Decisão em Saúde, Faculdade de Medicina, Universidade do Porto, Porto, Portugal
d Serviço de Angiologia e Cirurgia Vascular, Centro Hospitalar Tâmega e Sousa, Penafiel, Portugal
e Departamento de Cirurgia Vascular e Endovascular, Hospital Santa Maria, Lisboa, Portugal
]]> f Serviço de Angiologia e Cirurgia Vascular, Centro Hospitalar e Universitário de Coimbra, Coimbra, Portugalg Serviço de Angiologia e Cirurgia Vascular, Hospital Santa Marta, Lisboa, Portugal
h Serviço de Angiologia e Cirurgia Vascular, Centro Hospitalar Vila Nova de Gaia/Espinho, Vila Nova de Gaia, Portugal
RESUMO
A doença venosa crónica (DVC) é a patologia vascular mais frequente, com uma prevalência estimada nos países ocidentais de 40% nas mulheres e 17% nos homens. Os recursos humanos, técnicos e orçamentais necessários para permitir o tratamento de uma patologia tão prevalente são enormes. Torna-se, assim, imperativo conhecer as consequências da DVC e realçar os benefícios do seu tratamento cirúrgico. Os outcomes a avaliar na cirurgia de varizes são menos claros que nas restantes cirurgias vasculares, tornando-se por isso imperativo definir um conjunto claro e validado de resultados para confrontar os resultados nacionais com a literatura internacional. Em Portugal a cirurgia de varizes tem a particularidade de ser praticada em grande escala por cirurgiões gerais. Os outcomes definidos também serão importantes para comparar os resultados deste procedimento quando praticado por cirurgiões vasculares ou gerais.
Este artigo propõe a criação de um protocolo de avaliação da cirurgia de varizes em Portugal. É também elaborada uma revisão com o objetivo de destacar as diferentes áreas em que a DVC afeta a vida de um doente e de sistematizar, com base na evidência atual, as vantagens do seu tratamento cirúrgico.
Palavras-chave: Doença venosa crónica; Veias varicosas; Cirurgia de varizes; Cirurgia vascular; Cirurgia geral
]]>ABSTRACT
Chronic venous disease (CVD) it's the most frequent vascular pathology, with an estimated prevalence in western countries of 40% in females and 17% in males. The human and financial resources necessary to provide treatment to such a ubiquitous disease is massive. Therefore, it is imperative to know the consequences of CVD and to highlight the benefits of its surgical treatment. In contrast to other vascular surgeries, the outcomes to assess in varicose veins surgery are less well defined. It is so vital to define a concrete set of international validated outcomes to compare the national results with the international literature. Besides, varicose vein surgery in Portugal has the particularity of being performed by both vascular and general surgeons. The selected outcomes will be important to confront the results of this procedure between the two specialties.
The article proposes the creation of a varicose veins surgery evaluation protocol in Portugal. A literature revision of the main negative aspects of CVD and a systematization of the advantages of its surgical treatment will also be performed.
Keywords: Chronic venous disease; Varicose veins; Varicose veins surgery; Vascular surgery; General surgery
Introdução
A doença venosa crónica (DVC) é a patologia vascular mais frequente, com uma prevalência estimada nos países ocidentais de 40% nas mulheres e 17% nos homens1. Estima-se que a prevalência de veias varicosas (VV) seja ainda mais elevada, estando relatada em até 70% das mulheres e 56% dos homens1. Uma recente colaboração internacional «The Vein Consult Program» demonstrou que 60% dos mais de 91.000 indivíduos avaliados com base nos critérios CEAP apresentavam DVC entre C1 e C62. Os recursos humanos, técnicos e orçamentais necessários para permitir o tratamento de uma patologia tão prevalente são enormes3. Sendo a DVC uma patologia historicamente considerada ligeira e benigna, numa altura de contenção orçamental generalizada, há já países que não estão a oferecer tratamento a todos os doentes diagnosticados3,4. Torna-se, assim, imperativo conhecer as consequências da DVC e realçar os benefícios do seu tratamento cirúrgico5,6.
