Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Nascer e Crescer
versão impressa ISSN 0872-0754versão On-line ISSN 2183-9417
Nascer e Crescer vol.29 no.3 Porto set. 2020
https://doi.org/10.25753/BirthGrowthMJ.v29.i3.18244
ORIGINAL ARTICLES | ARTIGOS ORIGINAIS
Quality of life of adolescents with type 1 diabetes mellitus
Qualidade de vida de adolescentes com diabetes mellitus tipo 1
Sofia VasconcelosI, Sara Monteiro CunhaI, Alícia RebeloI, Carla FerreiraII, Carla MeirelesI, Ângela DiasI
I Department of Pediatrics, Hospital Senhora da Oliveira - Guimarães. 4835-044 Guimarães, Portugal. sofiavasconceloslopes@gmail.com; saracunha@hospitaldeguimaraes.min-saude.pt; aliciarebelo@hospitaldeguimaraes.min-saude.pt; carlabilhoto@hospitaldeguimaraes.min-saude.pt; angeladias@hospitaldeguimaraes.min-saude.pt
II Department of Pediatrics, Hospital de Braga. 4710-243 Braga, Portugal. carlamf85@hotmail.com
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Introduction: Type 1 diabetes mellitus is one of the most common endocrine-metabolic disorders of childhood and adolescence and requires a continuous and rigorous therapeutic approach, with recognized impact on children and adolescents’ quality of life.
The purpose of this study was to evaluate the quality of life of adolescents with type 1 diabetes mellitus and its relationship with clinical and laboratory aspects and lifestyle.
Material and Methods: DQOL questionnaire was applied to type 1 diabetes mellitus adolescents managed at the Pediatric Diabetology consultation of a level II hospital for more than one year. Questionnaire has a global score between 36 and 180, with higher scores reflecting worse quality of life. Statistical analysis was performed in SPSS®.
Results: Seventy-one percent (n=36) of adolescents responded to the survey, 55.6% of which male, with a median age of 15 years. Median DQOL global score was 66. Adolescents with good metabolic control had a median global score of 49, compared with 71 in adolescents with poor metabolic control (p=0.007). The median global score of self-perception of better health was 51 compared to 73 for self-perception of poorer health (p=0.007).
Discussion: In general, adolescents in this study revealed a satisfactory quality of life. Adolescents with better metabolic control have a higher satisfaction and better quality of life. Adolescents with better self-perceived health have a better quality of life.
Conclusion: Recognizing factors that affect quality of life of adolescents with type 1 diabetes mellitus is crucial to devise therapeutic strategies that meet their expectations, promoting treatment adherence and better metabolic control.
Keywords: adolescents; metabolic control; quality of life; type 1 diabetes mellitus
RESUMO
Introdução: A diabetes mellitus tipo 1 é uma das doenças endócrinas mais comuns em idade pediátrica e implica um tratamento contínuo e rigoroso, com impacto na qualidade de vida das crianças e adolescentes afetados.
O objetivo deste estudo foi avaliar a qualidade de vida de adolescentes com diabetes mellitus tipo 1 e a sua relação com aspetos clínico-laboratoriais e estilos de vida.
Material e Métodos: O questionário DQOL foi aplicado a adolescentes com diabetes mellitus tipo 1 seguidos em consulta de Diabetologia Pediátrica de um hospital de nível II há mais de um ano. O questionário tem uma pontuação global entre 36-180, com maior pontuação a refletir pior qualidade de vida. A análise estatística foi efetuada no software SPSS®.
Resultados: Responderam ao inquérito 71% (n=36) dos adolescentes, 55,6% dos quais do sexo masculino, com uma mediana de idades de 15 anos. A mediana de pontuação global no DQOL foi 66. Os adolescentes com bom controlo metabólico tiveram uma mediana de pontuação global de 49 em comparação com 71 no grupo com mau controlo metabólico (p=0,007). A pontuação global mediana de auto-perceção de melhor saúde foi 51 em comparação com 73 para a auto-perceção de pior saúde (p=0,007).
