
95% das tomas de antirretrovirais) nos últimos três meses foi estimada em 69% dos pacientes, mas 36% apresentam um mau resultado de contagem de Linfócitos T CD4 e 63% não cumprem o protocolo recomendado pelo Ministério da Saúde. Conclusões: O principal motivo alegado para o abandono da terapia antirretroviral é o estigma ligado à infeção pelo vírus da imunodeficiência humana adquirida, mas a insegurança alimentar constitui igualmente um fator determinante. Nos pacientes em terapia, a adesão estimada de 69% explica a alta incidência de infeções oportunistas (27%). O abandono da terapia em Nampula é um problema grave e complexo, resultante de fatores individuais, sociais e do funcionamento dos cuidados de saúde primários. Será necessário desenvolver uma ação interdisciplinar junto de pacientes, famílias e profissionais de saúde para inverter a situação e melhorar a adesão terapêutica.]]>
95% of pills were taken in the last three months) was found in 69% of patients, but 36 % of people who are adherent have a low CD4 count and 63% are not following the recommended treatment protocol. Conclusions: Perception of stigma from infection with the human immunodeficiency virus is considered the main reason for non-adherence with antiretroviral treatment, but food insecurity is also an important determinant. A treatment adherence rate of 69% explains the high incidence of opportunistic infections (27%). Abandonment of antiretroviral treatment in Nampula is a serious and complex problem due to individual, social and primary health care services factors. It will be necessary to develop an interdisciplinary intervention with patients, families, and health professionals, to reverse this situation and improve treatment adherence.]]>
Adesão à terapia antirretroviral em pacientes infetados pelo VIH nos cuidados de saúde primários em Nampula, Moçambique
Adherence to antiretroviral treatment among HIV positive patients in primary health care in Nampula, Mozambique
Paulo das Neves Pires,1 Abdoulaye Marega,2 José Miguel Creagh3
1. Universidade Lurio, Moçambique
2. Médico Generalista, Docente, Faculdade de Ciências de Saúde, Universidade Lúrio, Nampula, Moçambique
3. Docente, Faculdade de Ciências de Saúde, Universidade Lúrio, Nampula, Moçambique
Endereço para correspondência | Dirección para correspondencia | Correspondence
RESUMO
]]> Objetivos: Avaliar a taxa de adesão à terapia antirretroviral na província de Nampula e os fatores associados ao abandono do tratamento.Tipo de estudo: Descritivo transversal misto.
Local: Centros de saúde de cinco distritos da província de Nampula, Moçambique, 2014.
População: Pacientes infetados pelo vírus da imunodeficiência humana em terapia antirretroviral e pacientes que abandonaram, profissionais dos cuidados de saúde primários.
Métodos: Inquérito a pacientes em terapia antirretroviral e a pacientes que abandonaram a terapia, consulta documental de processos clínicos, registos da farmácia e relatórios estatísticos do programa Vírus da Imunodeficiência Humana Adquirida, entrevista aos profissionais de saúde.
Resultados: A taxa de abandono da terapia atinge os 40%. Foram inquiridos 208 pacientes em tratamento e 86 abandonos, 70% do sexo feminino, entre os 18 e os 62 anos de idade. Como causa principal de abandono 36% referem discriminação, mas 58% não dispõem de alimentos suficientes e 37% apresentam depressão. A boa adesão à terapia antirretroviral (>95% das tomas de antirretrovirais) nos últimos três meses foi estimada em 69% dos pacientes, mas 36% apresentam um mau resultado de contagem de Linfócitos T CD4 e 63% não cumprem o protocolo recomendado pelo Ministério da Saúde.
Conclusões: O principal motivo alegado para o abandono da terapia antirretroviral é o estigma ligado à infeção pelo vírus da imunodeficiência humana adquirida, mas a insegurança alimentar constitui igualmente um fator determinante. Nos pacientes em terapia, a adesão estimada de 69% explica a alta incidência de infeções oportunistas (27%). O abandono da terapia em Nampula é um problema grave e complexo, resultante de fatores individuais, sociais e do funcionamento dos cuidados de saúde primários. Será necessário desenvolver uma ação interdisciplinar junto de pacientes, famílias e profissionais de saúde para inverter a situação e melhorar a adesão terapêutica.
Palavras-chave: Adesão; Antirretroviral; VIH/SIDA; Cuidados de saúde primários; Moçambique
ABSTRACT
]]> Objectives: To evaluate adherence to antiretroviral treatment in Nampula province and to identify the determinants of non-compliance.Study type: Observational study with quantitative and qualitative methods.