A melhoria de outcomes domina a prática da cirurgia vascular. Enquanto a diminuição da mortalidade, do risco de AVC e do risco de amputação são facilmente compreendidos como os objetivos de determinadas cirurgias arteriais, os outcomes a avaliar na cirurgia de varizes são menos intuitivos. No sentido de comparar os resultados nacionais com a literatura internacional é importante definir um conjunto claro e validado de outcomes. Para maximizar os benefícios do tratamento cirúrgico das VV é igualmente importante perceber quais os cirurgiões mais aptos para promover um tratamento eficaz e com o mínimo de comorbilidades7. Nesse sentido, será importante comparar os resultados obtidos entre as diferentes especialidades que operam as varizes em Portugal.
Este artigo propõe a criação de um protocolo de avaliação centrado em outcomes validados internacionalmente. É também elaborada uma revisão com o objetivo de destacar as diferentes áreas em que a DVC afeta a vida de um doente e de sistematizar, com base na evidência atual, as vantagens do seu tratamento cirúrgico.
]]>Insuficiência venosa crónica: uma doença inofensiva?
A sensação de peso, cansaço, dor e edema dos membros inferiores que se agrava ao longo do dia, típica da DVC, é facilmente subvalorizada pelos agentes reguladores da saúde8. Estes sintomas aparentemente inocentes podem, contudo, mascarar um conjunto de problemas que não devem de todo ser desconsiderados.
A DVC é uma patologia progressiva onde aproximadamente 30% dos doentes têm um agravamento de 2 ou mais classes CEAP após 5 anos sem tratamento9. O prognóstico de um doente com úlcera venosa é desanimador, sendo esta uma condição de difícil tratamento e sucessivas recorrências10,11. Também o seu impacto socioeconómico é dramático, com estimativas a apontar para a perda de 2 milhões de dias de trabalho por ano só em Portugal12 e reforma antecipada em mais de 12% dos doentes12.
Contudo, não é só nos estádios mais avançados da DVC que é possível objetivar alterações importantes no quotidiano dos doentes. A qualidade de vida de um doente com insuficiência venosa tem sido amplamente estudada na última década e, mesmo nas fases mais precoces da DVC (CEAP C1 e C2), foi possível demonstrar alterações importantes13,14. Até serem publicados os primeiros estudos, esta patologia nos seus estádios mais precoces era considerada maioritariamente cosmética, afetando principalmente a estética e autoestima dos doentes. De facto, foi inicialmente Kurz et al. que em 2001 descreveram que eram maioritariamente as dimensões físicas do questionário SF36 as que registavam maiores alterações na DVC15. Estes dados foram corroborados por Kaplan et al. numa população de maiores dimensões (San Diego Population Study)13. A dimensão em que a DVC afeta a qualidade de vida dos doentes ganhou uma nova dimensão com o recente trabalho de Sritharan at al., que descreveram que até 30% dos doentes com doença venosa sintomática apresentam critérios de depressão crónica16.
Outra dimensão que não deve ser desvalorizada é a relação entre a DVC e a trombose venosa superficial (TVS) e profunda (TVP). O aumento do risco de TVS em doentes com VV está bem descrito17--19. Se a TVS foi no passado considerada uma patologia benigna de menor importância, estudos recentes vieram alertar para a elevada percentagem de doentes com TVP concomitante20,21. De facto, Galanaud et al. descrevem, numa amostra de 788 doentes com TVS, a presença de TVP em 29% dos doentes20, enquanto o grupo«Prospective Observational Superficial Thrombophlebitis» (POST) relatou a sua presença em 25% dos 844 doentes avaliados com TVS21. Independentemente do aumento do risco de TVS, foi descrita recentemente uma relação relevante entre a DVC e a TVP22. Com efeito, Müller-Bühl et al. avaliaram uma população superior a 83 mil indivíduos e descreveram um aumento importante do risco de TVP em doentes com VV (odds ratio ajustado de 7,33)22.
Cirurgia de varizes: análise de outcomes
O que esperar após a cirurgia de varizes
Os benefícios do tratamento cirúrgico das varizes, que vão desde uma importante melhoria da qualidade de vida à diminuição de diversas complicações associadas à DVC5,23, são irrefutáveis. A cirurgia mantém-se, por isso, como o gold standard do tratamento da DVC classe C2 a C623.
