Services on Demand
Journal
Article
Indicators
Related links
Share
Portuguese Journal of Nephrology & Hypertension
Print version ISSN 0872-0169
Port J Nephrol Hypert vol.29 no.4 Lisboa Dec. 2015
CASE REPORT
Pneumococcal peritonitis in peritoneal dialysis - three case reports and literature review
Peritonite pneumocócica em diálise peritoneal – três casos clínicos e revisão da literatura
Tiago Assis Pereira, Ricardo Vizinho, Patricia Branco, Augusta Gaspar, Jose Diogo Barata
Department of Nephrology, Hospital Santa Cruz. Carnaxide, Portugal
ABSTRACT
Peritonitis and catheter-related infections are a frequent complication in peritoneal dialysis, usually driven by commensal microorganisms. They carry a significant morbidity and mortality burden and have known consequences on viability of peritoneal dialysis and patient survival.
This article describes three clinical cases, in which three different peritoneal dialysis patients presented pneumococcal peritonitis, two of which were related with obvious previous or concomitant respiratory symptoms suggesting respiratory infection.
There is scarce literature reporting pneumococcal peritonitis; only four cases are described and, excepting one, with identified primary foci of infection other than respiratory tract. The authors reinforce the probable haematogenous route of infection by a probable respiratory primary point. Although no direct or contiguous relation is evident, peritoneal patients present a higher risk of peritonitis during extra-peritoneal infections, likewise invasive pneumococcal disease, and appropriate antimicrobial approach and pro-active prophylaxis, when applicable, is necessary (e.g., vaccination).
Key-Words: Invasive pneumococcal disease; peritoneal dialysis; pneumococcal peritonitis.
RESUMO
As peritonites e infeções associadas ao catéter de diálise peritoneal constituem uma complicação frequente na diálise peritoneal. Os microrganismos responsáveis mais comuns são os constituintes da flora comensal. Estes quadros infecciosos comportam um elevado risco de morbi-mortalidade e de sobrevivência da técnica dialítica.
O presente artigo reporta três casos clínicos de peritonite pneumocócica em diferentes doentes em diálise peritoneal. Em dois destes casos, a instalação do quadro clínico foi precedida ou simultaneamente acompanhada de sintomatologia infecciosa respiratória.
Apenas quatro casos clínicos de peritonite pneumocócica em diálise peritoneal foram descritos na literatura – destes, só num foi reportada relação causal e/ou temporal com quadro infeccioso respiratório.
Os autores consideram que os casos clínicos descritos neste artigo são sugestivos de disseminação hematogénica com ponto de partida respiratório. Assim, concluiu-se por doença pneumocócica invasiva que nos doentes em diálise peritoneal pode complicar-se de peritonite.
Assim, reconhecendo este risco, embora pouco frequente, as infecções extra-peritoneais devem ser abordadas adequadamente. Em particular, o risco de doença pneumocócica invasiva pode levar ao reforço de medidas profiláticas (por exemplo, a vacinação).
Palavras-Chave: Diálise peritoneal; doença pneumocócica invasiva; peritonite pneumocócica.
INTRODUCTION
Peritonitis remains one of the main complications and clinical causes of failure and dropout of peritoneal dialysis (PD), a worldwide implemented renal replacement treatment. Still, peritonitis remains an important cause of morbidity, namely through hospitalization, and mortality1,2.The most frequent aetiological microorganisms are skin commensal gram-positive bacteria, as Staphylococcus aureus and coagulase-negative species, followed by another pathogens and negative culture peritonitis.
Beyond more frequent per luminal or intraluminal contamination, trans-visceral, haematogenous and transvaginal pathways are recognized1,2. Streptococcus pneumonia is a common pathogen, gram-positive diplococci, which constitutes part of the oropharynx resident flora.
It is frequently involved in respiratory tract infections, from non-invasive to life-threatening invasive disease.
Invasive pneumococcal disease (meningitis, bacteraemia and endocarditis) is a serious medical complication associated with certain clinical conditions, such as immunodeficiency (HIV infection, splenectomy and alcoholism) and chronic heart, kidney or lung disease3,4.
Pneumococcal peritonitis in patients not treated with PD has been reported, as primary peritonitis in patients with cirrhosis and secondary peritonitis from the gastrointestinal tract or, in females, after upper genital tract infection, recent delivery or intrauterine contraceptive devices. Haematogenous spread of S. pneumoniae from a respiratory tract infection was considered the most probable origin of pneumococcal peritonitis in cirrhotic patients by Capdevilla et al. In addition, gastro-intestinal endoscopic procedures have been also related with pneumococcal peritonitis5,6.