Place: Five health centers in the Nampula province of Mozambique in 2014.
Population: Patients infected with human immunodeficiency virus receiving antiretroviral treatment, patients who had abandoned treatment, and primary health care professionals.
Methods: Patients on treatment and patients who were non-compliant with therapy completed a questionnaire, patient records (clinical files, pharmacy records, and statistical records) were reviewed, and interviews were conducted with health care professionals.
Results: Abandonment of antiretroviral treatment reached 40%. We surveyed 208 patients on treatment and 86 patients who were non-compliant with therapy. Of these 70% were female and they were between 18 and 62 years of age. The main reason for non-compliance with treatment (36%) was stigma attached to having the infection. In addition 58% of patients do not have enough food and 37% suffer from depressive ideation. Good treatment adherence (>95% of pills were taken in the last three months) was found in 69% of patients, but 36 % of people who are adherent have a low CD4 count and 63% are not following the recommended treatment protocol.
Conclusions: Perception of stigma from infection with the human immunodeficiency virus is considered the main reason for non-adherence with antiretroviral treatment, but food insecurity is also an important determinant. A treatment adherence rate of 69% explains the high incidence of opportunistic infections (27%). Abandonment of antiretroviral treatment in Nampula is a serious and complex problem due to individual, social and primary health care services factors. It will be necessary to develop an interdisciplinary intervention with patients, families, and health professionals, to reverse this situation and improve treatment adherence.
Keywords: Adherence; Antiretroviral; HIV/AIDS; Primary health care; Mozambique
Introdução
]]> Cerca de 34 milhões de pessoas viviam com o vírus da imunodeficiência humana (VIH) no mundo em 2010 e quase metade (47%, 6,6 milhões) das 14,2 milhões de pessoas elegíveis para tratamento tinham acesso à terapia antirretroviral (TARV).1A Declaração Política em VIH e Síndroma de Imunodeficiência Humana Adquirida (SIDA), da Assembleia das Nações Unidas, de 2011, constatava: “O Mecanismo Internacional de Aquisição de Medicamentos baseado no financiamento inovador e centrado no acesso, qualidade e redução de preços dos medicamentos antirretrovirais (ARV) permitiu a expansão do acesso à TARV. O acesso a medicamentos e serviços seguros, eficazes, acessíveis e de boa qualidade é fundamental para a realização dos direitos de todas as pessoas usufruirem dos mais elevados níveis de saúde física e mental.”2
A adesão à TARV constitui o fator determinante do grau e duração de supressão viral,3 sendo vários e complexos os fatores que influenciam esta condição, que varia no tempo. Um estudo realizado em Espanha demonstrou que ambientes sociofamiliares inadequados diminuem a taxa de aderência à TARV,4 outro no Uganda concluiu que, “em pacientes em TARV, a monitorização laboratorial de rotina está associada a melhor saúde e sobrevida em comparação com o acompanhamento clínico apenas”.5
Moçambique tem sofrido um impacto negativo da infeção pelo VIH resultante das altas taxas de morbilidade e mortalidade. Um dos desafios é a carga crescente sobre o sistema de saúde, que sofria já de uma carência generalizada de profissionais, sobretudo em áreas rurais.
Em 2011, Moçambique tinha uma prevalência estimada de VIH de 11,5%, dos quais 46% estavam em TARV,6 um aumento muito significativo comparativamente aos 3.500 pacientes em tratamento em 2003, atestando o esforço do Ministério da Saúde para levar a TARV a todos os distritos do país.
A descentralização dos cuidados de VIH/SIDA dos hospitais de dia para os cuidados de saúde primários (CSP), nos centros de saúde (CS) dos distritos, foi precedida da formação dos médicos, técnicos de medicina curativa, enfermeiros, técnicos de farmácia e agentes de medicina preventiva, atores principais dos CSP no Serviço Nacional de Saúde (SNS) moçambicano. Posteriormente foram colocados nos CSP técnicos de psicologia destinados ao aconselhamento dos pacientes e nutricionistas predominantemente dedicados ao problema da malnutrição infantil.
A nossa experiência profissional durante seis anos nos serviços VIH dos CS das províncias da Zambézia e Nampula e testemunhos de outros profissionais de saúde indicam que a insegurança alimentar e a baixa acessibilidade aos CSP foram duas das principais dificuldades na expansão da TARV em Moçambique.