]]> O impacto da cirurgia de varizes na qualidade de vida dos doentes com DVC é provavelmente o outcome mais claro e simples de avaliar. Existe atualmente evidência indiscutível a suportar uma melhoria importante em todos os domínios de qualidade de vida relacionada com a saúde após a cirurgia de varizes24,25. Os custos globais desta melhoria de qualidade de vida foram quantificados por Ratcliffe et al., que demonstram que a cirurgia de varizes custa ao sistema de saúde do Reino Unido 4.682 £ por quality-ajusted live year (QALY), um valor bem abaixo das 20.000 £ que aquele sistema de saúde está disposto a pagar por QALY26.Em doentes com DVC mais grave (CEAP C5 e C6), a cirurgia de varizes demonstrou ser um poderoso instrumento para diminuir a recorrência da úlcera venosa, embora não tenha demonstrado ser mais eficaz que a compressão isolada na cicatrização da mesma26,27. A diminuição do risco de progressão da DVC é mais difícil de avaliar, uma vez que sendo uma doença de evolução lenta não é eticamente correto randomizar um grupo de doentes com DVC classes C2-3 com e sem tratamento cirúrgico por diversos anos. Contudo, extrapolações da base de dados dos serviços de saúde suecos estimam que será necessário operar 100 doentes com DVC classe C2-C3 e 10 doentes classe C4 para evitar o aparecimento de uma úlcera venosa28.
O grau de recorrência após o tratamento cirúrgico mantém-se desanimador, estando descrita recorrência clínica em até 50% dos doentes 5 anos após serem submetidos a cirurgia29. O grau de recorrência avaliado por eco-Doppler é ainda maior, com perto de 70% dos doentes a apresentar recorrência detetada por eco-Doppler passados 5 anos29.
Influência da técnica cirúrgica no resultado da cirurgia de varizes
Nos últimos anos foi possível observar o desenvolvimento e massificação das novas técnicas de cirurgia de varizes. Inclusivamente, a cirurgia endovenosa já é proposta como a primeira linha de tratamento para as VV nas últimas guidelines da SVS e American Venous Forum23 . É, contudo, importante realizar uma análise imparcial da melhor evidência disponível a comparar as diferentes técnicas cirúrgicas. Foram publicadas em 2014 e 2015 3 meta-análises que demonstram uma aparente homogeneidade entre as diferentes técnicas, quer em termos de recorrência quer em termos de melhoria na qualidade de vida do doente30--32. Adicionalmente, uma técnica que não deve ser desprezada é a cirurgia de varizes por «Cure Conservatrice et Hemodynamique de l'Insufficience Veineuse en Ambulatoire» (CHIVA), uma vez que tem o potencial de restaurar a dinâmica do fluxo sanguíneo de uma forma minimamente invasiva. De facto, uma recente meta-análise publicada na Cochrane refere que o método CHIVA está associado a menor taxa de recorrência e a menos efeitos laterais que o stripping clássico33. Este procedimento tem ainda a vantagem de preservar o património venoso dos doentes que dessa forma se mantém disponível para no futuro ser usado como bypass arterial.
Cirurgia vascular versus cirurgia geral: há diferenças nos outcomes?
A cirurgia de varizes é singular no sentido em que há diversas especialidades cirúrgicas a operar esta patologia. Particularmente, em Portugal, a cirurgia geral é responsável por uma percentagem importante, mas desconhecida, das cirurgias de varizes. Do nosso conhecimento, apenas um estudo retrospetivo, de pequeno volume, comparou os resultados desta cirurgia entre cirurgia geral e vascular num centro único finlandês34. Neste estudo é descrito que os doentes operados por cirurgia geral apresentam maior taxa de recorrência da doença, avaliada por eco-Doppler, 3 anos após a cirurgia34. A preocupação de que a cirurgia geral possa estar a operar as varizes de forma subótima também já foi levantada em Espanha7. Um estudo comparativo, baseado em outcomes claros e bem definidos, da cirurgia de varizes realizada por cirurgiões vasculares e cirurgiões gerais será de enorme interesse.
]]> O desenvolvimento de um protocolo de avaliação
A criação de um protocolo de avaliação da cirurgia venosa em Portugal deverá incluir uma série de componentes que abranjam a avaliação pré-operatória dos doentes, a técnica cirúrgica utilizada e os resultados da mesma. No sentido de comparar os doentes operados por cirurgiões vasculares e cirurgiões gerais será importante incluir indivíduos com patologia semelhante e submetidos à mesma técnica cirúrgica. O protocolo proposto encontra-se esquematizado na figura 1.