To the extent of our knowledge, only four cases of pneumococcal peritonitis in PD have been reported to date. Instead of a local/regional infection, here we report three cases of probable systemic involvement, this is, secondary peritonitis following haematogenous dissemination.
CASE REPORTS
Case 1
A 58-year-old man who had been treated with automated PD due to hypertensive nephrosclerosis for 90 months started an upper respiratory tract infection, characterized by mild cough, mucous expectoration and nasal discharge, without fever. Symptomatic approach was adopted, with favourable response.
One week later, already without respiratory symptoms, patient presented with abdominal pain, vomits, fever and cloudy peritoneal effluent. On physical examination, his abdomen was mildly tender and there were no inflammatory changes of the catheter exit site or respiratory and oropharyngeal signs. The patients laboratorial findings included haemoglobin 8.9 g/dL peripheral white blood cell count (WBCC) 5.200/mm3 with 64% neutrophils, C-reactive protein (CRP) 8.3 mg/dL and peritoneal cell count (PCC) 4.500 cells/mm3 with more than 95% of neutrophils.
Chest and abdominal radiographies were normal. Pending culture results, empirical antibiotic treatment comprising intraperitoneal (IP) cefazolin and ceftazidime was instituted, with clinical and laboratorial response.
The peritoneal effluent microscopic observation revealed many gram-positive coccus bacteria, however blood and peritoneal cultures were negative.
Empirical therapy was pursued, with initial favourable clinical and laboratorial evolution. However, at the 14th day a clinical relapse emerged with increased inflammatory parameters. Antibiotic therapy was switched to IP vancomycin and gentamicin.
The new peritoneal fluid cultures were also sterile. Molecular identification of the first sample was prosecuted and S. pneumoniae was identified. Vancomycin was maintained for 21 days, with cure.
Case 2
A 41-year-old man with vesico-ureteral reflux kidney disease, smoker, receiving CAPD for two months presented with productive cough, without fever.
Empirical therapy included macrolide and symptomatic medication. After two weeks, there was an unfavourable evolution, including fever, pleuritic chest pain, dyspnoea, bloody sputum, abdominal pain and cloudy peritoneal effluent. Abdominal tenderness was detected and lung auscultation revealed crackles and diminished vesicular murmur in the intermediate region of the right lung.
Blood work revealed haemoglobin 7.4 g/dL, 18.000 WBC/mm3 with neutrophilia, CRP 29.6 mg/dL and PCC 32.620/mm3 with 93% neutrophils. Chest radiography showed a homogeneous consolidation involving the entire right middle lung lobe compatible with lobar pneumonia (Fig. 1).
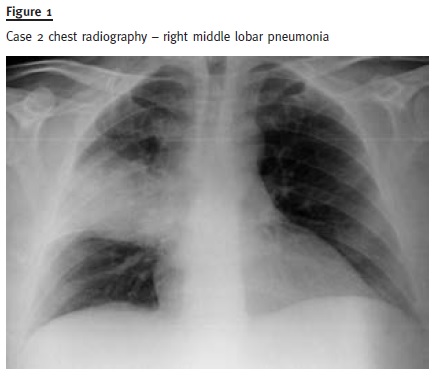
The patient was admitted and intravenous levofloxacin was instituted due to pneumonia, and IP cefazolin and ceftazidime due to peritonitis. Besides negative blood and sputum cultures, peritoneal culture was positive to S. pneumoniae, with sensitivity to penicillin.
Levofloxacin was maintained for 14 days, and cefazolin and ceftazidime switched to IP ampicillin for 14 days. The infection resolved and there were no further complications.
Case 3
A 62-year-old man with hypertensive nephrosclerosis, smoker with chronic lung disease, who started on automated PD 43 months ago, presented with generalized myalgia, abdominal pain and cloudy effluent.
No fever, haemodynamic instability or respiratory symptoms were noted. Laboratory investigations revealed haemoglobin 12.1 g/dL, 10.400 peripheral WBCC/mm3 (72% neutrophils), CRP 2 mg/dL and PCC 8.654/mm3 with 97% neutrophils. After collection of peritoneal fluid to be cultured, empirical IP cefazolin and gentamicin were initiated.
After 48 hours, there was no clinical and laboratorial response and the patient evolved with chills, and was admitted to our department. Cefazolin was changed to Vancomycin and peritoneal cultures showed S. pneumoniae, with sensitivity to penicillin.
No blood cultures were collected and thoracic radiography did not show remarkable lesions. Antibiotics were changed to IP ampicillin and oral levofloxacin.