Nos últimos três anos, o número de abandonos da terapia tem aumentado significativamente, colocando um novo desafio à saúde pública devido à perigosidade do desenvolvimento de resistência aos ARV quando a terapia é interrompida.
Na província de Nampula, a taxa de prevalência da infeção por VIH encontrava-se abaixo dos 10% em 2007 (média nacional 16%).7 Mas a baixa adesão à TARV pode provocar a disseminação de vírus resistentes e o aumento da mortalidade. Nos 21 distritos desta província (com uma população de 4.887.839 habitantes em fevereiro de 2014) estavam registados 106.197 pacientes VIH positivos, dos quais 46% em TARV com 4,8% de abandonos. A incidência média da infeção pelo VIH era de 4% nas grávidas e de 2% no Aconselhamento e Testagem em Saúde (ATS).
Assim, o problema do VIH continua preocupante e não existe um conhecimento sistematizado sobre os fatores determinantes de adesão terapêutica nesta população em Nampula.8-10
]]> Confrontada com esta situação, a Faculdade de Ciências de Saúde (FCS) da Universidade Lúrio propôs-se realizar um trabalho de investigação operacional, destinado a avaliar a adesão à TARV na província de Nampula e propor e implementar atividades de promoção da adesão terapêutica. Este artigo apresenta o estudo da linha de base inicial e tem três objetivos:1) Avaliar a adesão à TARV,11-12 nos CSP na província de Nampula;
2) Identificar os fatores associados ao abandono da TARV na perceção dos pacientes;
3) Identificar os fatores associados ao abandono da TARV na perceção dos profissionais de saúde.
Métodos
Estudo descritivo transversal, utilizando consulta documental das estatísticas da Direção Provincial de Saúde de Nampula (DPSN) e dos CS, utilizando métodos quantitativos (inquérito aos pacientes) e qualitativos (entrevistas aos profissionais e saúde).13
Universo: Oito mil, duzentos e cinquenta e um pacientes inscritos em TARV nos CSP, em terapia ou que abandonaram, em cinco CS das sedes dos distritos, durante o ano de 2014. Respetivos profissionais dos CSP, responsáveis pelos serviços TARV.
Amostra: O número de pacientes que abandonaram a TARV a entrevistar em cada distrito foi calculado utilizando a fórmula de Schuatz (n=ε2*p(1-p/i2), em que (n=número de sujeitos da amostra, ε=1,962, p=última prevalência da taxa de abandono da TARV no CS, que era em média nos cinco CS de 12%, considerando um intervalo de confiança=95%, com margem de erro de 5% i=0,05 margem de erro). Adicionaram-se 10% para perdas ocasionais ou desistências. O tamanho da amostra de pacientes que abandonaram a TARV foi aplicado para os pacientes em tratamento, de modo a permitir uma comparação das variáveis, totalizando 330 pacientes (165 pacientes em TARV e 165 abandonos). Os sujeitos foram escolhidos aleatoriamente, segundo uma data ao acaso de consulta ao serviço TARV (pacientes em terapia). Utilizamos a amostragem «bola de neve» para encontrar os pacientes que, no mesmo dia, tinham faltado à consulta ou levantamento de ARV na farmácia do CS há mais de dois meses (abandonaram a terapia), seguida de busca ativa (BA) e manifestação de disponibilidade individual (mediante explicação e assinatura de termo de consentimento informado). Os profissionais de saúde foram selecionados mediante disponibilidade individual e voluntariedade e, seguidamente, entrevistados.
Critérios de inclusão: 1) distritos: distritos com prevalência de VIH e taxa de abandono da TARV superiores à média provincial, geograficamente classificados nas categorias utilizadas no Programa Nacional de Combate ao VIH/SIDA (cidade, rural, corredor, litoral); 2) pacientes: inscritos em TARV com processo clínico localizado, maiores de idade, voluntariedade documentada em termo de consentimento informado, explicado e assinado; 3) profissionais de saúde dos CSP: atividade principal no serviço TARV, disponibilidade e voluntariedade.
Critérios de não inclusão: paciente ou profissional que não assina termo de consentimento informado.