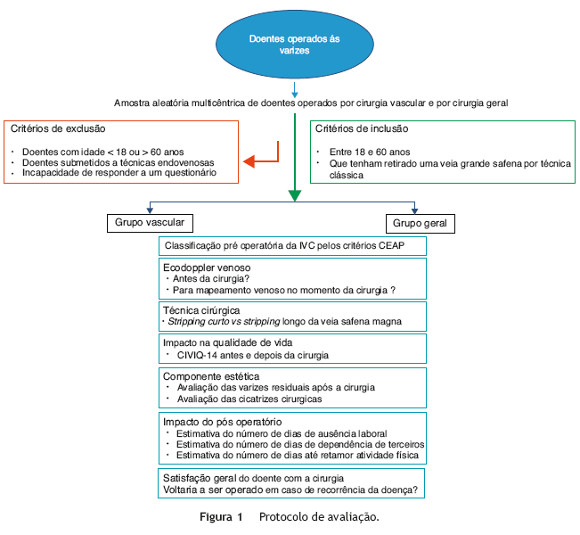
A avaliação por eco-Doppler venoso de todos os doentes com sintomas de DVC é uma indicação classe 1A das mais recentes guidelines de doença venosa23. Avaliar se todos os doentes que são submetidos a cirurgia de varizes realizaram previamente um eco-Doppler venoso será por isso de enorme importância. Está descrito que o mapeamento venoso com eco-Doppler no momento da cirurgia melhora os outcomes da mesma35, embora resultados opostos já tenham sido publicados36. Terá interesse avaliar a taxa de doentes operados com o apoio de eco-Doppler para mapeamento venoso e se este procedimento afeta os resultados da cirurgia. O nosso protocolo contempla a avaliação da realização deste exame antes e no momento da cirurgia de varizes (fig. 1).
A lesão do nervo safeno é uma complicação bem descrita do stripping da veia safena magna (VSM)37. Esta complicação é consideravelmente mais frequente se for realizado stripping longo (até ao tornozelo) em comparação com o curto (até ao joelho) da VSM38,39. Embora a lesão do nervo safeno esteja associada a algum desconforto, há autores que questionam se esta complicação deve influenciar a escolha da técnica cirúrgica40,41. Propomos avaliar a percentagem de doentes tratados por stripping curto versus longo e avaliar se a diferença técnica altera o seu outcome (fig. 1).
Foram desenvolvidos diversos questionários com o objetivo de avaliar especificamente a qualidade de vida relacionada com a patologia venosa crónica, tendo o seu desenvolvimento e validação sido detalhadamente descritos por Vasquez numa recente revisão42. Um dos mais utilizados é o «Chronic Venous Insufficiency Questionnaire» (CIVIQ)43,44, inicialmente desenvolvido por Launois45 e recentemente simplificado e validado por um grupo coordenado pelo professor Armando Mansilha, tendo sido criado o CIVIQ-1446. O CIVIQ-14 é formado por 14 perguntas que abrangem 3 dimensões dor, física e psicológica, variando o resultado entre 14 (melhor qualidade de vida) e 70 (pior qualidade de vida). O resultado bruto obtido pode ser convertido num score global de 0-100 conforme as normas fornecidas pelos autores46. O CIVIQ-14 encontra-se atualmente amplamente validado e o seu resultado correlaciona-se quer com a gravidade clínica da patologia venosa (com base no CEAP), quer com os restantes inquéritos específicos da doença, bem como de qualidade de vida geral relacionada com a saúde47. O protocolo de avaliação que propomos inclui a avaliação do score CIVIQ-14 antes e depois da cirurgia de varizes (no mínimo 6 meses após) (fig. 1).
Muitos dos outcomes associados à cirurgia de varizes são de maior subjetividade e dependem da perceção de cada doente operado. A escala visual analógica (EVA) é um importante instrumento de medição para caraterísticas subjetivas que não são facilmente mensuráveis de forma direta. A dor pós-operatória é um fator relevante na avaliação de qualquer procedimento cirúrgico e é um dos sintomas mais frequentemente medidos por EVA48. No nosso protocolo é incluída a avaliação da dor numa escala de 1-5, nos dias que imediatamente se seguem à cirurgia (fig. 1). A cirurgia de varizes tem uma componente estética inegável, sendo esta a principal razão da cirurgia em aproximadamente 26% dos doentes operados49. A perceção cosmética é uma caraterística que pela sua subjetividade é dificilmente mensurável de forma direta. As varizes residuais e as cicatrizes após a cirurgia são 2 dos maiores componentes com importância estética na perna submetida a cirurgia de varizes. Propomos a avaliação por EVA, de uma escala de 1-5, do número de varizes residuais que cada doente perceciona após a cirurgia (onde 1 é nenhumae5é numerosas) e da estética das cicatrizes operatórias (onde 1 corresponde a serem impercetíveis e 5 corresponde a serem deformadoras) (fig. 1). Também propomos avaliar por EVA a satisfação geral com o procedimento (fig. 1).