The patient recovered without complications, after 1 week of Levofloxacin and 2 weeks of IP ampicillin.
DISCUSSION
Streptococcus pneumoniae peritonitis is associated, in general, with predisposing conditions, like immunodeficiency, cirrhosis or gynaecologic complications6,7.
In PD, only one case of pneumococcal peritonitis secondary to respiratory infection was described to date to our knowledge8. Three other cases were reported, one associated with mild vaginitis and two others with intrauterine contraceptive devices9-11.
We report three cases of pneumococcal peritonitis in PD, two of which share the same infectious source (respiratory tract) but with some clinical differences (Table I). Besides chronic kidney disease in all, smoking in two patients (one with chronic pulmonary disease), the patients had no history of encapsulated bacterial strains infections, gastrointestinal diseases or recent procedures, and presented normal liver and spleen function and anatomy. It is noteworthy that they have not been vaccinated against pneumococcal disease.
In cases 1 and 2, once started in respiratory tract, the infection seemed to spread haematologically, with transdiafragmatic route less plausible in these cases, given the location of infection and absence of diaphragmatic-localized symptoms or pleural disease evidence. The third case did not present specific respiratory symptoms, which makes peritonitis secondary to respiratory airway entry and subjacent bacteraemia implausible. An alternative hypothesis is that whilst in incubation time, secondary peritonitis and subsequent clinical manifestations occurred before respiratory emerged. In this case, blood cultures (not collected) would be essential to document bacteraemia, as chills occurrence seems to indicate.
Diagnosis was possible in case 1 only by molecular techniques, whereas in cases 2 and 3 a peritoneal culture was positive. Although haematogenous spread was suspected, blood cultures were negative.
Urinary pneumococcal antigens were not pursued, however it could be collected since patients had renal residual function.
Regarding antibiotic susceptibility, only in case 1 there was probable methicillin-resistance to cefazolin and ceftazidime and susceptibility to vancomycin, given the clinical course. In the other patients, antibiotic susceptibility was evaluated in vitro and confirmed clinically.
Penicillin pneumococcal resistance has met a worldwide rising prevalence that varies between regions and populations, as well a greater macrolide resistance.
Vancomycin has been recognized as one alternative antibiotic against S. pneumoniae resistant to penicillin and other classes in pneumococcal disease12.
Chronic kidney disease is considered a high risk factor of invasive pneumococcal disease, probably due to reduced antibody response to bacterial polysaccharide antigens. Prevention of high-risk groups, targeting a minor incidence and severity of infection, has been advocated and concretized since the 1980s, by vaccination with polysaccharide and/or conjugate vaccine13.
Different medical organizations recommend pneumococcal vaccination for patients with chronic renal failure, but with discrepant recommendations (between single-time vaccinations to a 5-year interval vaccination schedule). Like other vaccinations response, the pneumococcal seems to lack a full serum response, supporting a more frequent revaccination plan13,14. An observational study by Gilbertson et al. evaluated pneumococcal vaccination in haemodialysis patients, revealing a significant association between vaccination and lower mortality, accounting some poorer prognosis factors associated with the vaccination group. The authors argued in favour of this vaccination in haemodialysis patients, even with reinforced vaccination schedules15. These results were further supported by a retrospective study where influenza and pneumococcal vaccination were independently associated with improved survival in this population16.
In Portugal, pneumococcal vaccination has been available since 2001, however it was not included in the National Immunization Plan (free of charge and universal) and was only granted to children pertaining to high-risk groups. Since July 2015, a new public clinical directive resulted in a universal and free vaccination in all children and adult highrisk groups for invasive pneumococcal disease. For this last group, which includes chronic kidney disease patients, it is recommended a sequential vaccination with 13-valent conjugate vaccines and 23-valent polysaccharide vaccines, in order to promote a broader protection against pneumococcal serotypes. The expected consequences are direct protection from the main pneumococcal serotypes and indirect protection by group immunization17.
These three cases reinforce the need of concretizing anti-pneumococcal vaccination in chronic kidney disease patients, as well as early diagnosis and timely approach of respiratory infectious illnesses in order to prevent invasive or systemic repercussion.
Although a rare cause of peritonitis in PD, pneumococcal infection should be included in the differential diagnoses in the setting of suspicious peritonitis simultaneously or shortly after respiratory tract infection, considered the potential invasive nature of this disease.