]]> Variáveis relativas aos distritos: número de pessoas VIH+ em seguimento, número de pacientes em TARV, número de pacientes que abandonaram a TARV, incidência de VIH. Variáveis relativas aos pacientes: distrito de residência, género, idade, em TARV, abandono, escolaridade, tempo em tratamento, número de tomas e de comprimidos por dia, depressão, consumo de psicotrópicos, apoio familiar, pertença a Grupo de Apoio a Adesão Comunitário (GAAC), utilização da medicina tradicional, conhecimento sobre os riscos da má adesão, levantamento regular de ARV na farmácia nos últimos três meses, disponibilidade de alimentos, índice de massa corporal (IMC), alimentação nas últimas 24 horas, falha da medicação nas últimas 72 horas e no último mês,14 último valor de contagem de Linfócitos T CD4 (CD4) e data, causas alegadas de abandono, ocorrência de diarreia ou vómitos na última semana e de tuberculose (TB) no último mês (Quadro I).
Variáveis relativas aos profissionais dos CSP: a entrevista avaliou a sua opinião sobre os pontos negativos na organização do serviço TARV, fatores percebidos determinantes de abandono do TARV, número de GAACs funcionais, sinergias possíveis com a comunidade para melhorar a adesão terapêutica (Quadro II).
Foram analisados os dados de abandono da TARV através dos registos da DPSN e dos CS dos distritos e entrevistados os responsáveis do programa TARV.
Foram selecionados e treinados sete inquiridores (ensino secundário completado, fluência na língua local, sem ligação com o SNS, desconhecidos dos inquiridos), assinado termo de compromisso ético para procederem às BA (dos pacientes que tinham abandonado a TARV) num raio pedestre do CS (5km), sendo pagos 100 meticais (dois euros) por cada inquérito realizado, acompanhado por um dos investigadores.
]]> O estudo decorreu em quatro fases: 1) seleção dos distritos e CS (de fevereiro a agosto de 2014), a partir da consulta documental dos registos da DPSN, critérios geográficos: CS 25 Setembro, Cidade Nampula - urbano; CS Nacaroa - corredor; CS Lalaua - rural; CS Murrupula - corredor; CS Mossuril - litoral; 2) identificação dos grupos alvo, a partir dos registos dos CS (em setembro de 2014): pacientes em TARV, pacientes que abandonaram a TARV; consulta documental (estatísticas do CS e processos clínicos); 3) recolha de dados no terreno (entre outubro e novembro de 2014): aplicação de inquéritos aos pacientes,15-17 avaliação dos registos no processo clínico e de levantamento de ARV nas farmácias; entrevistas aos profissionais de saúde responsáveis do programa TARV nos CSP; 4) tratamento da informação (de dezembro de 2014 a fevereiro de 2015): introdução de dados em programa Statistical Package for Social Sciences, vs. 21, tratamento e análise de dados invariável e interpretação dos resultados.O protocolo do estudo foi aprovado pelo Comité Institucional de Bioética para a Saúde da Universidade Lúrio e pela DPSN e o estudo respeitou todas as recomendações da Declaração de Helsínquia (2013).
Resultados
Nos cinco distritos estudados (com uma população de 246.683 habitantes em outubro de 2014), os dados estatísticos mostram 19.834 pacientes VIH positivos, dos quais 42% em TARV com uma média de 11% de abandono (variando de 40% em Nacaroa até 7% em Nampula), ultrapassando em todos os casos os números apresentados pela DPSN. A incidência média da infeção pelo VIH no mesmo mês de outubro era de 7% nas grávidas e de 10% no ATS.
Da amostra inicialmente calculada de 330 pacientes foram inquiridos 295 sujeitos nos cinco CS (Quadro III), 208 em TARV, ultrapassando o valor calculado de amostra (165) para compensar a perca de abandonos, em número de 86, inferior ao previsto devido a informação inexistente ou incorreta nos processos clínicos para a sua localização pelos inquiridores nas BA, e ainda um paciente que não tinha iniciado a TARV. De uma lista de 235 abandonos foram selecionados 165 pacientes com informação registada suficiente para a busca; destes, 32% tinham morada ou nome falso, 17% tinham mudado de residência, 8% eram óbitos; dos 73 (43%) de abandonos encontrados, 60 (82%) responderam ao inquérito e foram referidos ao CS; estes mesmos pacientes convidaram outros 26 abandonos que não estavam na lista de buscas, mas que responderam ao inquérito e foram referidos ao CS. As características demográficas (género, idade, residência) e sociais (grupo étnico-linguístico, escolaridade, fonte de renda, atividade económica, dieta, crenças tradicionais) são idênticas para o grupo em TARV e para o grupo que abandonou em cada CS.