Discussão: No geral, os adolescentes deste estudo revelaram uma boa qualidade de vida. Adolescentes com melhor controlo metabólico têm maior satisfação e melhor qualidade de vida e adolescentes com melhor auto-perceção de saúde têm melhor qualidade de vida.
Conclusão: Reconhecer os fatores que afetam a qualidade de vida dos adolescentes com diabetes mellitus tipo 1 é fundamental para delinear estratégias terapêuticas que vão de encontro às suas expectativas, promovendo a adesão à terapêutica e um melhor controlo metabólico.
Palavras-chave: adolescentes; controlo metabólico; diabetes mellitus tipo 1; qualidade de vida
Introduction
Type 1 diabetes mellitus (T1DM) is one of the most common endocrine-metabolic disorders of childhood and adolescence, affecting one in every 300 to 500 children and adolescents.1,2 It is caused by destruction of beta pancreatic cells that leads to progressive insulin production failure.3
T1DM treatment is continuous and very demanding, including multiple daily subcutaneous insulin administrations, blood glucose monitoring, dietary planning, physical activity, and frequent medical consultations.4
Patients frequently have difficulty in accepting such lifestyle changes, particularly during adolescence. Teenagers are in a critical developmental period, with physiologic, psychosocial, and behavioral changes, and a disease like T1DM can be a threat to their independence and autonomy. They may feel different from peers in a time when it is crucial to belong to social group as equal.3
Because of this, T1DM can have an important impact in adolescents’ quality of life (QoL), who are at greater risk of impaired metabolic control, treatment discontinuation, and resistance in accepting the disease and making lifestyle changes, potentially leading to serious T1DM complications.2,3,5
QoL is a core criterion in determining the therapeutic outcome of chronic conditions.1 Investigating the disease self-perception and aspects influencing QoL is crucial for a better approach to adolescents in consultation, in order to minimize T1DM impact in their QoL and improve metabolic control.
The purpose of this study was to evaluate QoL and disease self-perception in adolescents with T1DM managed at the Pediatric Diabetes consultation of “Hospital Senhora da Oliveira-Guimarães” and investigate its association with clinical and laboratorial features and different lifestyles.
Methods
A questionnaire was applied to adolescents managed at the Pediatric Diabetes consultation of “Hospital Senhora da Oliveira-Guimarães” aged between 10 and 17 years with T1DM diagnosis for more than one year. A total of 51 patients fitted these criteria and were eligible for study inclusion, 36 (71%) of which participated in the study.
The first part of the questionnaire included data regarding age, gender, household, parents’ civil status, residence, disease duration, age at diagnosis, insulin administration type, blood glucose control frequency, bolus calculator and/or flash system use, hypoglycemia episodes, hyperglycemia in the last three months, and physical activity.
Diabetes Quality of Life (DQOL) questionnaire comprised the second part of the questionnaire.6 DQOL evaluates QoL of adolescents with T1DM and is translated and validated for the Portuguese population. It comprises 36 items divided into three subscales: “Impact of diabetes”, with 13 questions; “Preoccupations related to diabetes”, with six questions; and “Satisfaction”, with 17 questions. These are Likert-type queries with five answer options, in which ‘one’ means ‘Never’ and ‘five’ means ‘Always’. The final global score (GS) is obtained from the sum of all question scores and varies between 36 and 180. Higher GS reflects worst QoL.
DQOL ends with a question about health self-perception compared with healthy adolescents, which can be classified as “Excellent”, “Good”, “Satisfactory”, or “Bad”.
Information of the last three glycated hemoglobin (HbA1c) measurements was retrieved from adolescents’ clinical records. A mean value of the three HbA1c measurements below 7.5% was considered good metabolic control. HbA1c was determined by point-of-care testing (AfinionTM).