References
1. Li PK, Szeto CC, Piraino B, et al. with the International Society for Peritoneal Dialysis. Peritoneal dialysis-related infections recommendations: 2010 update. Perit Dial Int 2010; 30(4): 393–423. [ Links ]
2. Davenport A. Peritonitis remains the major clinical complication of peritoneal dialysis: the London, UK, peritonitis audit 2002-2003. Perit Dial Int 2009; 29(3): 297–302. [ Links ]
3. Musher D. Streptococcus pneumoniae. In: Mandel G, Bennett J, Dolin R, eds. Mandel, Douglas and Bennetts Principles and Practice of Infectious Diseases. 7th ed. Philadelphia. Churchill Livingstone Elsevier; 2010: 2623-2642. [ Links ]
4. From the Centers for Disease Control and Prevention. Updated recommendations on the use of pneumococcal conjugate vaccine in a setting of vaccine shortage –Advisory Committee on Immunization Practices. JAMA 2002; 287(7): 833–834. [ Links ]
5. Capdevila O, Pallares R, Grau I, et al. Pneumococcal peritonitis in adult patients: report of 64 cases with special reference to emergence of antibiotic resistance. Arch Intern Med 2001; 161(14): 1742–1748. [ Links ]
6. Pasticci M, Donnini A, Mencacci A, Lapalorcia LM, Cavazzoni E, Baldelli F. A diagnosis of pneumococcal peritonitis secondary to pyo-salpinx in a young healthy female by culturing peritoneal pus. New Microbiol 2008; 31(2): 295–298. [ Links ]
7. Nielsen KR, Ejlertsen T, El-Batran S, Prag J. A five-year survey of pneumococcal peritonitis in two Danish counties–incidence, diagnosis and clinical entities. Clin Microbiol Infect 2003; 9(7): 738–740. [ Links ]
8. Al-Wali W, Baillod R, Hamilton-Miller JM, Brumfitt W. Peritonitis by Streptococcus pneumoniae secondary to pneumococcal chest infection in a patient on continuous ambulatory peritoneal dialysis. Nephron 1991; 59(1): 173. [ Links ]
9. Agarwal AK, Wilmer WA, Bay WH, Falkenhain ME, Mangino JE. Pneumococcal and gonococcal peritonitis due to vaginitis. Perit Dial Int 2002; 22(6): 731–732. [ Links ]
10. Korzets A, Chagnac A, Ori Y, Zevin D, Levi J. Pneumococcal peritonitis complicating CAPD-was the indwelling intrauterine device to blame? Clin Nephrol 1991; 35(1): 24–25. [ Links ]
11. Stuck A, Seiler A, Frey FJ. Peritonitis due to an intrauterine contraceptive device in a patient on CAPD. Perit Dial Bull 1986; 6:158-9 [ Links ]
12. Whitney CG, Farley MM, Hadler J, et al. with the Active Bacterial Core Surveillance Program of the Emerging Infections Program Network. Increasing prevalence of multidrug- resistant Streptococcus pneumoniae in the United States. N Eng J Med 2000; 343(26): 1917–1924. [ Links ]
13. Mahmoodi M, Aghamohammadi A, Rezaei N, et al. Antibody response to pneumococcal capsular polysaccharide vaccination in patients with chronic kidney disease. Eur Cytocine Netw 2009; 20(2): 69–74. [ Links ]
14. Pourfarziani V, Ramezani M, Taheri S, Izadi M, Einollahi B. Immunogenicity of pneumococcal vaccination in renal transplant recipients and hemodialysis patients: a comparative controlled trial. Ann Transplant 2008; 13(3): 43–47. [ Links ]
15. Gilbertson D, Guo H, Arneson TJ, Collins AJ. The association of pneumococcal vaccination with hospitalization and mortality in hemodialysis patients. Nephrol Dial Transplant 2011; 26(9): 2934–2939. [ Links ]
16. Bond TC, Spaulding AC, Krisher J, McClellan W. Mortality of dialysis patients according to influenza and pneumococcal vaccination status Am J Kidney Dis 2012; 60(6): 959–965. [ Links ]
17. Direcção-Geral da Saúde. Norma nº011/2015 – Vacinação contra infecções por Streptococcus pneumoniae de grupos com risco acrescido para doença invasiva pneumocócica. 2012. [ Links ]
Dr.Tiago Assis Pereira
Department of Nephrology, Hospital Santa Cruz,
Av. Prof. Dr Reinaldo dos Santos, 2799-523 Carnaxide, Portugal.
E-mail: tiago_assis_pereira@yahoo.com
Conflict of interest statement: None declared.
Received for publication: 30/08/2015
Accepted in revised form: 01/11/2015