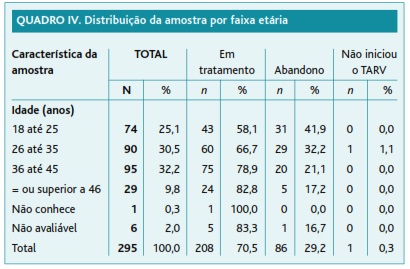
Dos 295 sujeitos inquiridos o género feminino representa 70% do grupo, com idades entre os 18 e os 62 anos. Verificamos que o abandono se manifesta inversamente proporcional à idade (Quadro IV) e que 81% tem um nível de escolaridade insuficiente (analfabetos ou nível primário) para o domínio da língua portuguesa oficial do país (compreensão e expressão limitadas).
]]>
O principal motivo evocado pelos 86 pacientes que abandonaram a TARV é o estigma ligado à infeção pelo VIH, seguido pela mudança temporária de residência e pelos efeitos secundários dos ARV. O Quadro V mostra as causas referidas por estes pacientes.
Os sinais ou sintomas de depressão estão, ou estiveram presentes, em 37% do grupo (295), mas a maioria (82%) declara que não consome psicotrópicos (o consumo de álcool é referido por 15%); a insegurança alimentar é mencionada por 58% do grupo e confirmada pelo questionário de frequência alimentar nas últimas 24 horas: 56% não consumiram fruta, 47% não comeram proteína animal, 32% não comeram proteína vegetal, 26% não comeram qualquer proteína, 22% não consumiram legumes, 21% tiveram uma única refeição no dia anterior; a magreza (IMC <18,5) ocorre em 12%.
Vários fatores associados ao abandono da TARV têm uma prevalência superior estatisticamente significativa no grupo que abandonou: início mais recente do tratamento, maior número de tomas diárias de ARV, falta de apoio familiar, desconhecimento dos GAACs e dos riscos da má adesão terapêutica (Quadro VI).
]]>
Nos pacientes em tratamento (208) 27% falharam pelo menos uma toma nos últimos três dias e 33% falharam pelo menos uma vez no último mês (a falha de duas ou mais tomas foi constatada em 23%); 26% não levantaram regularmente os ARV na farmácia do CS nos últimos três meses (o levantamento de medicamentos para todos estes pacientes está limitado à farmácia do CS). A boa adesão dos pacientes à TARV (>95% das tomas), média estimada nos cinco distritos para os últimos três meses, situa-se nos 69%, mas 36% apresentam um resultado mau ou medíocre na contagem de CD4 (<350) e 63% não estão a cumprir o protocolo de acompanhamento da TARV recomendado pelo Ministério da Saúde (contagem semestral de CD4). A ocorrência de diarreia ou vómitos na última semana é referida por 18% e a incidência de tuberculose no último mês é referida por 9%.
Os 31 profissionais dos CSP responsáveis dos serviços TARV entrevistados (cinco médicos, cinco técnicos de medicina, cinco enfermeiras de saúde materno-infantil, dois técnicos de psicologia, dois enfermeiros do Programa de Combate à Tuberculose, um licenciado e quatro técnicos de farmácia, três rececionistas, um nutricionista) transmitiram uma opinião da subestimada taxa de abandono da TARV, que a estigmatização da doença e as dificuldades alimentares constituem os fatores percebidos como determinantes principais da má adesão e do abandono, apontando ainda o deficiente registo clínico como um dos principais obstáculos ao acompanhamento eficiente destes pacientes (Quadro VII).
Discussão
Os investigadores confrontaram-se inicialmente com informação insuficiente e pouco fiável a nível central na DPSN e nos CS, incluindo a constante nos processos clínicos que não permite a busca ativa de faltosos e abandonos. As taxas de abandono da TARV estão subestimadas nas estatísticas da DPSN e na maioria dos CS.
Os principais motivos apontados para o abandono da TARV são o estigma e a discriminação, já apontados por outros autores.18 A ausência de apoio familiar é referida por mais de metade do grupo e significativamente mais prevalente nos que abandonaram a TARV.19 O baixo nível de escolaridade, poderá explicar a segunda causa referida de abandono, a viagem, na medida em que os pacientes mudavam de residência mas não faziam a transferência de documentação provisória para beneficiar da TARV no novo CS.20
A suspeita de diagnóstico de depressão é bastante prevalente e confirma outros estudos,21-22 não constando, no entanto, em nenhum registo clínico; também a maioria dos CS não dispõe de psicotrópicos antidepressivos, demonstrando a deficiência dos CSP no que respeita à saúde mental.23-26
]]> A insegurança alimentar é de alta prevalência neste grupo,27 não sendo, no entanto, referida pelos pacientes como causa direta de abandono.Embora o mau atendimento no CS ocupe o último lugar nas causas de abandono, pelo número de tomas e de comprimidos (superiores ao estipulado no programa TARV),28-30 pela data da última colheita de CD4 (superior a seis meses) e pela falta de conhecimento dos pacientes sobre os riscos de má adesão, poder-se-á inferir que muitos pacientes não estão a cumprir o protocolo recomendado para a TARV devido a um atendimento deficitário nos CSP.