Uma vez que a cirurgia de varizes não é um procedimento curativo e que uma percentagem importante dos doentes tem recorrência da doença29, será interessante perceber qual a percentagem de doentes que seria de novo submetida a cirurgia em caso de reaparecimento dos sinais e sintomas da doença (fig. 1).
]]> Face à enorme prevalência da DVC, a cirurgia de varizes é um dos mais frequentes procedimentos cirúrgicos em Portugal. O período de inatividade laboral que se segue a esta cirurgia pode por isso significar a perda de milhões de dias de trabalho por ano. O nosso protocolo propõe avaliar o número de dias de ausência laboral após a cirurgia (fig. 1). Também propomos avaliar o número de dias de total dependência de terceiros para as atividades de vida diárias (AVD) e, dessa forma, estimar o número de perda secundária de dias de trabalho (fig. 1). Com o objetivo de analisar o número total de dias com limitações associados à cirurgia de varizes, é incluída a avaliação do tempo necessário para retomar a atividade física (fig. 1).
Conclusão
A DVC é uma patologia ubíqua e de inegável gravidade. A cirurgia de varizes mantém-se na primeira linha do seu tratamento e não há, até ao presente, evidência que confira vantagens inequívocas às novas técnicas endovenosas. Até ao presente, nenhum estudo comparou de forma clara os resultados desta cirurgia realizada por cirurgiões vasculares e cirurgiões gerais. Propomos a criação de um protocolo de avaliação, que inclua os parâmetros previamente referidos (fig. 1), permitindo a comparação desta cirurgia entre as especialidades de cirurgia vascular e cirurgia geral, possibilitando a avaliação dos resultados nacionais à luz da literatura internacional.
Responsabilidades éticas
Proteção de pessoas e animais. Os autores declaram que para esta investigação não se realizaram experiências em seres humanos e/ou animais.
Confidencialidade dos dados. Os autores declaram que não aparecem dados de pacientes neste artigo.
Direito à privacidade e consentimento escrito. Os autores declaram que não aparecem dados de pacientes neste artigo.
]]> Conflito de interesses
Os autores declaram não haver conflito de interesses.
Referências
1. Beebe-Dimmer JL, Pfeifer JR, Engle JS, et al. The epidemiology of chronic venous insufficiency and varicose veins. Ann Epidemiol. 2005;15:175-84. [ Links ]
2. Rabe E, Guex JJ, Puskas A, et al. Epidemiology of chronic venous disorders in geographically diverse populations: results from the Vein Consult Program. Int Angiol. 2012;31:105-15. [ Links ]
3. Moore HM, Lane TR, Thapar A, et al. The European burden of primary varicose veins. Phlebology. 2013;28 Suppl 1:141-7. [ Links ]
]]>4. Mandavia R, Dharmarajah B, Qureshi MI, et al. The role of cost-effectiveness for vascular surgery service provision in the United Kingdom. J Vasc Surg. 2015;61:1331-9. [ Links ]
5. Meissner MH. What is the medical rationale for the treatment of varicose veins? Phlebology. 2012;27 Suppl 1:27-33. [ Links ]
6. Kelleher D, Lane TR, Franklin IJ, et al. Treatment options, clinical outcome (quality of life) and cost benefit (quality-adjusted life year) in varicose vein treatment. Phlebology. 2012;27 Suppl 1:16-22. [ Links ]
7. Morales-Cuenca G, Moreno-Egea A, Aguayo-Albasini JL. General surgeons and varicose vein surgery. Cir Esp. 2009;85:205-13. [ Links ]
8. Eberhardt RT, Raffetto JD. Chronic venous insufficiency. Circulation. 2014;130:333-46. [ Links ]
]]>9. Kostas TI, Ioannou CV, Drygiannakis I, et al. Chronic venous disease progression and modification of predisposing factors. J Vasc Surg. 2010;51:900-7. [ Links ]
10. Callam MJ, Harper DR, Dale JJ, et al. Chronic ulcer of the leg: Clinical history. Br Med J (Clin Res Ed). 1987;294:1389-91. [ Links ]
11. Green J, Jester R, McKinley R, et al. The impact of chronic venous leg ulcers: a systematic review. J Wound Care. 2014;23:601-12. [ Links ]