Data collection and statistical analysis was performed using IBM SPSS statistics 25®. Categorical variables were characterized by absolute and relative frequencies, and continuous variables by median and interquartile range. Comparison of questionnaire scores with categorical variables was performed using Mann-Whitney U test. A p value inferior to 0.05 was considered statistically significant.
Results
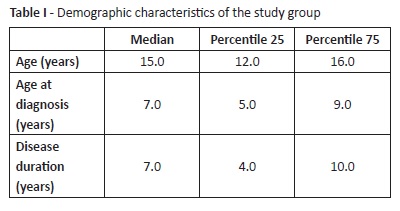
In the present cohort of 36 adolescents, 55.6% were male (n=20) and the median age was 15.0 years (P25-12.0; P75-16.0 years). Disease duration varied between one to 16.0 years, with a median of seven years (P25-4; P75-10 years). Most adolescents had been diagnosed before the age of ten (77.8%, n=28; Table I).
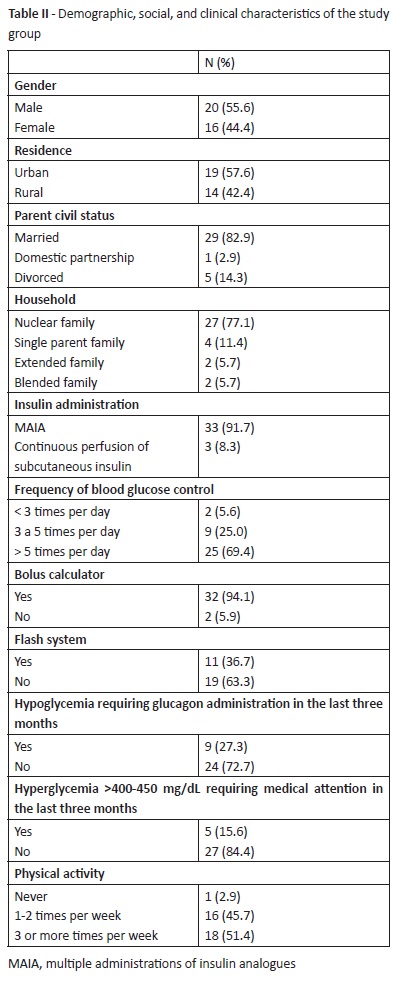
About half of adolescents (57.6%, n=19) lived in urban areas and 77.1% (n=27) belonged to a nuclear family (Table II).
Most adolescents (91.7%, n=33) underwent multiple administrations of insulin analogues (MAIA) and 69.4% (n=25) measured blood glucose control more than five times per day. Flash system was used by 36.7% (n=11) of patients and bolus calculator by 94.1% (n=32; Table II).
Median HbA1 was 8.2% (P25-7.5%; P75-9.8%). One quarter of patients (n=9) had good metabolic control.
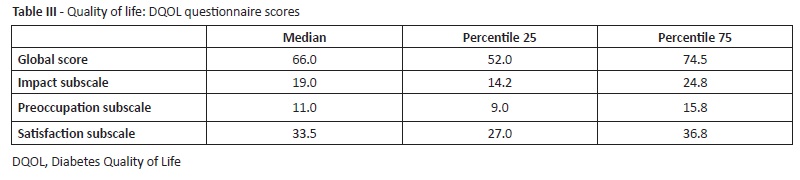
Median DQOL GS was 66.0 (P25-52; P75-74.5). Data from DQOL subscale scores is described on Table III.