Ainda o papel dos GAACs no apoio a estes pacientes, na sua perspetiva, apresenta-se insignificante em todos os distritos e mesmo discutível a sua utilidade.
Nos pacientes em TARV, a boa adesão (>95% das tomas) média estimada nos cinco distritos para os últimos três meses (69%) está abaixo da média regional e de outros estudos em África,31 o que pode explicar os resultados insuficientes na contagem de CD4 (<350) e a ocorrência de infeções oportunistas (27%), aumentando o risco de estirpes de VIH resistentes.
O abandono da TARV em Nampula é um problema grave e complexo resultante de fatores individuais (baixo nível escolar e económico),32 sociais (estigma, discriminação, falta de apoio familiar) e do funcionamento deficiente dos CSP.
Foram considerados os seguintes vieses para a realização deste estudo e respetivos modos de prevenção: vieses institucionais - fiabilidade baixa dos registos estatísticos de indicadores de saúde, controlada pela recolha in loco nos CS; insuficiências nos registos clínicos individuais, controladas pelo exame clínico dos pacientes; vieses do grupo alvo - fiabilidade das respostas aos inquéritos, controlada por triangulação de perguntas, dos registos nos processos clínicos e na farmácia do CS, para evitar vieses de aferição e de conclusão. O processo de seleção e o número da amostra dos dois grupos (em TARV e abandonos) foi diferente; no entanto, as características dos sujeitos são idênticas e o processo de recolha de dados foi igual. A predominância do género feminino nos dois grupos, ligeiramente inferior no grupo de abandonos, traduz a melhor adesão deste aos cuidados de saúde. Assim, consideramos que a amostra recolhida em cinco distritos de características geográficas distintas, englobando todas as faixas etárias da população adulta de ambos os géneros e de características sociais e económicas muito semelhantes, é representativa da população em TARV na província de Nampula.
Como implicações práticas considera-se necessário melhorar o sistema de registo e arquivo clínico dos pacientes em TARV, assim como o sistema de informação da saúde.33-34 Por outro lado, a literatura aconselha a desenvolver uma ação interdisciplinar junto de pacientes e famílias (informação e educação para a saúde, organização e formação dos GAACs, extensão rural com vista à produção local de proteína vegetal, legumes e frutas por parte das famílias), dos profissionais de saúde (organização e referenciação aos GAACs, visitas domiciliárias, formação em estratégias de prevenção da má adesão)35-37 e dos praticantes tradicionais de saúde (PTS) (alimentação saudável, doenças crónicas, dinamização dos GAACs), de forma recorrente e acompanhada para conseguir inverter esta situação e diminuir a morbilidade e mortalidade provocadas pelo VIH, assim como a sua incidência.