12. Da Silva A, Navarro MF, Batalheiro J. The importance of chronic venous insufficiency. Various preliminary data on its medico-social consequences. Phlebologie. 1992;45:439-43. [ Links ]
13. Kaplan RM, Criqui MH, Denenberg JO, et al. Quality of life in patients with chronic venous disease: San Diego population study. J Vasc Surg. 2003;37:1047-53. [ Links ]
]]>14. Lozano Sanchez FS, Sanchez Nevarez I, Gonzalez-Porras JR, et al. Quality of life in patients with chronic venous disease: Influence of the socio-demographical and clinical factors. Int Angiol. 2013;32:433-41. [ Links ]
15. Kurz X, Lamping DL, Kahn SR, et al. Do varicose veins affect quality of life? Results of an international population-based study. J Vasc Surg. 2001;34:641-8. [ Links ]
16. Sritharan K, Lane TR, Davies AH. The burden of depression in patients with symptomatic varicose veins. Eur J Vasc Endovasc Surg. 2012;43:480-4. [ Links ]
17. Karathanos C, Exarchou M, Tsezou A, et al. Factors associated with the development of superficial vein thrombosis in patients with varicose veins. Thromb Res. 2013;132:47-50. [ Links ]
18. Guex JJ. Thrombotic complications of varicose veins. A literature review of the role of superficial venous thrombosis. Dermatol Surg. 1996;22:378-82. [ Links ]
]]>19. Karathanos C, Sfyroeras G, Drakou A, et al. Superficial vein thrombosis in patients with varicose veins: Role of thrombophilia factors, age and body mass. Eur J Vasc Endovasc Surg. 2012;43:355-8. [ Links ]
20. Galanaud JP, Genty C, Sevestre MA, et al. Predictive factors for concurrent deep-vein thrombosis and symptomatic venous thromboembolic recurrence in case of superficial venous thrombosis. The OPTIMEV study. Thromb Haemost. 2011;105:31-9. [ Links ]
21. Decousus H, Quere I, Presles E, et al. Superficial venous thrombosis and venous thromboembolism: a large, prospective epidemiologic study. Ann Intern Med. 2010;152:218-24. [ Links ]
22. Muller-Buhl U, Leutgeb R, Engeser P, et al. Varicose veins are a risk factor for deep venous thrombosis in general practice patients. Vasa. 2012;41:360-5. [ Links ]
23. Gloviczki P, Comerota AJ, Dalsing MC, et al. The care of patients with varicose veins and associated chronic venous diseases: Clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum. J Vasc Surg. 2011;53:2S-48S. [ Links ]
]]>24. Smith JJ, Garratt AM, Guest M, et al. Evaluating and improving health-related quality of life in patients with varicose veins. J Vasc Surg. 1999;30:710-9. [ Links ]
25. Michaels JA, Campbell WB, Brazier JE, et al. Randomised clinical trial, observational study and assessment of cost-effectiveness of the treatment of varicose veins (REACTIV trial). Health Technol Assess. 2006;10:1-196, iii-iv. [ Links ]
26. Ratcliffe J, Brazier JE, Campbell WB, et al. Cost-effectiveness analysis of surgery versus conservative treatment for uncomplicated varicose veins in a randomized clinical trial. Br J Surg. 2006;93:182-6. [ Links ]
27. Gohel MS, Barwell JR, Taylor M, et al. Long term results of compression therapy alone versus compression plus surgery in chronic venous ulceration (ESCHAR): Randomised controlled trial. BMJ. 2007;335:83. [ Links ]
28. Neglen P, Eklof B, Kulwicki A, et al., Writing Group II of the Pacific Vascular Symposium 6. Prevention and treatment of venous ulcers in primary chronic venous insufficiency. J Vasc Surg. 2010;52:15S-20S. [ Links ]
]]>29. Van Rij AM, Jiang P, Solomon C, et al. Recurrence after varicose vein surgery: A prospective long-term clinical study with duplex ultrasound scanning and air plethysmography. J Vasc Surg. 2003;38:935-43. [ Links ]
30. Nesbitt C, Bedenis R, Bhattacharya V, et al. Endovenous ablation (radiofrequency and laser) and foam sclerotherapy versus open surgery for great saphenous vein varices. Cochrane Database Syst Rev. 2014;7:CD005624. [ Links ]