(clique para ampliar ! click to enlarge)
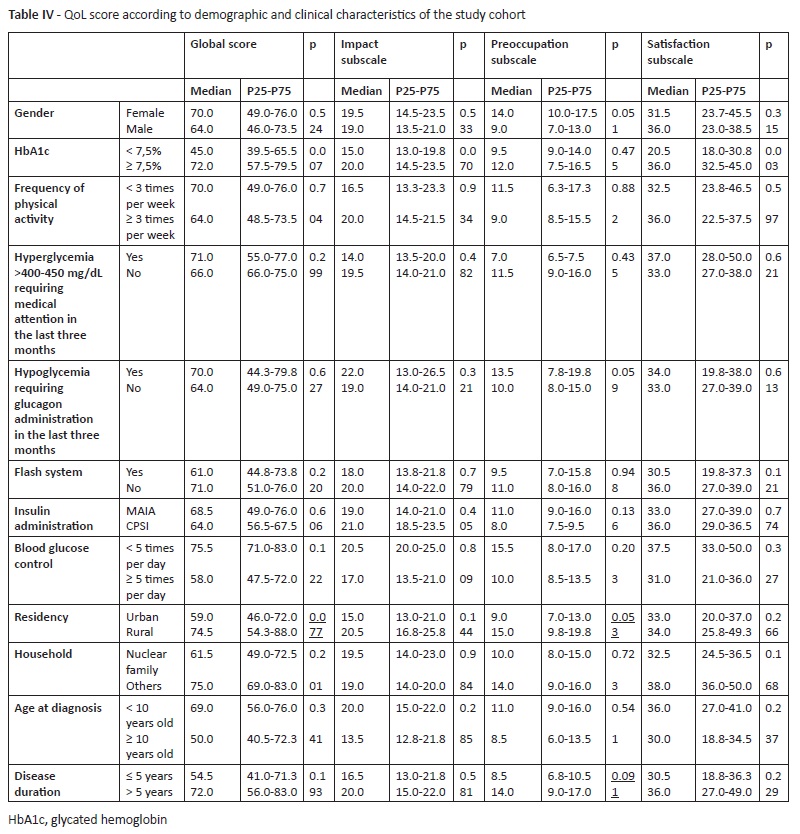
Adolescents with good metabolic control had a median GS of 45.0, and those with bad metabolic control of 72.0 (p=0.007). On “Satisfaction” subscale, median score was 20.5 for adolescents with HbA1c <7.5% and 36.0 for those with HbA1c ≥7.5% (p=0.003) (Table IV).
(clique para ampliar ! click to enlarge)
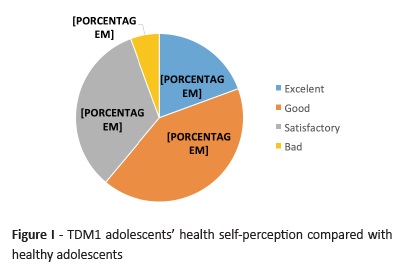
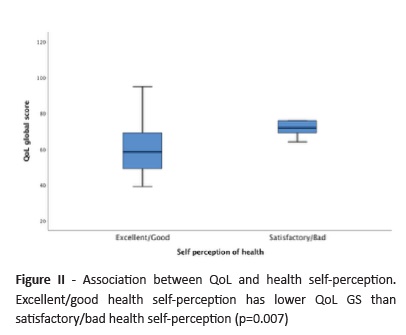
Sixty-one percent of patients classified their health as excellent or good compared with healthy adolescents (Figure I). Median self-perception of better health (excellent or good) GS was 58.5 (P25-48.3; P75-69.8) compared with 72.0 (P25-67.8; P75-78.8) for self-perception of worst health (satisfactory or bad; p=0.007; Figure II).
No statistically significant difference was found regarding the remaining variables (Table IV).
Discussion
GS results indicate that the present cohort generally reports satisfactory QoL, in agreement with the literature.1,2,3,7 This can be explained by good treatment adaptation and good medical team and family support.
A study by Oliveira et al. that applied the same questionnaire to a similar patient population reported a mean overall GS of 103.63 and a mean GS of 21.47 for “Impact” subscale, 15.33 for “Preoccupation” subscale, and 65.13 for “Satisfaction” subscale.1 Compared to the present study, Oliveira study reported worst QoL, both globally and in different subscales. Such discrepant results may be explained by the lower number of patients with good metabolic control included in that study compared with the present cohort. On the other hand, the present study included a higher percentage of male patients, who had better results in GS and in two subscales than female patients. Since the study by Oliveira included a majority of female patients, it can be hypothesized that this gender difference may also have contributed to its worst results regarding QoL.