REFERÊNCIAS BIBLIOGRÁFICAS
1. UNAIDS. UNAIDS report on the global AIDS epidemic 2010 (Internet). UNAIDS; 2010. ISBN 9789291738717. Available from: http://www.unaids.org/globalreport [ Links ]
2. United Nations. Political declaration on HIV/AIDS: intensifying our efforts to eliminate HIV/AIDS: draft resolution submitted by the President of the General Assembly (A/65/L.77) (Internet). United Nations; 2011. Available from: http://www.un.org/ga/search/view_doc.asp?symbol=A/65/L.77 [ Links ]
3. Jesus E. Clinical significance of simplicity and adherence in antiretroviral therapy. Clinical Care Options.com (Internet); 2007. Available from: https://www.clinicaloptions.com/HIV/Treatment%20Updates/Simple/Modules/Module%202.aspx [ Links ]
4. Arrondo Velasco A, Sainz Suberviola ML, Andrés Esteban EM, Iruin Sanz AI, Napal Lecumberri V. Factores relacionados con la adherencia en pacientes infectados por el virus de la inmunodeficiencia humana (Factors associated with adherence in HIV patients). Farm Hosp. 2009;33(1):4-11. Spanish
5. Mermin J, Ekwaru JP, Were W, Degerman R, Bunnell R, Kaharuza F, et al. Utility of routine viral load, CD4 cell count, and clinical monitoring among adults with HIV receiving antiretroviral therapy in Uganda: randomised trial. BMJ. 2011;343:d6792. [ Links ]
6. African Health Observatory. Atlas of African health statistics 2014: health situation analysis of the African Region (Internet). Brazzaville: World Health Organization, Regional Office for Africa; 2014. ISBN 9789290232254. Available from: http://www.aho.afro.who.int/sites/default/files/publications/921/AFRO-Statistical_Factsheet.pdf [ Links ]
7. Grupo Técnico Multisectorial de Apoio à Luta contra o HIV/SIDA em Moçambique. Ronda de vigilância epidemiológica do HIV de 2007 (Internet). Maputo: Direcção Nacional da Assistência Médica; 2008. Available from: http://www.rosc.org.mz/index.php/documentos/doc_details/67-ronda-de-vigilancia-epidemiologica-do-hiv-de-2007 [ Links ]
8. Nachega JB, Mills EJ, Schechter M. Antiretroviral therapy adherence and retention in care in middle-income and low-income countries: current status of knowledge and research priorities. Curr Opin HIV AIDS. 2010;5(1):70-7. [ Links ]
9. Reynolds NR. Adherence to antiretroviral therapies: state of the science. Curr HIV Res. 2004;2(3):207-14. [ Links ]
10. Marcellin F, Spire B, Carrieri MP, Roux P. Assessing adherence to antiretroviral therapy in randomized HIV clinical trials: a review of currently used methods. Expert Rev Anti Infect Ther. 2013;11(3):239-50. [ Links ]
11. Williams AB, Amico KR, Bova C, Womack JA. A proposal for quality standards for measuring medication adherence in research. AIDS Behav. 2013;17(1):284-97. [ Links ]
12. Berg KM, Arnsten JH. Practical and conceptual challenges in measuring antiretroviral adherence. J Acquir Immune Defic Syndr. 2006;43 Suppl 1:S79-87. [ Links ]
13. Sankar A, Golin C, Simoni JM, Luborsky M, Pearson C. How qualitative methods contribute to understanding combination antiretroviral therapy adherence. J Acquir Immune Defic Syndr. 2006;43 Suppl 1:S54-68. [ Links ]
14. Sullivan PS, Campsmith ML, Nakamura GV, Begley EB, Schulden J, Jakashima AK. Patient and regimen characteristics associated with self-reported non adherence to antiretroviral therapy. PLoS One. 2007;2(6):e552. [ Links ]
15. Stubbs BA, Micek MA, Pfeiffer JT, Montoya P, Gloyd S. Treatment partners and adherence to HAART in Central Mozambique. AIDS Care. 2009; 21(11):1412-9. [ Links ]
16. Bulgiba A, Mohammed UY, Chik Z, Lee C, Peramalah D. How well does self-reported adherence fare compared to therapeutic drug monitoring in HAART? Prev Med. 2013;57 Suppl:S34-6. [ Links ]
17. Al-Dakkak I, Patel S, McCann E, Gadkari A, Prajapati G, Maiese EM. The impact of specific HIV treatment-related adverse events on adherence to antiretroviral therapy: a systematic review and meta-analysis. AIDS Care. 2013;25(4):400-14. [ Links ]
18. Peltzer K, Pengpid S. Socioeconomic factors in adherence to HIV therapy in low- and middle-income countries. J Health Popul Nutr. 2013;31(2):150-70. [ Links ]
19. Simoni JM, Kurth AE, Pearson CR, Pantalone DW, Merrill JO, Frick PA. Self-report measures of antiretroviral therapy adherence: a review with recommendations for HIV research and clinical management. AIDS Behav. 2006;10(3):227-45. [ Links ]