31. Carroll C, Hummel S, Leaviss J, et al. Systematic review, network meta-analysis and exploratory cost-effectiveness model of randomized trials of minimally invasive techniques versus surgery for varicose veins. Br J Surg. 2014;101:1040-52. [ Links ]
32. Lynch NP, Clarke M, Fulton GJ. Surgical management of great saphenous vein varicose veins: A meta-analysis. Vascular. 2015;23:285-96. [ Links ]
33. Bellmunt-Montoya S, Escribano JM, Dilme J, et al. CHIVA method for the treatment of chronic venous insufficiency. The Cochrane database of systematic reviews. 2013;7:CD009648. [ Links ]
]]>34. Oinonen A, Sugano N, Lehtola A, et al. Service comparison between vascular and general surgery in the treatment of chronic venous insufficiency with special reference to preoperative Doppler techniques. Scand J Surg. 2006;95:45-8. [ Links ]
35. Blomgren L, Johansson G, Bergqvist D. Randomized clinical trial of routine preoperative duplex imaging before varicose vein surgery. Br J Surg. 2005;92:688-94. [ Links ]
36. Smith JJ, Brown L, Greenhalgh RM, et al. Randomised trial of pre-operative colour duplex marking in primary varicose vein surgery: Outcome is not improved. Eur J Vasc Endovasc Surg. [ Links ]
37. Holme K, Matzen M, Bomberg AJ, et al. Partial or total stripping of the great saphenous vein. 5-year recurrence frequency and 3-year frequency of neural complications after partial and total stripping of the great saphenous vein. Ugeskr Laeger. 1996;158:405-8. [ Links ]
38. Holme JB, Skajaa K, Holme K. Incidence of lesions of the saphenous nerve after partial or complete stripping of the long saphenous vein. Acta Chir Scand. 1990;156:145-8. [ Links ]
]]>39. Lacroix H, Nevelsteen A, Suy R. Invaginating versus classic stripping of the long saphenous vein. A randomized prospective study. Acta Chir Belg. 1999;99:22-5. [ Links ]
40. Morrison C, Dalsing MC. Signs and symptoms of saphenous nerve injury after greater saphenous vein stripping: Prevalence, severity, and relevance for modern practice. J Vasc Surg. 2003;38:886-90. [ Links ]
41. Vasquez MA, Munschauer CE. Venous Clinical Severity Score and quality-of-life assessment tools: Application to vein practice. Phlebology. 2008;23:259-75. [ Links ]
42. Launois R, Mansilha A, Lozano F. Linguistic validation of the 20 item-chronic venous disease quality-of-life questionnaire (CIVIQ-20). Phlebology. 2014;29:484-7. [ Links ]
43. Launois R, Mansilha A, Jantet G. International psychometric validation of the Chronic Venous Disease quality of life Questionnaire (CIVIQ-20). Eur J Vasc Endovasc Surg. 2010;40: 783-9. [ Links ]
]]>44. Launois R, Reboul-Marty J, Henry B. Construction and validation of a quality of life questionnaire in chronic lower limb venous insufficiency (CIVIQ). Qual Life Res. 1996;5:539-54. [ Links ]
45. Launois R, le Moine JG, Lozano FS, et al. Construction and international validation of CIVIQ-14 (a short form of CIVIQ-20), a new questionnaire with a stable factorial structure. Qual Life Res. 2012;21:1051-8. [ Links ]
46. Kuet ML, Lane TR, Anwar MA, et al. Comparison of disease-specific quality of life tools in patients with chronic venous disease. Phlebology. 2014;29:648-53. [ Links ]
47. Hawker GA, Mian S, Kendzerska T, et al. Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS). Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP). Arthritis Care Res (Hoboken). 2011;63 Suppl 11: S240-52. [ Links ]
48. O'Leary DP, Chester JF, Jones SM. Management of varicose veins according to reason for presentation. Ann R Coll Surg Engl Ann R Coll Surg Engl. 1996;78:214-6. [ Links ]
]]>Correio eletrónico: cferreira.ricardo@gmail.com (R. Castro-Ferreira).
Recebido a 26 de maio de 2015;
Aceite a 26 de julho de 2015
Disponível na Internet a 28 de agosto de 2015
]]>