This study showed no statistically significant differences regarding sociodemographic parameters. However, results also showed that adolescent girls are more worried about the disease than boys, what is in line with studies by Costa el al. and Hoey et al.5,8 This can be explained by the fact that females have earlier pubertal and hormonal changes, higher incidence of psychological disturbances, and potentially worry more about the effects of insulin injections or glucose monitoring on their figure than males.2,8 Some studies show a worst QoL of female adolescents with T1DM, a finding that could not be replicated in the present study. 2,5,8
Adolescents living in urban areas reported better QoL and less concern about the disease than those living in rural areas. This can be due to rural area populations having a lower education level and living farther away from medical resources, what may result in a greater risk of developing important hypoglycemia and hyperglycemia events. These findings are supported by other studies.2 Most patients in this cohort had a nuclear family, what precluded establishing an association between type of family and QoL.
Similarly to what has been reported by other authors, this study showed that adolescents with more than five years of disease were more concerned with the disease and had worse QoL than adolescents with less years of disease.3,5 Costa el al. found a correlation between lower satisfaction and longer time since diagnosis and, although not statistically significant, the same tendency was found in this study.5 In this cohort, median age was 14 years and median disease duration was seven years, meaning that most patients were diagnosed during childhood and were currently in the chronic phase of the disease, as reported by others.3 In this study, having a T1DM diagnosis during childhood or adolescence did not have a significant impact on QoL. This suggests that disease duration is more important in QoL deterioration than age at diagnosis.
As predicted, adolescents experiencing severe hypoglycemia episodes were more concerned with the disease. However, this did not reflect on QoL GS. Patients experiencing severe hypoglycemia episodes are probably those who do not comply with treatment nor make lifestyle changes to better manage the disease, what may explain why they believe not to have a worse QoL. Conversely, Hassan et al. reported that adolescents with severe hypoglycemia episodes had worse QoL.2
Although this study found no association between important hyperglycemia episodes and QoL, another study found a correlation between hyperglycemia and higher concern and lower satisfaction levels.3
Physical activity is a particularly important aspect of T1DM management and an important factor when it comes to evaluating QoL in healthy adolescents. An improvement in QoL and clinical disease control has been shown in adolescents who are physically active.5 As this study included only one patient with no physical activity, it was not possible to evaluate its impact on QoL. We did however verified that the amount of physical activity (> or < three times a week) had no relation with QoL GS or any sub-scale. The small sample included in this study precludes a solid explanation for these results.
In agreement with other authors, no significant association was found between insulin regimen and QoL in this study, but only three patients with continuous perfusion of subcutaneous insulin were included.7,8
Also no association was found between using flash system to monitor glucose and QoL in this study. Although blood glycemic evaluation frequency had no statistically significant association with QoL, patients assessing blood glucose less than five times a day had higher GS, meaning they report worse QoL. These findings were similar to other studies.2 Patients who monitor glucose can more frequently perform treatment adjustments with insulin or sugar according to results, resulting in better glucose stability and better metabolic control.
Metabolic control has been a target in T1DM treatment.5 It is well documented in different studies that poor metabolic control has a significant relation with worse QoL.1,2,5,8-10 This study’s results agree with that evidence, as adolescents with poor metabolic control evidenced worse quality of life and less satisfaction with the disease, and that was statistically significant. They also tend to experience a greater impact of the disease in their life, as reported by Oliveira et al.1
Most adolescents in this cohort classified their health perception as good or excellent compared with healthy adolescents. Despite their chronic condition, they consider themselves as healthy people, what can be partially explained by these patients being young and at a disease stage with no irreversible complications yet.