20. Falagas ME, Zarkadoulia EA, Pliatsika PA, Panos G. Socioeconomic status (SES) as a determinant of adherence to treatment in HIV infected patients: a systematic review of the literature. Retrovirology. 2008;5:13. [ Links ]
21. Nakimuli-Mpungu E, Bass JK, Alexandre P, Mills EJ, Musisi S, Ram M, et al. Depression, alcohol use and adherence to antiretroviral therapy in sub-Saharan Africa: a systematic review. AIDS Behav. 2012;16(8):2101-18. [ Links ]
22. Lucas GM. Substance abuse, adherence with antiretroviral therapy, and clinical outcomes among HIV-infected individuals. Life Sci. 2011;88(21-22):948-52. [ Links ]
23. Nel A, Kagee A. Common mental health problems and antiretroviral therapy adherence. AIDS Care. 2011;23(11):1360-5. [ Links ]
24. Nancy R. Optimizing adherence to antiretroviral therapy. In: Eron Jr JJ, Kuritzkes DR, Squires KE, editors. inPractice.com (Internet); 2014 (cited 2014 May 24; updated 2016 Apr 1). Available from: https://www.inpractice.com/Textbooks/HIV/Antiretroviral_Therapy/ch13_pt1_Adherence [ Links ]
25. Sandelowski M, Voils CI, Chang Y, Lee EJ. A systematic review comparing antiretroviral adherence descriptive and intervention studies conducted in the USA. AIDS Care. 2009;21(8):953-66. [ Links ]
26. Conway B. The role of adherence to antiretroviral therapy in the management of HIV infection. J Acquir Immune Defic Syndr. 2007;45 Suppl 1:S14-8. [ Links ]
27. Emamzadeh-Fard S, Fard SE, SeyedAlinaghi S, Paydary K. Adherence to anti-retroviral therapy and its determinants in HIV/AIDS patients: a review. Infect Disord Drug Targets. 2012;12(5):346-56. [ Links ]
28. Nischal KC, Khopkar U, Saple DG. Improving adherence to antiretroviral therapy. Indian J Dermatol Venereol Leprol. 2005;71(5):316-20. [ Links ]
29. Reisner SL, Mimiaga MJ, Skeer M, Perkovich B, Johnson CV, Safren SA. A review of HIV antiretroviral adherence and intervention studies among HIV-infected youth. Top HIV Med. 2009;17(1):14-25. [ Links ]
]]>30. Redfield RR, Blattner WA. New directions in HIV therapy and prevention: the next 25 years. In: Sanders S, editor. From cause to care: commemorating 25 years of HIV/AIDS research (Internet). Baltimore: The American Association for the Advancement of Science; 2009. p. 35-7. Available from: http://www.sciencemag.org/site/products/collectionbooks/HIV25.pdf [ Links ]
31. Mills EJ, Nachega JB, Buchan I, Orbinski J, Attaran A, Singh S, et al. Adherence to antiretroviral therapy in sub-Saharan Africa and North America: a meta-analysis. JAMA. 2006;296(6):679-90. [ Links ]
32. Rachlis BS, Mills EJ, Cole DC. Livelihood security and adherence to antiretroviral therapy in low and middle income settings: a systematic review. PLoS One. 2011;6(5):e18948. [ Links ]
33. Simoni JM, Amico KR, Smith L, Nelson K. Antiretroviral adherence interventions: translating research findings to the real world clinic. Curr HIV/AIDS Rep. 2010;7(1):44-51. [ Links ]
34. Leeman J, Chang YK, Lee EJ, Voils CI, Crandell J, Sandelowski M. Implementation of antiretroviral therapy adherence interventions: a realist synthesis of evidence. J Adv Nurs. 2010;66(9):1915-30. [ Links ]
35. Bangsberg DR. Preventing HIV antiretroviral resistance through better monitoring of treatment adherence. J Infect Dis. 2008;197 Suppl 3:S272-8. [ Links ]
36. Machtinger EL, Bangsberg DR. Seven steps to better adherence: a practical approach to promoting adherence to antiretroviral therapy. AIDS Read. 2007;17(1):43-51. [ Links ]
37. Amico KR, Orrell C. Antiretroviral therapy adherence support: recommendations and future directions. J Int Assoc Provid AIDS Care. 2013;12(2):128-37. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Paulo Das Neves Pires
Universidade Lurio, Moçambique
E-mail: druidatom@gmail.com
]]>Agradecimentos
Armindo Tonela (DPSN); Nérsio Malumbe e Januário Júnior (CS Lalaua); Ermenogildo Mulenga, Ivan Alberto, Edinete Liacha e Saide Maquina (CS Mossuril); Aguinaldo Mariano e Albino Maricoa (CS Murrupula); Eunice Zeca, Domingos Andrade, Gilda Graça e Esperança Francisco (CS Nacaroa); Carlos Felicidade e Aníbal Muteca (CS 25 de Setembro, Nampula).
Conflitos de interesse
Os autores declaram não ter quaisquer conflitos de interesse.
Recebido em 23-03-2016
Aceite para publicação em 23-01-2017
]]>