Adolescents with better health self-perception reported better QoL, less disease impact on their daily life, and less concern. They also tended to be more satisfied than adolescents with worse health perception, in agreement with another study.3
Conclusions
T1DM is a condition requiring intensive treatment and routine and lifestyle modifications. Metabolic control and QoL are very important in T1DM management.
Despite their chronic disease, T1DM adolescents regard themselves as healthy people with satisfactory QoL. Those with better metabolic control and health self-perception are more satisfied and have a better QoL.
Recognizing factors affecting QoL in these patients is crucial for devising therapeutic strategies that meet their expectations and promoting treatment adherence and better metabolic control.
REFERENCES
1. Oliveira RS, Santos S, Laranjo G, Luís A, Campos J. Diabetes, adolescência e qualidade de vida. Acta Pediatr Port. 2013; 44:156-60. [ Links ]
2. Hassan M, Musa N, Abdel Hai R, Fathy A, Ibrahim A. Assessment of health-related quality of life in Egyptian adolescents with type 1 diabetes: DEMPU survey. J Pediatr Endocrinol Metab. 2017; 30:277-83. Epub 2017/02/27. DOI: 10.1515/jpem-2016-0147. PubMed PMID: 28236627. [ Links ]
3. Santana PF, Oliveira LCB, Maia RS, Rocha NSPD. Avaliação da qualidade de vida em adolescentes com diabetes mellitus tipo 1 em um hospital universitário. Adolesc Saude. 2016; 13:24-32. [ Links ]
4. Kalyva E, Malakonaki E, Eiser C, Mamoulakis D. Health-related quality of life (HRQoL) of children with type 1 diabetes mellitus (T1DM): self and parental perceptions. Pediatr Diabetes. 2011; 12:34-40. Epub 2010/06/16. DOI: 10.1111/j.1399-5448.2010.00653.x. PubMed PMID: 20546163. [ Links ]
5. Costa LM, Vieira SE. Quality of life of adolescents with type 1 diabetes. Clinics. 2015; 70:173-9. DOI: 10.6061/clinics/2015(03)04. [ Links ]
6. Almeida JP, Pereira MG. Questionário de Avaliação da Qualidade de Vida para adolescentes com Diabetes Tipo 1: Estudo de validação do DQOL. Análise Psicológica. 2008; 2:295-307. [ Links ]
7. Laffel LMB, Connell A, Vangsness L, Goebel-Fabbri A, Mansfield A, Anderson BJ. General Quality of Life in Youth With Type 1 Diabetes. Diabetes Care. 2003; 26:3067-73. [ Links ]
8. Hoey H, Aanstoot H-J, Chiarelli F, Daneman D, Danne T, Dorchy H, et al. Good Metabolic Control Is Associated With Better Quality of Life in 2,101 Adolescents With Type 1 Diabetes. Diabetes Care. 2001; 24:1923-28. [ Links ]
9. Wagner VM, Muller-Godeffroy E, von Sengbusch S, Hager S, Thyen U. Age, metabolic control and type of insulin regime influences health-related quality of life in children and adolescents with type 1 diabetes mellitus. Eur J Pediatr. 2005; 164:491-6. Epub 2005/05/06. DOI: 10.1007/s00431-005-1681-4. PubMed PMID: 15875213. [ Links ]
10. Özyazıcıoğlu N, Avdal EÜ, Sağlam H. A determination of the quality of life of children and adolescents with type 1 diabetes and their parents. International Journal of Nursing Sciences. 2017; 4:94-8. DOI: 10.1016/j.ijnss.2017.01.008. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Sofia Vasconcelos
Department of Pediatrics
Hospital Senhora da Oliveira - Guimarães
Rua dos Cutileiros 114, Creixomil
4835-044 Guimarães
Email: sofiavasconceloslopes@gmail.com
Received for publication: 08.07.2019. Accepted in revised form: 11.03.2020